Abstract
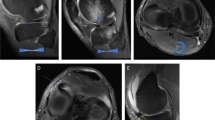
The majority of abnormal findings or lesions on T2-weighted fast spin-echo (FSE) magnetic resonance imaging (MRI) are hyperintense due to increased perfusion or fluid content, such as infections, tumours or synovitis. Hypointense lesions on T2-weighted images (both fat-suppressed and non-fat-suppressed) are less common and can sometimes be overlooked. Such lesions have limited differential diagnostic possibilities, and include vacuum phenomenon, loose body, tenosynovial giant cell tumour, rheumatoid arthritis, haemochromatosis, gout, amyloid, chondrocalcinosis, hydroxyapetite deposition disease, lipoma arborescens, arthrofibrosis and iatrogenic lesions. These lesions often show characteristic appearances and predilections in the knee. In this article, the authors describe the MRI features of hypointense T2 lesions on routine knee MRI and outline a systematic diagnostic approach towards their evaluation.
Key Points
• Hypointense lesions on T2 images (T2 Dark Lesions) encompass limited diagnostic possibilities.
• T2 Dark lesions often show characteristic appearances and predilections in the knee.
• A systematic diagnostic approach will help radiologists make the correct diagnosis.
















Similar content being viewed by others
Abbreviations
- ACL:
-
Anterior cruciate ligament
- CC:
-
Chondrocalcinosis
- CPPD:
-
Calcium pyrophosphate dehydrate
- fsPDW:
-
Fat-suppressed proton density
- GRE:
-
Gradient recalled echo
- LA:
-
Lipoma arborescens
- LBs:
-
Loose bodies
- MM:
-
Meniscomeniscal
- MRI:
-
Magnetic resonance imaging
- PVNS:
-
Pigmented villonodular synovitis
- RA:
-
Rheumatoid arthritis
- STIR:
-
Short tau inversion recovery
- TGCT:
-
Tenosynovial giant cell tumour
- VP:
-
Vacuum phenomenon
References
Narvaez JA, Narvaez J, Ortega R, De Lama E, Roca Y, Vidal N (2003) Hypointense synovial lesions on T2-weighted images: differential diagnosis with pathologic correlation. AJR Am J Roentgenol 181(3):761–9
Gohil I, Vilensky JA, Weber EC (2014) Vacuum phenomenon: Clinical relevance. Clin Anat 27(3):455–62
Mugera C, Suh KJ, Huisman TA, Weber K, Belzberg AJ, Carrino JA, Chhabra A (2013) Sclerotic lesions of the spine: MRI assessment. J Magn Reson Imaging 38(6):1310–24
Shogry ME, Pope TL Jr (1991) Vacuum phenomenon simulating meniscal or cartilaginous injury of the knee at MR imaging. Radiology 180(2):513–5
Sakamoto FA, Winalski CS, Schils JP, Parker RD, Polster JM (2011) Vacuum phenomenon: prevalence and appearance in the knee with 3 T magnetic resonance imaging. Skeletal Radiol 40(10):1275–85
Milgram JW (1977) The classification of loose bodies in human joints. Clin Orthop Relat Res 124:282–91
Felson DT (2004) An update on the pathogenesis and epidemiology of osteoarthritis. Radiol Clin North Am 42(1):1–9, v
Chhabra A, Soldatos T (2012) Soft-tissue lesions: when can we exclude sarcoma? AJR Am J Roentgenol 199(6):1345–57
Milgram JW (1977) Synovial osteochondromatosis: a histopathological study of thirty cases. J Bone Joint Surg Am 59(6):792–801
Crotty JM, Monu JU, Pope TL Jr (1996) Synovial osteochondromatosis. Radiol Clin North Am 34(2):327–42, xi
Murphey MD, Vidal JA, Fanburg-Smith JC, Gajewski DA (2007) Imaging of synovial chondromatosis with radiologic-pathologic correlation. Radiographics 27(5):1465–88
Yoshimitsu K, Kakihara D, Irie H, Tajima T, Nishie A, Asayama Y et al (2006) Papillary renal carcinoma: diagnostic approach by chemical shift gradient-echo and echo-planar MR imaging. J Magn Reson Imaging 23(3):339–44
Nguyen JC, De Smet AA, Graf BK, Rosas HG (2014) MR imaging-based diagnosis and classification of meniscal tears. Radiographics 34(4):981–99
Camacho MA (2004) The double posterior cruciate ligament sign. Radiology 233(2):503–4
Stoller DW, Tirman PFJ, Bredella MA (2004) Diagnostic Imaging: Orthopaedics: Amirsys
Fox AJ, Wanivenhaus F, Burge AJ, Warren RF, Rodeo SA. (2014) The human meniscus: A review of anatomy, function, injury, and advances in treatment. Clin Anat
Sanders TG, Linares RC, Lawhorn KW, Tirman PF, Houser C (1999) Oblique meniscomeniscal ligament: another potential pitfall for a meniscal tear--anatomic description and appearance at MR imaging in three cases. Radiology 213(1):213–6
Chan CM, Goldblatt JP (2012) Unilateral meniscomeniscal ligament. Orthopedics 35(12):e1815–7
Choi SH, Shin KE, Chang MJ, Woo SY, Lee SH (2013) Diagnostic criterion to distinguish between incomplete and complete discoid lateral meniscus on MRI. J Magn Reson Imaging 38(2):417–21
Singh K, Helms CA, Jacobs MT, Higgins LD (2006) MRI appearance of Wrisberg variant of discoid lateral meniscus. AJR Am J Roentgenol 187(2):384–7
Griffin AM, Ferguson PC, Catton CN, Chung PW, White LM, Wunder JS et al (2012) Long-term outcome of the treatment of high-risk tenosynovial giant cell tumor/pigmented villonodular synovitis with radiotherapy and surgery. Cancer 118(19):4901–9
Huang GS, Lee CH, Chan WP, Chen CY, Yu JS, Resnick D (2003) Localized nodular synovitis of the knee: MR imaging appearance and clinical correlates in 21 patients. AJR Am J Roentgenol 181(2):539–43
Ravi V, Wang WL, Lewis VO (2011) Treatment of tenosynovial giant cell tumor and pigmented villonodular synovitis. Curr Opin Oncol 23(4):361–6
Murphey MD, Rhee JH, Lewis RB, Fanburg-Smith JC, Flemming DJ, Walker EA (2008) Pigmented villonodular synovitis: radiologic-pathologic correlation. Radiographics 28(5):1493–518
Yu JS, Chung C, Recht M, Dailiana T, Jurdi R (1997) MR imaging of tophaceous gout. AJR Am J Roentgenol 168(2):523–7
Richette P, Bardin T (2010) Gout Lancet 375(9711):318–28
Ko KH, Hsu YC, Lee HS, Lee CH, Huang GS (2010) Tophaceous gout of the knee: revisiting MRI patterns in 30 patients. J Clin Rheumatol 16(5):209–14
Chen CK, Yeh LR, Pan HB, Yang CF, Lu YC, Wang JS et al (1999) Intra-articular gouty tophi of the knee: CT and MR imaging in 12 patients. Skeletal Radiol 28(2):75–80
Nicolaou S, Liang T, Murphy DT, Korzan JR, Ouellette H, Munk P (2012) Dual-energy CT: a promising new technique for assessment of the musculoskeletal system. AJR Am J Roentgenol 199(5 Suppl):S78–86
Bongartz T, Glazebrook KN, Kavros SJ, Murthy NS, Merry SP, Franz WB, 3rd, et al. (2014) Dual-energy CT for the diagnosis of gout: an accuracy and diagnostic yield study. Ann Rheum Dis
Gabriel SE (2001) The epidemiology of rheumatoid arthritis. Rheum Dis Clin North Am 27(2):269–81
Poleksic L, Musikic P, Zdravkovic D, Watt I, Bacic G (1996) MRI evaluation of the knee in rheumatoid arthritis. Br J Rheumatol 35(Suppl 3):36–9
Rominger MB, Bernreuter WK, Kenney PJ, Morgan SL, Blackburn WD, Alarcon GS (1993) MR imaging of the hands in early rheumatoid arthritis: preliminary results. Radiographics 13(1):37–46
Kursunoglu-Brahme S, Riccio T, Weisman MH, Resnick D, Zvaifler N, Sanders ME et al (1990) Rheumatoid knee: role of gadopentetate-enhanced MR imaging. Radiology 176(3):831–5
Economides CP, Soteriades ES, Hadjigavriel M, Seimenis I, Karantanas A (2013) Iron deposits in the knee joints of a thalassemic patient. Acta Radiologica Short Reports 2(1):2047981613477401
Axford JS, Bomford A, Revell P, Watt I, Williams R, Hamilton EB (1991) Hip arthropathy in genetic hemochromatosis. Radiographic and histologic features. Arthritis Rheum 34(3):357–61
Adamson TC 3rd, Resnik CS, Guerra J Jr, Vint VC, Weisman MH, Resnick D (1983) Hand and wrist arthropathies of hemochromatosis and calcium pyrophosphate deposition disease: distinct radiographic features. Radiology 147(2):377–81
Jager HJ, Mehring U, Gotz GF, Neise M, Erlemann R, Kapp HJ et al (1997) Radiological features of the visceral and skeletal involvement of hemochromatosis. Eur Radiol 7(8):1199–206
Sahinbegovic E, Dallos T, Aigner E, Axmann R, Manger B, Englbrecht M et al (2010) Musculoskeletal disease burden of hereditary hemochromatosis. Arthritis Rheum 62(12):3792–8
Rihl M, Kellner H (2004) Arthropathy of hereditary hemochromatosis. Z Rheumatol 63(1):22–9
Frenzen K, Schafer C, Keysser G (2013) Erosive and inflammatory joint changes in hereditary hemochromatosis arthropathy detected by low-field magnetic resonance imaging. Rheumatol Int 33(8):2061–7
Queiroz-Andrade M, Blasbalg R, Ortega CD, Rodstein MA, Baroni RH, Rocha MS et al (2009) MR imaging findings of iron overload. Radiographics 29(6):1575–89
Eustace S, Buff B, McCarthy C, MacMathuana P, Gilligan P, Ennis JT (1994) Magnetic resonance imaging of hemochromatosis arthropathy. Skeletal Radiol 23(7):547–9
M'Bappe P, Grateau G (2012) Osteo-articular manifestations of amyloidosis. Best Pract Res Clin Rheumatol 26(4):459–75
Jensen PS (1988) Chondrocalcinosis and other calcifications. Radiol Clin North Am 26(6):1315–25
Brower AC, Flemming DJ (2012) Arthritis in Black and White: Elsevier Health Sciences
Barskova VG, Kudaeva FM, Bozhieva LA, Smirnov AV, Volkov AV, Nasonov EL (2013) Comparison of three imaging techniques in diagnosis of chondrocalcinosis of the knees in calcium pyrophosphate deposition disease. Rheumatology (Oxford) 52(6):1090–4
Beltran J, Marty-Delfaut E, Bencardino J, Rosenberg ZS, Steiner G, Aparisi F et al (1998) Chondrocalcinosis of the hyaline cartilage of the knee: MRI manifestations. Skeletal Radiol 27(7):369–74
Burke BJ, Escobedo EM, Wilson AJ, Hunter JC (1998) Chondrocalcinosis mimicking a meniscal tear on MR imaging. AJR Am J Roentgenol 170(1):69–70
Kaushik S, Erickson JK, Palmer WE, Winalski CS, Kilpatrick SJ, Weissman BN (2001) Effect of chondrocalcinosis on the MR imaging of knee menisci. AJR Am J Roentgenol 177(4):905–9
Senocak E, Gurel K, Gurel S, Ozturan KE, Cakici H, Yilmaz F et al (2007) Lipoma arborescens of the suprapatellar bursa and extensor digitorum longus tendon sheath: report of 2 cases. J Ultrasound Med 26(10):1427–33
Kloen P, Keel SB, Chandler HP, Geiger RH, Zarins B, Rosenberg AE (1998) Lipoma arborescens of the knee. J Bone Joint Surg (Br) 80(2):298–301
Al-Shraim MM (2011) Intra-articular lipoma arborescens of the knee joint. Ann Saudi Med 31(2):194–6
Sheldon PJ, Forrester DM, Learch TJ (2005) Imaging of intraarticular masses. Radiographics 25(1):105–19
Coll JP, Ragsdale BD, Chow B, Daughters TC (2011) Best cases from the AFIP: lipoma arborescens of the knees in a patient with rheumatoid arthritis. Radiographics 31(2):333–7
Apple JS, Martinez S, Hardaker WT, Daffner RH, Gehweiler JA (1982) Synovial plicae of the knee. Skeletal Radiol 7(4):251–4
Dupont JY (1997) Synovial plicae of the knee. Controversies and review. Clin Sports Med 16(1):87–122
Boles CA, Martin DF (2001) Synovial plicae in the knee. AJR Am J Roentgenol 177(1):221–7
Garcia-Valtuille R, Abascal F, Cerezal L, Garcia-Valtuille A, Pereda T, Canga A et al (2002) Anatomy and MR imaging appearances of synovial plicae of the knee. Radiographics 22(4):775–84
Horton LK, Jacobson JA, Lin J, Hayes CW (2000) MR imaging of anterior cruciate ligament reconstruction graft. AJR Am J Roentgenol 175(4):1091–7
Papakonstantinou O, Chung CB, Chanchairujira K, Resnick DL (2003) Complications of anterior cruciate ligament reconstruction: MR imaging. Eur Radiol 13(5):1106–17
Bradley DM, Bergman AG, Dillingham MF (2000) MR imaging of cyclops lesions. AJR Am J Roentgenol 174(3):719–26
McCauley TR (2005) MR imaging evaluation of the postoperative knee. Radiology 234(1):53–61
Recht MP, Kramer J (2002) MR imaging of the postoperative knee: a pictorial essay. Radiographics 22(4):765–74
Harris WH (1994) Osteolysis and particle disease in hip replacement. A review. Acta Orthop Scand 65(1):113–23
Acknowledgments
The authors would like to thank Ms. Pam Curry for creating the beautiful illustrations. The scientific guarantor of this publication is Avneesh Chhabra. The authors of this manuscript declare a relationships with the following company: Dr. Avneesh Chhabra serves as research consultant with Siemens CAD group. The authors state that this work has not received any funding. No complex statistical methods were necessary for this paper. Institutional Review Board approval was not required because it is a review article. Written informed consent was not required for this study because it is a review article. No study subjects or cohorts have been previously reported. Methodology: performed at one institution.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wadhwa, V., Cho, G., Moore, D. et al. T2 black lesions on routine knee MRI: differential considerations. Eur Radiol 26, 2387–2399 (2016). https://doi.org/10.1007/s00330-015-4027-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-015-4027-2