Abstract
Background
To determine whether minimally invasive surgery (MIS) training improves outcomes in laparoscopic appendectomy, a procedure that is commonly performed in general surgery training.
Methods
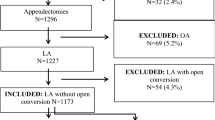
Retrospective review was conducted of all patients undergoing laparoscopic appendectomy for suspected acute appendicitis between 2014 and 2015 at a single-center, tertiary-care academic institution. Patients operated on by MIS-trained surgeons (MIS group) were compared to those operated on by general surgeons (GS group). Single-incision and multiport laparoscopic appendectomies were included; open approach, known malignancy, and interval appendectomies were excluded.
Results
A total of 507 patients were included in the study: 181 patients in the MIS group and 326 in the GS group. There were no differences in patient demographics or medical comorbidities between groups and most patients were ASA class 1 or 2. Patients operated on by MIS-trained surgeons had significantly shorter operative time (43 min, IQR 32–60 vs. 58 min, IQR 44–81; p < 0.001) and fewer intra-operative adverse events (0/181 vs. 8/326, 2.5%; p = 0.03). There was no difference in number of postoperative adverse events between groups (6/181, 3.3% vs. 21/326, 6.4%; p = 0.13). In the MIS group, subgroup analysis of single-incision versus multiport appendectomy showed no differences in intra-operative or postoperative adverse events. On multivariable linear regression, lack of MIS training and traditional multiport approach had the greatest effects on prolonging operative time (11.2 and 12.8 min, respectively; p = 0.001).
Conclusions
MIS fellowship improves operative metrics and patient outcomes even in basic laparoscopy.


Similar content being viewed by others
References
Swanstrom LL, Park A, Arregui M et al (2006) Bringing order to the chaos: developing a matching process for minimally invasive and gastrointestinal postgraduate fellowships. Ann Surg 243:431–435. https://doi.org/10.1097/01.sla.0000205217.45477.25
Ali MR, Tichansky DS, Kothari SN et al (2010) Validation that a 1-year fellowship in minimally invasive and bariatric surgery can eliminate the learning curve for laparoscopic gastric bypass. Surg Endosc 24:138–144. https://doi.org/10.1007/s00464-009-0550-z
Agrawal S (2011) Impact of bariatric fellowship training on perioperative outcomes for laparoscopic Roux-en-Y gastric bypass in the first year as consultant surgeon. Obes Surg 21:1817–1821. https://doi.org/10.1007/s11695-011-0482-2
Decker MR, Dodgion CM, Kwok AC et al (2014) Specialization and the current practices of general surgeons. J Am Coll Surg 218:8–15. https://doi.org/10.1016/j.jamcollsurg.2013.08.016
Richards MK, McAteer JP, Drake FT et al (2015) A national review of the frequency of minimally invasive surgery among general surgery residents: assessment of ACGME case logs during 2 decades of general surgery resident training. JAMA Surg 150:169–172. https://doi.org/10.1001/jamasurg.2014.1791
Kim JH, Kim HY, Park SK et al (2015) Single-incision laparoscopic appendectomy versus conventional laparoscopic appendectomy: experiences from 1208 cases of single-incision laparoscopic appendectomy. Ann Surg 262:1054–1058. https://doi.org/10.1097/SLA.0000000000001064
Carter JT, Kaplan JA, Nguyen JN et al (2014) A prospective, randomized controlled trial of single-incision laparoscopic vs conventional 3-port laparoscopic appendectomy for treatment of acute appendicitis. J Am Coll Surg 218:950–959. https://doi.org/10.1016/j.jamcollsurg.2013.12.052
Lin YY, Shabbir A, So JBY (2010) Laparoscopic appendectomy by residents: evaluating outcomes and learning curve. Surg Endosc 24:125–130. https://doi.org/10.1007/s00464-009-0691-0
Liao Y-T, Lin T-H, Lee P-C et al (2013) Learning curve of single-port laparoscopic appendectomy for noncomplicated acute appendicitis: a preliminary analysis compared with conventional laparoscopic appendectomy. J Laparoendosc Adv Surg Tech A 23:441–446. https://doi.org/10.1089/lap.2012.0265
Murata A, Mayumi T, Muramatsu K et al (2015) Effect of hospital volume on outcomes of laparoscopic appendectomy for acute appendicitis: an observational study. J Gastrointest Surg 19:897–904. https://doi.org/10.1007/s11605-015-2746-y
Abelson JS, Afaneh C, Rich BS et al (2015) Advanced laparoscopic fellowship training decreases conversion rates during laparoscopic cholecystectomy for acute biliary diseases: a retrospective cohort study. Int J Surg 13:221–226. https://doi.org/10.1016/j.ijsu.2014.12.016
Wagner PL, Eachempati SR, Aronova A et al (2011) Contemporary predictors of conversion from laparoscopic to open appendectomy. Surg Infect (Larchmt) 12:261–266. https://doi.org/10.1089/sur.2010.079
Finnerty BM, Wu X, Giambrone GP et al (2017) Conversion-to-open in laparoscopic appendectomy: a cohort analysis of risk factors and outcomes. Int J Surg 40:169–175. https://doi.org/10.1016/j.ijsu.2017.03.016
Unawane A, Kamyab A, Patel M et al (2013) Changing paradigms in minimally invasive surgery training. Am J Surg 205:284–288. https://doi.org/10.1016/j.amjsurg.2012.10.018
Suh SG, Sohn HJ, Kim BG et al (2016) Single-incision laparoscopic appendectomy by surgical trainees. Surg Laparosc Endosc Percutan Tech 26:470–472. https://doi.org/10.1097/SLE.0000000000000340
Papandria D, Rhee D, Ortega G et al (2012) Assessing trainee impact on operative time for common general surgical procedures in ACS-NSQIP. J Surg Educ 69:149–155. https://doi.org/10.1016/j.jsurg.2011.08.003
Johnson JJ, Thurman JB, Garwe T et al (2013) Variations in procedure time based on surgery resident postgraduate year level. J Surg Res. https://doi.org/10.1016/j.jss.2013.06.056
Koperna T (2004) How long do we need teaching in the operating room? The true costs of achieving surgical routine. Langenbecks Arch Surg 389:204–208. https://doi.org/10.1007/s00423-003-0421-3
von Strauss Und Torney M, Dell-Kuster S, Mechera R et al (2012) The cost of surgical training: analysis of operative time for laparoscopic cholecystectomy. Surg Endosc 26:2579–2586. https://doi.org/10.1007/s00464-012-2236-1
Acknowledgements
The authors wish to acknowledge Aaron Burshtein for chart review.
Funding
This study was internally funded.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Dr. Pomp reports honoraria from WL Gore & Associates, Medtronic, and Ethicon, outside the submitted work. Dr. Dakin reports honoraria from Medtronic, outside the submitted work. Dr. Afaneh reports honoraria from Intuitive Surgical, outside the submitted work. Dr. Gray, Mr. J. Burshtein, Dr. Obeid, and Dr. Moore have nothing to disclose.
Rights and permissions
About this article
Cite this article
Gray, K.D., Burshtein, J.G., Obeid, L. et al. Laparoscopic Appendectomy: Minimally Invasive Surgery Training Improves Outcomes in Basic Laparoscopic Procedures. World J Surg 42, 1706–1713 (2018). https://doi.org/10.1007/s00268-017-4374-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-017-4374-z