Abstract
Objectives
To investigate patients’ perception of the radiology service when the radiologist communicates the findings to patients.
Methods
After routine MRI, patients in group 1 (n = 101) were given the opportunity to discuss the findings with the radiologist. Patients in group 2 (n = 101) left the radiology department without any personal communication. Subsequently, by means of a questionnaire designed by an expert psychologist, both groups were asked regarding their anxiety, emotional attachment to the institute and subjective assessment of competence.
Results
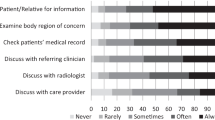
Overall 76 % of all patients were concerned about their imaging findings without significant difference between both groups (p = 0.179). Significantly more patients in group 1 (81%) versus group 2 (14%; p < 0.001) perceived the opportunity to discuss their imaging findings with a radiologist to be a characteristic of a good radiology consultation. A larger number of patients in group 1 experienced significantly higher bonding and only wanted in the future to be examined in the department with communication (p = 0.001) (93%/75%). Significantly more patients in group 1 regarded the radiology department they attended as being more competent (mean score 4.72/4.09, p < 0.001).
Conclusion
Direct communication of imaging findings from radiologists to patients after an MRI examination leads to increased confidence in the radiology service and higher bonding between the patient and radiologist. Radiologists who refrain from direct communication have a lower bonding to patients and are assessed to have lower competence from the patient’s point of view.
Key Points
• Communication between radiologists and patients leads to an increased bonding affinity.
• Direct communication leads to increased patient confidence in the radiology service.
• Patients perceived discussion with a radiologist of high value.


Similar content being viewed by others
References
Lo Re G, De Luca R, Muscarneri F et al (2016) Relationship between anxiety level and radiological investigation. Comparison among different diagnostic imaging exams in a prospective single-center study. Radiol Med 121:763–768
Mettler FA, Bhargavan M, Faulkner K et al (2009) Radiologic and nuclear medicine studies in the United States and worldwide: frequency, radiation dose, and comparison with other radiation sources—1950–2007. Radiology 253:520–531
Dendl LM, Teufel A, Schleder S et al (2017) Analysis of radiological case presentations and their impact on therapy and treatment concepts in internal medicine. Rofo 189:239–246
Miller LS, Shelby RA, Balmadrid MH (2016) Patient anxiety before and immediately after imaging-guided breast biopsy procedures: impact of radiologist-patient communication. J Am Coll Radiol 13:e62–e71
Berlin L (2009) Communicating results of all outpatient radiologic examinations directly to patients: the time has come. AJR Am J Roentgenol 192:571–573
Glazer GM, Ruiz-Wibbelsmann JA (2011) The invisible radiologist. Radiology 258:18–22
Margulis AR, Sostman HD (2004) Radiologist-patient contact during the performance of cross-sectional examinations. J Am Coll Radiol 1:162–163
Boland GW, Glenn L, Goldberg-Stein S et al (2017) Report of the ACR's economics committee on value-based payment models. J Am Coll Radiol 14:6–14
Spielberger CD et al (1980) State-trait anxiety inventory—Forma Y. Milano, Giunti O.S, pp 81–95
Rogers CR, Dorfman E, Nosbüsch E (1972) Client-centered therapy. Kindler Verlag, München
Schulz von Thun F (2006) Miteinander Reden. Rowohlt-Taschenbuch-Verlag, München
Sacristán J (2013) Patient-centered medicine and patient-oriented research: improving health outcomes for individual patients. BMC Med Inform Decis Mak 13:6
Kahn CE, Langlotz CP, Burnside ES et al (2009) Toward best practices in radiology reporting. Radiology 252:852–856
Levitsky DB, Frank MS, Richardson ML, Shneidman RJ (1993) How should radiologists reply when patients ask about their diagnoses? A survey of radiologists' and clinicians' preferences. AJR Am J Roentgenol 161:433–436
Pahade J, Couto C, Davis RB, Patel P, Siewert B, Rosen MP (2012) Reviewing imaging examination results with a radiologist immediately after study completion: patient preferences and assessment of feasibility in an academic department. AJR Am J Roentgenol 199:844–851
Smith JN, Gunderman RB (2010) Should we inform patients of radiology results? Radiology 255:317–321
O'Mahony N, McCarthy E, McDermott R, O'Keeffe S (2012) Who's the doctor? Patients' perceptions of the role of the breast radiologist: a lesson for all radiologists. Br J Radiol 85:e1184–e1189
Koney N, Roudenko A, Ro M, Bahl S, Kagen A (2016) Patients want to meet with imaging experts. J Am Coll Radiol 13:465–470
Cabarrus M, Naeger DM, Rybkin A, Qayyum A (2015) Patients prefer results from the ordering provider and access to their radiology reports. J Am Coll Radiol 12:556–562
European Society of Radiology (ESR) (2017) ESR concept paper on value-based radiology. Insights Imaging 8:447–454
Erdoğan N, İmamoğlu H, Görkem SB, Doğan S, Şenol S, Öztürk A (2017) Preferences of referring physicians regarding the role of radiologists as direct communicators of test results. Diagn Interv Radiol 23:81–85
Mangano MD, Rahman A, Choy G, Sahani DV, Boland GW, Gunn AJ (2014) Radiologists' role in the communication of imaging examination results to patients: perceptions and preferences of patients. AJR Am J Roentgenol 203:1034–1039
Miller P, Lightburn J, Gunderman R, Miller D (2012) Radiologists' role: the patient's perspective. Radiological Society of North America 2012 Scientific Assembly and Annual Meeting, 25–30 November 30, 2012
Norbash A, Bluth E, Lee CI (2014) Radiologist manpower considerations and Imaging 3.0: effort planning for value-based imaging. J Am Coll Radiol 11:953–958
Flory N, Lang EV (2011) Distress in the radiology waiting room. Radiology 260:166–173
European Society of Radiology (Statement) (2010) The future role of radiology in healthcare. Insights Imaging 1:2–11
Knechtges PM, Carlos RC (2007) The evolving role of radiologists within the health care system. J Am Coll Radiol 4:626–635
Acknowledgements
Deep thanks are due to Friedemann Schulz von Thun from Hamburg in Germany, who is an important scientist and teacher of psychology and communication. The education in his institute opened our minds in many aspects.
We would like to thank our medical technologists, who try to improve good communication practice doing the best possible for our patients.
We thank Nicole Graf, who has supported us as a professional statistician in the evaluations (www.graf@biostatistics.ch).
Funding
The authors state that this work has not received any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Andreas Gutzeit.
Conflict of interest
The authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article.
Statistics and biometry
Nicole Graf kindly provided statistical advice for this manuscript.
Informed consent
Written informed consent was obtained from all subjects (patients) in this study.
Ethical approval
Institutional review board approval was obtained.
Methodology
• prospective
• randomised controlled trial
• performed at one institution
Rights and permissions
About this article
Cite this article
Gutzeit, A., Heiland, R., Sudarski, S. et al. Direct communication between radiologists and patients following imaging examinations. Should radiologists rethink their patient care?. Eur Radiol 29, 224–231 (2019). https://doi.org/10.1007/s00330-018-5503-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-018-5503-2