Abstract
Objectives
To investigate the effect of a radiation reduction program on total dose, fluoroscopy dose per second corrected for body habitus and degree of collimation in left varicocele embolizations (LVE).
Methods
A radiation reduction program for LVE was implemented, consisting of a technique minimizing fluoroscopy time, using low-dose presets, virtual collimation, and virtual patient positioning. Height, weight, fluoroscopy time, kerma area product (KAP) and reference air kerma (Ka,r) were recorded for 100 consecutive cases satisfying the inclusion criteria. For each patient, a device specific dose correction factor, determined using a phantom, was used to standardize the KAP to that of the cylindrical diameter of the standard man and a collimation index was derived from the KAP and Ka,r.
Results
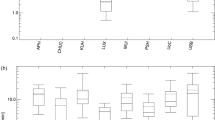
Median fluoroscopy time was 3 minutes (mean 4.5, range 1-23.8). Median KAP was 0.54 Gy/cm2 (mean 0.82, range 0.12-6.52). There was a significant decrease in KAP/second corrected for cylindrical diameter (p < 0.001) and the collimation index (p < 0.001) over time.
Conclusions
This study shows that a dedicated dose reduction program can achieve very low total radiation dose rates for LVE. The significant decrease in collimation index and standardized KAP per second during this study suggest a learning curve for collimation.
Key Points
• Left varicocele embolization can be performed with very low radiation doses.
• The most effective real time radiation reduction measure is collimation.
• There is a learning curve to achieving optimal collimation.




Similar content being viewed by others
Abbreviations
- KAP:
-
kerma area product
- Ka,r:
-
Reference air kerma
- STD:
-
sodium tetradecylsulphate
- BMI:
-
body mass index
- CI:
-
collimation index
- CT:
-
computerized tomography
- LVE:
-
left varicocele embolization
- IRP:
-
interventional reference point
References
Sabanegh E, Agarwal A (2012) Male infertility. In: Wein AJ, Kavoussi LR, Novick AC, Partin AW, Peters CA (eds) Campbell-Walsh urology, 10th edn. Saunders, Philadelphia, pp 636–637
World Health Organization (1992) The influence of varicocele on parameters of fertility in a large group of men presenting to infertility clinics. Fertil Steril 57:1289–1293
Gorelick JI, Goldstein M (1993) Loss of fertility in men with varicocele. Fertil Steril 59:613–616
Agarwal A, Deepinder F, Cocuzza M, Agarwal R, Short RA, Sabanegh E et al (2007) Efficacy of varicocelectomy in improving semen parameters: new meta-analytical approach. Urology 70:532–538
Diegidio P, Jhaveri JK, Ghannam S, Pinkhasov R, Shabsigh R, Fisch H (2011) Review of current varicocelectomy techniques and their outcomes. BJU Int 108:1157–1172
Storm DW, Hogan MJ, Jayanthi VR (2010) Initial experience with percutaneous selective embolization: a truly minimally invasive treatment of the adolescent varicocele with no risk of hydrocele development. J Pediatr Urol 6:567–571
Cassidy D, Jarvi K, Grober E, Lo K (2012) Varicocele surgery or embolization: which is better? Can Urol Assoc J 6:266–268
Brenner DJ, Hall EJ (2007) Computed tomography—an increasing source of radiation exposure. N Engl J Med 357:2277–2284
Miller D, Balter S, Cole PE et al (2003) Radiation doses in interventional radiology procedures: the RAD-IR study. Part 1: overall measure of dose. J Vasc Interv Radiol 14:711–727
Chalmers N, Hufton AP, Jackson RW, Conway B (2000) Radiation risk estimation in varicocele embolization. Br J Radiol 73:293–297
Flacke S, Schuster M, Kovacs A et al (2008) Embolization of varicocles: pretreatment sperm motility predicts later pregnancy in partners of infertile men. Radiology 248:540–549
Calama Santiago JA, PenedoCobos JM, Molina López MY, González Ruiz C, GarcíaMollá R, Sierra Díaz F (2008) Paediatric varicocele embolization dosimetric study. Actas Urol Esp 32:833–842
Walters TE, Kistler PM, Morton JB, Sparks PB, Halloran K, Kalman JM (2012) Impact of collimation on radiation exposure during interventional electrophysiology. Europace 14:1670–1673
Miller DL, Balter S, Dixon RG et al (2012) Quality improvement guidelines for recording patient radiation dose in the medical records for fluoroscopically guided procedures. J Vasc Interv Radiol 23:11–18
Reiner E, Pollack JS, Henderson KJ, Weiss RM, White RI (2008) Initial experience with 3 % sodium tetradecyl sulfate foam and fibered coils for management of adolescent varicocele. J Vasc Interv Radiol 19:207–210
Chapple C-L, Broadhead DA, Faulkner K (1995) A phantom method for deriving typical doses from measurements of dose-area product on populations of patients. Br J Radiol 68:1083–1086
(2003) International Commission on Radiological Protection Basic anatomical and physiological data for use in radiological protection: reference values, ICRP Publication 89. Pergamon Press, Oxford, UK
Murray RR Jr, Mitchell SE, Kadir S, Kaufman SL, Chang R, Kinnison ML et al (1986) Comparison of recurrent varicocele anatomy following surgery and percutaneous balloon occlusion. J Urol 135:286–289
Miller DL, Kwon D, Bonavia GH (2009) Reference levels for patient radiation doses in interventional radiology: proposed initial values for U.S. practice. Radiology 253:753–764
Acknowledgments
The authors wish to thank Dr Keith Faulkner, Public Health England, Newcastle Upon Tyne for his thoughtful insights and for reviewing the physics and Oded Olsha MD for his valuable contributions. The scientific guarantor of this publication is Anthony Verstandig MD. The authors of this manuscript declare no relationships with any companies, whose products or services may be related to the subject matter of the article. The authors state that this work has not received any funding. One of the authors has significant statistical expertise. Institutional Review Board approval was obtained. Written informed consent was obtained from all subjects (patients) in this study. Methodology: prospective, experimental, performed at one institution.
Author information
Authors and Affiliations
Corresponding author
Appendices
Appendix 1
A device-specific correction factor K(cm-1) relating radiation dose to thickness of area irradiated was derived using a variation of the method described by Chapple [16]. A water bath 30 centimeters in height was placed on the tabletop allowing determination of KAP for different depths of water starting from zero and increasing by three centimeter increments. The exact level of the water was determined using a ruler taped to the inside of the water bath. Each depth of water was irradiated for five seconds on the low-dose fluoroscopy setting at 7.5 pulses per second to allow autocalilbration of tube output. The KAP was the then recorded for five minutes of continuous fluoroscopy. The table detector distance (set arbitrarily at 32 cm) and collimation were unchanged throughout the procedure. The water phantom thickness and the KAP were plotted on a scatter diagram to yield an exponential gradient K, which was used to correct the radiation doses of the varicocele embolization procedures to that of the reference man of 73 kg weight and 176 cm height.
Appendix 2
The accuracy of the KAP meter for different irradiated areas was investigated using a 23 cm thick water phantom. Each area was irradiated for five seconds on the normal dose fluoroscopy setting at 7.5 pulses per second to allow autocalibration of tube output. The KAP and Ka,r were then recorded for two minutes of continuous fluoroscopy and the results plotted against the area irradiated which was calculated from measurements made using the inbuilt software (Fig 5).
Plot of KAP and Ka,r against area irradiated demonstrating linear increase in KAP over the entire range of areas irradiated in the study. The slight decrease in Ka,r with increasing area is caused by the automatic brightness control compensating for the increased scatter radiation with larger field size
The results demonstrated a linear increase in KAP over areas from 6.5-180 cm2 which covered the entire range used for left varicocele embolization in this study.
Rights and permissions
About this article
Cite this article
Verstandig, A.G., Shamieh, B., Shraibman, V. et al. Radiation dose reduction in fluoroscopic procedures: left varicocele embolization as a model. Eur Radiol 25, 1639–1645 (2015). https://doi.org/10.1007/s00330-014-3556-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-014-3556-4