Abstract
Purpose
Morphine is avoided by many neurosurgeons following cranial surgery. There exists a concern regarding the potential complications and a perception that cranial surgery is less painful than other surgical procedures. At British Columbia Children’s Hospital continuous morphine infusions (CMI) have been used to control pain in pediatric neurosurgical patients. The purpose of this study was to compare the safety and efficacy of continuous intravenous morphine infusion to standard oral analgesics in a neurosurgical ward setting.
Methods
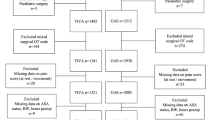
A retrospective review of medical records for 71 children was completed. The patients underwent either cranial reconstruction (2002–2007) or craniotomies for intradural pathology (2005–2007) at British Columbia Children’s Hospital. Outcome measures included pain control and adverse events. Comparison was made between patients receiving a CMI and patients receiving acetaminophen and codeine.
Results
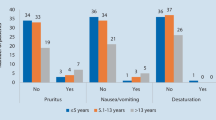
Thirty-seven children received CMI on the ward (30 cranial reconstruction and 7 craniotomy), while 34 (10 cranial reconstruction and 24 craniotomy) received acetaminophen and codeine. There was no statistical difference in pain control. There was significantly more nausea on post-operative day one in the CMI group (p = 0.002). There were no other significant adverse events.
Conclusions
These findings suggest that CMI is comparable to acetaminophen and codeine with respect to analgesia and serious side effects. We recommend the use of CMIs as an alternative when pain is poorly controlled in post-operative pediatric neurosurgical patients to prevent the potential adverse consequences of inadequate analgesia.
Similar content being viewed by others
References
Ayoub C, Girard F, Boudreault D, Chouinard P, Ruel M, Moumdjian R (2006) A comparison between scalp nerve block and morphine for transitional analgesia after remifentanil-based anesthesia in neurosurgery. Anesth Analg 103:1237–1240
Bala I, Gupta B, Bhardwaj N, Ghai B, Khosla VK (2006) Effect of scalp block on postoperative pain relief in craniotomy patients. Anaesth Intensive Care 34:224–227
Berde CB, Lehn BM, Yee JD, Sethna NF, Russo D (1991) Patient-controlled analgesia in children and adolescents: a randomized, prospective comparison with intramuscular administration of morphine for postoperative analgesia. J Pediatr 118:460–466
Biswas BK, Bithal PK (2003) Preincision 0.25% bupivacaine scalp infiltration and postcraniotomy pain: a randomized double-blind, placebo-controlled study. J Neurosurg Anesth 15:234–239
Chiaretti A, Viola L, Pietrini D, Piastra M, Savioli A, Tortorolo L, Caldarelli M, Stoppa F, Di Rocco C (2000) Preemptive analgesia with tramadol and fentanyl in pediatric neurosurgery. Childs Nerv Syst 16:93–99, discussion 100
Chiaretti A, Genovese O, Antonelli A, Tortorolo L, Ruggiero A, Focareli B, Di Rocco C (2008) Patient-controlled analgesia with fentanil and midazolam in children with postoperative neurosurgical pain. Childs Nerv Syst 24:119–124
De Benedittis G, Lorenzetti A, Migliore M, Spagnoli D, Tiberio F, Villani RM (1996) Postoperative pain in neurosurgery: a pilot study in brain surgery. Neurosurgery 38:466–469
de Gray LC, Matta BF (2005) Acute and chronic pain following craniotomy: a review. Anaesthesia 60:693–704
Dunbar PJ, Visco E, Lam AM (1999) Craniotomy procedures are associated with less analgesic requirements than other surgical procedures. Anesth Analg 88:335–340
Esmail Z, Montgomery C, Courtrn C, Hamilton D, Kestle J (1999) Efficacy and complications of morphine infusions in postoperative paediatric patients. Paediatr Anesth 9:321–327
Gottschalk A, Berkow LC, Stevens RD, Mirski M, Thompson RE, White ED, Weingart JD, Long DM, Yester M (2007) Prospective evaluation of pain and analgesic use following major elective intracranial surgery. J Neurosurg 106:210–216
Grossman R, Ram Z, Perel A, Yusim Y, Zaslansky R, Berkenstadt H (2007) Control of postoperative pain after awake craniotomy with local intradermal analgesia and metamizol. Isr Med Assoc J 9:380–382
Herbert C (2001) Use of morphine for pain after intracranial surgery. Prof Nurse 16:1029–1033
Honnma T, Imaizumi T, Chiba M, Niwa J (2002) Preemptive analgesia for postoperative pain after frontotemporal craniotomy. No Shinkei Geka 30:171–174
Kincaid MS, Lam AM (2007) Pain and the craniotomy. J Neurosurg 106:1136–1137, author reply 1137
Klimek M, Ubben JF, Ammann J, Borner U, Klein J, Verbrugge SJ (2006) Pain in neurosurgically treated patients: a prospective observational study. J Neurosurg 104:350–359
Quiney N, Cooper R, Stoneham M, Walters F (1996) Pain after craniotomy. A time for reappraisal? Br J Neurosurg 10:295–299
Rahimi SY, Vender JR, Macomson SD, French A, Smith JR, Alleyne CH Jr (2006) Postoperative pain management after craniotomy: evaluation and cost analysis. Neurosurgery 59:852–857, discussion 857
Rahimi SY, Alleyne CH, Vernier E, Witcher MR, Vender JR (2010) Postoperative pain management with tramadol after craniotomy: evaluation and cost analysis. J Neurosurg 112:268–272
Roberts G (2004) A review of the efficacy and safety of opioid analgesics post-craniotomy. Nurs Crit Care 9:277–283
Roberts GC (2005) Post-craniotomy analgesia: current practices in british neurosurgical centres—a survey of post-craniotomy analgesic practices. Eur J Anaesthesiol 22:328–332, comment 325–7
Smyth MD, Banks JT, Tubbs RS, Wellons JC 3rd, Oakes WJ (2004) Efficacy of scheduled nonnarcotic analgesic medications in children after suboccipital craniectomy. J Neurosurg 100:183–186
Verchere E, Grenier B (2004) Pain and postoperative analgesia after craniotomy. Ann Fr Anesth Reanim 23:417–421
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Warren, D.T., Bowen-Roberts, T., Ou, C. et al. Safety and efficacy of continuous morphine infusions following pediatric cranial surgery in a surgical ward setting. Childs Nerv Syst 26, 1535–1541 (2010). https://doi.org/10.1007/s00381-010-1123-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-010-1123-0