Abstract
Background
Multimodal therapy has improved survival outcomes for rectal cancer (RC) significantly with an exemption for older patients. We sought to assess whether older non-comorbid patients receive substandard oncological treatment for localized RC referring to the National Comprehensive Cancer Network (NCCN) guidelines and whether it affects survival outcomes.
Methods
This is a retrospective study using patient data from the National Cancer Data Base (NCDB) for histologically confirmed RC from 2002 to 2014. Non-comorbid patients between ≥50 and ≤85 years and defined treatment for localized RC were included and assigned to a younger (<75 years) and an older group (≥75 years). Treatment approaches and their impact on relative survival (RS) were analyzed using loess regression models and compared between both groups. Furthermore, mediation analysis was performed to measure the independent relative effect on age and other variables on RS. Data were assessed using the Strengthening the Reporting of Observational studies in Epidemiology (STROBE) checklist.
Results
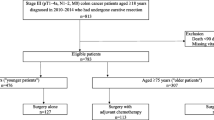
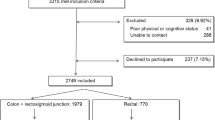
Of 59,769 included patients, 48,389 (81.0%) were assigned to the younger group (<75 years). Oncologic resection was performed in 79.6% of the younger patients compared to 67.2% of the older patients (p < 0.001). Chemotherapy (74.3% vs. 56.1%) and radiotherapy (72.0% vs. 58.1%) were provided less often in older patients, respectively (p < 0.001). Increasing age was associated with enhanced 30- and 90-day mortality with 0.6% and 1.1% in the younger and 2.0% and 4.1% in the elderly group (p < 0.001) and worse RS rates [multivariable adjusted HR: 1.93 (95% CI 1.87–2.00), p < 0.001]. Adherence to standard oncological therapy resulted in a significant increase in 5-year RS (multivariable adjusted HR: 0.80 (95% CI 0.74–0.86), p < 0.001). Mediation analysis revealed that RS was mainly affected by age itself (84%) rather than the choice of therapy.
Conclusions
The likelihood to receive substandard oncological therapy increases in the older population and negatively affects RS. Since age itself has a major impact on RS, better patient selection should be performed to identify those that are potentially eligible for standard oncological care regardless of their age.



Similar content being viewed by others
References
Manceau G, Karoui M, Werner A, Mortensen NJ, Hannoun L (2012) Comparative outcomes of rectal cancer surgery between elderly and non-elderly patients: a systematic review. Lancet Oncol 13(12):e525-536. https://doi.org/10.1016/S1470-2045(12)70378-9
Elferink MA, Krijnen P, Wouters MW, Lemmens VE, Jansen-Landheer ML, van de Velde CJ, Langendijk JA, Marijnen CA, Siesling S, Tollenaar RA (2010) Variation in treatment and outcome of patients with rectal cancer by region, hospital type and volume in the Netherlands. Eur J Surg Oncol 36(Suppl 1):S74-82. https://doi.org/10.1016/j.ejso.2010.06.028
Papamichael D, Audisio RA, Glimelius B, de Gramont A, Glynne-Jones R, Haller D, Kohne CH, Rostoft S, Lemmens V, Mitry E, Rutten H, Sargent D, Sastre J, Seymour M, Starling N, Van Cutsem E, Aapro M (2015) Treatment of colorectal cancer in older patients: International Society of Geriatric Oncology (SIOG) consensus recommendations 2013. Ann Oncol 26(3):463–476. https://doi.org/10.1093/annonc/mdu253
Siegel RL, Miller KD, Fuchs HE, Jemal A (2021) Cancer statistics, 2021. CA Cancer J Clin 71(1):7–33. https://doi.org/10.3322/caac.21654
Kim JH (2015) Chemotherapy for colorectal cancer in the elderly. World J Gastroenterol 21(17):5158–5166. https://doi.org/10.3748/wjg.v21.i17.5158
Schmoll HJ, Tabernero J, Maroun J, de Braud F, Price T, Van Cutsem E, Hill M, Hoersch S, Rittweger K, Haller DG (2015) Capecitabine plus oxaliplatin compared with fluorouracil/folinic acid as adjuvant therapy for stage iii colon cancer: final results of the no16968 randomized controlled phase iii trial. J Clin Oncol 33(32):3733–3740. https://doi.org/10.1200/JCO.2015.60.9107
Hofheinz RD, Wenz F, Post S, Matzdorff A, Laechelt S, Hartmann JT, Muller L, Link H, Moehler M, Kettner E, Fritz E, Hieber U, Lindemann HW, Grunewald M, Kremers S, Constantin C, Hipp M, Hartung G, Gencer D, Kienle P, Burkholder I, Hochhaus A (2012) Chemoradiotherapy with capecitabine versus fluorouracil for locally advanced rectal cancer: a randomised, multicentre, non-inferiority, phase 3 trial. Lancet Oncol 13(6):579–588. https://doi.org/10.1016/S1470-2045(12)70116-X
Montroni I, Ugolini G, Saur NM, Spinelli A, Rostoft S, Millan M, Wolthuis A, Daniels IR, Hompes R, Penna M, Furst A, Papamichael D, Desai AM, Cascinu S, Gerard JP, Myint AS, Lemmens V, Berho M, Lawler M, De Liguori CN, Potenti F, Nanni O, Altini M, Beets G, Rutten H, Winchester D, Wexner SD, Audisio RA (2018) Personalized management of elderly patients with rectal cancer: expert recommendations of the European Society of Surgical Oncology, European Society of Coloproctology, International Society of Geriatric Oncology, and American College of Surgeons Commission on cancer. Eur J Surg Oncol 44(11):1685–1702. https://doi.org/10.1016/j.ejso.2018.08.003
Hurria A, Dale W, Mooney M, Rowland JH, Ballman KV, Cohen HJ, Muss HB, Schilsky RL, Ferrell B, Extermann M, Schmader KE, Mohile SG, Cancer and Aging Research Group (2014) Designing therapeutic clinical trials for older and frail adults with cancer: U13 conference recommendations. J Clin Oncol 32(24):2587–2594. https://doi.org/10.1200/JCO.2013.55.0418
Guillerme F, Clavier JB, Nehme-Schuster H, Leroy V, Heitz D, Schumacher C, Abdelghani MB, Brigand C, Kurtz JE, Noel G (2014) Age impacts the pattern of care for elderly patients with rectal cancer. Int J Colorectal Dis 29(2):157–163. https://doi.org/10.1007/s00384-013-1778-6
Hathout L, Maloney-Patel N, Malhotra U, Wang SJ, Chokhavatia S, Dalal I, Poplin E, Jabbour SK (2018) Management of locally advanced rectal cancer in the elderly: a critical review and algorithm. J Gastrointest Oncol 9(2):363–376. https://doi.org/10.21037/jgo.2017.10.10
Liu W, Zhang M, Wu J, Tang R, Hu L (2020) Oncologic outcome and efficacy of chemotherapy in colorectal cancer patients aged 80 years or older. Front Med (Lausanne) 7:525421. https://doi.org/10.3389/fmed.2020.525421
Thiels CA, Bergquist JR, Meyers AJ, Johnson CL, Behm KT, Hayman AV, Habermann EB, Larson DW, Mathis KL (2016) Outcomes with multimodal therapy for elderly patients with rectal cancer. Br J Surg 103(2):e106-114. https://doi.org/10.1002/bjs.10057
Vernet R, Borras JM, Aliste L, Antonio M, Guarga A, Manchon-Walsh P (2018) Influence of age on variation in patterns of care in patients with rectal cancer in Catalonia (Spain). Clin Transl Oncol 20(12):1538–1547. https://doi.org/10.1007/s12094-018-1882-8
Liu SL, O’Brien P, Zhao Y, Hopman WM, Lamond N, Ramjeesingh R (2018) Adjuvant treatment in older patients with rectal cancer: a population-based review. Curr Oncol 25(6):e499–e506. https://doi.org/10.3747/co.25.4102
Aparicio T, Navazesh A, Boutron I, Bouarioua N, Chosidow D, Mion M, Choudat L, Sobhani I, Mentre F, Soule JC (2009) Half of elderly patients routinely treated for colorectal cancer receive a sub-standard treatment. Crit Rev Oncol Hematol 71(3):249–257. https://doi.org/10.1016/j.critrevonc.2008.11.006
Vandenbroucke JP, von Elm E, Altman DG, Gotzsche PC, Mulrow CD, Pocock SJ, Poole C, Schlesselman JJ, Egger M, Initiative S (2014) Strengthening the reporting of observational studies in epidemiology (STROBE): explanation and elaboration. Int J Surg 12(12):1500–1524. https://doi.org/10.1016/j.ijsu.2014.07.014
Surgeons ACo (2020) National Cancer Database. Updated 2020. https://www.facs.org/quality-programs/cancer/ncdb
Boffa DJ, Rosen JE, Mallin K, Loomis A, Gay G, Palis B, Thoburn K, Gress D, McKellar DP, Shulman LN, Facktor MA, Winchester DP (2017) Using the national cancer database for outcomes research: a review. JAMA Oncol 3(12):1722–1728. https://doi.org/10.1001/jamaoncol.2016.6905
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40(5):373–383. https://doi.org/10.1016/0021-9681(87)90171-8
(NCCN) NCCN (2022) NCCN clinical practice guidelines in oncology (NCCN Guidelines®)—rectal cancer. www.nccn.org
Bos A, Kortbeek D, van Erning FN, Zimmerman DDE, Lemmens V, Dekker JWT, Maas H (2019) Postoperative mortality in elderly patients with colorectal cancer: the impact of age, time-trends and competing risks of dying. Eur J Surg Oncol 45(9):1575–1583. https://doi.org/10.1016/j.ejso.2019.04.020
Bouassida M, Charrada H, Chtourou MF, Hamzaoui L, Mighri MM, Sassi S, Azzouz MM, Touinsi H (2015) Surgery for colorectal cancer in elderly patients: how could we improve early outcomes? J Clin Diagn Res 9(5):PC04-08. https://doi.org/10.7860/JCDR/2015/12213.5973
Lal N, Chan DKH, Ng ME, Vermeulen L, Buczacki SJA (2022) Primary tumour immune response and lymph node yields in colon cancer. Br J Cancer 126(8):1178–1185. https://doi.org/10.1038/s41416-022-01700-1
National Cancer Institute—Surveillance EaERP expected survival life tables. https://seer.cancer.gov/expsurvival/
DuMontier C, Loh KP, Bain PA, Silliman RA, Hshieh T, Abel GA, Djulbegovic B, Driver JA, Dale W (2020) Defining undertreatment and overtreatment in older adults with cancer: a scoping literature review. J Clin Oncol 38(22):2558–2569. https://doi.org/10.1200/JCO.19.02809
Krook JE, Moertel CG, Gunderson LL, Wieand HS, Collins RT, Beart RW, Kubista TP, Poon MA, Meyers WC, Mailliard JA et al (1991) Effective surgical adjuvant therapy for high-risk rectal carcinoma. New Engl J Med 324(11):709–715. https://doi.org/10.1056/NEJM199103143241101
Valentini V, Beets-Tan R, Borras JM, Krivokapic Z, Leer JW, Pahlman L, Rodel C, Schmoll HJ, Scott N, Velde CV, Verfaillie C (2008) Evidence and research in rectal cancer. Radiother Oncol 87(3):449–474. https://doi.org/10.1016/j.radonc.2008.05.022
FORDS (2016). https://www.facs.org/quality-programs/cancer/ncdb/registrymanuals/cocmanuals/fordsmanual. Accessed 11 July 2016
The R project for statistical computing. www.r-project.org
Pohar M, Stare J (2007) Making relative survival analysis relatively easy. Comput Biol Med 37(12):1741–1749. https://doi.org/10.1016/j.compbiomed.2007.04.010
Hakulinen T, Seppa K, Lambert PC (2011) Choosing the relative survival method for cancer survival estimation. Eur J Cancer 47(14):2202–2210. https://doi.org/10.1016/j.ejca.2011.03.011
Ederer F, Axtell LM, Cutler SJ (1961) The relative survival rate: a statistical methodology. Natl Cancer Inst Monogr 6:101–121
Syriopoulou E, Rutherford MJ, Lambert PC (2021) Understanding disparities in cancer prognosis: an extension of mediation analysis to the relative survival framework. Biom J 63(2):341–353. https://doi.org/10.1002/bimj.201900355
Warschkow R, Tsai C, Kohn N, Erdem S, Schmied B, Nussbaum DP, Gloor B, Muller SA, Blazer D 3rd, Worni M (2020) Role of lymphadenectomy, adjuvant chemotherapy, and treatment at high-volume centers in patients with resected pancreatic cancer-a distinct view on lymph node yield. Langenbecks Arch Surg 405(1):43–54. https://doi.org/10.1007/s00423-020-01859-2
Lawler M, Selby P, Aapro MS, Duffy S (2014) Ageism in cancer care. BMJ 348:g1614. https://doi.org/10.1136/bmj.g1614
Millan M, Merino S, Caro A, Feliu F, Escuder J, Francesch T (2015) Treatment of colorectal cancer in the elderly. World J Gastrointest Oncol 7(10):204–220. https://doi.org/10.4251/wjgo.v7.i10.204
Rutten HJ, den Dulk M, Lemmens VE, van de Velde CJ, Marijnen CA (2008) Controversies of total mesorectal excision for rectal cancer in elderly patients. Lancet Oncol 9(5):494–501. https://doi.org/10.1016/S1470-2045(08)70129-3
De Felice F, Crocetti D, Maiuri V, Parisi M, Marampon F, Izzo L, De Toma G, Musio D, Tombolini V (2020) Locally advanced rectal cancer: treatment approach in elderly patients. Curr Treat Options Oncol 21(1):1. https://doi.org/10.1007/s11864-019-0692-8
Couwenberg AM, de Beer FSA, Intven MPW, Burbach JPM, Smits AB, Consten ECJ, Schiphorst AHW, Wijffels NAT, de Roos MAJ, Hamaker ME, van Grevenstein WMU, Verkooijen HM (2018) The impact of postoperative complications on health-related quality of life in older patients with rectal cancer; a prospective cohort study. J Geriatr Oncol 9(2):102–109. https://doi.org/10.1016/j.jgo.2017.09.005
Abelson JS, Bauer PS, Barron J, Bommireddy A, Chapman WC Jr, Schad C, Ohman K, Hunt S, Mutch M, Silviera M (2021) Fragmented care in the treatment of rectal cancer and time to definitive therapy. J Am Coll Surg 232(1):27–33. https://doi.org/10.1016/j.jamcollsurg.2020.10.017
Dekker JW, van den Broek CB, Bastiaannet E, van de Geest LG, Tollenaar RA, Liefers GJ (2011) Importance of the first postoperative year in the prognosis of elderly colorectal cancer patients. Ann Surg Oncol 18(6):1533–1539. https://doi.org/10.1245/s10434-011-1671-x
Cai X, Wu H, Peng J, Zhu J, Cai S, Cai G, Zhang Z (2013) Tolerability and outcomes of radiotherapy or chemoradiotherapy for rectal cancer in elderly patients aged 70 years and older. Radiat Oncol 8:86. https://doi.org/10.1186/1748-717X-8-86
Margalit DN, Mamon HJ, Ancukiewicz M, Kobayashi W, Ryan DP, Blaszkowsky LS, Clark J, Willett CG, Hong TS (2011) Tolerability of combined modality therapy for rectal cancer in elderly patients aged 75 years and older. Int J Radiat Oncol Biol Phys 81(5):e735-741. https://doi.org/10.1016/j.ijrobp.2010.12.056
Smith FM, Rao C, Oliva Perez R, Bujko K, Athanasiou T, Habr-Gama A, Faiz O (2015) Avoiding radical surgery improves early survival in elderly patients with rectal cancer, demonstrating complete clinical response after neoadjuvant therapy: results of a decision-analytic model. Dis Colon Rectum 58(2):159–171. https://doi.org/10.1097/DCR.0000000000000281
Rao C, Sun Myint A, Athanasiou T, Faiz O, Martin AP, Collins B, Smith FM (2017) Avoiding radical surgery in elderly patients with rectal cancer is cost-effective. Dis Colon Rectum 60(1):30–42. https://doi.org/10.1097/DCR.0000000000000708
Smith JJ, Strombom P, Chow OS, Roxburgh CS, Lynn P, Eaton A, Widmar M, Ganesh K, Yaeger R, Cercek A, Weiser MR, Nash GM, Guillem JG, Temple LKF, Chalasani SB, Fuqua JL, Petkovska I, Wu AJ, Reyngold M, Vakiani E, Shia J, Segal NH, Smith JD, Crane C, Gollub MJ, Gonen M, Saltz LB, Garcia-Aguilar J, Paty PB (2019) Assessment of a watch-and-wait strategy for rectal cancer in patients with a complete response after neoadjuvant therapy. JAMA Oncol 5(4):e185896. https://doi.org/10.1001/jamaoncol.2018.5896
Rullier E, Vendrely V, Asselineau J, Rouanet P, Tuech JJ, Valverde A, de Chaisemartin C, Rivoire M, Trilling B, Jafari M, Portier G, Meunier B, Sieleznieff I, Bertrand M, Marchal F, Dubois A, Pocard M, Rullier A, Smith D, Frulio N, Frison E, Denost Q (2020) Organ preservation with chemoradiotherapy plus local excision for rectal cancer: 5-year results of the GRECCAR 2 randomised trial. Lancet Gastroenterol Hepatol 5(5):465–474. https://doi.org/10.1016/S2468-1253(19)30410-8
Habr-Gama A, Perez RO, Nadalin W, Sabbaga J, Ribeiro U Jr, SilvaeSousa AH Jr, Campos FG, Kiss DR, Gama-Rodrigues J (2004) Operative versus nonoperative treatment for stage 0 distal rectal cancer following chemoradiation therapy: long-term results. Ann Surg 240(4):711–717. https://doi.org/10.1097/01.sla.0000141194.27992.32. (discussion 717–718)
Mohanty S, Bilimoria KY (2014) Comparing national cancer registries: The National Cancer Data Base (NCDB) and the Surveillance, Epidemiology, and End Results (SEER) program. J Surg Oncol 109(7):629–630. https://doi.org/10.1002/jso.23568
Lambert PC, Dickman PW, Rutherford MJ (2015) Comparison of different approaches to estimating age standardized net survival. BMC Med Res Methodol 15:64. https://doi.org/10.1186/s12874-015-0057-3
Mohile SG, Dale W, Somerfield MR, Schonberg MA, Boyd CM, Burhenn PS, Canin B, Cohen HJ, Holmes HM, Hopkins JO, Janelsins MC, Khorana AA, Klepin HD, Lichtman SM, Mustian KM, Tew WP, Hurria A (2018) Practical assessment and management of vulnerabilities in older patients receiving chemotherapy: asco guideline for geriatric oncology. J Clin Oncol 36(22):2326–2347. https://doi.org/10.1200/JCO.2018.78.8687
Acknowledgements
We thank the American College of Surgeons and the American Cancer Society for providing patient information through the NCDB used for this investigation. Furthermore, we thank the patients whose information through the NCDB allowed us to perform the investigation for this manuscript.
Funding
This study was in part supported by the Swiss Cancer Foundation.
Author information
Authors and Affiliations
Contributions
SE, MW performed conceptualizing,SE, MW did methodology, RW done formal analysis and investigation, SE, JF, MW prepared writing—original draft preparation, SE, PS, CT, DN, BS, DB, MW done writing—review and editing, DN, DB, MW did resources, BS, DB, MW performed supervision.
Corresponding author
Ethics declarations
Conflict of interest
All authors declare no conflicts of interest.
Ethical approval
This retrospective cohort study was approved by the Duke Institutional Review Board. This article does not contain any studies with human participants performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendix
Appendix
See Table 5.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Erdem, S., Warschkow, R., Studer, P. et al. The Impact of Age in the Treatment of Non-comorbid Patients with Rectal Cancer: Survival Outcomes from the National Cancer Database. World J Surg 47, 2023–2038 (2023). https://doi.org/10.1007/s00268-023-07008-2
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-023-07008-2