Abstract
Purpose
Shunt placement indications are stringent and require confirmation of clinical and radiological evidence of hydrocephalus (HC). The aim of this study was to determine the rate of shunting and discuss the outcome in the first year of life in patients with myelomeningocele (MMC) on the basis of review of the literature.
Methods
All patients who underwent postnatal repair of MMC at our institution between March 2014 and March 2015 were evaluated. Patients were only included if they underwent both MMC repair and ventriculoperitoneal (VP) shunt insertion at our institution and were followed up for at least 12 months. The mean ages for repair of MMC, MMC levels, timing of VP shunt placement, shunt revisions, and causes of shunt revisions were documented.
Results
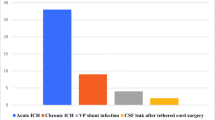
Fifty-two patients with MMC were included in this study. The average gestational age at birth was 38 weeks. The level of MMC was thoracolumbar in 13 cases, 11 times lumbar, 21 times lumbosacral, and 7 times sacral. Thirty-one patients (59.61%) suffered from hydrocephalus and required placement of a shunt. When we evaluate the lesion levels of patients who require shunting, 13 cases were thoracolumbar, 6 cases were lumbar, and 11 cases were lumbosacral. None of the sacral cases needed VP shunt. Seven patients (13.4%) had shunt revision within the first year of life. The cause of shunt revision was wound problem in one patient (1.9%), underdrainage in two patients (3.8%), infection in three patients (5.7%), and mechanical obstruction in another one patient (1.9%).
Conclusion
MMC closure and management of the associated HC are one of the most basic, but never simple, legs of the pediatric neurosurgery around the world. As clinicians and neurosurgeons, we are obligated to analyze recent evidences and evaluate present approaches to achieve optimization in this subject until further technologies or approaches became more advantageous for our patients.
Similar content being viewed by others
References
Tulipan N, Sutton LN, Bruner JP, Cohen BM, Johnson M, Adzick NS (2003) The effect of intrauterine myelomeningocele repair on the incidence of shunt-dependent hydrocephalus. Pediatr Neurosurg 38(1):27–33. https://doi.org/10.1159/000067560
Botto LD, Lisi A, Robert-Gnansia E, Erickson JD, Vollset SE, Mastroiacovo P, Botting B, Cocchi G, de Vigan C, de Walle H, Feijoo M, Irgens LM, McDonnell B, Merlob P, Ritvanen A, Scarano G, Siffel C, Metneki J, Stoll C, Smithells R, Goujard J (2005) International retrospective cohort study of neural tube defects in relation to folic acid recommendations: are the recommendations working? BMJ 330(7491):571–570. https://doi.org/10.1136/bmj.38336.664352.82
Alatas I, Demirci H, Canaz H, Akdemir O, Baydin S, Ozel K (2015) The role of urodynamic studies in the diagnosis and treatment of patients with spina bifida. Asian J neurosurgery 10(2):83–86. https://doi.org/10.4103/1793-5482.154872
Rintoul NE, Sutton LN, Hubbard AM, Cohen B, Melchionni J, Pasquariello PS, Adzick NS (2002) A new look at myelomeningoceles: functional level, vertebral level, shunting, and the implications for fetal intervention. Pediatrics 109(3):409–413. https://doi.org/10.1542/peds.109.3.409
Steinbok P, Irvine B, Cochrane DD, Irwin BJ (1992) Long-term outcome and complications of children born with meningomyelocele. Child’s Nervous System: ChNS: Official J Int Society Pediatric Neurosurgery 8(2):92–96. https://doi.org/10.1007/BF00298448
Adzick NS, Thom EA, Spong CY, Brock JW 3rd, Burrows PK, Johnson MP, Howell LJ, Farrell JA, Dabrowiak ME, Sutton LN et al (2011) A randomized trial of prenatal versus postnatal repair of myelomeningocele. N Engl J Med 364(11):993–1004. https://doi.org/10.1056/NEJMoa1014379
Chakraborty A, Crimmins D, Hayward R, Thompson D (2008) Toward reducing shunt placement rates in patients with myelomeningocele. J Neurosurg Pediatr 1(5):361–365. https://doi.org/10.3171/PED/2008/1/5/361
Bowman RM, McLone DG, Grant JA, Tomita T, Ito JA (2001) Spina bifida outcome: a 25-year prospective. Pediatr Neurosurg 34(3):114–120. https://doi.org/10.1159/000056005
Hetherington R, Dennis M, Barnes M, Drake J, Gentili F (2006) Functional outcome in young adults with spina bifida and hydrocephalus. Child’s Nervous System: ChNS: Official J Int Society Pediatric Neurosurgery 22(2):117–124. https://doi.org/10.1007/s00381-005-1231-4
Wills KE, Holmbeck GN, Dillon K, McLone DG (1990) Intelligence and achievement in children with myelomeningocele. J Pediatr Psychol 15(2):161–176. https://doi.org/10.1093/jpepsy/15.2.161
Phillips BC, Gelsomino M, Pownall AL, Ocal E, Spencer HJ, O’Brien MS, Albert GW (2014) Predictors of the need for cerebrospinal fluid diversion in patients with myelomeningocele. J Neurosurg Pediatr 14(2):167–172. https://doi.org/10.3171/2014.4.PEDS13470
Bowman RM, McLone DG (2010) Neurosurgical management of spina bifida: research issues. Developmental Disabilities Res Reviews 16(1):82–87. https://doi.org/10.1002/ddrr.100
Wakhlu A, Ansari NA (2004) The prediction of postoperative hydrocephalus in patients with spina bifida. Child’s Nervous System: ChNS: Official J Int Society Pediatric Neurosurgery 20(2):104–106. https://doi.org/10.1007/s00381-003-0849-3
Melo JR, Pacheco P, Melo EN, Vasconcellos A, Passos RK (2015) Clinical and ultrasonographic criteria for using ventriculoperitoneal shunts in newborns with myelomeningocele. Arq Neuropsiquiatr 73(9):759–763. https://doi.org/10.1590/0004-282X20150110
Rodrigues AB, Krebs VL, Matushita H, de Carvalho WB (2016) Short-term prognostic factors in myelomeningocele patients. Child’s Nervous System: ChNS: Official J Int Society Pediatric Neurosurgery 32(4):675–680. https://doi.org/10.1007/s00381-016-3012-7
Sinha SK, Dhua A, Mathur MK, Singh S, Modi M, Ratan SK (2012) Neural tube defect repair and ventriculoperitoneal shunting: indications and outcome. J Neonatal Surgery 1(2):21
Januschek E, Rohrig A, Kunze S, Fremerey C, Wiebe B, Messing-Junger M (2016) Myelomeningocele—a single institute analysis of the years 2007 to 2015. Child’s Nervous System: ChNS: Official J Int Society Pediatric Neurosurgery 32(7):1281–1287. https://doi.org/10.1007/s00381-016-3079-1
Vinchon M, Dhellemmes P (2006) Cerebrospinal fluid shunt infection: risk factors and long-term follow-up. Child’s Nervous System: ChNS: Official J Int Society Pediatric Neurosurgery 22(7):692–697. https://doi.org/10.1007/s00381-005-0037-8
Hanak BW, Bonow RH, Harris CA, Browd SR (2017) Cerebrospinal fluid shunting complications in children. Pediatr Neurosurg. https://doi.org/10.1159/000452840
McGirt MJ, Leveque JC, Wellons JC 3rd, Villavicencio AT, Hopkins JS, Fuchs HE, George TM (2002) Cerebrospinal fluid shunt survival and etiology of failures: a seven-year institutional experience. Pediatr Neurosurg 36(5):248–255. https://doi.org/10.1159/000058428
Choux M, Genitori L, Lang D, Lena G (1992) Shunt implantation: reducing the incidence of shunt infection. J Neurosurg 77(6):875–880. https://doi.org/10.3171/jns.1992.77.6.0875
Caldarelli M, Di Rocco C, La Marca F (1996) Shunt complications in the first postoperative year in children with meningomyelocele. Child’s Nervous System: ChNS: Official J Int Society Pediatric Neurosurgery 12(12):748–754. https://doi.org/10.1007/BF00261592
Machado HR, Santos de Oliveira R (2004) Simultaneous repair of myelomeningocele and shunt insertion. Child’s Nervous System: ChNS: Official J Int Society Pediatric Neurosurgery 20(2):107–109. https://doi.org/10.1007/s00381-003-0853-7
Riva-Cambrin J, Kestle JR, Holubkov R, Butler J, Kulkarni AV, Drake J, Whitehead WE, Wellons JC 3rd, Shannon CN, Tamber MS et al (2016) Risk factors for shunt malfunction in pediatric hydrocephalus: a multicenter prospective cohort study. J Neurosurg Pediatr 17(4):382–390. https://doi.org/10.3171/2015.6.PEDS14670
Drake JM, Kestle JR, Milner R, Cinalli G, Boop F, Piatt J Jr, Haines S, Schiff SJ, Cochrane DD, Steinbok P et al (1998) Randomized trial of cerebrospinal fluid shunt valve design in pediatric hydrocephalus. Neurosurgery 43(2):294–303; discussion 303-295. https://doi.org/10.1097/00006123-199808000-00068
Gebert AF, Schulz M, Schwarz K, Thomale UW (2016) Long-term survival rates of gravity-assisted, adjustable differential pressure valves in infants with hydrocephalus. J Neurosurg Pediatr 17(5):544–551. https://doi.org/10.3171/2015.10.PEDS15328
Pedreira DA, Zanon N, de Sa RA, Acacio GL, Ogeda E, Belem TM, Chmait RH, Kontopoulos E, Quintero RA (2014) Fetoscopic single-layer repair of open spina bifida using a cellulose patch: preliminary clinical experience. J Maternal-Fetal & Neonatal Medicine : Official J European Association Perinatal Medicine, Federation Asia Oceania Perinatal Societies, Int Society Perinatal Obstet 27(16):1613–1619. https://doi.org/10.3109/14767058.2013.871701
Tulipan N, Wellons JC 3rd, Thom EA, Gupta N, Sutton LN, Burrows PK, Farmer D, Walsh W, Johnson MP, Rand L et al (2015) Prenatal surgery for myelomeningocele and the need for cerebrospinal fluid shunt placement. J Neurosurg Pediatr 16(6):613–620. https://doi.org/10.3171/2015.7.PEDS15336
Garabedian C, Di Rocco F, Fallet-Bianco C, Zerah M, Jouannic JM (2013) Prenatal repair of myelomeningocele: state of the art. J de Gynecologie, Obstetrique et Biologie de la Reproduction 42(3):227–231. https://doi.org/10.1016/j.jgyn.2012.10.015
Alatas I, Canaz H, Ozel K, Gedikbasi A, Kohl T (2016) Repair of spina bifida aperta with percutaneous minimal invasive fetoscopic method: first two cases in Turkey. Perinatal J 24(1):54–60. https://doi.org/10.2399/prn.16.0241010
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
There are no conflicts of interest.
Rights and permissions
About this article
Cite this article
Alatas, I., Canaz, G., Kayran, N.A. et al. Shunt revision rates in myelomeningocele patients in the first year of life: a retrospective study of 52 patients. Childs Nerv Syst 34, 919–923 (2018). https://doi.org/10.1007/s00381-017-3663-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-017-3663-z