Abstract
Objectives
To compare 3.0 Tesla breast magnetic resonance imaging (MRI) with galactography for detection of benign and malignant causes of nipple discharge in patients with negative mammography and ultrasound.
Methods
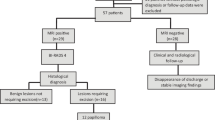
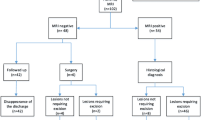
We prospectively evaluated 56 breasts of 50 consecutive patients with nipple discharge who had inconspicuous mammography and ultrasound, using 3.0 Tesla breast MRI with a dedicated 16-channel breast coil, and then compared the results with galactography. Histopathological diagnoses and follow-ups were used as reference standard. Lesion size estimated on MRI was compared with the size at histopathology.
Results
Sensitivity and specificity of MRI vs. galactography for detecting pathologic findings were 95.7 % vs. 85.7 % and 69.7 % vs. 33.3 %, respectively. For the supposed concrete pathology based on MRI findings, the specificity was 67.6 % and the sensitivity 77.3 % (PPV 60.7 %, NPV 82.1 %). Eight malignant lesions were detected (14.8 %). The estimated size at breast MRI showed excellent correlation with the size at histopathology (Pearson’s correlation coefficient 0.95, p < 0.0001).
Conclusions
MRI of the breast at 3.0 Tesla is an accurate imaging test and can replace galactography in the workup of nipple discharge in patients with inconspicuous mammography and ultrasound.
Key Points
• Breast MRI is an excellent diagnostic tool for patients with nipple discharge.
• MRI of the breast reveals malignant lesions despite inconspicuous mammography and ultrasound.
• MRI of the breast has greater sensitivity and specificity than galactography.
• Excellent correlation of lesion size measured at MRI and histopathology was found.





Similar content being viewed by others
Abbreviations
- BI-RADS®:
-
Breast Imaging Reporting and Data System
- DCIS:
-
Ductal carcinoma in situ
- DTPA:
-
Diethylene triamine pentaacetic acid
- EUSOMA:
-
European Society of Breast Cancer Specialists
- Hp.:
-
Histopathology
- MHz:
-
Megahertz
- MRI:
-
Magnetic resonance imaging
- NPV:
-
Negative predictive value
- PPV:
-
Positive predictive value
- ROI:
-
Region of interest
- SD:
-
Standard deviation
- SPAIR:
-
Spectrally adiabatic inversion recovery
- TE:
-
Echo time
- TR:
-
Repetition time
- TSE:
-
Turbo spin-echo
References
Zervoudis S, Iatrakis G, Economides P, Polyzos D, Navrozoglou I (2010) Nipple discharge screening. Womens Health (Lond Engl) 6:135–151
Leis HP Jr (1989) Management of nipple discharge. World J Surg 13:736–742
Morrogh M, Park A, Elkin EB, King TA (2010) Lessons learned from 416 cases of nipple discharge of the breast. Am J Surg 200:73–80
Orel SG, Dougherty CS, Reynolds C, Czerniecki BJ, Siegelman ES, Schnall MD (2000) MR imaging in patients with nipple discharge: initial experience. Radiology 216:248–254
Lorenzon M, Zuiani C, Linda A, Londero V, Girometti R, Bazzocchi M (2011) Magnetic resonance imaging in patients with nipple discharge: should we recommend it? Eur Radiol 21:899–907
Fischer U, Kuhl CK (2013) Paradigmenwechsel in der Mammadiagnostik im Zeitalter der Mamma-MRT. Radiologie 13:245–258
Adepoju LJ, Chun J, El-Tamer M, Ditkoff BA, Schnabel F, Joseph KA (2005) The value of clinical characteristics and breast-imaging studies in predicting a histopathologic diagnosis of cancer or high-risk lesion in patients with spontaneous nipple discharge. Am J Surg 190:644–646
Son EJ, Kim EK, Kim JA, Kwak JY, Jeong J (2009) Diagnostic value of 3D fast low-angle shot dynamic MRI of breast papillomas. Yonsei Med J 50:838–844
Kuhl CK, Schrading S, Bieling HB et al (2007) MRI for diagnosis of pure ductal carcinoma in situ: a prospective observational study. Lancet 370:485–492
Kuhl CK (2007) Current status of breast MR imaging. Part 2. Clinical applications. Radiology 244:672–691
Sardanelli F, Boetes C, Borisch B et al (2010) Magnetic resonance imaging of the breast: recommendations from the EUSOMA working group. Eur J Cancer 46:1296–1316
American College of Radiology (2003) ACR BI-RADS breast imaging reporting and data system: breast imaging atlas, 4th edn. American College of Radiology, Reston
Sabel MS, Helvie MA, Breslin T et al (2012) Is duct excision still necessary for all cases of suspicious nipple discharge? Breast J 18:157–162
Gray RJ, Pockaj BA, Karstaedt PJ (2007) Navigating murky waters: a modern treatment algorithm for nipple discharge. Am J Surg 194:850–854, discussion 854–855
Morrogh M, Morris EA, Liberman L, Borgen PI, King TA (2007) The predictive value of ductography and magnetic resonance imaging in the management of nipple discharge. Ann Surg Oncol 14:3369–3377
Albrecht C, Thele F, Grunwald S et al (2013) Nipple discharge: role of ductoscopy in comparison with standard diagnostic tests. Onkologie 36:12–16
Pinker K, Grabner G, Bogner W et al (2009) A combined high temporal and high spatial resolution 3 Tesla MR imaging protocol for the assessment of breast lesions: initial results. Invest Radiol 44:553–558
Kuhl CK, Jost P, Morakkabati N, Zivanovic O, Schild HH, Gieseke J (2006) Contrast-enhanced MR imaging of the breast at 3.0 and 1.5 T in the same patients: initial experience. Radiology 239:666–676
Schmitz AC, Peters NH, Veldhuis WB et al (2008) Contrast-enhanced 3.0-T breast MRI for characterization of breast lesions: increased specificity by using vascular maps. Eur Radiol 18:355–364
Pinker-Domenig K, Bogner W, Gruber S et al (2012) High resolution MRI of the breast at 3 T: which BI-RADS(R) descriptors are most strongly associated with the diagnosis of breast cancer? Eur Radiol 22:322–330
Elsamaloty H, Elzawawi MS, Mohammad S, Herial N (2009) Increasing accuracy of detection of breast cancer with 3-T MRI. AJR Am J Roentgenol 192:1142–1148
Matsuoka A, Minato M, Harada M et al (2008) Comparison of 3.0- and 1.5-tesla diffusion-weighted imaging in the visibility of breast cancer. Radiat Med 26:15–20
Liberman L, Mason G, Morris EA, Dershaw DD (2006) Does size matter? Positive predictive value of MRI-detected breast lesions as a function of lesion size. AJR Am J Roentgenol 186:426–430
Langer SA, Horst KC, Ikeda DM, Daniel BL, Kong CS, Dirbas FM (2005) Pathologic correlates of false positive breast magnetic resonance imaging findings: which lesions warrant biopsy? Am J Surg 190:633–640
Schouten van der Velden AP, Schlooz-Vries MS, Boetes C, Wobbes T (2009) Magnetic resonance imaging of ductal carcinoma in situ: what is its clinical application? A review. Am J Surg 198:262–269
Grunwald S, Heyer H, Paepke S et al (2007) Diagnostic value of ductoscopy in the diagnosis of nipple discharge and intraductal proliferations in comparison to standard methods. Onkologie 30:243–248
Sickles EA (2000) Galactography and other imaging investigations of nipple discharge. Lancet 356:1622–1623
Funovics MA, Philipp MO, Lackner B, Fuchsjaeger M, Funovics PT, Metz V (2003) Galactography: method of choice in pathologic nipple discharge? Eur Radiol 13:94–99
Kopans DB (1994) Caution on core. Radiology 193:325–326, discussion 326–328
Acknowledgments
We would like to thank Andrew McLeod for careful review of the manuscript as native speaker. The scientific guarantor of this publication is Prof. Thorsten Alexander Bley. The authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article. The authors state that this work has not received any funding. One of the authors, Dr. Andreas Max Weng, has significant statistical expertise. Institutional review board approval was obtained from the ethics committee of the Medical Faculty of the University of Würzburg. Written informed consent was obtained from all subjects (patients) in this study. Methodology: prospective, diagnostic or prognostic study, performed at one institution.
Author information
Authors and Affiliations
Corresponding author
Additional information
Nóra Lubina and Ulla Schedelbeck contributed equally to this work.
Rights and permissions
About this article
Cite this article
Lubina, N., Schedelbeck, U., Roth, A. et al. 3.0 Tesla breast magnetic resonance imaging in patients with nipple discharge when mammography and ultrasound fail. Eur Radiol 25, 1285–1293 (2015). https://doi.org/10.1007/s00330-014-3521-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-014-3521-2