Abstract
Objectives
After an acute ischemic stroke, patients with a large CT perfusion (CTP) predicted infarct core (pIC) have poor clinical outcome. However, previous research suggests that this relationship may be relevant for subgroups of patients determined by pretreatment and treatment-related variables while negligible for others. We aimed to identify these variables.
Methods
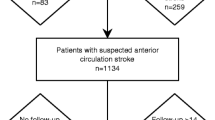
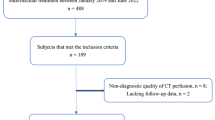
We included a cohort of 828 patients with acute proximal carotid arterial occlusions imaged with a whole-brain CTP within 8 h from stroke onset. pIC was computed on CTP Maps (cerebral blood flow < 30%), and poor clinical outcome was defined as a 90-day modified Rankin Scale score > 2. Potential mediators of the association between pIC and clinical outcome were evaluated through first-order and advanced interaction analyses in the derivation cohort (n = 654) for obtaining a prediction model. The derived model was further validated in an independent cohort (n = 174).
Results
The volume of pIC was significantly associated with poor clinical outcome (OR = 2.19, 95% CI = 1.73 – 2.78, p < 0.001). The strength of this association depended on baseline National Institute of Health Stroke Scale, glucose levels, the use of thrombectomy, and the interaction of age with thrombectomy. The model combining these variables showed good discrimination for predicting clinical outcome in both the derivation cohort and validation cohorts (area under the receiver operating characteristic curve 0.780 (95% CI = 0.746–0.815) and 0.782 (95% CI = 0.715–0.850), respectively).
Conclusions
In patients imaged within 8 h from stroke onset, the association between pIC and clinical outcome is significantly modified by baseline and therapeutic variables. These variables deserve consideration when evaluating the prognostic relevance of pIC.
Key Points
•The volume of CT perfusion (CTP) predicted infarct core (pIC) is associated with poor clinical outcome in acute ischemic stroke imaged within 8 h of onset.
•The relationship between pIC and clinical outcome may be modified by baseline clinical severity, glucose levels, thrombectomy use, and the interaction of age with thrombectomy.
•CTP pIC should be evaluated in an individual basis for predicting clinical outcome in patients imaged within 8 h from stroke onset.





Similar content being viewed by others
Abbreviations
- AAI:
-
Advanced analysis of interaction
- ASPECTS:
-
Alberta Stroke Program Early CT Score
- AUC-ROC:
-
Area under the receiver operating characteristic curve
- CV:
-
Cross-validation
- CTP:
-
CT perfusion
- ICA-T:
-
Internal carotid artery terminal segment
- IVT:
-
Intravenous treatment
- MT:
-
Mechanical thrombectomy
- mRS:
-
Modified Rankin Scale score
- mTICI:
-
Modified thrombolysis in cerebral infarction
- NIHSS:
-
National Institute of Health Stroke Scale
- PO:
-
Poor outcome
- pIC:
-
Predicted infarct core
- rCBF:
-
Relative cerebral blood flow threshold
- SE:
-
Standard error
- TOAST:
-
Trial of Org 10 172 in acute stroke treatment
- VAR:
-
Variance
References
Powers WJ, Rabinstein AA, Ackerson T et al (2019) Guidelines for the early management of patients with acute ischemic stroke: 2019 update to the 2018 guidelines for the early management of acute ischemic stroke: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 50:e344–e418
d'Esterre CD, Fainardi E, Aviv RI, Lee TY (2012) Improving acute stroke management with computed tomography perfusion: a review of imaging basics and applications. Transl Stroke Res 3:205–220
Ribo M, Flores A, Mansilla E et al (2014) Age-adjusted infarct volume threshold for good outcome after endovascular treatment. J Neurointerv Surg 6:418–422
Goyal M, Ospel JM, Menon B et al (2020) Challenging the ischemic core concept in acute ischemic stroke imaging. Stroke 51:3147–3155
Wintermark M, Albers GW, Broderick JP et al (2013) Acute stroke imaging research roadmap II. Stroke 44:2628–2639
Laredo C, Renú A, Tudela R et al (2020) The accuracy of ischemic core perfusion thresholds varies according to time to recanalization in stroke patients treated with mechanical thrombectomy: a comprehensive whole-brain computed tomography perfusion study. J Cereb Blood Flow Metab 40:966–977
Albers GW, Goyal M, Jahan R et al (2016) Ischemic core and hypoperfusion volumes predict infarct size in SWIFT PRIME. Ann Neurol 79:76–89
Vagal A, Menon BK, Foster LD et al (2016) Association between CT angiogram collaterals and CT perfusion in the Interventional Management of Stroke III Trial. Stroke 47:535–538
Haussen DC, Dehkharghani S, Rangaraju S et al (2016) Automated CT perfusion ischemic core volume and noncontrast CT ASPECTS (Alberta Stroke Program Early CT Score): correlation and clinical outcome prediction in large vessel stroke. Stroke 47:2318–2322
Adams HP Jr, Bendixen BH, Kappelle LJ et al (1993) Classification of subtype of acute ischemic stroke. Definitions for use in a multicenter clinical trial. TOAST. Trial of Org 10172 in Acute Stroke Treatment. Stroke 24:35–41
Lin L, Bivard A, Krishnamurthy V, Levi CR, Parsons MW (2016) Whole-brain CT perfusion to quantify acute ischemic penumbra and core. Radiology 279:876–887
Tan IY, Demchuk AM, Hopyan J et al (2009) CT angiography clot burden score and collateral score: correlation with clinical and radiologic outcomes in acute middle cerebral artery infarct. AJNR Am J Neuroradiol 30:525–531
Cereda CW, Christensen S, Campbell BCV et al (2016) A benchmarking tool to evaluate computer tomography perfusion infarct core predictions against a DWI standard. J Cereb Blood Flow Metab 36:1780–1789
Qiao Y, Zhu G, Patrie J et al (2014) Optimal perfusion computed tomographic thresholds for ischemic core and penumbra are not time dependent in the clinically relevant time window. Stroke 45:1355–1362
Parsons MW, Pepper EM, Chan V et al (2005) Perfusion computed tomography: prediction of final infarct extent and stroke outcome. Ann Neurol 58:672–679
Xie Y, Oppenheim C, Guillemin F et al (2018) Pretreatment lesional volume impacts clinical outcome and thrombectomy efficacy. Ann Neurol 83:178–185
d'Esterre CD, Boesen ME, Ahn SH et al (2015) Time-dependent computed tomographic perfusion thresholds for patients with acute ischemic stroke. Stroke 46:3390–3397
Schaefer PW, Souza L, Kamalian S et al (2015) Limited reliability of computed tomographic perfusion acute infarct volume measurements compared with diffusion-weighted imaging in anterior circulation stroke. Stroke 46:419–424
Tian H, Parsons MW, Levi CR et al (2019) Influence of occlusion site and baseline ischemic core on outcome in patients with ischemic stroke. Neurology 92:e2626–e2643
Ay H, Koroshetz WJ, Vangel M et al (2005) Conversion of ischemic brain tissue into infarction increases with age. Stroke 36:2632–2636
Rosso C, Attal Y, Deltour S et al (2011) Hyperglycemia and the fate of apparent diffusion coefficient-defined ischemic penumbra. AJNR Am J Neuroradiol 32:852–856
Bouslama M, Haussen DC, Rodrigues GM et al (2021) Age-adjusted infarct volume cut-off points improve stroke outcome prognostication beyond modeling with age and infarct volume. J Neurointerv Surg. https://doi.org/10.1136/neurintsurg-2020-017066
Acknowledgements
This work was partially developed at the building Centro Esther Koplowitz, Barcelona, CERCA Programme / Generalitat de Catalunya.
Funding
This study has received funding from Instituto de Salud Carlos III (ISCIII) and was co-funded by the European Regional Development Fund. CL and SR receive funding from ISCIII (PFIS-FI16/00231, CM18/00116) and JCP from MCIU (PTA2017-13580-I).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Guarantor
The scientific guarantor of this publication is Sergio Amaro, MD, PhD.
Conflict of Interest
The authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article.
Statistics and Biometry
Two of the authors have significant statistical expertise.
Informed Consent
Written informed consent was waived by the Institutional Review Board.
Ethical Approval
Institutional Review Board approval was obtained.
Methodology
-
Retrospective
-
Cross-sectional study
-
Performed at one institution
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Laredo, C., Solanes, A., Renú, A. et al. Clinical and therapeutic variables may influence the association between infarct core predicted by CT perfusion and clinical outcome in acute stroke. Eur Radiol 32, 4510–4520 (2022). https://doi.org/10.1007/s00330-022-08590-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-022-08590-0