Abstract
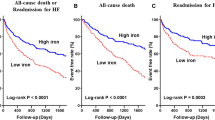
The effects of serum iron level without anemia on long-term prognosis of patients with coronary heart disease (CHD) complicated with chronic heart failure (CHF) is still unclear. The objective of this study was to explore the effects of serum iron level without anemia on long-term prognosis of patients with CHD complicated with CHF. In this retrospective cohort study, 221 patients with CHD complicated with CHF were consecutively investigated. These patients were divided into three groups according to the tertiles of the serum iron level: low-iron group (n = 71), medium-iron group (n = 76) and high-iron group (n = 74). The overall serum iron without anemia was 13.0 ± 5.50 μmol/L and serum iron in each group was 7.58 ± 1.63 μmol/L, 11.94 ± 1.79 μmol/L, and 19.37 ± 3.81 μmol/L, respectively. Composite endpoint events were composed of major adverse cardiovascular and cerebrovascular events (MACCE), including recurrent heart failure, all-cause death, acute coronary syndrome (ACS) and ischemic stroke. The median follow-up duration was 239 days. After adjusting relevant confounding risk factors, we found that excessively low or high serum iron level is correlated to the MACCE in patients with CHD complicated with CHF and that the prognosis of patients with excessively high serum iron level is poorer than that of patients with excessively low serum iron level. We further revealed the effect of serum iron level on MACCE is U-shaped, but not linear relationship. Sensitivity analysis showed that the correlation between serum iron level and MACCE is stable. In addition, according to the test for interaction, the variables that modify the effect including CRP (P for interaction < 0.0001), diuretics (P for interaction = 0.0212) and antiplatelet drugs (P for interaction = 0.0167). This study showed that excessively low or high serum iron level without anemia is an independent risk factor of MACCE in patients with CHD complicating with CHF.

Similar content being viewed by others
References
Roger VL (2013) Epidemiology of heart failure. Circ Res 113:646–659
Ponikowski P, Voors AA, Anker SD, Bueno H, Cleland JG, Coats AJ, Falk V, González-Juanatey JR, Harjola VP, Jankowska EA, Jessup M, Linde C, Nihoyannopoulos P, Parissis JT, Pieske B, Riley JP, Rosano GM, Ruilope LM, Ruschitzka F, Rutten FH, van der Meer P, Authors Task Force, Members Document Reviewers (2016) 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: the Task Force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC). Developed with the special contribution of the Heart Failure Association (HFA) of the ESC. Eur J Heart Fail 18:891–975
Mosterd A, Hoes AW (2007) Clinical epidemiology of heart failure. Heart 93:1137–1146
Wong CY, Chaudhry SI, Desai MM, Krumholz HM (2011) Trends in comorbidity, disability, and polypharmacy in heart failure. Am J Med 124:136–143
Ganz T (2013) Systemic iron homeostasis. Physiol Rev 93:1721–1741
Klip IT, Comin-Colet J, Voors AA, Ponikowski P, Enjuanes C, Banasiak W, Lok DJ, Rosentryt P, Torrens A, Polonski L, van Veldhuisen DJ, van der Meer P, Jankowska EA (2013) Iron deficiency in chronic heart failure: an international pooled analysis. Am Heart J 165:575–582.e3
Hamaguchi S, Tsuchihashi-Makaya M, Kinugawa S, Yokota T, Takeshita A, Yokoshiki H, Tsutsui H, Investigators JCARE-CARD (2009) Anemia is an independent predictor of long-term adverse outcomes in patients hospitalized with heart failure in Japan. A report from the Japanese Cardiac Registry of Heart Failure in Cardiology (JCARE-CARD). Circ J 73:1901–1908
Drozd M, Jankowska EA, Banasiak W, Ponikowski P (2017) Iron therapy in patients with heart failure and iron deficiency: review of iron preparations for practitioners. Am J Cardiovasc Drugs 17:183–201
Jankowska EA, Rozentryt P, Witkowska A, Nowak J, Hartmann O, Ponikowska B, Borodulin-Nadzieja L, Banasiak W, Polonski L, Filippatos G, McMurray JJ, Anker SD, Ponikowski P (2010) Iron deficiency: an ominous sign in patients with systolic chronic heart failure. Eur Heart J 31:1872–1880
Okonko DO, Mandal AK, Missouris CG, Poole-Wilson PA (2011) Disordered iron homeostasis in chronic heart failure: prevalence, predictors, and relation to anemia, exercise capacity, and survival. J Am Coll Cardiol 58:1241–1251
McDonagh T, Macdougall IC (2015) Iron therapy for the treatment of iron deficiency in chronic heart failure: intravenous or oral. Eur J Heart Fail 17:248–262
Lee DH, Folsom AR, Jacobs DR Jr (2005) Iron, zinc, and alcohol consumption and mortality from cardiovascular diseases: the Iowa Women’s Health Study. Am J Clin Nutr 81:787–791
Zhang W, Iso H, Ohira T, Date OC, Tanabe N, Kikuchi S, Tamakoshi A (2012) Associations of dietary iron intake with mortality from cardiovascular disease: the JACC study. J Epidemiol 22:484–493
Kaluza J, Wolk A, Larsson SC (2013) Heme iron intake and risk of stroke: a prospective study of men. Stroke 44:334–339
Ascherio A, Willett WC, Rimm EB, Giovannucci EL, Stampfer MJ (1994) Dietary iron intake and risk of coronary disease among men. Circulation 89:969–974
Kaluza J, Larsson SC, Håkansson N, Wolk A (2014) Heme iron intake and acute myocardial infarction: a prospective study of men. Int J Cardiol 172:155–160
Galan P, Vergnaud AC, Tzoulaki I, Buyck JF, Blacher J, Czernichow S, Hercberg S (2010) Low total and nonheme iron intakes are associated with a greater risk of hypertension. J Nutr 140:75–80
Nakano H, Nagai T, Sundaram V, Nakai M, Nishimura K, Honda Y, Honda S, Iwakami N, Sugano Y, Asaumi Y, Aiba T, Noguchi T, Kusano K, Yokoyama H, Ogawa H, Yasuda S, Chikamori T, Anzai T, NaDEF investigators (2018) Impact of iron deficiency on long-term clinical outcomes of hospitalized patients with heart failure. Int J Cardiol 261:114–118
Saraon T, Katz SD (2016) Targeting iron deficiency anemia in heart failure. Prog Cardiovasc Dis 58:407–415
Saeed O, Otsuka F, Polavarapu R, Karmali V, Weiss D, Davis T, Rostad B, Pachura K, Adams L, Elliott J, Taylor WR, Narula J, Kolodgie F, Virmani R, Hong CC, Finn AV (2012) Pharmacological suppression of hepcidin increases macrophage cholesterol efflux and reduces foam cell formation and atherosclerosis. Arterioscler Thromb Vasc Biol 32:299–307
Li JJ, Meng X, Si HP, Zhang C, Lv HX, Zhao YX, Yang JM, Dong M, Zhang K, Liu SX, Zhao XQ, Gao F, Liu XL, Cui TX, Zhang Y (2012) Hepcidin destabilizes atherosclerotic plaque via overactivating macrophages after erythrophagocytosis. Arterioscler Thromb Vasc Biol 32:1158–1166
Jankowska EA, von Haehling S, Anker SD, Macdougall IC, Ponikowski P (2013) Iron deficiency and heart failure: diagnostic dilemmas and therapeutic perspectives. Eur Heart J 34:816–829
van der DL A, Peeters PH, Grobbee DE, Marx JJ, van der Schouw YT (2005) Dietary haem iron and coronary heart disease in women. Eur Heart J 26:257–262
Wang Y, Wu M, Al-Rousan R, Liu H, Fannin J, Paturi S, Arvapalli RK, Katta A, Kakarla SK, Rice KM, Triest WE, Blough ER (2011) Iron-induced cardiac damage: role of apoptosis and deferasirox intervention. J Pharmacol Exp Ther 336:56–63
Munoz JP, Chiong M, García L, Troncoso R, Toro B, Pedrozo Z, Diaz-Elizondo J, Salas D, Parra V, Núñez MT, Hidalgo C, Lavandero S (2010) Iron induces protection and necrosis in cultured cardiomyocytes: role of reactive oxygen species and nitric oxide. Free Radic Biol Med 48:526–534
Fang X, Wang H, Han D, Xie E, Yang X, Wei J, Gu S, Gao F, Zhu N, Yin X, Cheng Q, Zhang P, Dai W, Chen J, Yang F, Yang HT, Linkermann A, Gu W, Min J, Wang F (2019) Ferroptosis as a target for protection against cardiomyopathy. Proc Natl Acad Sci U S A 116:2672–2680
van der Wal HH, Grote Beverborg N, Dickstein K, Anker SD, Lang CC, Ng LL, van Veldhuisen DJ, Voors AA, van der Meer P (2019) Iron deficiency in worsening heart failure is associated with reduced estimated protein intake, fluid retention, inflammation, and antiplatelet use. Eur Heart J 40:3616–3625
Acknowledgements
We would like to thank all Emergency Department colleagues for their significant contributions to this work.
Funding
There were no external funding sources for this study.
Author information
Authors and Affiliations
Contributions
JLY and SHD performed the study design, data analysis, data interpretation and manuscript drafting. YBP, YQH, WMS and RNW contributed to collect data, review the manuscript and statistical problems. YBP, WMS and RNW contributed to the study design and provided feedback on the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yan, J., Pan, Y., He, Y. et al. The effects of serum iron level without anemia on long-term prognosis of patients with coronary heart disease complicated with chronic heart failure: a retrospective cohort study. Heart Vessels 35, 1419–1428 (2020). https://doi.org/10.1007/s00380-020-01613-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00380-020-01613-0