Abstract
Objective
Symptom recurrence remains a problem for some patients after surgical decompression for Chiari I malformation. We set out to identify variables at presentation that could identify subgroups most likely to experience incomplete symptom relief after hindbrain decompression for Chiari I malformation.
Materials and methods
We retrospectively reviewed the records of all pediatric patients undergoing first-time suboccipital decompression for Chiari I malformation over a 10-year period. Measured outcomes included (1) persistence or recurrence of symptoms regardless of severity and (2) need for revision decompression.
Results
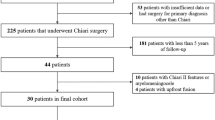
Two hundred fifty-six children (10 5years old) underwent surgery for Chiari I malformation and were followed up for a mean of 27months. Presenting symptoms included headache in 192 (75%) patients and brainstem or cranial nerve symptoms in 68 (27%) patients. Fifty-seven (22%) patients experienced mild to moderate symptom recurrence. Nineteen (7%) patients required revision decompression for significant symptom recurrence. Headache was 70% more likely to persist or recur versus cranial nerve or brainstem symptoms (relative risk 1.70, p < 0.05). Vertigo and frontal headache independently increased the odds of symptom recurrence 2.9- and 1.5-fold, respectively. Each increasing year of preoperative headache duration was independently associated with 15% increase in likelihood of symptom persistence (p < 0.05). Severe tonsilar ectopia (caudal to C2 lamina) was twice as likely to require revision decompression (14% versus 6%).
Conclusion
In our experience, recurrence of mild symptomatology not severe enough to justify revision surgery may occur in nearly a fifth of patients after surgery. Headache was more likely to recur than objective cranial nerve or brainstem symptoms. Increasing duration of headaches, frontal headaches, and vertigo may be more refractory symptoms of Chiari I malformation.


Similar content being viewed by others
References
Alzate JC, Kothbauer KF, Jallo GI, Epstein FJ (2001) Treatment of Chiari I malformation in patients with and without syringomyelia: a consecutive series of 66 cases. Neurosurg Focus 11:E3
Bindal AK, Dunsker SB, Tew JM Jr (1995) Chiari I malformation: classification and management. Neurosurgery 37:1069–1074
Cahan LD, Bentson JR (1982) Considerations in the diagnosis and treatment of syringomyelia and the Chiari malformation. J Neurosurg 57:24–31
Caldarelli M, Novegno F, Vassimi L, Romani R, Tamburrini G, Di Rocco C (2007) The role of limited posterior fossa craniectomy in the surgical treatment of Chiari malformation Type I: experience with a pediatric series. J Neurosurg 106:187–195
Chiari H (1891) Uber Veranderungen des Kleinhirns infolge von Hydrocephalie des Grosshirns [in German]. Dtsch Med Wochenschr 17:1172–1175
Dones J, De Jesus O, Colen CB, Toledo MM, Delgado M (2003) Clinical outcomes in patients with Chiari I malformation: a review of 27 cases. Surg Neurol 60:142–147 discussion 147–148
Dyste GN, Menezes AH, VanGilder JC (1989) Symptomatic Chiari malformations. An analysis of presentation, management, and long-term outcome. J Neurosurg 71:159–168
Elster AD, Chen MY (1992) Chiari I malformations: clinical and radiologic reappraisal. Radiology 183:347–353
Fagan LH, Ferguson S, Yassari R, Frim DM (2006) The Chiari pseudotumor cerebri syndrome: symptom recurrence after decompressive surgery for Chiari malformation type I. Pediatr Neurosurg 42:14–19
Levy WJ, Mason L, Hahn JF (1983) Chiari malformation presenting in adults: a surgical experience in 127 cases. Neurosurgery 12:377–390
McGirt MJ, Nimjee SM, Fuchs HE, George TM (2006) Relationship of cine phase-contrast magnetic resonance imaging with outcome after decompression for Chiari I malformations. Neurosurgery 59:140–146 discussion 140–146
Meadows J, Kraut M, Guarnieri M, Haroun RI, Carson BS (2000) Asymptomatic Chiari Type I malformations identified on magnetic resonance imaging. J Neurosurg 92:920–926
Milhorat TH, Chou MW, Trinidad EM, Kula RW, Mandell M, Wolpert C, Speer MC (1999) Chiari I malformation redefined: clinical and radiographic findings for 364 symptomatic patients. Neurosurgery 44:1005–1017
Nevo Y, Kramer U, Rieder-Groswasser I, Harel S (1994) Clinical categorization of 312 children with chronic headache. Brain Develop 16:441–444
Park JK, Gleason PL, Madsen JR, Goumnerova LC, Scott RM (1997) Presentation and management of Chiari I malformation in children. Pediatr Neurosurg 26:190–196
Paul KS, Lye RH, Strang FA, Dutton J (1983) Arnold–Chiari malformation. Review of 71 cases. J Neurosurg 58:183–187
Pillay PK, Awad IA, Little JR, Hahn JF (1991) Symptomatic Chiari malformation in adults: a new classification based on magnetic resonance imaging with clinical and prognostic significance. Neurosurgery 28:639–645
Ropper AH, Adams RD, Victor M, Brown RH, Victor M (2005) Adams and Victor’s principles of neurology. McGraw-Hill Medical, New York
Saez RJ, Onofrio BM, Yanagihara T (1976) Experience with Arnold–Chiari malformation, 1960 to 1970. J Neurosurg 45:416–422
Schwedt TJ, Guo Y, Rothner AD (2006) “Benign” imaging abnormalities in children and adolescents with headache. Headache 46:387–398
Stevens JM, Serva WA, Kendall BE, Valentine AR, Ponsford JR (1993) Chiari malformation in adults: relation of morphological aspects to clinical features and operative outcome. J Neurol Neurosurg Psychiatry 56:1072–1077
Tubbs RS, McGirt MJ, Oakes WJ (2003) Surgical experience in 130 pediatric patients with Chiari I malformations. J Neurosurg 99:291–296
Weinberg JS, Freed DL, Sadock J, Handler M, Wisoff JH, Epstein FJ (1998) Headache and Chiari I malformation in the pediatric population. Pediatr Neurosurg 29:14–18
Acknowledgment
This work was supported by the American Syringomyelia Alliance Project, Monktin Institute Fellowship.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
McGirt, M.J., Attenello, F.J., Atiba, A. et al. Symptom recurrence after suboccipital decompression for pediatric Chiari I malformation: analysis of 256 consecutive cases. Childs Nerv Syst 24, 1333–1339 (2008). https://doi.org/10.1007/s00381-008-0651-3
Received:
Revised:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-008-0651-3