Abstract
Background
Approximately 5 billion people do not have access to safe, timely, and affordable surgical and anesthesia care, with this number disproportionately affecting those from low–middle-income countries (LMICs). Perioperative mortality rates (POMRs) have been identified by the World Health Organization as a potential health metric to monitor quality of surgical care provided. The purpose of this systematic review was to evaluate published reports of POMR and suggest recommendations for its appropriate use as a health metric.
Methods
The protocol was registered a priori with PROSPERO. A peer-reviewed search strategy was developed adhering with the PRISMA guidelines. Relevant articles were identified through Medline, Embase, CENTRAL, CDSR, LILACS, PubMed, BIOSIS, Global Health, Africa-Wide Information, Scopus, and Web of Science databases. Two independent reviewers performed a primary screening analysis based on titles and abstracts, followed by a full-text screen. Studies describing POMRs of adult emergency abdominal surgeries in LMICs were included.
Results
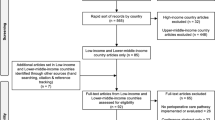
A total of 7787 articles were screened of which 7466 were excluded based on title and abstract. Three hundred and twenty-one articles entered full-text screen of which 70 articles met the inclusion criteria. Variables including timing of POMR reporting, intraoperative mortality, length of hospital stay, complication rates, and disease severity score were collected. Complication rates were reported in 83% of studies and postoperative stay in 46% of studies. 40% of papers did not report the specific timing of POMR collection. 7% of papers reported on intraoperative death. Additionally, 46% of papers used a POMR timing specific to the duration of their study. Vital signs were discussed in 24% of articles, with disease severity score only mentioned in 20% of studies.
Conclusion
POMR is an important health metric for quantifications of quality of care of surgical systems. Further validation and standardization are necessary to effectively use this health metric.






Similar content being viewed by others
References
Funk LM (2010) Global operating theatre distribution and pulse oximetry supply: an estimation from reported data. The Lancet. 376(9746):1055–1061
www.healthdata.org, Sharp decline in maternal and child deaths globally, new data show
Meara JG (2015) Global Surgery 2030: evidence and solutions for achieving health, welfare, and economic development. Lancet 386(9993):569–624
Organization G.W.H. (2018) Global reference list of 100 core health indicators (plus health-related SDGs). World Health Organization, Geneva
Ozmen T, Javadov M, Yegen CS (2016) Factors affecting surgical site infection rate after elective gastric cancer surgery. Turk J Surg 32(3):178–184
Moher D et al (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS medicine 6(7):e1000097
Slim K et al (2003) Methodological index for non-randomized studies (minors): development and validation of a new instrument. ANZ J Surg 73(9):712–716
Bank TW (2018) The world bank classification of country by income. https://datahelpdesk.worldbank.org/knowledgebase/articles/906519-world-bank-country-and-lending-groups
Haynes AB et al (2009) A surgical safety checklist to reduce morbidity and mortality in a global population. New Engl J Med 360(5):491–499
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors disclose no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Felizaire, MR., Paradis, T., Beckett, A. et al. Perioperative Mortality Rates as a Health Metric for Acute Abdominal Surgery in Low- and Middle-Income Countries: A Systematic Review and Future Recommendations. World J Surg 43, 1880–1889 (2019). https://doi.org/10.1007/s00268-019-04993-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-019-04993-1