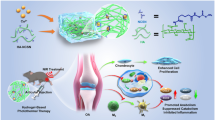
Abstract
The purpose of this study is to observe the differences of osteopontin (OPN) phosphorylation in osteoarthritis (OA) cartilage and normal cartilage, and evaluate the possible correlations between the OPN phosphorylation and MMP-13 expression. Degenerative cartilage (n = 29) and normal cartilage (n = 10) were identified by hematoxylin-eosin, safranin-O staining and modified Mankin score. The phosphorylation level of OPN in OA cartilage and normal cartilage was detected by immunoprecipitation. Chondrocytes were treated with phospho-OPN, OPN or buffer. Quantitative reverse transcription polymerase chain reaction (qPCR) and ELISA were used to assess the expression of MMP-13 in different treatments. The OD values of phosphorylation of OPN in normal cartilage and OA cartilage were 137.89 ± 10.59 and 153.52 ± 8.80, respectively, (P = 0.000). Chondrocytes treated with OPN showed a higher MMP-13 expression at gene and protein level compared with control group. Chondrocytes treated with phospho-OPN showed the highest MMP-13 expression in gene and protein. In conclusion, our results revealed a higher phosphorylation level of OPN in OA cartilage than in normal cartilage. We found OPN leads to elevated expression of MMP-13 (both at gene level and protein level), and phospho-OPN had a more obvious upregulation effect on MMP-13 expression than nonphospho-OPN. Further studies are needed to reveal the mechanism of OPN phosphorylation on cartilage degeneration.


Similar content being viewed by others
References
Buckwalter JA, Martin JA (2006) Osteoarthritis. Adv Drug Deliv Rev 58(2):150–167. doi:10.1016/j.addr.2006.01.006
Aigner T, Fundel K, Saas J, Gebhard PM, Haag J, Weiss T, Zien A, Obermayr F, Zimmer R, Bartnik E (2006) Large-scale gene expression profiling reveals major pathogenetic pathways of cartilage degeneration in osteoarthritis. Arthritis Rheum 54(11):3533–3544. doi:10.1002/art.22174
Knauper V, Lopez-Otin C, Smith B, Knight G, Murphy G (1996) Biochemical characterization of human collagenase-3. J Biol Chem 271(3):1544–1550
Otero M, Plumb DA, Tsuchimochi K, Dragomir CL, Hashimoto K, Peng H, Olivotto E, Bevilacqua M, Tan L, Yang Z, Zhan Y, Oettgen P, Li Y, Marcu KB, Goldring MB (2012) E74-like factor 3 (ELF3) impacts on matrix metalloproteinase 13 (MMP13) transcriptional control in articular chondrocytes under proinflammatory stress. J Biol Chem 287(5):3559–3572. doi:10.1074/jbc.M111.265744
Yin J, Yang Z, Cao YP, Ge ZG (2011) Characterization of human primary chondrocytes of osteoarthritic cartilage at varying severity. Chin Med J 124(24):4245–4253
Tetlow LC, Adlam DJ, Woolley DE (2001) Matrix metalloproteinase and proinflammatory cytokine production by chondrocytes of human osteoarthritic cartilage: associations with degenerative changes. Arthritis Rheum 44(3):585–594. doi:10.1002/1529-0131(200103)44:3<585:AID-ANR107>3.0.CO;2-C
Buckland J (2012) Osteoarthritis: complement-mediated inflammation in OA progression. Nat Rev Rheumatol 8(1):2. doi:10.1038/nrrheum.2011.182
Kapoor M, Martel-Pelletier J, Lajeunesse D, Pelletier JP, Fahmi H (2011) Role of proinflammatory cytokines in the pathophysiology of osteoarthritis. Nat Rev Rheumatol 7(1):33–42. doi:10.1038/nrrheum.2010.196
Hasegawa M, Segawa T, Maeda M, Yoshida T, Sudo A (2011) Thrombin-cleaved osteopontin levels in synovial fluid correlate with disease severity of knee osteoarthritis. J Rheumatol 38(1):129–134. doi:10.3899/jrheum.100637
Gao SG, Li KH, Zeng KB, Tu M, Xu M, Lei GH (2010) Elevated osteopontin level of synovial fluid and articular cartilage is associated with disease severity in knee osteoarthritis patients. Osteoarthr Cartil/OARS Osteoarthr Res Soc 18(1):82–87. doi:10.1016/j.joca.2009.07.009
Honsawek S, Tanavalee A, Sakdinakiattikoon M, Chayanupatkul M, Yuktanandana P (2009) Correlation of plasma and synovial fluid osteopontin with disease severity in knee osteoarthritis. Clin Biochem 42(9):808–812. doi:10.1016/j.clinbiochem.2009.02.002
Martin I, Jakob M, Schafer D, Dick W, Spagnoli G, Heberer M (2001) Quantitative analysis of gene expression in human articular cartilage from normal and osteoarthritic joints. Osteoarthr Cartil/OARS, Osteoarthr Res Soc 9(2):112–118. doi:10.1053/joca.2000.0366
Pullig O, Weseloh G, Gauer S, Swoboda B (2000) Osteopontin is expressed by adult human osteoarthritic chondrocytes: protein and mRNA analysis of normal and osteoarthritic cartilage. Matrix Biol 19(3):245–255
Qin C, Baba O, Butler WT (2004) Post-translational modifications of sibling proteins and their roles in osteogenesis and dentinogenesis. Critical Rev Oral Biol Med 15(3):126–136
Sodek J, Ganss B, McKee MD (2000) Osteopontin. Crit Rev Oral Biol Med 11(3):279–303
Christensen B, Klaning E, Nielsen MS, Andersen MH, Sorensen ES (2012) C-terminal modification of osteopontin inhibits interaction with the alphaVbeta3-integrin. J Biol Chem 287(6):3788–3797. doi:10.1074/jbc.M111.277996
Christensen B, Kazanecki CC, Petersen TE, Rittling SR, Denhardt DT, Sorensen ES (2007) Cell type-specific post-translational modifications of mouse osteopontin are associated with different adhesive properties. J Biol Chem 282(27):19463–19472. doi:10.1074/jbc.M703055200
Anborgh PH, Mutrie JC, Tuck AB, Chambers AF (2011) Pre- and post-translational regulation of osteopontin in cancer. J Cell Commun Signal 5(2):111–122. doi:10.1007/s12079-011-0130-6
Rasheed Z, Akhtar N, Haqqi TM (2010) Pomegranate extract inhibits the interleukin-1beta-induced activation of MKK-3, p38alpha-MAPK and transcription factor RUNX-2 in human osteoarthritis chondrocytes. Arthritis Res Ther 12(5):R195. doi:10.1186/ar3166
Mankin HJ, Dorfman H, Lippiello L, Zarins A (1971) Biochemical and metabolic abnormalities in articular cartilage from osteo-arthritic human hips. II. Correlation of morphology with biochemical and metabolic data. J Bone Jt Surg Am Vol 53(3):523–537
Rodrigues LR, Teixeira JA, Schmitt FL, Paulsson M, Lindmark-Mansson H (2007) The role of osteopontin in tumor progression and metastasis in breast cancer. Cancer Epidemiol Biomarkers Prev 16(6):1087–1097. doi:10.1158/1055-9965.EPI-06-1008
O’Regan A (2003) The role of osteopontin in lung disease. Cytokine Growth Factor Rev 14(6):479–488
McKee MD, Pedraza CE, Kaartinen MT (2011) Osteopontin and wound healing in bone. Cells Tissues Organs 194(2–4):313–319. doi:10.1159/000324244
Buback F, Renkl AC, Schulz G, Weiss JM (2009) Osteopontin and the skin: multiple emerging roles in cutaneous biology and pathology. Exp Dermatol 18(9):750–759. doi:10.1111/j.1600-0625.2009.00926.x
Haylock DN, Nilsson SK (2006) Osteopontin: a bridge between bone and blood. Br J Haematol 134(5):467–474. doi:10.1111/j.1365-2141.2006.06218.x
Gravallese EM (2003) Osteopontin: a bridge between bone and the immune system. J Clin Investig 112(2):147–149. doi:10.1172/JCI19190
Weber GF, Zawaideh S, Hikita S, Kumar VA, Cantor H, Ashkar S (2002) Phosphorylation-dependent interaction of osteopontin with its receptors regulates macrophage migration and activation. J Leukoc Biol 72(4):752–761
Al-Shami R, Sorensen ES, Ek-Rylander B, Andersson G, Carson DD, Farach-Carson MC (2005) Phosphorylated osteopontin promotes migration of human choriocarcinoma cells via a p70 S6 kinase-dependent pathway. J Cell Biochem 94(6):1218–1233. doi:10.1002/jcb.20379
Ek-Rylander B, Flores M, Wendel M, Heinegard D, Andersson G (1994) Dephosphorylation of osteopontin and bone sialoprotein by osteoclastic tartrate-resistant acid phosphatase. Modulation of osteoclast adhesion in vitro. J Biol Chem 269(21):14853–14856
Ek-Rylander B, Andersson G (2010) Osteoclast migration on phosphorylated osteopontin is regulated by endogenous tartrate-resistant acid phosphatase. Exp Cell Res 316(3):443–451. doi:10.1016/j.yexcr.2009.10.019
Zhang FJ, Gao SG, Cheng L, Tian J, Xu WS, Luo W, Song Y, Yang Y, Lei GH (2012) The effect of hyaluronic acid on osteopontin and CD44 mRNA of fibroblast-like synoviocytes in patients with osteoarthritis of the knee. Rheumatol Int. doi:10.1007/s00296-011-2339-3
Matsui Y, Iwasaki N, Kon S, Takahashi D, Morimoto J, Denhardt DT, Rittling S, Minami A, Uede T (2009) Accelerated development of aging-associated and instability-induced osteoarthritis in osteopontin-deficient mice. Arthritis Rheum 60(8):2362–2371. doi:10.1002/art.24705
Morimoto J, Kon S, Matsui Y, Uede T (2010) Osteopontin; as a target molecule for the treatment of inflammatory diseases. Curr Drug Targets 11(4):494–505
Mori N, Majima T, Iwasaki N, Kon S, Miyakawa K, Kimura C, Tanaka K, Denhardt DT, Rittling S, Minami A, Uede T (2007) The role of osteopontin in tendon tissue remodeling after denervation-induced mechanical stress deprivation. Matrix Biol 26(1):42–53. doi:10.1016/j.matbio.2006.09.002
Christensen B, Nielsen MS, Haselmann KF, Petersen TE, Sorensen ES (2005) Post-translationally modified residues of native human osteopontin are located in clusters: identification of 36 phosphorylation and five O-glycosylation sites and their biological implications. Biochem J 390(Pt 1):285–292. doi:10.1042/BJ20050341
Li X, Li J, Cheng K, Lin Q, Wang D, Zhang H, An H, Gao M, Chen A (2011) Effect of low-intensity pulsed ultrasound on MMP-13 and MAPKs signaling pathway in rabbit knee osteoarthritis. Cell Biochem Biophys 61(2):427–434. doi:10.1007/s12013-011-9206-4
Acknowledgments
We thank the reviewers and the Rheumatology International (Clinical and Experimental Investigations) manuscript editorial staffs for their helpful comments that have helped to considerably improve this paper. Mai Xu has received Sports Medicine Research Fund of Central South University. Shuguang Gao is currently receiving the Young Teacher’s boosting project of the Fundamental Research Funds for the Central Universities in Central South University, National Natural Science Foundation of China (81201420). Guanghua Lei has received the National 863 project of China (2011AA030101), National Natural Science Foundation of China (81272034), the Provincial Science Foundation of Hunan, the freedom explore Program of Central South University (2012QNZT103), Distinguished Young Scientists fund of Central South university, the foundation of development and reform commission of Hunan province and National Clinical Key Department Construction Projects of China. For the remaining authors none were declared.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Xu, M., Zhang, L., Zhao, L. et al. Phosphorylation of osteopontin in osteoarthritis degenerative cartilage and its effect on matrix metalloprotease 13. Rheumatol Int 33, 1313–1319 (2013). https://doi.org/10.1007/s00296-012-2548-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00296-012-2548-4