Abstract
Purpose
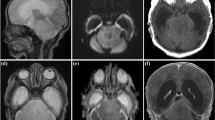
Pediatric brain stem tumors (BsT) are a heterogeneous group of diseases. Our aim was to analyze our experience to find out prognostic factors.
Method
A retrospective study with BsT patients was performed. Imaging characteristics, extension of surgery, pathology, and adjuvant therapy were analyzed and correlated with overall survival (OS) and progression-free survival (PFS) as outcome measures.
Result
Since 1980 to 2010, we analyzed 65 BsT patients, 41 of them girls (63 %), median age of 8 years (range 13.9 months to 17.6 years). Twenty-two patients (33.8 %) had diffuse intrinsic pontine gliomas (DIPG) and 43 (66.2 %) presented with focal BsT. Histology was available in 42 patients; the most frequent is low-grade glioma in 24/42 patients (57 %). DIPG’s histology (obtained usually at necropsy) confirmed five high-grade gliomas. After median follow-up of 49.3 months (0.5–175 months), 20/22 DIPG patients have died (90.9 %), while 27/43 with focal tumors were alive (62.8 %). Variables related to outcome were histology (better for low-grade glioma (LGG) OS p < 0.001), surgery (better if operated OS p < 0.001), and adjuvant therapy (worse if given, PFS p = 0.001, OS p = 0.024). The outcome for DIPG was dismal, median OS/EFS of 14.2/9.4 months, significantly worse than focal BsT (p = 0.000), while OS/EFS was 122.8/87.2 months for focal intrinsic, 88.2/47.1 months for exophytic, and 124.4/54 months for cervico–medullary tumors: no differences were found among them, except the histology (OS p < 0.001 for low-grade vs high-grade tumors).
Conclusion
BsT in children comprised two different groups: diffuse (DIPG) and focal gliomas. The DIPGs continue having a dismal prognosis, needing new approaches, while focal tumors including LGG have better prognosis.





Similar content being viewed by others
References
Albright AL, Price RA, Guthkelch AN (1983) Brain stem gliomas of children. A clinicopathological study. Cancer 52:2313–2319
Alvisi C, Cerisoli M, Maccheroni ME (1985) Long-term results of surgically treated brainstem gliomas. Acta Neurochir 76:12–17
Barkovich AJ, Krischer J, Kun LE et al (1990) Brain stem gliomas: a classification system based on magnetic resonance imaging. Pediatr Neurosurg 16:73–83
Behnke J, Christen HJ, Bruck W, Markakis E (1997) Intra-axial endophytic tumors in the pons and/ or medulla oblongata. I. Symptoms, neuroradiological findings, and histopathology in 30 children. Childs Nerv Syst 13:122–134
Bowers DC, Georgiades C, Aronson LJ et al (2000) Tectal gliomas: natural history of an indolent lesion in pediatric patients. Pediatr Neurosurg 32:24–29
Choux M, Lena G, Do L (2000) Brainstem tumors. In: Choux M, Di Rocco C, Hockley A (eds) Pediatric neurosurgery. Churchill Livingstone, New York, pp 471–491
Donaldson SS, Laningham F, Fisher PG (2006) Advances toward an understanding of brainstem gliomas. J Clin Oncol 24:1266–1272
Eipstein F, McCleary EL (1986) Intrinsic brain-stem tumors in childhood: surgical indications. J Neurooncol 6:309–317
Fischbein NJ, Prados MD, Wara W, Russo C, Edwards MS, Barkovich AJ (1996) Radiologic classification of brain stem tumors: correlation of magnetic resonance imaging appearance with clinical outcome. Pediatr Neurosurg 24:9–23
Frazier JL, Lee J, Thomale UW, Noggle JC, Cohen KJ, Jallo GI (2009) Treatment of diffuse intrinsic brainstem gliomas: failed approaches and future strategies. J Neurosurg Pediatr 3:259–269
Fried I, Hawkins C, Scheinemann K et al (2012) Favorable outcome with conservative treatment for children with low grade brainstem tumors. Pediatr Blood Cancer 58:556–560
Hoffman HJ, Becker L, Craven MA (1980) A clinically and pathologically distinct group of benign brain stem gliomas. Neurosurgery 7:243–248
Jalali R, Raut N, Arora B, Gupta T, Dutta D, Munshi A, Sarin R, Kurkure P (2010) Prospective evaluation of radiotherapy with concurrent and adjuvant temozolomide in children with newly diagnosed diffuse intrinsic pontine glioma. Int J Radiat Oncol Biol Phys 77:113–118
Jallo G, Biser-Rohrbaugh A, Freed D (2004) Brainstem gliomas. Childs NervSyst 20:143–153
Jallo G, Kothbauer K, Epstein F (2000) Surgical management of cervicomedullary and dorsally exophytic brain stem tumors. Oper Tech Neurosurg 3:131–136
Jallo GI, Freed MS, Roonprapunt C, Epstein F (2003) Current management of brainstem gliomas. Ann Neurosurg 3:1–17
Milstein JM, Geyer JR, Berger MS, Bleyer WA (1989) Favorable prognosis for brainstem gliomas in neurofibromatosis. J Neurooncol 7:367–371
Mora J, Cruz O, Gala S, Navarro R (2007) Successful treatment of childhood intramedullary spinal cord astrocytomas with irinotecan and cisplatin. Neuro Oncol 9(1):39–46
Peris-Bonet R, Felipe GS, Pardo RE et al. (2011) [Cancer in Infancy: 30th years of statistics 1980–2010. National Registry of Infancy tumors (RNTI-SEHOP)]. Valencia, Universitat de València (Prelimiar Edition in CD-ROM). (Spanish)
Pierre-Kahn A, Hirsch JF, Vinchon M et al (1993) Surgical management of brain-stem tumors in children: results and statistical analysis of 75 cases. J Neurosurg 79:845–852
Pollack IF, Hoffman HJ, Humphreys RP, Becker L (1993) The long-term outcome after surgical treatment of dorsally exophytic brain-stem gliomas. J Neurosurg 78:859–863
Pollack IF, Shultz B, Mulvihill JJ (1996) The management of brainstem gliomas in patients with neurofibromatosis 1. Neurology 46:1652–1660
Ronghe M, Hargrave D, Bartels U, Tabori U et al (2000) Vincristine and carboplatin chemotherapy for unresectable and/or recurrent low-grade astrocytoma of the brainstem. Ped Blood & Cancer 55:471–477
Ullrich NJ, Raja AI, Irons MB, Kieran MW, Goumnerova L (2007) Brainstem lesions in neurofibromatosis type 1. Neurosurgery 61:762–766
Acknowledgments
We thank all patients and their families for their trust. We are grateful to our nursing and multidisciplinary staff for their support in patient care. We thank Raquel Iniesta for her support in Statistics (Fundació Sant Joan de Déu, working under financial support from the Instituto Carlos III, contract number CA08/00151) and Daniel Cuadras, Servei d’Assessoria en Estadística.
The authors also thank the institutional Biobank “Biobanco del Hospital Materno-Infantil de San Juan de Dios para la Investigación” as part of the “Red Temática de Biobancos Hospitalarios del ISCIII”.
Financial support
This study was partially supported by a grant from the Alicia Pueyo Fund (www.fondoaliciapueyo.org).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Garzón, M., García-Fructuoso, G., Guillén, A. et al. Brain stem tumors in children and adolescents: single institutional experience. Childs Nerv Syst 29, 1321–1331 (2013). https://doi.org/10.1007/s00381-013-2137-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-013-2137-1