Abstract
Purpose
A prospective multicenter phase I/II trial was performed to evaluate the clinical safety and efficacy of radiofrequency ablation (RFA) for metastatic bone tumors.
Materials and Methods
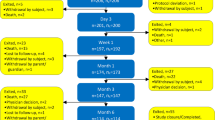
Thirty-three patients (27 men, 6 women, mean age 61 years) with metastatic bone tumors were enrolled. In phase I, nine patients were enrolled, and the safety of RFA was evaluated. In phase II, 23 patients were included, and an intent-to-treat analysis was performed. The primary endpoint was to evaluate the treatment’s safety. The secondary endpoint was to evaluate the efficacy of pain relief at 1 week after RFA.
Results
RFA was performed in 32 of 33 enrolled patients. No serious complications were observed during the phase I, so phase II was performed. Four patients exhibited adverse events, including one case each of Grade 3 pain and, Grade 2 hypotension, and one patient developed Grade 1 burns at the grounding pad and puncture site. One patient died of liver failure on day 7 after RFA due to the progression of the primary lesion. The efficacy was excellent (no increase in analgesic dosage, post-RFA VAS score of 0–2 or decreased by not less than 5 compared to before RFA) in 20 patients (60.6%), good (no increase in analgesic dosage, post-RFA VAS score decreased by not less than 2 but by < 5 compared to before RFA) in 3 (9.1%), and poor in 10 patients (30.3%). Thus, the response rate was 69.7%.
Conclusion
RFA is a safe and effective method for treating painful metastatic bone tumors.


Similar content being viewed by others
References
McGahan JP, Browning PD, Brock JM, et al. Hepatic ablation using radiofrequency electrocautery. Invest Radiol. 1990;25:267–70.
Rossi S, Di Stasi M, Buscarini E, et al. Percutaneous RF interstitial thermal ablation in the treatment of hepatic cancer. AJR. 1996;167:759–68.
Rossi S, Buscarini E, Garbagnati F, et al. Percutaneous treatment of small hepatic tumors by an expandable RF needle electrode. AJR. 1998;170:1015–22.
Livraghi T, Goldberg SN, Lazzaroni S, et al. Small hepatocellular carcinoma: treatment with radio-frequency ablation versus ethanol injection. Radiology. 1999;210:655–61.
Curley SA, Izzo F, Ellis LM, et al. Radiofrequency ablation of hepatocellular cancer in 110 patients with cirrhosis. Ann Surg. 2000;232:381–91.
Tong D, Gillick L, Hendrickson FR. The palliation of symptomatic osseous metastases: final results of the study the radiation therapy oncology group. Cancer. 1982;50:893–9.
Ratanatharathon V, Powers WE, Moss WT, Peres CA. Bone metastasis: review and critical analysis of random allocation trials of local field treatment. Int J Radiat Oncol Phys. 1999;44:1–18.
Di Staso M, Zugaro L, Gravina GL, et al. A feasibility study of percutaneous radiofrequency ablation followed by radiotherapy in the management of painful osteolytic bone metastases. Eur Radiol. 2011;21:2004–10.
Dupuy DE, Zagoria RJ, Akerley W, et al. Percutaneous radiofrequency ablation of malignancies in the lung. AJR. 2000;174:57–9.
Putnam JB Jr. New and evolving treatment methods for pulmonary metastases. Semin Thorac Cardiovasc Surg. 2002;14:49–56.
Barei DP, Moreau G, Scarborough MT, et al. Percutaneous radiofrequency ablation of osteoid osteoma. Clin Orthop Relat Res. 2000;373:115–24.
Izzo F, Thomas R, Delrio P, et al. Radiofrequency ablation in patients with primary breast carcinoma. Cancer. 2001;92:2036–44.
Dupuy DE, Fernando HC, Hillman S, et al. Radiofrequency ablation of stage IA non-small cell lung cancer in medically inoperable patients: results from the American College of Surgeons Oncology Group Z4033 (Alliance) trial. Cancer. 2015;121:3491–8.
Mimura H, Arai Y, Yamakado K, et al. Phase I/II study of radiofrequency ablation for malignant renal tumors: Japan interventional radiology in Oncology Study Group 0701. Cardiovasc Intervent Radiol. 2016;39:717–23.
Miyazaki M, Arai Y, Myoui A, et al. Phase I/II multi-institutional study of percutaneous radiofrequency ablation for painful osteoid osteoma (JIVROSG-0704). Cardiovasc Intervent Radiol. 2016;39:1464–70.
Goetz MP, Callstrom MR, Chaboneau JW, et al. Percutaneous image-guided radiofrequency ablation of painful metastases involving bone: a multicenter study. J Clin Oncol. 2004;22(2):300–6.
Kobayashi T, Arai Y, Takeuchi Y, et al. Phase I/II clinical study of percutaneous vertebroplasty (PVP) as palliation for painful malignant vertebral compression fractures (PMVCF): JIVROSG-0202. Ann Oncol. 2009;20:1943–7.
Cancer Therapy Evaluation Program. Common toxicity criteria, version 2.0.1998. http://ctep.cancer.gov/protocolDevelopment/electronic_applications/docs/ctcv20_4-30-992.pdf. Accessed 15 April 2009.
Callstrom MR, Dupuy DE, Solomon SB, et al. Percutaneous image-guided cryoablation of painful metastases involving bone: multicenter trial. Cancer. 2013;119:1033–41.
Nakatsuka A, Yamakado K, Maeda M, et al. Radiofrequency ablation combined with bone cement injection for the treatment of bone malignancies. J Vasc Interv Radiol. 2004;15:707–12.
Toyota N, Naito A, Kakizawa H, et al. Radiofrequency ablation therapy combined with cementoplasty for painful bone metastases: initial experience. Cardiovasc Intervent Radiol. 2005;28:578–83.
Kojima H, Tanigawa N, Kariya S, et al. Clinical assessment of percutaneous radiofrequency ablation for painful metastatic bone tumors. Cardiovasc Interv Radiol. 2006;29:1022–6.
Callstrom MR, Charboneau JW, Goetz MP, et al. Painful metastases involving bone: feasibility of percutaneous CT- and US-guided radio-frequency ablation. Radiology. 2002;224:87–97.
Acknowledgements
This research was supported by the Practical Research for Innovative Cancer Control (16ck0106058h0003) from the Japan Agency for Medical Research and Development (AMED), Health and Labor Sciences Research Grant (H26-055) from the Ministry of Health, Labour and Welfare of Japan, and the National Cancer Center Research and Development Fund (26-A-27).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical Approval
The ethics committee of the Japanese Society of Interventional Radiology and the Institutional Review Board from each participating hospital approved the study protocol prior to patient entry. All of the patients provided written informed consent.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Tanigawa, N., Arai, Y., Yamakado, K. et al. Phase I/II Study of Radiofrequency Ablation for Painful Bone Metastases: Japan Interventional Radiology in Oncology Study Group 0208. Cardiovasc Intervent Radiol 41, 1043–1048 (2018). https://doi.org/10.1007/s00270-018-1944-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-018-1944-x