Abstract
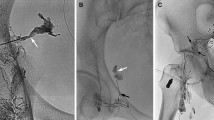
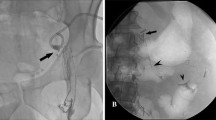
Since the advent of computed tomography, numbers and expertise in Lymphangiography (LAG) have markedly dropped. The intention of our study was to demonstrate the persisting diagnostic and therapeutic impact of LAG on the postoperative patient with known or suspected lymphatic vessel leakage. Between May 1, 1999, and April 30, 2006, we investigated pedal lipiodol-LAGs (18 monopedal, 2 bipedal) on 22 patients (16 male, 6 female) with known or suspected postoperative chylothorax, chylaskos, lymphocele, or lymphatic fistula. Ages varied from 26 to 81 years. The spectrum of operative procedures was broad: 6 thoracic, 5 abdominal, and 11 peripheral operations were performed. In 20 patients who underwent mono- or bipedal LAG for lymphatic vessel injury, we were able to demonstrate the specific site of leakage in 15 cases (75%) and found signs of extravasation in 5 patients (25%). Furthermore, in 11 patients (55%) we were able to avoid surgery because of closure of the leak after LAG. As the conservative therapeutic approach usually takes 2–3 weeks to reveal its therapeutic effects, 73.3% (11/15) of the patients who were not reoperated before this hallmark was passed did not need any further operation. Our study clearly demonstrates that even in the decades of modern cross-sectional imaging, classic LAG is a powerful and highly reliable tool to visualize and even assist occlusion of the postoperatively damaged lymphatic vessel and may thereby avoid the need for reoperation.



Similar content being viewed by others
References
Guermazi A, Brice P, Hennequin C, et al. (2003) Lymphography: an old technique retains its usefulness. Radiographics 23(6):1541–1558, discussion 1559–1560
Luchtenberg M, Mikowski A, Schalnus R, et al. (2000) Erythematous eyelid swelling after dacryocystography. Perforation of the efferent lacrimal ducts in dacryocystography with contrast medium extravasation. Ophthalmologe 97(12):894–895
Browse NL, Allen DR, Wilson NM (1997) Management of chylothorax. Br J Surg 84(12):1711–1716
Cope C, Salem R, Kaiser LR (1999) Management of chylothorax by percutaneous catheterization and embolization of the thoracic duct:prospective trial. J Vasc Interv Radiol 10(9):1248–1254
Cerfolio RJ, Allen MS, Deschamps C, et al. (1996) Postoperative chylothorax. J Thorac Cardiovasc Surg 112(5):1361–1365, discussion 1365–1366
Hoffer EK, Bloch RD, Mulligan MS, et al. (2001) Treatment of chylothorax: percutaneous catheterization and embolization of the thoracic duct. AJR 176(4):1040–1042
Sachs PB, Zelch MG, Rice TW, et al. (1991) Diagnosis and localization of laceration of the thoracic duct: usefulness of LAG and CT. AJR Am J Roentgenol, 157(4):703-5
Halloul Z, Meyer F, Burger T, et al. (1995) Chylous ascites, a rare complication of aortic surgery. Vasa 24(4):377–381
Allen W, Parrott TS, Saripkin L, et al. (1986) Chylous ascites following retroperitoneal lymphadenectomy for granulosa cell tumor of the testis. J Urol 135(4):797–798
Jansen TT, Debruyne FM, Delaere KP, et al. (1984) Chylous ascites after retroperitoneal lymph node dissection. Urology 23(6):565–567
Campieri C, Raimondi C, Dalmastri V, et al. (1996) Posttraumatic chyluria due to lymphorenal fistula regressed after somatostatin therapy. Nephron 72(4):705–707
Peh WC, Ooi GC, Ngan H (1996) Case quiz. Lymphographic demonstration of chylothorax. Australas Radiol 40(4):463–464
Shermak MA, Yee K, Wong L, et al. (2005) Surgical management of groin lymphatic complications after arterial bypass surgery. Plast Reconstr Surg 115(7):1954–1962
Karcaaltincaba M, Akhan O (2005) Radiologic imaging and percutaneous treatment of pelvic lymphocele. Eur J Radiol 55(3):340–354
Canovas B, Morlan MA, Familiar C, et al. (2005) Resolution of a neck chylous fistula with oral diet treatment. Nutr Hosp 20(6):429–432
Heilmann RD, Collins VP (1963) Identification of laceration of the thoracic duct by LAG. Radiology 81:470–472
Samaniego V, Moguel R, Meaney E, et al. (1993) Massive chylopericardium due to congenital fistulas. Am Heart J 126(4):1005–1006
Jarman PR, Whyte K, Sabroe I, et al. (1995) Sarcoidosis presenting with chylothorax. Thorax 50(12):1324–1325
Dugue L, Sauvanet A, Farges O, et al. (1998) Output of chyle as an indicator of treatment for chylothorax complicating oesophagectomy. Br J Surg 85(8):1147–1149
Alexiou C, Watson M, Beggs D, et al. (1998) Chylothorax following oesophagogastrectomy for malignant disease. Eur J Cardiothorac Surg 14(5):460–466
Wurnig PN, Hollaus PH, Ohtsuka T, et al. (2000) Thoracoscopic direct clipping of the thoracic duct for chylopericardium and chylothorax. Ann Thorac Surg 70:1662–1665
Maloney JV, Spencer FC (1956) The nonoperative treatment of traumatic chylothorax. Surgery 40(1):121–128
Selle JG, Snyder WH (1971) Chylothorax: indication for surgery. Ann Surg 177:245–249
Cope C, Kaiser LR (2002) Management of unremitting chylothorax by percutaneous embolization and blockage of retroperitoneal lymphatic vessel leakage. J Vasc Int Radiol 13:1139–1148
Ngan H, Fok M, Wong J (1988) The role of lymphography in chylothorax following thoracic surgery. Br J Radiol 61(731):1032–1036
Kusumoto S, Imamura A, Watanabe K (1991) Case report:the incidental lipid embolization to the brain and kidney after lymphography in a patient with malignant lymphoma: CT findings. Clin Radiol 44(4):279–280
Mortazavi SH, Burrows BD (1971) Allergic reaction to patient blue dye in LAG. Clin Radiol 22(3):389–390
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kos, S., Haueisen, H., Lachmund, U. et al. Lymphangiography: Forgotten Tool or Rising Star in the Diagnosis and Therapy of Postoperative Lymphatic Vessel Leakage. Cardiovasc Intervent Radiol 30, 968–973 (2007). https://doi.org/10.1007/s00270-007-9026-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-007-9026-5