Abstract
Background
Recurrent hepatocellular carcinoma after a patient’s initial therapy, whether it is transplantation, resection, or ablation, remains a challenging clinical problem. Since recurrence occurs in 70% of all initially treated disease within 5 years, optimal management to treat this recurrence is needed. Currently, a bias exists toward mono-therapy (i.e., ablation alone, hepatic arterial therapy alone, or sorafenib therapy alone) instead of concurrent sequential therapy—as is common in other primary and metastatic disease to the liver. Thus, the aim of our study was to evaluate the overall survival of recurrent HCC based on either mono-therapy or multimodality therapy.
Methods
A review of our prospective 2245 patient hepato-pancreatico-biliary database was performed for all patients who underwent treatment with curative intent for hepatocellular carcinoma and had complete recurrence treatment data from June 2002 to May 2015. Mono-therapy was defined as initiation of a solitary therapy until disease progression or intolerance. Multimodality therapy was defined as at least 2 therapies that occurred simultaneously or within 4 weeks of each therapy.
Results
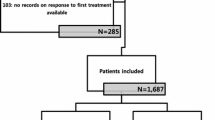
A total of 281 patients underwent treatment with curative intent for hepatocellular carcinoma, in which 192 experienced recurrence. These patients were treated with either thermal ablation or liver resection (LR) (N = 51), transarterial chemoembolization (TACE) or radiation (N = 68), systemic therapy (N = 26), or multimodality therapy (N = 47). The extent of the first recurrence was similar in regard to the number of tumors (median 1), the type of radiologic HCC, gender, BMI, and percentage of liver involvement. They differed in regard to size (MMT largest, median 5.6 cm, p = 0.02), and MMT had higher Hepatitis C involvement (37% of patients, p = 0.001). In evaluation of first recurrence treatment, after a median follow-up of 24 months, multimodality therapy has a significant improvement in overall survival (median 40 months, range 8–85), when compared to LR/Ablation (27 months, range 4–75), TACE/XRT (13 months, range 4–68), and systemic (26 months, range 3–59) (p = 0.003).
Conclusion
Multimodality therapy should be considered in all patients with recurrent HCC based on tumor biology and underlying hepatic reserve. Hepatocellular cancer should be treated like other hepatic malignancies in which concurrent therapies are utilized simultaneously to optimize oncologic effects (response rates and overall survival) and minimize quality-of-life side effects. Multimodality therapy can lead to far superior overall survival and is well tolerated in the majority of recurrent HCC patients.



Similar content being viewed by others
References
Torre LA et al (2015) Global cancer statistics, 2012. CA Cancer J Clin 65(2):87–108
European Association For The Study Of The, L., R. European Organisation For, and C. Treatment Of (2012) EASL-EORTC clinical practice guidelines: management of hepatocellular carcinoma. J Hepatol 56(4):908–943
Bruix J, Sherman M, D. American Association for the Study of Liver (2011) Management of hepatocellular carcinoma: an update. Hepatology 53(3):1020–1022
Martin RC 2nd et al (2015) Randomized controlled trial of irinotecan drug-eluting beads with simultaneous FOLFOX and bevacizumab for patients with unresectable colorectal liver-limited metastasis. Cancer 121(20):3649–3658. doi:10.1002/cncr.29534
Schiffman SC et al (2014) Molecular factors associated with recurrence and survival following hepatectomy in patients with intrahepatic cholangiocarcinoma: a guide to adjuvant clinical trials. J Surg Oncol 109(2):98–103
Schiffman SC et al (2011) Precision hepatic arterial irinotecan therapy in the treatment of unresectable intrahepatic cholangiocellular carcinoma: optimal tolerance and prolonged overall survival. Ann Surg Oncol 18(2):431–438
Schiffman SC et al (2010) Hepatectomy is superior to thermal ablation for patients with a solitary colorectal liver metastasis. J Gastrointest Surg 14(12):1881–1886 (discussion 1886–1887)
Coakley FV, Schwartz LH (2001) Imaging of hepatocellular carcinoma: a practical approach. Semin Oncol 28(5):460–473
Bruix J, Sherman M, A.A.f.t.S.o.L.D (2005) Practice guidelines committee, management of hepatocellular carcinoma. Hepatology 42(5):1208–1236
Woodall CE et al (2007) Hepatic imaging characteristics predict overall survival in hepatocellular carcinoma. Ann Surg Oncol 14(10):2824–2830
Martin RC, Scoggins CR, McMasters KM (2007) Microwave hepatic ablation: initial experience of safety and efficacy. J Surg Oncol 96(6):481–486
Martin RC 2nd et al (2011) Hepatic arterial infusion of doxorubicin-loaded microsphere for treatment of hepatocellular cancer: a multi-institutional registry. J Am Coll Surg 213(4):493–500
Llovet JM et al (2008) Sorafenib in advanced hepatocellular carcinoma. N Engl J Med 359(4):378–390
Woodall CE et al (2009) Is selective internal radioembolization safe and effective for patients with inoperable hepatocellular carcinoma and venous thrombosis? J Am Coll Surg 208(3):375–382
Lencioni R et al (2012) Transcatheter treatment of hepatocellular carcinoma with doxorubicin-loaded DC Bead (DEBDOX): technical recommendations. Cardiovasc Intervent Radiol 35(5):980–985
Martin R et al (2011) Optimal technique and response of doxorubicin beads in hepatocellular cancer: bead size and dose. Korean J Hepatol 17(1):51–60
Martin RC, Scoggins CR, McMasters KM (2010) Safety and efficacy of microwave ablation of hepatic tumors: a prospective review of a 5-year experience. Ann Surg Oncol 17(1):171–178
North DA et al (2014) Microwave ablation for hepatic malignancies: a call for standard reporting and outcomes. Am J Surg 208(2):284–294
Martin RC 2nd et al (2007) Kentucky hepatoma: epidemiologic variant or same problem in a different region? Arch Surg 142(5):431–436 (discussion 436–437)
Ng KK et al (2008) Analysis of recurrence pattern and its influence on survival outcome after radiofrequency ablation of hepatocellular carcinoma. J Gastrointest Surg 12(1):183–191
Llovet JM et al (2008) Sorafenib in advanced hepatocellular carcinoma. N Engl J Med 359(4):378–390
Belghiti J et al (2003) Resection prior to liver transplantation for hepatocellular carcinoma. Ann Surg 238(6):885–892 (discussion 892–893)
Sala M et al (2004) High pathological risk of recurrence after surgical resection for hepatocellular carcinoma: an indication for salvage liver transplantation. Liver Transpl 10(10):1294–1300
Faber W et al (2011) Repeated liver resection for recurrent hepatocellular carcinoma. J Gastroenterol Hepatol 26(7):1189–1194
Chan AC et al (2012) Survival analysis of re-resection versus radiofrequency ablation for intrahepatic recurrence after hepatectomy for hepatocellular carcinoma. World J Surg 36(1):151–156. doi:10.1007/s00268-011-1323-0
Kan X et al (2015) Sorafenib combined with percutaneous radiofrequency ablation for the treatment of medium-sized hepatocellular carcinoma. Eur Rev Med Pharmacol Sci 19(2):247–255
Wang K et al (2015) Early intrahepatic recurrence of hepatocellular carcinoma after hepatectomy treated with re-hepatectomy, ablation or chemoembolization: a prospective cohort study. Eur J Surg Oncol 41(2):236–242
Lencioni R, Llovet JM (2010) Modified RECIST (mRECIST) assessment for hepatocellular carcinoma. Semin Liver Dis 30(1):52–60
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Fields, T.D., Philips, P., Scoggins, C.R. et al. Multi-disciplinary Concurrent Management of Recurrent Hepatocellular Therapy is Superior to Sequential Therapy. World J Surg 41, 1331–1339 (2017). https://doi.org/10.1007/s00268-016-3844-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-016-3844-z