Abstract
Purpose
We aim to evaluate the accuracy of micro-ultrasound (microUS) in predicting extraprostatic extension (EPE) of Prostate Cancer (PCa) prior to surgery.
Methods
Patients with biopsy-proven PCa scheduled for robot-assisted radical prostatectomy (RARP) were prospectively recruited. The following MRI-derived microUS features were evaluated: capsular bulging, visible breach of the prostate capsule (visible extracapsular extension; ECE), presence of hypoechoic halo, and obliteration of the vesicle-prostatic angle. The ability of each feature to predict EPE was determined.
Results
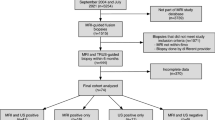
Overall, data from 140 patients were examined. All predictors were associated with non-organ-confined disease (p < 0.001). Final pathology showed that 79 patients (56.4%) had a pT2 disease and 61 (43.3%) ≥ pT3. Rate of non-organ-confined disease increased from 44% in those individuals with only 1 predictor (OR 7.71) to 92.3% in those where 4 predictors (OR 72.00) were simultaneously observed. The multivariate logistic regression model including clinical parameters showed an area under the curve (AUC) of 82.3% as compared to an AUC of 87.6% for the model including both clinical and microUS parameters. Presence of ECE at microUS predicted EPE with a sensitivity of 72.1% and a specificity of 88%, a negative predictive value of 80.5% and positive predictive value of 83.0%, with an AUC of 80.4%.
Conclusions
MicroUS can accurately predict EPE at the final pathology report in patients scheduled for RARP.

Similar content being viewed by others
Availability of data, materials, and code
Data, code, and analysis are available upon request.
References
Mottet N, Bastian P, Bellmunt J, et al (2020) EAU - EANM - ESTRO - ESUR - SIOG: Guidelines on Prostate Cancer, presented. EAU Guidelines Office, Arnhem, The Netherlands
Bjurlin MA, Carroll PR, Eggener S et al (2020) Update of the standard operating procedure on the use of multiparametric magnetic resonance imaging for the diagnosis, staging and management of prostate cancer. J Urol 203:706–712. https://doi.org/10.1097/JU.0000000000000617
Schiavina R, Bianchi L, Borghesi M et al (2018) MRI displays the prostatic cancer anatomy and improves the bundles management before robot-assisted radical prostatectomy. J Endourol 32:315–321. https://doi.org/10.1089/end.2017.0701
Herlemann A, Overland MR, Washington SL et al (2020) How often does magnetic resonance imaging detect prostate cancer missed by transrectal ultrasound? Eur Urol Focus. https://doi.org/10.1016/j.euf.2020.08.003
Zhang F, Liu C-L, Chen Q et al (2019) Accuracy of multiparametric magnetic resonance imaging for detecting extracapsular extension in prostate cancer: a systematic review and meta-analysis. Br J Radiol 92:20190480. https://doi.org/10.1259/bjr.20190480
Lughezzani G, Saita A, Lazzeri M et al (2019) Comparison of the diagnostic accuracy of micro-ultrasound and magnetic resonance imaging/ultrasound fusion targeted biopsies for the diagnosis of clinically significant prostate cancer. Eur Urol Oncol 2:329–332. https://doi.org/10.1016/j.euo.2018.10.001
Claros OR, Tourinho-Barbosa RR, Fregeville A et al (2020) Comparison of initial experience with transrectal magnetic resonance imaging cognitive guided micro-ultrasound biopsies versus established transperineal robotic ultrasound magnetic resonance imaging fusion biopsies for prostate cancer. J Urol 203:918–925. https://doi.org/10.1097/JU.0000000000000692
Laurence Klotz CM (2020) Can high resolution micro-ultrasound replace MRI in the diagnosis of prostate cancer? Eur Urol Focus 6:419–423. https://doi.org/10.1016/j.euf.2019.11.006
Rodríguez Socarrás ME, Gomez Rivas J, Cuadros Rivera V et al (2020) Prostate mapping for cancer diagnosis: the Madrid protocol. Transperineal prostate biopsies using multiparametric magnetic resonance imaging fusion and micro-ultrasound guided biopsies. J Urol 204:726–733. https://doi.org/10.1097/JU.0000000000001083
Avolio PP, Lughezzani G, Paciotti M et al (2021) The use of 29 MHz transrectal micro-ultrasound to stratify the prostate cancer risk in patients with PI-RADS III lesions at multiparametric MRI: a single institutional analysis. Urol Oncol Semin Orig Investig. https://doi.org/10.1016/j.urolonc.2021.05.030
Ghai S, Eure G, Fradet V et al (2016) Assessing cancer risk on novel 29 MHz micro-ultrasound images of the prostate: creation of the micro-ultrasound protocol for prostate risk identification. J Urol 196:562–569. https://doi.org/10.1016/j.juro.2015.12.093
Mehralivand S, Shih JH, Harmon S et al (2019) A grading system for the assessment of risk of extraprostatic extension of prostate cancer at multiparametric MRI. Radiology 290:709–719. https://doi.org/10.1148/radiol.2018181278
Staerman F (2019) Can high resolution micro-ultrasound detect extra-prostatic extension? Eur Urol Suppl 18:e3389. https://doi.org/10.1016/S1569-9056(19)34491-4
van Leenders GJLH, van der Kwast TH, Grignon DJ, et al (2020) The 2019 International society of urological pathology (ISUP) consensus conference on grading of prostatic carcinoma. Am J Surg Pathol 44:e87–e99. https://doi.org/10.1097/PAS.0000000000001497
James D. Brierley (Editor), Mary K. Gospodarowicz (Editor) CW (Editor) (2017) TNM Classification of Malignant Tumours, 8th Edition
Ahmed HU, El-Shater Bosaily A, Brown LC et al (2017) Diagnostic accuracy of multi-parametric MRI and TRUS biopsy in prostate cancer (PROMIS): a paired validating confirmatory study. Lancet (London, England) 389:815–822. https://doi.org/10.1016/S0140-6736(16)32401-1
de Rooij M, Hamoen EHJ, Witjes JA et al (2016) Accuracy of magnetic resonance imaging for local staging of prostate cancer: a diagnostic meta-analysis. Eur Urol 70:233–245. https://doi.org/10.1016/j.eururo.2015.07.029
Feng TS, Sharif-Afshar AR, Wu J et al (2015) Multiparametric MRI improves accuracy of clinical nomograms for predicting extracapsular extension of prostate cancer. Urology 86:332–337. https://doi.org/10.1016/j.urology.2015.06.003
Rayn KN, Bloom JB, Gold SA et al (2018) Added value of multiparametric magnetic resonance imaging to clinical nomograms for predicting adverse pathology in prostate cancer. J Urol 200:1041–1047. https://doi.org/10.1016/j.juro.2018.05.094
Diamand R, Ploussard G, Roumiguié M et al (2021) External validation of a multiparametric magnetic resonance imaging–based nomogram for the prediction of extracapsular extension and seminal vesicle invasion in prostate cancer patients undergoing radical prostatectomy. Eur Urol 79:180–185. https://doi.org/10.1016/j.eururo.2020.09.037
Somford DM, Hamoen EH, Fütterer JJ et al (2013) The predictive value of endorectal 3 tesla multiparametric magnetic resonance imaging for extraprostatic extension in patients with low, intermediate and high risk prostate cancer. J Urol 190:1728–1734. https://doi.org/10.1016/j.juro.2013.05.021
Kam J, Yuminaga Y, Krelle M et al (2019) Evaluation of the accuracy of multiparametric MRI for predicting prostate cancer pathology and tumour staging in the real world: an multicentre study. BJU Int 124:297–301. https://doi.org/10.1111/bju.14696
Regis F, Casale P, Persico F et al (2020) Use of 29-MHz micro-ultrasound for local staging of prostate cancer in patients scheduled for radical prostatectomy: a feasibility study. Eur Urol Open Sci 19:20–23. https://doi.org/10.1016/j.euros.2020.05.002
Rosenkrantz AB, Shanbhogue AK, Wang A et al (2016) Length of capsular contact for diagnosing extraprostatic extension on prostate MRI: assessment at an optimal threshold. J Magn Reson Imaging 43:990–997. https://doi.org/10.1002/jmri.25040
Washino S, Okochi T, Saito K et al (2017) Combination of prostate imaging reporting and data system (PI-RADS) score and prostate-specific antigen (PSA) density predicts biopsy outcome in prostate biopsy naïve patients. BJU Int 119:225–233. https://doi.org/10.1111/bju.13465
Sountoulides P, Pyrgidis N, Polyzos SA et al (2021) Micro-ultrasound–guided vs multiparametric magnetic resonance imaging-targeted biopsy in the detection of prostate cancer: a systematic review and meta-analysis. J Urol 205:1254–1262. https://doi.org/10.1097/JU.0000000000001639
Lopci E, Lughezzani G, Castello A et al (2021) PSMA-PET and micro-ultrasound potential in the diagnostic pathway of prostate cancer. Clin Transl Oncol 23:172–178. https://doi.org/10.1007/s12094-020-02384-w
Fossati N, Buffi NM, Haese A et al (2015) Preoperative prostate-specific antigen isoform p2PSA and its derivatives, %p2PSA and prostate health index, predict pathologic outcomes in patients undergoing radical prostatectomy for prostate cancer: results from a multicentric European prospective study. Eur Urol 68:132–138. https://doi.org/10.1016/j.eururo.2014.07.034
Guazzoni G, Lazzeri M, Nava L et al (2012) Preoperative prostate-specific antigen isoform p2PSA and its derivatives, %p2PSA and prostate health index, predict pathologic outcomes in patients undergoing radical prostatectomy for prostate cancer. Eur Urol 61:455–466. https://doi.org/10.1016/j.eururo.2011.10.038
de la Calle CM, Fasulo V, Cowan JE et al (2021) Clinical utility of 4Kscore ®, ExosomeDxTM and magnetic resonance imaging for the early detection of high grade prostate cancer. J Urol 205:452–460. https://doi.org/10.1097/JU.0000000000001361
Funding
The authors did not receive support from any organization for the submitted work.
Author information
Authors and Affiliations
Contributions
VF: data collection or management, data analysis, manuscript writing/editing, protocol/project development. NMB: protocol/project development, manuscript writing/editing. FR: data collection or management, Manuscript writing/editing. MP: data collection or management, data analysis, manuscript writing/editing, Protocol/project development. FP: data collection or management, manuscript writing/editing. DM: data collection or management, Manuscript writing/editing. AU: data collection or management, manuscript writing/editing. AS: data collection or management, manuscript writing/editing. PC: data collection or management, manuscript writing/editing. RH: data collection or management, manuscript writing/editing. ML: data collection or management, manuscript writing/editing. GG: Data collection or management, manuscript writing/editing. GL: data collection or management, data analysis, manuscript writing/editing, protocol/project development.
Corresponding author
Ethics declarations
Conflicts of interest
The authors have no relevant financial or non-financial interests to disclose.
Research involving human participants, their data or biological material
The study was approved by local authorities (Prot.n°2570-ICH-006) and all patients signed a written informed consent before enrollment.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
345_2021_3890_MOESM1_ESM.tiff
Supplementary file1 (TIFF 1521 KB) Figure depicting a PRIMUS 5 mixed-echo lesion on the right lateral aspect of the prostate with associated hypoechoic halo (orange arrows) and capsular bulging. Needle biopsy tracks con also be observed as hyperechoic lines
345_2021_3890_MOESM2_ESM.tiff
Supplementary file2 (TIFF 1521 KB) Figure depicting a PRIMUS 5 mixed-echo lesion on the left lateral aspect of the prostate with associated hypoechoic halo (orange arrows)

345_2021_3890_MOESM5_ESM.docx
Supplementary file5 (DOCX 16 KB) Logistic regression univariate analysis and multivariate analysis of predictors and clinical risk factors
345_2021_3890_MOESM6_ESM.pdf
Supplementary file6 (PDF 75 KB) Diagnostic accuracy represented as the Area under the ROC curve, for two multivariate logistic regression model (MLRM) tested as clinical model alone, compared with a clinical added with the microUS parameters. represented teas the Area under the ROC curve. Outcome= non-organ-confined disease at final pathology report; dependent variables (clinical model)=total PSA, DRE, ISUP at biopsy, PRI-MUS; dependent variables (clinical + microUS predictors): clinical + visible ECE, capsular bulge, hypoechoic halo or ring at microUS
Rights and permissions
About this article
Cite this article
Fasulo, V., Buffi, N.M., Regis, F. et al. Use of high-resolution micro-ultrasound to predict extraprostatic extension of prostate cancer prior to surgery: a prospective single-institutional study. World J Urol 40, 435–442 (2022). https://doi.org/10.1007/s00345-021-03890-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-021-03890-4