Abstract
Purpose
Robotic radical prostatectomy focuses on oncologic cure, urinary continence and sexual function recovery. However, little is known about the effect of declines in urinary continence and sexual function on healthcare utilization. We aim to identify these factors.
Materials and methods
From March 2011 to September 2013, all men undergoing robotic prostatectomy within our healthcare system were enrolled. Men completed the expanded prostate cancer index composite-26 survey at the time of diagnosis and 90 days post-operatively. Patients were stratified according to change in scores in the sexual function and urinary incontinence domains. Patient, treatment and post-op utilization patterns were examined for association with the extent of decline in sexual function and urinary continence. Multivariate linear regression was used to identify factors independently associated with decline in continence and sexual function.
Results
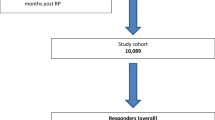
A total of 411 men who completed the baseline survey and at 90 days postoperatively were included. On multivariate linear regression, younger age (p < 0.01), higher preoperative sexual function (< 0.01), single marital status (p = 0.04) and more post-surgery email contacts (p = 0.04) were associated with higher declines in sexual function. For continence, no family history of prostate cancer (p = 0.01), higher baseline continence (p < 0.01) and more post-surgery physical therapy visits (p < 0.01) were associated with higher declines.
Conclusions
Patients with the poorest quality of life outcomes at 90 days post-operatively were more likely to seek care via email and physical therapy encounters related to sexual function and urinary incontinence, respectively. This suggests that maximizing post-treatment quality of life can potentially reduce healthcare utilization.
Similar content being viewed by others
Abbreviations
- US:
-
United States
- PCa:
-
Prostate cancer
- RALP:
-
Robotic-assisted robotic prostatectomy
- HRQOL:
-
Healthcare-related quality of life
- UI:
-
Urinary incontinence
- SF:
-
Sexual function
- KPSC:
-
Kaiser Permanente Southern California
- EPIC-26:
-
Expanded Prostate Cancer Index composite 26
- BMI:
-
Body mass index
- CCI:
-
Charlson Comorbidity Index
- PDE5i:
-
Phosphodiesterase-5
- EBL:
-
Estimated blood loss
References
Porter ME (2010) What is value in health care? N Engl J Med 363(26):2477–2481. https://doi.org/10.1056/NEJMp1011024
Kural AR, Obek C, Doganca T (2017) Can we accomplish better oncological results with robot-assisted radical prostatectomy? J Endourol 31(S1):S54–S58. https://doi.org/10.1089/end.2016.0585
Borregales LD, Berg WT, Tal O, Wambi C, Kaufman S, Gaya JM, Urzua C, Badani KK (2013) ‘Trifecta’ after radical prostatectomy: is there a standard definition? BJU Int 112(1):60–67. https://doi.org/10.1111/bju.12002
Hamdy FC, Donovan JL, Lane JA, Mason M, Metcalfe C, Holding P, Davis M, Peters TJ, Turner EL, Martin RM, Oxley J, Robinson M, Staffurth J, Walsh E, Bollina P, Catto J, Doble A, Doherty A, Gillatt D, Kockelbergh R, Kynaston H, Paul A, Powell P, Prescott S, Rosario DJ, Rowe E, Neal DE, Protec TSG (2016) 10-Year outcomes after monitoring, surgery, or radiotherapy for localized prostate cancer. N Engl J Med 375(15):1415–1424. https://doi.org/10.1056/NEJMoa1606220
Wei JT, Dunn RL, Litwin MS, Sandler HM, Sanda MG (2000) Development and validation of the expanded prostate cancer index composite (EPIC) for comprehensive assessment of health-related quality of life in men with prostate cancer. Urology 56(6):899–905
Mabry C (2008) The global surgical package–let’s get the facts straight. J Trauma 64(2):385–387. https://doi.org/10.1097/TA.0b013e318166e8f4 (discussion 388-9)
Mariotto AB, Yabroff KR, Shao Y, Feuer EJ, Brown ML (2011) Projections of the cost of cancer care in the United States: 2010–2020. J Natl Cancer Inst 103(2):117–128. https://doi.org/10.1093/jnci/djq495
Miller DC, Murtagh DS, Suh RS, Knapp PM, Dunn RL, Montie JE (2010) Establishment of a urological surgery quality collaborative. J Urol 184(6):2485–2490. https://doi.org/10.1016/j.juro.2010.08.015
Chien GW, Slezak JM, Harrison TN, Jung H, Gelfond JS, Zhang C, Wu E, Contreras R, Loo RK, Jacobsen SJ (2017) Health-related quality of life outcomes from a contemporary prostate cancer registry in a large diverse population. BJU Int. https://doi.org/10.1111/bju.13843
Punnen S, Cowan JE, Chan JM, Carroll PR, Cooperberg MR (2015) Long-term health-related quality of life after primary treatment for localized prostate cancer: results from the CaPSURE registry. Eur Urol 68(4):600–608. https://doi.org/10.1016/j.eururo.2014.08.074
Mols F, Coebergh JW, van de Poll-Franse LV (2007) Health-related quality of life and health care utilisation among older long-term cancer survivors: a population-based study. Eur J Cancer 43(15):2211–2221. https://doi.org/10.1016/j.ejca.2007.06.022
McKay R, Haider B, Duh MS, Valderrama A, Nakabayashi M, Fiorillo M, Ristovska L, Wen L, Kantoff P (2017) Impact of symptomatic skeletal events on health-care resource utilization and quality of life among patients with castration-resistant prostate cancer and bone metastases. Prostate Cancer Prostatic Dis. https://doi.org/10.1038/pcan.2017.4
Johanson R (2017) Interview with KPSC Billing Department on Cost of Physical Therapy Visits
Kazley AS, Simpson AN, Simpson KN, Teufel R (2014) Association of electronic health records with cost savings in a national sample. Am J Manag Care 20(6):e183–e190
Reed M, Graetz I, Gordon N, Fung V (2015) Patient-initiated e-mails to providers: associations with out-of-pocket visit costs, and impact on care-seeking and health. Am J Manag Care 21(12):e632–e639
Bergmo TS, Kummervold PE, Gammon D, Dahl LB (2005) Electronic patient-provider communication: will it offset office visits and telephone consultations in primary care? Int J Med Inform 74(9):705–710. https://doi.org/10.1016/j.ijmedinf.2005.06.002
Shanafelt TD, Dyrbye LN, Sinsky C, Hasan O, Satele D, Sloan J, West CP (2016) Relationship between clerical burden and characteristics of the electronic environment with physician burnout and professional satisfaction. Mayo Clin Proc 91(7):836–848. https://doi.org/10.1016/j.mayocp.2016.05.007
Friedberg MW, Chen PG, Van Busum KR, Aunon F, Pham C, Caloyeras J, Mattke S, Pitchforth E, Quigley DD, Brook RH, Crosson FJ, Tutty M (2014) Factors affecting physician professional satisfaction and their implications for patient care, health systems, and health policy. Rand Health Q 3(4):1
Arndt BG, Beasley JW, Watkinson MD, Temte JL, Tuan WJ, Sinsky CA, Gilchrist VJ (2017) Tethered to the EHR: primary care physician workload assessment using EHR event log data and time-motion observations. Ann Fam Med. 15(5):419–426. https://doi.org/10.1370/afm.2121
Hampson LA, Cowan JE, Zhao S, Carroll PR (2015) Cooperberg MR (2015) Impact of age on quality-of-life outcomes after treatment for localized prostate cancer. Eur Urol 68(3):480–486. https://doi.org/10.1016/j.eururo.2015.01.008
Deveci S, Gotto GT, Alex B, O’Brien K, Mulhall JP (2016) A survey of patient expectations regarding sexual function following radical prostatectomy. BJU Int 118(4):641–645. https://doi.org/10.1111/bju.13398
Schroeck FR, Krupski TL, Sun L, Albala DM, Price MM, Polascik TJ, Robertson CN, Tewari AK, Moul JW (2008) Satisfaction and regret after open retropubic or robot-assisted laparoscopic radical prostatectomy. Eur Urol 54(4):785–793. https://doi.org/10.1016/j.eururo.2008.06.063
Author information
Authors and Affiliations
Contributions
PA Elliott: Data collection, manuscript writing/editing. GA Abdelsayed: Data collection, manuscript writing/editing. PS Kilday: Data collection, manuscript writing/editing. BJ Kim: Data collection and management. JN Slezak: Data analysis. GW Chien: Research question, design, data analysis, interpretation, manuscript writing/editing.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Human and animal participation
This article does not contain any studies with animals performed by any of the authors.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Elliott, P.A., Abdelsayed, G.A., Kilday, P.S. et al. Healthcare utilization in men with poorer sexual and urinary function recovery following robot-assisted radical prostatectomy. World J Urol 36, 21–26 (2018). https://doi.org/10.1007/s00345-017-2112-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-017-2112-7