Abstract
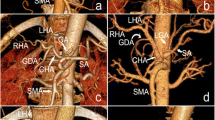
In modern surgical and transplantation procedures the recognition of anatomic vascular abnormalities of the hepatic arteries is of greater importance than ever. The purpose of this study was to evaluate and classify these variations with respect to their impact on visceral surgery. A total of 604 selective celiac and superior mesenteric angiographies performed on patients with known or suspected liver cirrhosis or hepatic or pancreatic malignancies and on donors of partial liver grafts were analyzed retrospectively. The vascular anatomy of the liver was classified according to different established systems and with particular attention to rare variations. Hepatic arterial anatomy as considered normal in textbook descriptions was found in 79.1%, an aberrant or accessory left hepatic artery (LHA) arising from the left gastric artery in 3.0% and an aberrant or accessory right hepatic artery (RHA) branching off the superior mesenteric artery in 11.9% of the cases. In 1.4% of the cases there was a combination of anomalies of both the LHA and RHA. Variants of the celiac trunk, double hepatic arteries branching at the celiac trunk or hepatic arteries arising directly from the aorta, occurred in 4.1% of the cases. Further atypical branches of the LHA and RHA were found in 0.5% of the cases. Since the incidence and pattern of different types of hepatic arterial anatomy can require specialized preoperative diagnostic as well as intraoperative strategies, knowledge of these abnormalities and their frequency is of major importance for the surgeon as well as the radiologist.


Similar content being viewed by others
References
Adachi B (1928) Das Arteriensystem der Japaner. Kenkyusha Press, Kyoto
Browne EZ (1940) Variations in origin and course of the hepatic artery and its branches. Surgery 8: 424–445
Chen CY, Lee RC, Tseng HS, Chiang JH, Hwang JI, Teng MMH (1998) Normal and variant anatomy of hepatic arteries: Angiographic experience. Chin Med J 61: 17–23
Chevallier JM, Hannoun L (1991) Anatomic bases for liver transplantation. Surg Radiol Anat 13: 7-16
Daly JM, Kemeny N, Oderman P, Botet J (1984) Long-term hepatic arterial infusion chemotherapy. Arch Surg 119: 936–941
Daseler EH, Anson BY, Hambley WC, Reimann AF (1947) The cystic artery and constituents of the hepatic pedicle. Surg Gynecol Obstet 85: 47–63
Decurtins M, Friend PJ, Calne RY (1987) Incidence and outcome of donor arterial anomalies in liver allografts. Transplant Proc 19: 2394–2395
De Santis M, Ariosi P, Calo GF, Romagnoli R (2000) Anatomia vascolare arteriosa epatica e sue varianti. Radiol Med 100: 145–151
Douard R, Ettorre GM, Sommacale D, Jan D, Révillon Y, Farges O, Belghiti J (2002) A two-step strategy for enlargement of left arterial branch in a living related liver graft with dual arterial supply. Transplantation 73: 993–994
Fasel JHD, Muster M, Gailloud P, Mentha G, Terrier F (1996) Duplicated hepatic artery: Radiologic and surgical implications. Acta Anat 157: 164–168
Gupta SC, Gupta CD, Gupta SB (1979) Intrahepatic supply pattern in cases of double hepatic arteries: A study by corrosion casts. Anat Anz 146: 166–170
Haller A (1756) Icones anatomicae in quibus aliquae partes corporis humani delineatae proponuntur et arteriarum potissimum historia continetur. Vandenhoeck, Göttingen
Hiatt JR, Gabbay J, Busuttil RW (1994) Surgical anatomy of the hepatic arteries in 1000 cases. Ann Surg 220: 50–52
Ikegami T, Kawasaki S, Matsunami H, Hashikura Y, Nakazawa Y, Miyagawa S, Furuta S, Iwanaka T, Makuuchi M (1996) Should all hepatic arterial branches be reconstructed in living-related liver transplantation? Surgery 119: 431–436
Jurim O, Shaked A, Kianusch K, Millis JM, Colquhoun SD, Busuttil RW (1993) Celiac compression syndrome and liver transplantation. Ann Surg 218: 10–12
Kemeny MM, Hogan JM, Goldberg DA, Lieu C, Beatty D, Kokal WA, Riihimaki DU, Terz JJ (1986) Continuous hepatic artery infusion with an implantable pump: problems with hepatic artery anomalies. Surgery 99: 501–504
Koehler RE, Korobkin M, Lewis E (1997) Arteriographic demonstration of collateral supply to the liver after hepatic arterial ligation. Radiology 177: 49
Krupski G, Rogiers X, Nicolas V, Berdien E, Maas R., Malagó M, Broelsch CE, Bücheler E (1997) Die Bedeutung der arteriellen Gefäßversorgung von Segment IV bei der Leberlebendspende. Fortschr Rontgenstr 167: 32–36
Kubota K, Makuuchi M, Takayama T, Harihara Y, Hasegawa K, Aoki T, Asato H, Kawarasaki H (2000) Simple test on the back table for justifying single hepatic-arterial reconstruction in living related liver transplantation. Transplantation 70: 696–697
Lippert H, Pabst R (1985) Arterial variations in man: classification and frequency. Bergmann, Munich
Lunderquist A (1967) Arterial segmental supply of the liver. Acta Radiol Stockh Suppl 272
Mäkisalo H, Chaib E, Krokos N, Calne R (1993) Hepatic arterial variations and liver-related diseases of 100 consecutive donors. Transplant Int 6: 325–329
Mays ET, Wheeler CS (1974) Demonstration of collateral arterial flow after interruption of hepatic arteries in man. N Engl J Med 290: 993
Michels NA (1966) Newer anatomy of the liver and its variant blood supply and collateral circulation. Am J Surg 112: 337–347
Miyaki T, Sakagami S, Ito H (1989) Intrahepatic territory of the accessory hepatic artery in human. Acta Anat 136: 34–37
Mori K, Nagata I, Yamagata S, Sasaki H, Nishizawa F, Takada Y, Mariyasu F, Tanaka K, Yamaoka Y, Kumada K, Kikuchi H, Ozawa K (1992) The introduction of microvascular surgery to hepatic artery reconstruction in living-related liver transplantation: its surgical advantages compared with conventional procedures. Transplantation 54: 263–268
Niederhuber JE, Ensminger WD (1983) Surgical considerations in the management of hepatic neoplasia. Semin Oncol 10: 135–147
Noah EM, Klinzing S, Zwaan M, Schramm U, Bruch HP, Weiss HD (1995) Normvarianten der arteriellen Leberversorgung in Mesenterico-Coeliacographien. Ann Anat 177: 305–312
Ödman P (1958) Percutaneous selective angiography of the celiac artery. Acta Radiol Stockh Suppl 159
Reimann B, Lierse W, Schreiber HW (1983) Anastomosen zwischen Segmentarterien der Leber und phrenicohepatische arterio-arterielle Anastohmosten. Langenbecks Arch Chir 359: 81
Rong GH, Sindelar WF (1987) Aberrant peripancreatic arterial anatomy. Considerations in performing pancreatectomy for malignant neoplasms. Am Surg 53: 726–729
Rygaard H, Forrest M, Mygind T, Baden H (1986) Anatomic variants of the hepatic arteries. Acta Radiol Diagn 27: 425–427
Scott-Conner CEH, Hall TJ (1992) Variant arterial anatomy in laparoscopic cholecystectomy. Am J Surg 163: 590–592
Soin AS, Friend PJ, Rasmussen A, Saxena R, Tokat Y, Alexander GJM, Jamieson NV, Calne RY (1996) Donor arterial variations in liver transplantation: management and outcome of 527 consecutive grafts. Br J Surg 83: 637–641
Suzuki T, Nakayasu A, Kawabe K, Takeda H, Honjo I (1971) Surgical significance of anatomic variations of the hepatic artery. Am J Surg 122: 505–512
Todo S, Makowka L, Tzakis AG, Marsh JW, Karrer FM, Armany M, Miller C, Tallent MB, Esquivel CO, Gordon RD, Iwatsuki S, Starzl TE (1987) Hepatic artery in liver transplantation. Transplant Proc 19: 2406–2411
Tzakis AG, Gordon RD, Shaw BW, Iwatsuki S, Stanzl TE (1985) Clinical presentation of hepatic artery thrombosis after liver transplantation in the cyclosporine era. Transplantation 40: 667
Vandamme JPJ, Bonte J, van der Schueren G (1969) A revaluation of hepatic and cystic arteries: the importance of the aberrant hepatic branches. Acta Anat 73: 192–209
Weiglein AH (1996) Variations and topography of the arteries in the lesser omentum in humans. Clin Anat 9: 143–150
Weimann A, Meyer HJ, Mauz S, Ringe B, Jähne J, Pichlmayr R (1991) Anatomische Verlaufsvariationen der Arteria hepatica sinistra: ein Problem für die systematische Lymphadenektomie bei Gastrektomie oder proximaler Magenresektion vor Magenschlauchbildung. Chirurg 62: 552–556
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Koops, A., Wojciechowski, B., Broering, D.C. et al. Anatomic variations of the hepatic arteries in 604 selective celiac and superior mesenteric angiographies. Surg Radiol Anat 26, 239–244 (2004). https://doi.org/10.1007/s00276-004-0229-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00276-004-0229-z