Abstract
Purpose
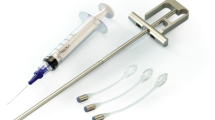
(1) To describe the minimally invasive adjustable continence therapy (ACT)® balloon placement surgical technique. (2) To analyse the results of ACT® balloon in the treatment for female stress urinary incontinence (SUI).
Method
A review of the literature was performed by searching the PubMed database using the following search terms: ACT balloons, female urinary incontinence, and female continence.
Results
Eight studies were published between 2007 and 2013. The mean follow-up of these studies was 1–6 years. The mean age of the patients ranged between 62 and 73 years; 40–100 % of patients had already been treated surgically for their SUI. A significant reduction in the number of pads used per day was observed after ACT® balloon placement, with improvement of short pad tests from 49.6 to 77.3 g preoperatively to 11.2–25.7 g after ACT® balloon placement. Fifteen to 44 % of patients considered that their SUI had been cured and 66–78.4 % were satisfied with the result. The explantation rate ranged between 18.7 and 30.8 %. Quality of life was significantly improved, and no major complication was reported.
Conclusion
ACT® balloons constitute a reasonable, minimally invasive alternative for the treatment for female SUI due to intrinsic sphincter disorder, especially in patients who have already experienced failure of standard surgical treatment and in clinical settings incompatible with invasive surgical placement of an artificial urinary sphincter (especially women over the age of 80 years). Long-term results are essential to evaluate the efficacy of this treatment.


Similar content being viewed by others
References
Abrams P, Cardozo L, Fall M, Griffiths D, Rosier P, Ulmsten U et al (2003) The standardisation of terminology in lower urinary tract function: report from the standardisation sub-committee of the International Continence Society. Urology 61(1):37–49
Reynolds WS, Dmochowski RR, Penson DF (2011) Epidemiology of stress urinary incontinence in women. Curr Urol Rep 12(5):370–376
Chartier-Kastler E, Van Kerrebroeck P, Olianas R, Cosson M, Mandron E, Delorme E et al (2011) Artificial urinary sphincter (AMS 800) implantation for women with intrinsic sphincter deficiency: a technique for insiders? BJU Int 107(10):1618–1626
Costa P, Poinas G, Ben Naoum K, Bouzoubaa K, Wagner L, Soustelle L et al (2013) Long-term results of artificial urinary sphincter for women with type III stress urinary incontinence. Eur Urol 63(4):753–758. doi:10.1016/j.eururo.2012.03.008
Vidart A, Cour F (2010) Guidelines for the treatment of non-neurological urinary incontinence in women using periurethral balloons. Prog Urol 20(Suppl 2):S150–S154
Novara G, Artibani W, Barber MD, Chapple CR, Costantini E, Ficarra V et al (2010) Updated systematic review and meta-analysis of the comparative data on colposuspensions, pubovaginal slings, and midurethral tapes in the surgical treatment of female stress urinary incontinence. Eur Urol 58(2):218–238
Lebret T, Cour F, Benchetrit J, Grise P, Bernstein J, Delaporte V et al (2008) Treatment of postprostatectomy stress urinary incontinence using a minimally invasive adjustable continence balloon device, ProACT: results of a preliminary, multicenter, pilot study. Urology 71(2):256–260
Mehnert U, Bastien L, Denys P, Cardot V, Even-Schneider A, Kocer S et al (2012) Treatment of neurogenic stress urinary incontinence using an adjustable continence device: 4-Year followup. J Urol 188(6):2274–2280
Chartier-Kastler E, Costa P, Ben Naoum K, Cour F, Le Normand L, Haab F (2007) French multicentre prospective study of the use of ACT balloons (Uromedica, Inc., Plymouth, Min, USA; Medtronic, Minneapolis, USA) for the treatment of female stress urinary incontinence. Prog Urol 17(7):1372–1377
Vayleux B, Luyckx F, Thélu S, Rigaud J, Bouchot O, Karam G et al (2010) Adjustable continence therapy in women, middle term follow-up and a new technique for balloon positioning. Prog Urol 20(7):520–526
Aboseif SR, Franke EI, Nash SD, Slutsky JN, Baum NH, Tu LM et al (2009) The adjustable continence therapy system for recurrent female stress urinary Incontinence: 1-year results of the North America clinical study group. J Urol 181(5):2187–2191
Aboseif S, Sassani P, Franke E, Nash S, Slutsky J, Baum N et al (2011) Treatment of moderate to severe female stress urinary incontinence with the adjustable continence therapy (ACT) device after failed surgical repair. World J Urol 29(2):249–253
Kocjancic E, Crivellaro S, Smith JJ 3rd, Ranzoni S, Bonvini D, Frea B (2008) Adjustable continence therapy for treatment of recurrent female urinary incontinence. J Endourol 22(7):1403–1407
Kocjancic E, Crivellaro S, Ranzoni S, Bonvini D, Grosseti B, Frea B (2010) Adjustable continence therapy for severe intrinsic sphincter deficiency and recurrent female stress urinary incontinence: long-term experience. J Urol 184(3):1017–1021
Wachter J, Henning A, Roehlich M, Marszalek M, Rauchenwald M, Madersbacher S (2008) Adjustable continence therapy for female urinary incontinence: a minimally invasive option for difficult cases. Urol Int 81(2):160–166
Lucas MG, Bosch RJL, Burkhard FC, Cruz F, Madden TB, Nambiar AK et al (2012) EAU guidelines on surgical treatment of urinary incontinence. Eur Urol 62(6):1118–1129
Hermieu J-F, Conquy S, Leriche B, Debodinance P, Delorme E, Boccon Gibod L et al (2010) Synthesis of the guidelines for the treatment of non-neurological urinary incontinence in women. Prog Urol 20(Suppl 2):S94–S99
Nacir M, Ballanger P, Donon L, Bernhard J-C, Douard A, Marit-Ducamp E et al (2013) ACT device: what place in the treatment of female urinary incontinence? Prog Urol 23(4):276–282
Gregori A, Romanò AL, Scieri F, Pietrantuono F, Incarbone GP, Salvaggio A et al (2010) Transrectal ultrasound–guided implantation of adjustable continence therapy (ProACT): surgical technique and clinical results after a mean follow-up of 2 years. Eur Urol 57(3):430–436
Rouprêt M, Misraï V, Gosseine P-N, Bart S, Cour F, Chartier-Kastler E (2011) Management of stress urinary incontinence following prostate surgery with minimally invasive adjustable continence balloon implants: functional results from a single center prospective study. J Urol 186(1):198–203
Chapple CR, Wein AJ, Brubaker L, Dmochowski R, Pons ME, Haab F et al (2005) Stress incontinence injection therapy: what is best for our patients? Eur Urol 48(4):552–565
Van Kerrebroeck P (2006) The motion: injectables are justified as a first option for stress urinary incontinence. Eur Urol 50(4):857–858 discussion 860
Corcos J, Fournier C (1999) Periurethral collagen injection for the treatment of female stress urinary incontinence: 4-year follow-up results. Urology 54(5):815–818
Nilsson CG, Palva K, Rezapour M, Falconer C (2008) Eleven years prospective follow-up of the tension-free vaginal tape procedure for treatment of stress urinary incontinence. Int Urogynecol J Pelvic Floor Dysfunct 19(8):1043–1047
Bullock TL, Ghoniem G, Klutke CG, Staskin DR (2006) Advances in female stress urinary incontinence: mid-urethral slings. BJU Int 98(Suppl 1):32–40 discussion 41–42
Lapitan MCM, Cody JD, Grant A (1996) Open retropubic colposuspension for urinary incontinence in women. In: Cochrane database of systematic reviews [Internet]. Wiley. Available on http://onlinelibrary.wiley.com.accesdistant.upmc.fr/doi/10.1002/14651858.CD002912.pub2/abstract
Norton P, Brubaker L (2006) Urinary incontinence in women. Lancet 367(9504):57–67
Bezerra CC, Bruschini H, Cody JD (1996) Traditional suburethral sling operations for urinary incontinence in women. In: Cochrane database of systematic reviews [Internet]. Wiley. Available on http://onlinelibrary.wiley.com.accesdistant.upmc.fr/doi/10.1002/14651858.CD001754.pub2/abstract
Wadie BS, Edwan A, Nabeeh AM (2005) Autologous fascial sling vs polypropylene tape at short-term follow up: a prospective randomized study. J Urol 174(3):990–993
Bai SW, Sohn WH, Chung DJ, Park JH, Kim SK (2005) Comparison of the efficacy of Burch colposuspension, pubovaginal sling, and tension-free vaginal tape for stress urinary incontinence. Int J Gynecol Obstet 91(3):246–251
Phé V, Rouprêt M, Mozer P, Chartier-Kastler E (2013) Trends in the landscape of artificial urinary sphincter implantation in men and women in France over the past decade. Eur Urol 63(2):407–408. doi:10.1016/j.eururo.2012.10.040
Vayleux B, Rigaud J, Luyckx F, Karam G, Glémain P, Bouchot O et al (2011) Female urinary incontinence and artificial urinary sphincter: study of efficacy and risk factors for failure and complications. Eur Urol 59(6):1048–1053
Revaux A, Rouprêt M, Seringe E, Misraï V, Cour F, Chartier-Kastler E (2011) Is the implantation of an artificial urinary sphincter with a large cuff in women with severe urinary incontinence associated with worse perioperative complications and functional outcomes than usual? Int Urogynecol J 22(10):1319–1324
Roupret M, Chartier-Kastler E, Richard F (2005) Artificial urinary sphincters in women: indications, techniques, results. Prog Urol 15(3):489–493
Chung E, Cartmill RA (2010) 25-year experience in the outcome of artificial urinary sphincter in the treatment of female urinary incontinence. BJU Int 106(11):1664–1667
Petero VG Jr, Diokno AC (2006) Comparison of the long-term outcomes between incontinent men and women treated with artificial urinary sphincter. J Urol 175(2):605–609
Chung E, Navaratnam A, Cartmill R (2011) Can artificial urinary sphincter be an effective salvage option in women following failed anti-incontinence surgery? Int Urogynecol J 22(3):363–366
Thomas K, Venn SN, Mundy AR (2002) Outcome of the artificial urinary sphincter in female patients. J Urol 167(4):1720–1722
Venn SN, Greenwell TJ, Mundy AR (2000) The long-term outcome of artificial urinary sphincters. J Urol 164(3, Part 1):702–707
Diokno AC, Hollander JB, Alderson TP (1987) Artificial urinary sphincter for recurrent female urinary incontinence: indications and results. J Urol 138(4):778–780
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Phé, V., Nguyen, K., Rouprêt, M. et al. A systematic review of the treatment for female stress urinary incontinence by ACT® balloon placement (Uromedica, Irvine, CA, USA). World J Urol 32, 495–505 (2014). https://doi.org/10.1007/s00345-013-1117-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-013-1117-0