Abstract
Background
Neck ultrasound (US) and Technetium-99 m Sestamibi (MIBI) scan are the most commonly used imaging studies for preoperative localization of parathyroid adenomas. The aim of this study was to determine the added value of MIBI scan and its effect on the operative plan via a hypothetical model where a stepwise approach is conducted and MIBI is considered only after the ultrasound is evaluated.
Methods
Patients who underwent parathyroidectomy for primary hyperparathyroidism (PHPT) between 2012 and 2019 at two tertiary centers were included. Data collected included demographic data, preoperative workup, operative findings and follow-up. The added value of MIBI scans was determined for patients with positive ultrasound.
Results
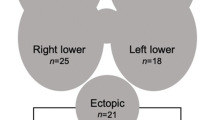
A total of 513 patients with positive US result and a MIBI scan were included. If a stepwise approach was conducted then MIBI scan would not change the operative plan in 492 (95.9%). Among the remaining 21 patients, MIBI scan would correctly change the ultrasound-based operative plan in only 12 (2.3%) patients, while incorrectly change the plan in 9 (1.8%), resulting in unnecessary exploration of the contralateral side. In patients with sonographic appearance of a parathyroid gland larger than 1.2 cm, MIBI scan would correctly change the operative plan in only 1 of the 287 (0.35%) patients.
Conclusions
Our study suggests that the routine use of MIBI scans may have limited added value in patients with PHPT and a positive neck ultrasound, especially in those with adenoma size larger than 1.2 cm. Positive ultrasound alone may be sufficient for the preoperative localization of parathyroid disease.

Similar content being viewed by others
References
Press DM, Siperstein AE, Berber E et al (2013) The prevalence of undiagnosed and unrecognized primary hyperparathyroidism: a population-based analysis from the electronic medical record. Surgery 154(6):1232–1238
Bilezikian JP, Bandeira L, Khan A, Cusano NE (2018) Hyperparathyroidism. Lancet 391:168–178
Wilhelm SM, Wang TS, Ruan DT et al (2017) The definitive management of primary hyperparathyroidism who needs an operation? JAMA - J Am Med Assoc 317(11):959–968
Henry JF (2008) Minimally invasive thyroid and parathyroid surgery is not a question of length of the incision. Langenbeck’s Arch Surg 393(5):621–626. https://doi.org/10.1007/s00423-008-0406-3
Schneider DF, Mazeh H, Chen H, Sippel RS (2014) Predictors of recurrence in primary hyperparathyroidism: an analysis of 1386 cases. Ann Surg 259(3):563–568
Kuzminski SJ, Sosa JA, Hoang JK (2018) Update in parathyroid imaging. Magn Reson Imaging Clin N Am 26(1):151–166
Zafereo M, Yu J, Angelos P et al (2019) American head and neck society endocrine surgery section update on parathyroid imaging for surgical candidates with primary hyperparathyroidism. Head Neck 41(7):2398–2409
Bilezikian JP, Khan AA, Potts JT (2009) Guidelines for the management of asymptomatic primary hyperparathyroidism: summary statement from the third international workshop. J Clin Endocrinol Metab 94(2):335–339
Bilezikian JP, Brandi ML, Eastell R et al (2014) Guidelines for the management of asymptomatic primary hyperparathyroidism: summary statement from the fourth international workshop. J Clin Endocrinol Metab 99(10):3561–3569
Doppman J (1986) No title. Reoperative Parathyr Surg localization Proced 18:117–132
Frank E, Watson WA, Fujimoto S, De Andrade FP, Inman J, Simental A (2020) Surgery versus imaging in non-localizing primary hyperparathyroidism: a cost-effectiveness model. Laryngoscope 130(12):E963–E969
Cheung K, Wang TS, Farrokhyar F, Roman SA, Sosa JA (2012) A meta-analysis of preoperative localization techniques for patients with primary hyperparathyroidism. Ann Surg Oncol 19(2):577–583. https://doi.org/10.1245/s10434-011-1870-5
Moghadam RN, Amlelshahbaz AP, Namiranian N et al (2017) Comparative diagnostic performance of ultrasonography and 99mTc-Sestamibi scintigraphy for parathyroid adenoma in primary hyperparathyroidism; systematic review and meta-analysis. Asian Pacific J Cancer Prev 18(12):3195–3200
Al-kurd A, Levit B, Assaly M, Mizrahi I (2018) Preoperative localization modalities in primary hyperparathyroidism: correlation with postoperative cure. Surgery 164(1):1–7
Ebner Y, Garti-gross Y, Margulis A, Levy Y, Nabrisky D, Ophir D (2015) Parathyroid surgery: correlation between pre-operative localization studies and surgical outcome. Clin Endocrinol 83(5):733–738
Korwar V, Yuen Chang F, Teasdale E, Suchett-Kaye I, Edwards A, Morgan J (2020) Stepwise approach for parathyroid localisation in primary hyperparathyroidism. World J Surg 44(3):803–809
Funding
The authors have no funding sources to report.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declared that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yalon, T., Neymark, M., Rottenberg, A. et al. The Added Value of Technetium-99 m Sestamibi Scan in Patients with Primary Hyperparathyroidism and Positive Ultrasound. World J Surg 45, 2148–2154 (2021). https://doi.org/10.1007/s00268-021-06066-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-021-06066-8