Abstract
Purpose
To evaluate the effect of excision repair cross-complementing group 1 (ERCC1) and X-ray cross-complementing group 1 (XRCC1) gene polymorphisms on treatment outcome in patients receiving oxaliplatin-based regimens for metastatic colorectal cancer.
Methods
Hundred and thirteen patients with a diagnosis of metastatic colorectal cancer were treated with oxaliplatin-based chemotherapy. ERCC1 codon 118C/T and XRCC1 codon 399A/G polymorphisms were tested by real-time polymerase chain reaction (RT-PCR) method in peripheral blood lymphocytes of these patients. Disease control rates and survivals were compared by types of genotypes.
Results
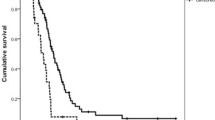
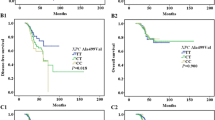
Analyses of the patterns of the polymorphism located at ERCC1 codon 118 showed that 55 (48.67%) patients were homozygous for C/C genotype, 15 (13.27%) were homozygous for the T/T genotype, and 43 (38.06%) were heterozygous for C/T genotype. Analyses of the polymorphism located at XRCC1 codon 399 showed that 61 (53.98%) patients were homozygous for A/A genotype, 13 (11.50%) were homozygous for the G/G genotype, and 39 (34.52%) were heterozygous for A/G genotype. After two cycles of chemotherapy, there was complete response (CR) in 1 patient, partial response (PR) in 24 patients, and stable disease (SD) in 56 patients. Altogether in 81 (71.68%) patients the disease was controlled after chemotherapy. Thirty-two (28.32%) patients showed disease progression. After adjusting for some clinical factors, both the ERCC1 polymorphism and the XRCC1 polymorphism lost their roles in predicting DCR (P = 0.662, P = 0.631) and MST (P = 0.692, P = 0.572). But the combination of ERCC1 and XRCC1 polymorphisms was significantly associated with DCR (P = 0.01) and MST (P = 0.000) independently.
Conclusions
This is the first study which showed that polymorphisms of ERCC1 and XRCC1, in combination not individually, were independent predictors for DCR and OS. This may contribute to the selection of patients who would benefit from oxaliplatin-based chemotherapy for metastatic colorectal cancer.



Similar content being viewed by others
References
Weitz J, Koch M, Debus J, Hohler T, Galle PR, Buchler MW (2005) Colorectal cancer. Lancet 365(9454):153–165
Midgley R, Kerr D (1999) Colorectal cancer. Lancet 353:391–399
Punt CJ (2004) New options and old dilemmas in the treatment of patients with advanced colorectal cancer. Ann Oncol 15:1453–1459
Ries LAG, Melbert D, Krapcho M et al (2007) SEER Cancer Statistics Review, 1975–2004. National Cancer Institute, Bethesda, MD. Available at http://seer.cancer.gov/csr/1975_2004/. Accessed 15 November 2007
De Gramont A, Figer A, Seymour M et al (2000) Leucovorin and fluorouracil with or without oxaliplatin as first-line treatment in advanced colorectal cancer. J Clin Oncol 18:2938–2947
Kelly H, Goldberg RM (2005) Systemic therapy for metastatic colorectal cancer: current options, current evidence. J Clin Oncol 23:4553–4560
Raymond E, Chaney SG, Taamma A et al (1998) Oxaliplatin: a review of preclinical and clinical studies. Ann Oncol 9:1053–1071
Raymond E, Faivre S, Chaney S et al (2002) Cellular and molecular pharmacology of oxaliplatin. Mol Cancer Ther 1:227–235
Rosell R, Mendez P, Isla D (2007) Platinum resistance related to a functional NER pathway. J Thorac Oncol 2(12):1063–1066
Gossage L, Madhusudan S (2007) Current status of excision repair cross complementing-group 1 (ERCC1) in cancer. Cancer Treat Rev 33(6):565–577
Fortini P, Pascucci B, Parlanti E et al (2003) The base excision repair: mechanisms and its relevance for cancer susceptibility. Biochimie 85(11):1053–1071
Horton JK, Watson M, Stefanick DF et al (2008) XRCC1 and DNA polymerase beta in cellular protection against cytotoxic DNA single-strand breaks. Cell Res 18(1):48–63
Yu JJ, Mu C, Lee KB et al (1997) A nucleotide polymorphism in ERCC1 in human ovarian cancer cell lines and tumor tissues. Mutat Res Genomics 382:13–20
Sorenson MA, Kurland CG, Pederson S et al (1989) Codon usage determines translation rate in Escherichia coli. J Mol Biol 207:365–377
Kimchi-Sarfaty C, Oh JM, Kim IW et al (2007) A “silent” polymorphism in the MDR1 gene changes substrate specificity. Science 315:525–528
Martin LP, Hamilton TC, Schilder RJ (2008) Platinum resistance: the role of DNA repair pathways. Clin Cancer Res 14(5):1291–1295
Sharma RA, Dianov GL (2007) Targeting base excision repair to improve cancer therapies. Mol Aspects Med 28(3–4):345–374
Kweekel DM, Gelderblom H, Guchelaar HJ et al (2005) Pharmacology of oxaliplatin and the use of pharmacogenomics to individualize therapy. Cancer Treat Rev 31:90–105
Yu JJ, Lee KB, Mu C et al (2000) Comparison of two human ovarian carcinoma cell lines (A2780/CP70 and MCAS) that are equally resistant to platinum, but differ at codon 118 of the ERCC1 gene. Int J Oncol 16:555–560
Kamikozuru H, Kuramochi H, Hayashi K, Nakajima G, Amamoto M (2008) ERCC1 codon 118 polymorphism is a useful prognostic marker in patients with pancreatic cancer treated with platinum-based chemotherapy. Int J Oncol 32:1091–1096
Tibaldi C, Giovannetti E, Vasile E, Mey V et al (2008) Correlation of CDA, ERCC1, and XPD polymorphisms with response and survival in capecitabine/cisplatin-treated advanced non-small cell lung cancer patients. Clin Cancer Res 14:1797–1803
Smith S, Su D, Rigault de la Longrais IA et al (2007) ERCC1 genotype and phenotype in epithelial ovarian cancer identify patients likely to benefit from paclitaxel treatment in addition to platinum-based therapy. J Clin Oncol 25(33):5172–5179
Viguier J, Boige V, Miquel C, Pocard M, Giraudeau B, Sabourin C, Ducreux M, Sarasin A, Praz F (2005) ERCC1 codon 118 polymorphism s a predictive factor for the tumor response to oxaliplatin/5-Xuorouracil combination chemotherapy in patients with advanced colorectal cancer. Clin Cancer Res 11:6212–6217
Martinez-Balibrea E, Abad A, Aranda E et al (2008) Pharmacogenetic approach for capecitabine or 5-Xuorouracil selection to be combined with oxaliplatin as first-line chemotherapy in advanced colorectal cancer. Eur J Cancer 44:1229–1237
Ruzzo A, Graziano F, Loupakis F et al (2007) Pharmacogenetic profiling in patients with advanced colorectal cancer treated with first-line FOLFOX-4 chemotherapy. J Clin Oncol 25(10):1247–1254
Lindahl T, Lood RD (1999) Quality control by DNA repair. Science 286:1897–1905
Stoehlmacher J, Park DJ, Zhang W, Yang D, Groshen S, Zahedy S, Lenz H-J (2004) A multivariate analysis of genomic polymorphisms: prediction of clinical outcome to 5-FU/oxaliplatin combination chemotherapy in refractory colorectal cancer. Br J Cancer 91:344–354
Liu B, Wei J, Zou Z, Qian X, Nakamura T, Zhang W, Ding Y, Feng J, Yu L (2007) Polymorphism of XRCC1 predicts overall survival of gastric cancer patients receiving oxaliplatin-based chemotherapy in Chinese population. Eur J Hum Genet 15:1049–1053
Colhoun HM, McKeigue PM, Davey Smith G et al (2003) Problems of reporting genetic associations with complex outcomes. Lancet 361:865–872
Huang ZH, Hua D, Du X et al (2009) Polymorphisms in p53, GSTP1 and XRCC1 predict relapse and survival of gastric cancer patients treated with oxaliplatin-based adjuvant chemotherapy. Cancer Chemother Pharmacol 64(5):1001–1007
Li WQ, Zhang L, Ma JL et al (2009) Association between genetic polymorphisms of DNA base excision repair genes and evolution of precancerous gastric lesions in a Chinese population. Carcinogenesis 30(3):500–505
Kim HS, Kim MK, Chung HH et al (2009) Genetic polymorphisms affecting clinical outcomes in epithelial ovarian cancer patients treated with taxanes and platinum compounds: a Korean population-based study. Gynecol Oncol 113:264–269
Improta G, Sgambato A, Bianchino G et al (2008) Polymorphisms of the DNA repair genes XRCC1 and XRCC3 and risk of lung and colorectal cancer: a case–control study in a Southern Italian population. Anticancer Res 28(5B):2941–2946
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Liang, J., Jiang, T., Yao, Ry. et al. The combination of ERCC1 and XRCC1 gene polymorphisms better predicts clinical outcome to oxaliplatin-based chemotherapy in metastatic colorectal cancer. Cancer Chemother Pharmacol 66, 493–500 (2010). https://doi.org/10.1007/s00280-009-1186-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00280-009-1186-3