Abstract
Objectives
To evaluate the influence of different biopsy forcipes on the deflection, irrigant flow, and optical characteristics of flexible ureterorenoscopes and to assess tissue quality for histopathologic evaluation in an ex vivo setting.
Materials and methods
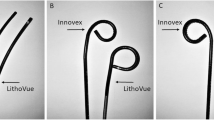
The following five different biopsy forcipes were compared: Olympus (FB-56D-1; diameter 5Fr.), R. Wolf (829.601; 3Fr.), Karl Storz Medical (11275ZE; 3Fr.), Boston Scientific (Piranha; 505-160; 3 Fr.), and Cook BIGopsy (115CM; 2.4 Fr.). The devices were tested in 3 different ureterorenoscopes: Storz 11278 VU (Flex-X2), Storz 11278 V (Flex-XC), and Wolf Cobra (7326071/-6). Tissue samples were obtained from porcine upper urinary tracts.
Results
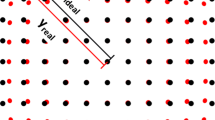
Baseline irrigation flow rates with empty channels were significantly higher in the Wolf Cobra than in Storz ureterorenoscopes (30.5 vs. 23 and 21 ml/min). The BIGopsy forceps allowed for higher flow rates in both Storz ureterorenoscopes (2.2 and 1.3, respectively) when compared to the other devices (0.5 and 0.6 ml/min). The Storz and Wolf biopsy forcipes resulted in the highest impairment of the deflection angle. In all 3 ureterorenoscopes, flow rates and deflection angle were least impaired by the BIGopsy. However, BIGopsy compromised the field of view (20 % reduction vs. 12 % by others). The largest sample of renal pelvis and ureter biopsies was obtained with BIGopsy and Storz® forcipes, respectively. The extent of artifacts and denuded urothelium were comparable in all samples.
Conclusions
The various biopsy devices showed different impacts on irrigation flow, deflection, and field of view. The Cook BIGopsy best retains irrigation flow in single-channel flexible ureterorenoscopes and deflection. However, a smaller field of view may complicate handling and tissue acquisition.


Similar content being viewed by others
References
Jemal A, Siegel R, Xu J, Ward E (2010) Cancer statistics. CA Cancer J Clin 60:277–300
Roupret M, Zigeuner R, Palou J, et al. (2011) European guidelines for the diagnosis and management of upper urinary tract urothelial cell carcinomas. Eur Urol 59:584–594
Elliott DS, Segura JW, Lightner D, Patterson DE, Blute ML (2001) Is nephroureterectomy necessary in all cases of upper tract transitional cell carcinoma? Long-term results of conservative endourologic management of upper tract transitional cell carcinoma in individuals with a normal contralateral kidney. Urology 58:174–178
McCoy JG, Honda H, Reznicek M, Williams RD (1991) Computerized tomography for detection and staging of localized and pathologically defined upper tract urothelial tumors. J Urol 146:1500–1503
Shiraishi K, Eguchi S, Mohri J, Kamiryo Y (2003) Role of ureteroscopic biopsy in the management of upper urinary tract malignancy. Int J Urol 10:627–630
Guarnizo E, Pavlovich CP, Seiba M, Carlson DL, Vaughan ED Jr, Sosa RE (2000) Ureteroscopic biopsy of upper tract urothelial carcinoma: improved diagnostic accuracy and histopathological considerations using a multi-biopsy approach. J Urol 163:52–55
Williams SK, Denton KJ, Minervini A et al (2008) Correlation of upper-tract cytology, retrograde pyelography, ureteroscopic appearance, and ureteroscopic biopsy with histologic examination of upper-tract transitional cell carcinoma. J Endourol 22:71–76
Michel MS, Knoll T, Ptaschnyk T, Kohrmann KU, Alken P (2002) Flexible ureterorenoscopy for the treatment of lower pole calyx stones: influence of different lithotripsy probes and stone extraction tools on scope deflection and irrigation flow. Eur Urol 41:312–316 (discussion 6–7)
Keeley FX, Kulp DA, Bibbo M, McCue PA, Bagley DH (1997) Diagnostic accuracy of ureteroscopic biopsy in upper tract transitional cell carcinoma. J Urol 157:33–37
Renshaw AA (2006) Comparison of ureteral washing and biopsy specimens in the community setting. Cancer 108:45–48
El-Hakim A, Weiss GH, Lee BR, Smith AD (2004) Correlation of ureteroscopic appearance with histologic grade of upper tract transitional cell carcinoma. Urology 63:647–650 (discussion 50)
Smith AK, Stephenson AJ, Lane BR et al (2011) Inadequacy of biopsy for diagnosis of upper tract urothelial carcinoma: implications for conservative management. Urology 78:82–86
Pasqui F, Dubosq F, Tchala K et al (2004) Impact on active scope deflection and irrigation flow of all endoscopic working tools during flexible ureteroscopy. Eur Urol 45:58–64
Paffen ML, Keizer JG, de Winter GV, Arends AJ, Hendrikx AJ (2008) A comparison of the physical properties of four new generation flexible ureteroscopes: (de)flection, flow properties, torsion stiffness, and optical characteristics. J Endourol 22:2227–2234
Gorin MA, Santos Cortes JA, Kyle CC, Carey RI, Bird VG (2011) Initial clinical experience with use of ureteral access sheaths in the diagnosis and treatment of upper tract urothelial carcinoma. Urology 78(3):523–527
Blew BD, Dagnone AJ, Pace KT, Honey RJ (2005) Comparison of Peditrol irrigation device and common methods of irrigation. J Endourol 19:562–565
Marquez J, Lee C, Anderson JK, Slaton J, Monga M (2005) Temperature activated deflection of a novel ureteroscopic laser fiber sheath. J Urol 173:131–134
Haberman K, Ortiz O, Chotikawanich E, Monga M (2011) A dual-channel flexible ureteroscope: evaluation of deflection, flow, illumination, and optics. J Endourol 25(9):1411–1414
Bach T, Netsch C, Herrmann TR, Gross AJ (2011) Objective assessment of working tool impact on irrigation flow and visibility in flexible ureterorenoscopes. J Endourol 25:1125–1129
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
M. Ritter and C. Bolenz contributed equally to this paper.
Rights and permissions
About this article
Cite this article
Ritter, M., Bolenz, C., Bach, T. et al. Standardized ex vivo comparison of different upper urinary tract biopsy devices: impact on ureterorenoscopes and tissue quality. World J Urol 31, 907–912 (2013). https://doi.org/10.1007/s00345-012-0854-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-012-0854-9