Abstract
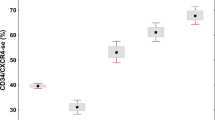
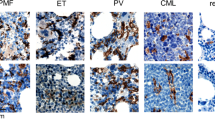
A high number of circulating CD34+ cells has been advocated to distinguish primary myelofibrosis from other Philadelphia-negative myeloproliferative neoplasms. We re-evaluated the diagnostic interest of measuring circulating CD34+ cells in 26 healthy volunteers and 256 consecutive patients at diagnosis for whom a myeloproliferative neoplasm was suspected. The ROC curve analysis showed that a number of CD34+ <10/μl excludes the diagnosis of primary myelofibrosis with a sensitivity of 97 % and a specificity of 90 % (area under the curve: 0.93 [0.89–0.98]; p < 0.001). Patients with PMF harboring a CALR mutation had more circulating CD34+ cells than patients with either a JAK 2 or MPL mutation (p = 0.02 and p < 0.01, respectively). These results suggest that this fast, simple, non-invasive, and standardized test is of particular interest to exclude the diagnosis of primary myelofibrosis.


Similar content being viewed by others
References
Barosi G, Viarengo G, Pecci A et al (2001) Diagnostic and clinical relevance of the number of circulating CD34 (+) cells in myelofibrosis with myeloid metaplasia. Blood 98:3249–3255
Andréasson B, Swolin B, Kutti J (2002) Patients with idiopathic myelofibrosis show increased CD34+ cell concentrations in peripheral blood compared to patients with polycythaemia vera and essential thrombocytopenia. Eur J Haematol 68:189–193
Passamonti F, Vanelli L, Malabarba L et al (2003) Clinical utility of the absolute number of circulating CD34-positive cells in patients with chronic myeloproliferative disorders. Haematologica 88:1123–1129
Arora B, Sirhan S, Hoyer JD, Mesa RA, Tefferi A (2005) Peripheral blood CD34 count in myelofibrosis with myeloid metaplasia: a prospective evaluation of prognostic value in 94 patients. Br J Haematol 128:42–48
Arber DA, Orazi A, Hasserjian R et al (2016) The 2016 revision to the World Health Organization classification of myeloid neoplasms and acute leukemia. Blood 127:2391–2405
Klampfl T, Gisslinger H, Harutyunyan AS et al (2013) Somatic mutations of calreticulin in myeloproliferative neoplasms. N Engl J Med 369:2379–2390
Nangalia J, Massie CE, Baxter EJ et al (2013) Somatic CALR mutations in myeloproliferative neoplasms with nonmutated JAK2. N Engl J Med 369:2391–2405
Tefferi A, Thiele J, Vannucchi AM, Barbui T (2014) An overview on CALR and CSF3R mutations and a proposal for revision of the WHO diagnostic criteria for myeloproliferative neoplasms. Leukemia 28:1407–1413
Dobo I, Boiret N, Lippert E et al (2004) A standardized endogenous megakaryocytic erythroid colony assay for the diagnosis of essential thrombocythemia. Haematologica 89:1207–1212
Rumi E, Pietra D, Pascutto C et al (2014) Clinical effect of driver mutations of JAK2, CALR, or MPL in primary myelofibrosis. Blood 124:1062–1069
Tefferi A, Guglielmelli P, Larson DR et al (2014) Long-term survival and blast transformation in molecularly annotated essential thrombocythemia, polycythemia vera, and myelofibrosis. Blood 124:2507–2513
Massa M, Rosti V, Ramajoli I et al (2005) Circulating CD34+, CD133+, and vascular endothelial growth factor receptor 2-positive endothelial progenitor cells in myelofibrosis with myeloid metaplasia. J Clin Oncol 23:5688–5695
Pietra D, Rumi E, Ferretti VV et al (2016) Differential clinical effects of different mutation subtypes in CALR-mutant myeloproliferative neoplasms. Leukemia 30:431–438
Acknowledgments
We thank the technicians from both centers for their help.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The study was performed in accordance with institutional ethical guidelines and the Declaration of Helsinki.
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
C. Orvain and D. Luque Paz contributed equally to this work.
Rights and permissions
About this article
Cite this article
Orvain, C., Luque Paz, D., Dobo, I. et al. Circulating Cd34+ cell count differentiates primary myelofibrosis from other Philadelphia-negative myeloproliferative neoplasms: a pragmatic study. Ann Hematol 95, 1819–1823 (2016). https://doi.org/10.1007/s00277-016-2784-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00277-016-2784-x