Abstract
Purpose
To study if <30 % residual stenosis post angioplasty (PTA) correlates with primary access circuit patency, and if any variables predict technical success.
Materials and Methods
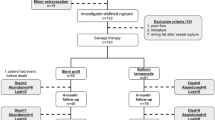
A prospective observational study was performed between January 2009 and December 2012, wherein 76 patients underwent 154 PTA events in 56 prosthetic grafts (AVG) and 98 autogenous fistulas (AVF). Data collected included patient age, gender, lesion location and laterality, access type and location, number of prior interventions, and transonic flow rates pre- and postintervention. Impact of technical outcome on access patency was assessed. Univariate logistic regression was used to assess the impact of variables on technical success with significant factors assessed with a multiple variable model.
Results
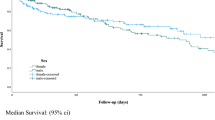
Technical success rates of PTA in AVFs and AVGs were 79.6 and 76.7 %, respectively. Technical failures of PTA were associated with an increased risk of patency loss among circuits with AVFs (p < 0.05), but not with AVGs (p = 0.7). In AVFs, primary access patency rates between technical successes and failures at three and 6 months were 74.4 versus 61.9 % (p = 0.3) and 53.8 versus 23.8 % (p < 0.05), respectively. In AVGs, primary access patency rates between technical successes and failures at three and six months were 72.1 versus 53.9 % (p = 0.5) and 33.6 versus 38.5 % (p = 0.8), respectively. Transonic flow rates did not significantly differ among technically successful or failed outcomes at one or three months.
Conclusion
Technical failures of PTA had a significant impact on access patency among AVFs with a trend toward poorer access patency within AVGs.

Similar content being viewed by others
Abbreviations
- CI:
-
Confidence interval
- KDOQI:
-
Kidney disease outcomes quality initiative
- SIR:
-
Society of interventional radiology
References
Aftab SA, Tay KH, Irani FG, Gong Lo RH, Gogna A, Haaland B, et al. Randomized clinical trial of cutting balloon angioplasty versus high-pressure balloon angioplasty in hemodialysis arteriovenous fistula stenoses resistant to conventional balloon angioplasty. J Vasc Interv Radiol. 2014;25(2):190–8.
Ahya SN, Windus DW, Vesely TM. Flow in hemodialysis grafts after angioplasty: Do radiologic criteria predict success? Kidney Int. 2001;59(5):1974–8.
Aruny JE, Lewis CA, Cardella JF, Cole PE, Davis A, Drooz AT, et al. Quality improvement guidelines for percutaneous management of the thrombosed or dysfunctional dialysis access. Standards of Practice Committee of the Society of Cardiovascular & Interventional Radiology. J Vasc Interv Radiol. 1999;10(4):491–8.
Gray RJ, Sacks D, Martin LG, Trerotola SO. Reporting standards for percutaneous interventions in dialysis access. Technology Assessment Committee. [see comments]. J Vasc Interv Radiol. 1999;10(10):1405–15.
Haskal ZJ, Trerotola S, Dolmatch B, Schuman E, Altman S, Mietling S, et al. Stent graft versus balloon angioplasty for failing dialysis-access grafts. N Engl J Med. 2010;362(6):494–503.
Turmel-Rodrigues L, Pengloan J, Baudin S, Testou D, Abaza M, Dahdah G, et al. Treatment of stenosis and thrombosis in haemodialysis fistulas and grafts by interventional radiology. Nephrol Dial Transplant. 2000;15(12):2029–36.
Kanterman RY, Vesely TM, Pilgram TK, Guy BW, Windus DW, Picus D. Dialysis access grafts: anatomic location of venous stenosis and results of angioplasty. [Erratum appears in Radiology 1995 Aug; 196(2):582]. Radiology. 1995;195(1):135–9.
Safa AA, Valji K, Roberts AC, Ziegler TW, Hye RJ, Oglevie SB. Detection and treatment of dysfunctional hemodialysis access grafts: effect of a surveillance program on graft patency and the incidence of thrombosis. Radiology. 1996;199(3):653–7.
Turmel-Rodrigues L, Pengloan J, Blanchier D, Abaza M, Birmele B, Haillot O, et al. Insufficient dialysis shunts: improved long-term patency rates with close hemodynamic monitoring, repeated percutaneous balloon angioplasty, and stent placement. Radiology. 1993;187(1):273–8.
Aktas A, Bozkurt A, Aktas B, Kirbas I. Percutaneous transluminal balloon angioplasty in stenosis of native hemodialysis arteriovenous fistulas: technical success and analysis of factors affecting postprocedural fistula patency. Diagn Interv Radiol. 2015;21(2):160–6.
Rajan DK, Sidhu A, Noel-Lamy M, Mahajan A, Simons ME, Sniderman KW, et al. Elastic recoil after balloon angioplasty in hemodialysis accesses: does it actually occur and is it clinically relevant? Radiology. 2015;279(3):961–7.
Clark TW, Hirsch DA, Jindal KJ, Veugelers PJ, LeBlanc J. Outcome and prognostic factors of restenosis after percutaneous treatment of native hemodialysis fistulas. J Vasc Interv Radiol. 2002;13(1):51–9.
Heye S, Maleux G, Vaninbroukx J, Claes K, Kuypers D, Oyen R. Factors influencing technical success and outcome of percutaneous balloon angioplasty in de novo native hemodialysis arteriovenous fistulas. Eur J Radiol. 2012;81(9):2298–303.
Rajan DK, Bunston S, Misra S, Pinto R, Lok CE. Dysfunctional autogenous hemodialysis fistulas: outcomes after angioplasty—are there clinical predictors of patency? Radiology. 2004;232(2):508–15.
Vesely TM, Siegel JB. Use of the peripheral cutting balloon to treat hemodialysis-related stenoses. J Vasc Interv Radiol. 2005;16(12):1593–603.
Elramah M, Boujelbane L, Yevzlin AS, Wakeen M, Astor BC, Chan MR. Dialysis access venous stenosis: treatment with balloon angioplasty 30-second vs. 1-minute inflation times. Hemodial Int. 2015;19(1):108–14.
Forauer AR, Hoffer EK, Homa K. Dialysis access venous stenoses: treatment with balloon angioplasty–1- versus 3-minute inflation times. Radiology. 2008;249(1):375–81.
Lin YS, Yang CH, Chu CM, Fang CY, Chen CJ, Hsu JT, et al. The role of postintervention pullback pressure gradient in percutaneous transluminal angioplasty for central vein stenosis in dialysis patients. Cardiovasc Intervent Radiol. 2013;36(5):1296–305.
Goyal A, Orth RC, Parekh RS, Wolfson T, Gamst A, Kuo MD. Endpoints for hemodialysis access procedures: correlation between fistulography and intraaccess blood flow measurements. J Vasc Interv Radiol. 2011;22(12):1733–9.
Leontiev O, Mondschein JI, Dagli MS, Clark TW, Soulen MC, Stavropoulos SW, et al. Catheter-based intraaccess blood flow measurement as a problem-solving tool in hemodialysis access intervention. J Vasc Interv Radiol. 2013;24(5):717–21.
Acknowledgments
We thank William S. Harmsen for his statistical analysis of the data.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
All authors declare that they have no relevant conflicts of interest or financial disclosures.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Sidhu, A., Tan, K.T., Noel-Lamy, M. et al. Does Technical Success of Angioplasty in Dysfunctional Hemodialysis Accesses Correlate with Access Patency?. Cardiovasc Intervent Radiol 39, 1400–1406 (2016). https://doi.org/10.1007/s00270-016-1401-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-016-1401-7