Abstract
Background
Anal fistulae are common, predominantly cryptoglandular, and almost invariably require surgical treatment. Recurrences are common for procedures other than fistulotomy regardless of technique and adequacy of repair. Growing evidence supports the pivotal role of specific intestinal bacteria in anastomotic failures after bowel resection. Anal crypts harbor colonic microbiota suggesting that similar mechanisms to anastomotic healing might prevail after anal fistula repair and hence influence healing. This study aims at assessing the potential role of the intestinal microbiome in the clinical outcomes after surgical repair of cryptoglandular anal fistula.
Methods
This is a pilot prospective cohort study enrolling patients with anal fistula undergoing endoanal advancement flap. For microbiome analysis, stool samples are taken via rectal swab before the procedure; additionally, a portion of the fistula is collected intraoperatively after fistulectomy. Samples from groups with treatment failure are compared to samples from patients who healed after surgical repair. Alpha and beta diversities and differential abundance of microbial taxa are determined and compared between groups with DADA2 analytical pipeline.
Results
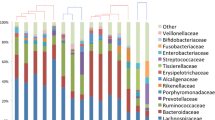
Five patients have been enrolled to date (one female, four male). At median follow-up of 6 months (2–11), one patient experienced disease recurrence at 3 months. DNA from the 5 rectal swab and tissue samples was extracted, showing increased relative abundance of Enterococcus faecalis in samples from the patient who developed a recurrent fistula but not in those without recurrence.
Conclusion
These very preliminary data suggest that intestinal microbiome may represent a crucial determinant of the surgical outcomes after anal fistula surgery.




Similar content being viewed by others
References
Sainio P (1984) Fistula-in-ano in a defined population. Incidence and epidemiological aspects. Ann Chir Gynaecol 73:219–224
Owen HA, Buchanan GN, Schizas A, Cohen R, Williams AB (2016) Quality of life with anal fistula. Ann R Coll Surg Engl 98:334–338
Boenicke L, Karsten E, Zirngibl H, Ambe P (2017) Advancement flap for treatment of complex cryptoglandular anal fistula: prediction of therapy success or failure using anamnestic and clinical parameters. World J Surg 41:2395–2400
vander Mijnsbrugge GJH, Felt-Bersma RJF, HoMolenaar DKFCBH (2019) Perianal fistulas and the lift procedure: results, predictive factors for success, and long-term results with subsequent treatment. Tech Coloproctol 23:639
Włodarczyk M, Włodarczyk J, Sobolewska-Włodarczyk A, Trzciński R, Dziki Ł, Fichna J (2021) Current concepts in the pathogenesis of cryptoglandular perianal fistula. J Int Med Res. https://doi.org/10.1177/0300060520986669
Gaines S, Shao C, Hyman N, Alverdy JC (2018) Gut microbiome influences on anastomotic leak and recurrence rates following colorectal cancer surgery. Br J Surg 105:e131–e141
Anderson DI, Keskey R, Ackerman MT, Zaborina O, Hyman N, Alverdy JC, Shogan BD (2021) Enterococcus faecalis is associated with anastomotic leak in patients undergoing colorectal surgery. Surg Infect (Larchmt) 22:1047–1051
(2013) 16s metagenomic sequencing library preparation. Illumina. https://support.illumina.com/documents/documentation/chemistry_documentation/16s/16s-metagenomic-libraryprep-guide-15044223-b.pdf
Callahan BJ, McMurdie PJ, Rosen MJ, Han AW, Johnson AJA, Holmes SP (2016) DADA2: high resolution sample inference from Illumina amplicon data. Nat Methods 13:581
Quast C, Pruesse E, Yilmaz P, Gerken J, Schweer T, Yarza P, Peplies J, Glöckner FO (2013) The SILVA ribosomal RNA gene database project: improved data processing and web-based tools. Nucleic Acids Res. https://doi.org/10.1093/NAR/GKS1219
McMurdie PJ, Holmes S (2013) Phyloseq: an R package for reproducible Interactive analysis and graphics of microbiome census data. PLoS ONE. https://doi.org/10.1371/journal.pone.0061217
Shogan BD, Belogortseva N, Luong PM et al (2015) Collagen degradation and MMP9 activation by Enterococcus faecalis contribute to intestinal anastomotic leak. Sci Transl Med. https://doi.org/10.1126/SCITRANSLMED.3010658
Guyton K, Alverdy JC (2017) The gut microbiota and gastrointestinal surgery. Nat Rev Gastroenterol Hepatol 14:43–54
Reddy RM, Weir WB, Barnett S et al (2018) Increased variance in oral and gastric microbiome correlates with esophagectomy anastomotic leak. Ann Thorac Surg 105:865–870
van Praagh JB, de Goffau MC, Bakker IS, Harmsen HJM, Olinga P, Havenga K (2016) Intestinal microbiota and anastomotic leakage of stapled colorectal anastomoses: a pilot study. Surg Endosc 30:2259–2265
di Cristofaro L, Ruffolo C, Pinto E et al (2014) Complications after surgery for colorectal cancer affect quality of life and surgeon-patient relationship. Colorectal Dis 16:O407–O419
Limura E, Giordano P (2015) Modern management of anal fistula. World J Gastroenterol 21:12–20
Vogel JD, Johnson EK, Morris AM, Paquette IM, Saclarides TJ, Feingold DL, Steele SR (2016) Clinical practice guideline for the management of anorectal abscess, fistula-in-ano, and rectovaginal fistula. Dis Colon Rectum 59:1117–1133
Hyman N, O’Brien S, Osler T (2009) Outcomes after fistulotomy: results of a prospective, multicenter regional study. Dis Colon Rectum 52:2022–2027
Abbas MA, Jackson CH, Haigh PI (2011) Predictors of outcome for anal fistula surgery. Arch Surg 146:1011–1016
Mei Z, Wang Q, Zhang Y, Liu P, Ge M, Du P, Yang W, He Y (2019) Risk factors for recurrence after anal fistula surgery: a meta-analysis. Int J Surg 69:153–164
Bosmans JWAM, Jongen ACHM, Bouvy ND, Derikx JPM (2015) Colorectal anastomotic healing: why the biological processes that lead to anastomotic leakage should be revealed prior to conducting intervention studies. BMC Gastroenterol. https://doi.org/10.1186/S12876-015-0410-3
Mocanu V, Dang JT, Ladak F, Tian C, Wang H, Birch DW, Karmali S (2019) Antibiotic use in prevention of anal fistulas following incision and drainage of anorectal abscesses: a systematic review and meta-analysis. Am J Surg 217:910–917
Zhu J, Wang Q, Mei Z (2021) Preliminary study on the pathogenesis of anal fistula. medRxiv. 04.15.21254769
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors. No author has any relevant financial relationships to disclose.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This study has been approved by the Columbia University Medical Center Institutional Review Board (protocol ID: AAAU0274).
Informed consent
Written consent was obtained from all patients enrolled in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Bertucci Zoccali, M., Moallem, D.H., Park, H. et al. Role of Microbiome in the Outcomes Following Surgical Repair of Perianal Fistula: Prospective Cohort Study Design and Preliminary Results. World J Surg 47, 3373–3379 (2023). https://doi.org/10.1007/s00268-023-07212-0
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-023-07212-0