Abstract
Objective
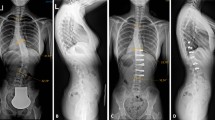
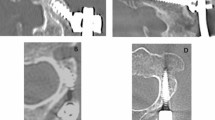
Progressive spinal deformity after cervical intramedullary spinal cord tumor (IMSCT) resection requiring subsequent fusion occurs in many cases among pediatric patients. It remains unknown which subgroups of patients represent the greatest risk for progressive spinal deformity.
Materials and methods
The data for 58 patients undergoing surgical resection of cervical IMSCT at a single institution were retrospectively collected and analyzed for development of progressive spinal deformity requiring fusion. The association of all clinical, radiographic, and operative variables to subsequent progressive spinal deformity as a function of time was assessed via Kaplan–Meier plots and Log-rank and Cox analyses.
Results
Mean age at the time of surgery was 11 ± 6years. Eleven (19%) patients required subsequent fusion for progressive spinal deformity at a median [interquartile range (IQR)] of 4 (2–6) years after IMSCT resection. Five (36%) of 14 patients with preoperative scoliosis or loss of lordosis developed postoperative progressive spinal deformity compared to only 6 (13%) of 44 patients with normal preoperative sagittal and coronal balance, p = 0.06. Patients <13years of age were more than three times more likely to develop postoperative progressive deformity, p = 0.05. Decompression spanning both the axial cervical spine (C1–C2) and the cervico–thoracic junction (C7–T1) increased the risk for progressive spinal deformity fourfold, p = 0.04. Number of spinal levels decompressed, revision surgery, radiotherapy, involvement of C1–C2 or C7–T1 alone in the decompression, or any other recorded variables were not associated with progressive postoperative spinal deformity.
Conclusion
Patients possessing one or more of these characteristics should be monitored closely for progressive spinal deformity after surgery.


Similar content being viewed by others
References
Aronson DD, Kahn RH, Canady A, Bollinger RO, Towbin R (1991) Instability of the cervical spine after decompression in patients who have Arnold-Chiari malformation. J Bone Joint Surg Am 73:898–906
Barker DJ, Weller RO, Garfield JS (1976) Epidemiology of primary tumours of the brain and spinal cord: a regional survey in southern England. J Neurol Neurosurg Psychiatry 39:290–296
Bell DF, Walker JL, O’Connor G, Tibshirani R (1994) Spinal deformity after multiple-level cervical laminectomy in children. Spine 19:406–411
Constantini S, Houten J, Miller DC, Freed D, Ozek MM, Rorke LB, Allen JC, Epstein FJ (1996) Intramedullary spinal cord tumors in children under the age of 3 years. J Neurosurg 85:1036–1043
Constantini S, Miller DC, Allen JC, Rorke LB, Freed D, Epstein FJ (2000) Radical excision of intramedullary spinal cord tumors: surgical morbidity and long-term follow-up evaluation in 164 children and young adults. J Neurosurg 93:183–193
de Jonge T, Slullitel H, Dubousset J, Miladi L, Wicart P, Illes T (2005) Late-onset spinal deformities in children treated by laminectomy and radiation therapy for malignant tumours. Eur Spine J 14:765–771
Fassett DR, Clark R, Brockmeyer DL, Schmidt MH (2006) Cervical spine deformity associated with resection of spinal cord tumors. Neurosurg Focus 20:E2
Ford DM, Bagnall KM, McFadden KD, Greenhill BJ, Raso VJ (1984) Paraspinal muscle imbalance in adolescent idiopathic scoliosis. Spine 9:373–376
Kaptain GJ, Simmons NE, Replogle RE, Pobereskin L (2000) Incidence and outcome of kyphotic deformity following laminectomy for cervical spondylotic myelopathy. J Neurosurg 93:199–204
Katsumi Y, Honma T, Nakamura T (1989) Analysis of cervical instability resulting from laminectomies for removal of spinal cord tumor. Spine 14:1171–1176
Lunardi P, Licastro G, Missori P, Ferrante L, Fortuna A (1993) Management of intramedullary tumours in children. Acta Neurochir (Wien) 120:59–65
McCormick PC, Torres R, Post KD, Stein BM (1990) Intramedullary ependymoma of the spinal cord. J Neurosurg 72:523–532
Meir AR, Fairbank JC, Jones DA, McNally DS, Urban JP (2007) High pressures and asymmetrical stresses in the scoliotic disc in the absence of muscle loading. Scoliosis 2:4
Saito T, Yamamuro T, Shikata J, Oka M, Tsutsumi S (1991) Analysis and prevention of spinal column deformity following cervical laminectomy. I. Pathogenetic analysis of postlaminectomy deformities. Spine 16:494–502
Stokes IA, Spence H, Aronsson DD, Kilmer N (1996) Mechanical modulation of vertebral body growth. Implications for scoliosis progression. Spine 21:1162–1167
Yasuoka S, Peterson HA, Laws ER Jr, MacCarty CS (1981) Pathogenesis and prophylaxis of postlaminectomy deformity of the spine after multiple level laminectomy: difference between children and adults. Neurosurgery 9:145–152
Yasuoka S, Peterson HA, MacCarty CS (1982) Incidence of spinal column deformity after multilevel laminectomy in children and adults. J Neurosurg 57:441–445
Yeh JS, Sgouros S, Walsh AR, Hockley AD (2001) Spinal sagittal malalignment following surgery for primary intramedullary tumours in children. Pediatr Neurosurg 35:318–324
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
McGirt, M.J., Chaichana, K.L., Attenello, F. et al. Spinal deformity after resection of cervical intramedullary spinal cord tumors in children. Childs Nerv Syst 24, 735–739 (2008). https://doi.org/10.1007/s00381-007-0513-4
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-007-0513-4