Abstract
Purpose
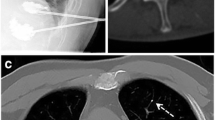
To compare safety and efficacy of percutaneous vertebroplasty (PVP) when treating up to three vertebrae or more than three vertebrae per session.
Materials and Methods
We prospectively compared two groups of patients with symptomatic vertebral fractures who had no significant response to conservative therapy. Pathologic substrate included osteoporosis (n = 77), metastasis (n = 24), multiple myeloma (n = 13), hemangioma (n = 15), and lymphoma (n = 1). Group A patients (n = 94) underwent PVP of up to three treated vertebrae (n = 188). Group B patients (n = 36) underwent PVP with more than three treated vertebrae per session (n = 220). Decreased pain and improved mobility were recorded the day after surgery and at 12 and 24 months after surgery per clinical evaluation and the use of numeric visual scales (NVS): the Greek Brief Pain Inventory, a linear analogue self-assessment questionnaire, and a World Health Organization questionnaire.
Results
Group A presented with a mean pain score of 7.9 ± 1.1 NVS units before PVP, which decreased to 2.1 ± 1.6, 2.0 ± 1.5 and 2.0 ± 1.5 NVS units the day after surgery and at 12 and 24 months after surgery, respectively. Group B presented with a mean pain score of 8.1 ± 1.3 NVS units before PVP, which decreased to 2.2 ± 1.3, 2.0 ± 1.5, and 2.1 ± 1.6 NVS units the day after surgery and at 12 and 24 months after surgery, respectively. Overall pain decrease and mobility improvement throughout the follow-up period presented no statistical significance neither between the two groups nor between different underlying aetiology. Reported cement leakages presented no statistical significance between the two groups (p = 0.365).
Conclusion
PVP is an efficient and safe technique for symptomatic vertebral fractures independently of the vertebrae number treated per session.



Similar content being viewed by others
References
Riggs BL, Meltron LJ III (1995) The worldwide problem of osteoporosis: insights afforded by epidemiology. Bone 17(Suppl 5):505S–511S
Silverman SL (1992) The clinical consequences of vertebral compression fracture. Bone 13(Suppl 2):27–31
Jensen ME, Evans AJ, Mathis JM, Kallmes DF, Cloft HJ, Dion JE (1997) Percutaneous polymethylmethacrylate vertebroplasty in the treatment of osteoporotic vertebral compression fractures: technical aspects. Am J Neuroradiol 18:1897–1904
Mathis JM, Barr JD, Belkoff SM, Barr MS, Jensen ME, Deramond H (2001) Percutaneous vertebroplasty: a developing standard of care for vertebral compression fractures. Am J Neuroradiol 22:373–381
Cortet B, Cotten A, Boutry N et al (1999) Percutaneous vertebroplasty in the treatment of osteoporotic vertebral compression fractures: an open prospective study. J Rheumatol 26(10):2222–2228
Cook DJ, Guyatt GH, Adachi JD, Clifton J, Griffith LE, Epstein RS et al (1993) Quality of life issues in women with vertebral fractures due to osteoporosis. Arthritis Rheum 36(6):750–756
Gold DT (1996) The clinical impact of vertebral fractures: quality of life in women with osteoporosis. Bone 18(Suppl 3):185–189
Schlaich C, Minne HW, Bruckner T, Wagner G, Gebest HJ, Grunze M et al (1998) Reduced pulmonary function in patients with spinal osteoporotic fractures. Osteoporos Int 8(3):261–267
Kado DM, Browner WS, Palermo L, Nevitt MC, Genant HK, Cummings SR (1999) Vertebral fractures and mortality in older women: a prospective study. Arch Intern Med 159(11):1215–1220
Amar AP, Larsen DW, Esnaashari N, Albuquerque FC, Lavine SD, Teitelbaum GP (2001) Percutaneous transpedicular polymethylmethacrylate vertebroplasty for the treatment of spinal compression fractures. Neurosurgery 49(5):1105–1114
Galibert P, Deramond H, Rosat P, Le Gars D (1087) Preliminary note on the treatment of vertebral angioma by percutaneous acrylic vertebroplasty. Neurochirurgie 33:166–168
Gangi A, Sabharwal T, Irani F et al (2006) Quality assurance guidelines for percutaneous vertebroplasty. Cardiovasc Intervent Radiol 29:173–178
McGraw JK, Candella J, Barr JD et al (2003) Society of Interventional Radiology Quality Improvement Guidelines for Percutaneous Vertebroplasty. J Vasc Interv Radiol 14:827–831
Mystekidou K, Mendoza T, Tsilika E et al (2001) Greek brief pain inventory: validation and utility in cancer pain. Oncology 60:35–42
Cleeland CS (1989) Measurement of pain by subjective report. In: Chapman LJ, Loeser JD (eds) Advances in pain research and therapy, vol 12. Raven Press, New York, pp 391–403
Doyle D, Hans GWC, MacDonald N (1995) Pain assessment and cancer pain syndromes. In: Oxford textbook of palliative medicine. Oxford University Press, Oxford, p 148
Mendoza T, Chen C, Brugger A et al (2004) The utility and validity of the modified brief pain inventory in a multiple-dose postoperative analgesic trial. Clin J Pain 20(5):357–362
Coates A, Dillenbeck CF, McNeil DR et al (1983) Linear analogue self-assessment (LASA) in evaluation of aspects of quality of life of cancer patients receiving therapy. Eur J Clin Oncol 19:1633–1637
Gough IR, Furnival CM, Schilder L, Grove W (1983) Assessment of the quality of life of patients with advanced cancer. Eur J Clin Oncol 19(8):1161–1165
Hurny C, Bernhard J, Coates A et al (1996) Responsiveness of a single-item indicator versus a multi-item scale: assessment of the emotional well-being in an international adjuvant breast cancer trial. Med Care 34(3):234–248
Padilla GV, Grant MM, Ferrell BR, et al. (1996) Quality of life—Cancer. In: Spiker B (ed) Quality of life and pharmacoeconomics in clinical trials, 2nd edn. Lippincott-Raven, Philadelphia
Roila F, Lupatteli M, Basurto C et al (1991) Intra and interobserver variability in cancer patients’ performance status assessed according to Karnofsky and ECOG scales. Ann Oncol 2(6):437–439
Oken MM, Creech RH, Tormey DC et al (1982) Toxicity and response criteria of the Eastern Cooperative Oncology Group. Am J Clin Oncol 5:649–655
Anselmetti GC, Corrao G, Monica PD et al (2007) Pain relief following percutaneous vertebroplasty: Results of a series of 283 consecutive patients treated in a single institution. Cardiovasc Interv Radiol 30(3):441–447
McGraw JK, Lippert J, Minkus K et al (2002) Prospective evaluation of pain relief in 100 patients undergoing percutaneous vertebroplasty. J Vasc Interv Radiol 13:883–886
Zoarski GH, Snow P, Olan WJ et al (2002) Percutaneous vertebroplasty for osteoporotic compression fractures: quantitative prospective evaluation of long term outcomes. J Vasc Interv Radiol 13:139–148
Singh AK, Pilgram TK, Gilula LA (2006) Osteoporotic compression fractures: outcomes after single- versus multiple-level percutaneous vertebroplasty. Radiology 238:211–220
Voormolen MH, Lohle PN, Lampmann LE, van den Wildenberg W, Juttmann JR, Diekerhof CH et al (2006) Prospective clinical follow-up after percutaneous vertebroplasty in patients with painful osteoporotic vertebral compression fractures. J Vasc Interv Radiol 17(8):1313–1320
Weill A, Chiras J, Simon JM et al (1996) Spinal metastases: indications for and results of percutaneous injection of acrylic surgical cement. Radiology 199(1):241–247
Cotten A, Dewatre F, Cortet B et al (1996) Percutaneous vertebroplasty for osteolytic metastases and myeloma: effects of the percentage of lesion filling and the leakage of methyl methacrylate at the clinical follow-up. Radiology 200:525–530
Shimony JS, Gilula LA, Zeller AJ, Brown DB (2004) Percutaneous vertebroplasty for malignant compression fractures with epidural involvement. Radiology 232:846–853
Barr JD, Barr MS, Lemley TJ, McCann RM (2000) Percutaneous vertebroplasty for pain relief and spinal stabilization. Spine 25(8):923–928
Murphy KJ, Deramond H (2000) Percutaneous vertebroplasty in benign and malignant disease. Neuroimaging Clin N Am 10(3):535–545
Hulme PA, Krebs J, Ferguson SJ, Berlemann U (2006) Vertebroplasty and kyphoplasty: a systematic review of 69 clinical studies. Spine 31(17):1983–2001
Layton KF, Thielen KR, Koch CA, Luetmer PH, Lane JI, Wald JT et al (2007) Vertebroplasty, first 1000 levels of a single center: evaluation of the outcomes and complications. Am J Neuroradiol 28(4):683–689
Uppin AA, Hirsch JA, Cantenera LV et al (2003) Occurrence of new vertebral body fracture after percutaneous vertebroplasty in patients with osteoporosis. Radiology 226:119–124
Tanigawa N, Komemushi A, Kariya S et al (2006) Radiological follow-up of new compression fractures following percutaneous vertebroplasty. Cardiovasc Interv Radiol 29:92–96
Mubin IS, Neel AP, Solomon J et al (2005) New symptomatic vertebral compression fractures within a year following vertebroplasty in osteoporotic women. Am J Neuroradiol 26:1601–1604
Voormolen MH, Lohle PN, Juttmann JR, van der Graaf Y, Fransen H, Lampmann LE (2006) The risk of new osteoporotic vertebral compression fractures in the year after percutaneous vertebroplasty. J Vasc Interv Radiol 17(1):71–76
Kim SH, Kang HS, Choi JA, Ahn JM (2004) Risk factors of new compression fractures in adjacent vertebrae after percutaneous vertebroplasty. Acta Radiol 45(4):440–445
Conflict of interest
There is no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mailli, L., Filippiadis, D.K., Brountzos, E.N. et al. Clinical Outcome and Safety of Multilevel Vertebroplasty: Clinical Experience and Results. Cardiovasc Intervent Radiol 36, 183–191 (2013). https://doi.org/10.1007/s00270-012-0379-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-012-0379-z