Abstract
Background
Enterothorax (ET) is a rare complication after hepatic surgery. The literature in this field is limited and mainly based on case reports. The aim of this study was to review our department’s experience.
Patients and methods
We retrospectively analyzed 602 patients who underwent hepatic resection between November 2008 and December 2016. Major hepatic surgery (n = 321) was defined as right or extended right hepatectomy (n = 227), left or extended left hepatectomy (n = 63), trisegmentectomy (n = 13), and living donor liver transplantation (n = 18). ET cases were identified by analyzing clinical courses and radiological imaging.
Results
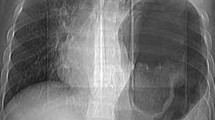
ET was observed in five out of 602 patients (0.8%). All patients developed the complication after major hepatic surgery (five out of 321, 1.6%). ET exclusively occurred after right (n = 3) or extended right hepatectomy (n = 2). Median time to diagnosis was 22 months. Radiological imaging showed herniation of small (n = 2), large bowel (n = 2), or omental fat (n = 1) with a median diaphragmatic defect of 3.9 cm. Two patients presented with acute incarceration and underwent emergency surgery, one patient reported recurrent pain and underwent elective repair, and two patients refused surgery. Follow-up imaging in two operated patients showed no recurrence of ET after 36 and 8 months.
Conclusions
Patients after right hepatectomy have a substantial risk of ET. Acute right upper quadrant pain and/or dyspnea after hepatectomy should be investigated with adequate radiological imaging. Elective surgical repair of ET is recommended to avoid emergency surgery in case of incarceration.




Similar content being viewed by others
References
Raakow J, Schulte-Mäter J, Andreou A et al (2017) Diaphragmatic herniation of abdominal contents: case series and review of the literature. Zentralbl Chir 142:113–121
Rottier R, Tibboel D (2005) Fetal lung and diaphragm development in congenital diaphragmatic hernia. Semin Perinatol 29:86–93
Johnson CD, Ellis H (1988) Acquired hernias of the diaphragm. Postgrad Med J 64:317–321
Crandall M, Popowich D, Shapiro M et al (2007) Posttraumatic hernias: historical overview and review of the literature. Am Surg 73(9):845–850
Willer BL, Worrell SG, Fitzgibbons RJ Jr et al (2012) Incidence of diaphragmatic hernias following minimally invasive versus open transthoracic Ivor Lewis McKeown esophagectomy. Hernia 16:185–190
Johnson CD, Shandall A (1987) Incisional hernia of the diaphragm causing large bowel obstruction. J R Coll Surg Edinb 21:51–52
Ganeshan DM, Correa AM, Bhosale P et al (2013) Diaphragmatic hernia after esophagectomy in 440 patients with long-term follow-up. Ann Thorac Surg 96:1138–1145
Benjamin G, Ashfaq A, Chang YH et al (2015) Diaphragmatic hernia post-minimally invasive esophagectomy: a discussion and review of literature. Hernia 19:635–643
Wood TF, Rose DM, Chung M et al (2000) Radiofrequency ablation of 231 unresectable hepatic tumors: indications, limitations and complications. Ann Surg Oncol 7:593–600
Tabrizian P, Jibara G, Shrager B et al (2012) Diaphragmatic hernia after hepatic resection: case series at a single Western institution. J Gastrointest Surg 16:1910–1914
Hawxby AM, Mason DP, Klein AS (2006) Diaphragmatic hernia after right donor and hepatectomy: a rare donor complication of partial hepatectomy for transplantation. Hepatobiliary Pancreat Dis Int 5(3):459–461
Vernadakis A, Paul A, Kykalos S et al (2012) Incarcerated diaphragmatic hernia after right hepatectomy for living donor liver transplantation: case report of a extremely rare late donor complication. Transplant Proc 44:2770–2772
Jeng KS, Huang CC, Lin CK et al (2015). Early incarcerated diaphragmatic hernia following right donor hepatectomy: a case report. In: Transplantation proceedings, vol 47, pp 815–816
Yaprak O, Dayangac M, Tolga Demirbas B et al (2011) Analysis of right lobe living-liver donor complications: a single center experience. Exp Clin Transplant 1:56–59
Terminology Committee of the international Hepato-Pancreato-Biliary Association: Chairman, SM Strasberg (USA), Belghiti J, Clavien PA, Gadzijev E et al (2000) The Brisbane 2000 terminology of liver anatomy and resections. HPB 2(3):333–339
Mullins ME, Stein J, Saini SS et al (2001) Prevalence of incidental Bochdalek’s hernia in a large adult population. AJR 177:363–366
Livingstone SM, Andres A, Shapiro J et al (2016) Diaphragmatic hernia after living donor right hepatectomy: proposal for a screening protocol. Transplant Direct 2(7):e84
Kousoulas L, Becker T, Richter N et al (2011) Living donor liver transplantation: effect of the type of liver graft donation on donor mortality and morbidity. Transpl Int 24(3):251–258
Perwaiz A, Mehta N, Mohanka R et al (2010) Right-sided diaphragmatic hernia in an adult after living donor liver transplant: a rare cause of post-transplant recurrent abdominal pain. Hernia 14:547–549
Dieter RA Jr, Spitz J, Kuzycz G (2011) Incarcerated diaphragmatic hernia with intrathoracic bowel obstruction after right liver donation. Int Surg 96(3):239–244
Yonemura Y, Umeda K, Kumashiro R et al (2013) Laparoscopic repair of incarcerated diaphragmatic hernia as a late complication of laparoscopic right hepatectomy: a case report. Fukuoka Igaku Zasshi 104(12):599–602
Mizuno S, Tanemura A, Isaji S (2014) Incarcerated left diaphragmatic hernia following left hepatectomy for living donor liver transplantation. Transpl Int 27(7):e65–e67
Koda M, Ueki M, Maeda N et al (2003) Diaphragmatic perforation and hernia after hepatic radiofrequency ablation. Am J Roentgenol 180:1561–1562
Sugita M, Nagahori K, Kudo T et al (2003) Diaphragmatic hernia resulting from injury during microwave-assisted laparoscopic surgery. Surg Endosc 17:1849
Rochester DF, Arora NS, Braun NM (1982) Maximum contractile force of human diaphragm muscle, determined in vivo. Trans Am Clin Climatol Assoc 93:200–208
Price TN, Allen MS, Nichols FC 3rd et al (2011) Hiatal hernia after esophagectomy: analysis of 2,182 esophagectomies from a single institution. Ann Thorac Surg 92:2041–2045
Van Sandick JW, Knegjens JL, van Lanschot JJ et al (1999) Diaphragmatic herniation following oesophagectomy. Br J Surg 86:109–112
Vallbohmer D, Holscher AH, Herbold T et al (2007) Diaphragmatic hernia after conventional of laparoscopic-assisted transthoracic esophagectomy. Ann Thorac Surg 84:1847–1852
Biere SS, van Berge Henegouwen MI, Maas KW et al (2012) Minimally invasive versus open oesophagectomy for patients with oesophageal cancer: a multicenter, open-label, randomized controlled trial. Lancet 379:1887–1892
Fumagalli U, Rosati R, Caputo M et al (2006) Diaphragmatic acute massive herniation after laparoscopic gastroplasty for esophagectomy. Dis Esophagus 19:40–43
Kent MS, Luketich JD, Tsai W et al (2008) Revisional surgery after esophagectomy: an analysis of 43 patients. Ann Thorac Surg 86:975–983
Messenger DE, Higgs SM, Dwerryhouse SJ et al (2015) Symptomatic diaphragmatic herniation following open and minimally invasive oesophagectomy: experience from UK specialist unit. Surg Endosc 29:417–424
Oor JE, Wiezer MJ, Hazebroek EJ (2016) Hiatal hernia after open versus minimally invasive esophagectomy: a systematic review and meta-analysis. Ann Surg Oncol 23:2690–2698
Kim JH (2018) Pure laparoscopic right hepatectomy using modified liver hanging maneuver: technical evolution from caudal approach toward ventral approach. J Gastroint Surg. https://doi.org/10.1007/s11605-018-3736-7 (Epub ahead of print)
Guro H, Cho JY, Han HS et al (2018) Outcomes of major laparoscopic liver resection for hepatocellular carcinoma. Surg Oncol 27(1):31–35
Marino MV, Shabat G, Guarrasi D et al (2018) Comparative study of the initial experience in performing robotic and laparoscopic right hepatectomy with technical description of the robotic technique. Dig Surg. https://doi.org/10.1159/000487686 (Epub ahead of print)
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards. Institutional review board approval was obtained for this study (BASEC-Number 2017-01878).
Rights and permissions
About this article
Cite this article
Manzini, G., Kuemmerli, C., Reiner, C.S. et al. Enterothorax After Hepatic Surgery: A Single-Center Experience. World J Surg 43, 902–909 (2019). https://doi.org/10.1007/s00268-018-4838-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-018-4838-9