Abstract
Background
Postoperative nosocomial pneumonia is a common immediate complication following lung resection. However, the incidence and mortality of pneumonia developing after discharge (PDAD) for lung-resected patients during long-term observation remain unclear. The aim of this study was to investigate the clinical features of PDAD in patients with resected lung cancer.
Methods
We conducted a retrospective cohort study of 357 consecutive patients with lung cancer who had undergone lung resection at a single institution, between April 2007 and December 2016. The clinical characteristics, pathological features, and overall survival were analyzed. Propensity score matched analysis was used for the evaluation of overall survival between PDAD and non-PDAD groups with adjusted relevant confounding factors.
Results
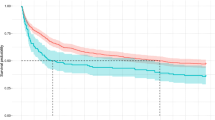
PDAD was observed in 66 patients (18.5%). The cumulative incidence of PDAD was 14.9% at 3 years and 21.6% at 5 years. Mortality of PDAD was 30.3%. Multivariate analysis demonstrated that the risk factors for PDAD were age (OR 1.07; P = 0.005), oral steroid use (OR 5.62; P = 0.046), and lower-lobe resection (OR 1.87; P = 0.034). After propensity score matching, 52 patients with PDAD and 52 patients without it were compared. The incidence of PDAD resulted in a worse 5-year overall survival (56.1 vs. 69.3%; P = 0.024). The Cox proportional hazards model indicated that PDAD was associated with poor overall survival (HR 1.99, P = 0.027).
Conclusions
Our findings revealed a high incidence and mortality of PDAD among patients who had undergone lung resection with long-term follow-up. Therefore, PDAD could be associated with poorer overall survival.



Similar content being viewed by others
Abbreviations
- CAP:
-
Community acquired pneumonia
- CEA:
-
Carcinoembryonic antigen
- CCI:
-
Chronic coronary insufficiency
- COPD:
-
Chronic obstructive pulmonary disease
- CT:
-
Computed tomography
- OS:
-
Overall survival
- PDAD:
-
Pneumonia developing after discharge
- SCLC:
-
Small cell lung cancer
- VATS:
-
Video-assisted thoracoscopic surgery
References
File TM, Marrie TJ (2010) Burden of community acquired pneumonia in North American adults. Postgrad Med 122:130–141
Morimoto K, Suzuki M, Ishifuji T et al (2015) The burden and etiology of community-onset pneumonia in the aging Japanese population: a multicenter prospective study. PLoS ONE 10:e0122247
Marrie TJ, Huang JQ (2005) Epidemiology of community-acquired pneumonia in Edmonton, Alberta: an emergency department-based study. Can Respir J 12:139–142
Fitzmaurice C, Dicker D, Pain A et al (2015) Global burden of disease cancer collaboration. The global burden of cancer 2013. JAMA Oncol 1:505–527
Deslauriers J, Ginsberg RJ, Piantadosi S (1994) Prospective assessment of 30-day operative morbidity for surgical resections in lung cancer. Chest 106:329S–334S
Kearny DJ, Lee TH, Reilly JJ, DeCamp MM et al (1994) Assessment of operative risk in patients undergoing lung resection. Chest 105:753–759
Duque JL, Ramos G, Castrodeza J et al (1997) Early complications in surgical treatment of lung cancer: a prospective multicenter study. Ann Thorac Surg 63:944–950
Farjah F, Backhus L, Cheng A et al (2015) Failure to rescue and pulmonary resection for lung cancer. J Thorac Cardiovasc Surg 149:1365–1371
Bugge AS, Lund MB, Valberg M et al (2018) Cause-specific death after surgical resection for early-stage non-small-cell lung cancer. Eur J Cardiothorac Surg 53:221–227
Torres A, Peetermans WE, Viegi G et al (2013) Risk factors for community-acquired pneumonia in adults in Europe: a literature review. Thorax 68:1057–1065
Simonsen DF, Sogaard M, Bozi I et al (2015) Risk factors for postoperative pneumonia after lung cancer surgery and impact of pneumonia on survival. Respir Med 109:1340–1346
Normand ST, Landrum MB, Guadagnoli E et al (2001) Validating recommendations for coronary angiography following an acute myocardial infarction in the elderly: a matched analysis using propensity scores. J Clin Epidemiol 54:387–398
Seok Y, Lee E, Cho S (2013) Respiratory complications during mid and long-term follow-up periods in patients who underwent pneumonectomy for non-small cell lung cancer. Ann Thorac Cardiovasc Surg 19:335–340
Hanyu T, Kanda T, Yajima K et al (2011) Community-acquired pneumonia during long-term follow-up of patients after radical esophagectomy for esophageal cancer: analysis of incidence and associated risk factors. World J Surg 35:2454–2462. https://doi.org/10.1007/s00268-011-1226-0
Almirall J, Bolibar I, Serra-Prat M et al (2008) New evidence of risk factors for community-acquired pneumonia: a population-based study. Eur Respir J 31:1274–1284
Jagoe RT, Goodship TH, Gibson GJ (2001) The influence of nutritional status on complications after operations for lung cancer. Ann Thorac Surg 71:936–943
Jackson ML, Neuzil KM, Thompson WW et al (2014) The burden of community-acquired pneumonia in seniors: results of a population-based study. Clin Infect Dis 39:1642–1650
Fine MJ, Smith MA, Carson CA et al (1996) Prognosis and outcomes of patients with community-acquired pneumonia: a meta-analysis. JAMA 275:134–141
Schussler O, Alifano M, Dermine H et al (2006) Postoperative pneumonia after major lung resection. Am J Respir Crit Care Med 173:1161–1169
Cillóniz C, Polverino E, Ewig S et al (2013) Impact of age and comorbidity on cause and outcome in community-acquired pneumonia. Chest 144:999–1007
Shiono S, Yoshida J, Nishimura M et al (2007) Risk factors of postoperative respiratory infections in lung cancer surgery. J Thorac Oncol 2:34–38
Klemperer J, Ginsberg RJ (1999) Morbidity and mortality after pneumonectomy. Chest Surg Clin N Am 9:515–525
Whitson BA, Groth SS, Duval SJ et al (2008) Surgery for early stage non-small cell lung cancer: a systematic review of the video-assisted thoracoscopic surgery versus thoracotomy approaches to lobectomy. Ann Thorac Surg 86:2008–2018
Smetana GW (1999) Preoperative pulmonary evaluation. N Engl J Med 340:937–944
Lugg ST, Agostini PJ, Tikka T et al (2016) Long-term impact of developing a postoperative pulmonary complication after lung surgery. Thorax 71:171–176
Kraicer-Melamed H, O’Donnell S, Quach C (2016) The effectiveness of pneumococcal polysaccharide vaccine 23 (PPV23) in the general population of 50 years of age and older: a systematic review and meta-analysis. Vaccine 34:1540–1550
Htar MT, Stuurman AL, Ferreira G et al (2017) Effectiveness of pneumococcal vaccines in preventing pneumonia in adults, a systematic review and meta-analyses of observational studies. PLoS ONE 12:e0177985
Yoneyama T, Yoshida M, Ohrui T et al (2002) Oral care reduces pneumonia in older patients in nursing homes. J Am Geriatr Soc 50:430–433
Hollaar V, van der Maarel-Wierink C, van der Putten GJ et al (2015) Effect of daily application of a 0.05% chlorhexidine solution on the incidence of (aspiration) pneumonia in care home residents: design of a multicentre cluster randomized controlled clinical trial. BMJ Open 5:e007889
Chan EY, Ruest A, Meade MO et al (2007) Oral decontamination for prevention of pneumonia in mechanically ventilated adults: systematic review and meta-analysis. BMJ 334:889
Shigeishi H, Ohta K, Fujimoto S et al (2016) Preoperative oral health care reduces postoperative inflammation and complications in oral cancer patients. Exp Ther Med 12:1922–1928
Akutsu Y, Matsubara H, Shuto K et al (2010) Pre-operative dental brushing can reduce the risk of postoperative pneumonia in esophageal cancer patients. Surgery 147:497–502
Leone FT, Evers-Casey S, Toll BA et al (2013) Treatment of tobacco use in lung cancer: diagnosis and management of lung cancer, 3rd ed: American college of chest physicians evidence-based clinical practice guidelines. Chest 143:e61S–e77S
van Domburg RT, Meeter K, van Berkel DF et al (2000) Smoking cessation reduces mortality after coronary artery bypass surgery: a 20-year follow-up study. J Am Coll Cardiol 36:878–883
Acknowledgements
SS is responsible for the study’s integrity. SM, MM, and SS contributed to the study design and concept. OT, SM, MK and SS contributed to data collection. OT, MM, MK, and SS gathered appropriate literature references. SS, SM, and TF analyzed and interpreted the data and results. SM and TF revised the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declared that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Shinohara, S., Sugaya, M., Onitsuka, T. et al. Impact of Postoperative Pneumonia Developing After Discharge on Long-Term Follow-up for Resected Lung Cancer. World J Surg 42, 3979–3987 (2018). https://doi.org/10.1007/s00268-018-4727-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-018-4727-2