Abstract
Background
Esophageal resection for cancer (EC) is still associated with considerable mortality and morbidity rates. Allogenic blood transfusion (aBT) is associated with poor short-term and long-term outcome in surgical oncology. We aimed to evaluate the effect of aBT in a homogeneous population of EC patients undergoing esophagectomy without perioperative treatment.
Methods
We analyzed 565 esophagectomies performed due to EC. Allogenic blood transfusion was correlated to clinicopathological parameters, perioperative mortality and morbidity as well as the long-term outcome. Results are presented as adjusted odds ratio (OR) or hazard ratio (HR) with 95 % confidence interval (95 % CI).
Results
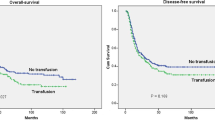
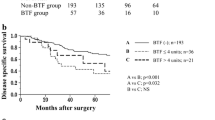
Patients receiving aBT (aBT(+)) had no higher tumor stages or higher rates of lymph node metastasis (P = 0.65 and 0.17, respectively) compared to patients without aBT (aBT(−)). Allogenic blood transfusion was strongly associated with perioperative morbidity (OR 1.9, 95 % CI 1.1–3.5, P = 0.02) and mortality (OR 2.9, 95 % CI 1.0–8.6, P = 0.04). Tumor recurrence rate was significantly higher in aBT(+) patients (P = 0.001). The disease-free and overall survival were significantly longer in aBT(−) compared to aBT(+) patients (P = 0.016 and <0.001, respectively). Patients receiving aBT had almost doubled risk for tumor recurrence (HR 1.8, 95 % CI 1.2–2.5, P = 0.001) and death (HR 2.2, 95 % CI 1.5–3.2, P < 0.001).
Conclusion
Allogenic blood transfusion has a significant impact on the natural course of EC after complete resection. The poor short-term and long-term outcome warrants further evaluation of the underlying molecular mechanisms induced by allogenic blood transfusion in cancer patients.

Similar content being viewed by others
Abbreviations
- aBT:
-
Allogenic blood transfusion
- AC:
-
Adenocarcinoma
- AJCC:
-
American Joint Committee on Cancer
- autoBT:
-
Autologous blood transfusion
- CD:
-
Cluster of differentiation
- CI:
-
Confidence interval
- DFS:
-
Disease-free survival
- EC:
-
Esophageal cancer
- HR:
-
Hazard ratio
- OR:
-
Odds ratio
- OS:
-
Overall survival
- SCC:
-
Squamous cell carcinoma
- TA:
-
Thoracoabdominal
- TH:
-
Transhiatal
- TRICC:
-
Transfusion requirements in critical care
- WBC:
-
White blood cell
References
Jemal A, Bray F, Center MM, Ferlay J, Ward E, Forman D (2011) Global cancer statistics. CA Cancer J Clin 61:69–90
Makowiec F, Baier P, Kulemann B et al (2013) Improved long-term survival after esophagectomy for esophageal cancer: influence of epidemiologic shift and neoadjuvant therapy. J Gastrointest Surg 17:1193–1201
Wouters MW, Krijnen P, Le Cessie S et al (2009) Volume- or outcome-based referral to improve quality of care for esophageal cancer surgery in The Netherlands. J Surg Oncol 99:481–487
Pennathur A, Luketich JD (2008) Resection for esophageal cancer: strategies for optimal management. Ann Thorac Surg 85:S751–S756
Dixon E, Datta I, Sutherland FR, Vauthey JN (2009) Blood loss in surgical oncology: neglected quality indicator? J Surg Oncol 99:508–512
Rovera F, Dionigi G, Boni L et al (2006) Postoperative infections after oesophageal resections: the role of blood transfusions. World J Surg Oncol 4:80
Nozoe T, Miyazaki M, Saeki H, Ohga T, Sugimachi K (2001) Significance of allogenic blood transfusion on decreased survival in patients with esophageal carcinoma. Cancer 92:1913–1918
Motoyama S, Okuyama M, Kitamura M et al (2004) Use of autologous instead of allogeneic blood transfusion during esophagectomy prolongs disease-free survival among patients with recurrent esophageal cancer. J Surg Oncol 87:26–31
Hajjar LA, Vincent JL, Galas FR et al (2010) Transfusion requirements after cardiac surgery: the TRACS randomized controlled trial. JAMA 304:1559–1567
Lange MM, van Hilten JA, van de Watering LM et al (2009) Leucocyte depletion of perioperative blood transfusion does not affect long-term survival and recurrence in patients with gastrointestinal cancer. Br J Surg 96:734–740
Komatsu Y, Orita H, Sakurada M, Maekawa H, Hoppo T, Sato K (2012) Intraoperative blood transfusion contributes to decreased long-term survival of patients with esophageal cancer. World J Surg 36:844–850. doi:10.1007/s00268-012-1433-3
Takemura M, Osugi H, Higashino M, Takada N, Lee S, Kinoshita H (2005) Effect of substituting allogenic blood transfusion with autologous blood transfusion on outcomes after radical oesophagectomy for cancer. Ann Thorac Cardiovasc Surg 11:293–300
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Goodnough LT, Shander A, Spivak JL et al (2005) Detection, evaluation, and management of anemia in the elective surgical patient. Anesth Analg 101:1858–1861
Hebert PC, Wells G, Blajchman MA et al (1999) A multicenter, randomized, controlled clinical trial of transfusion requirements in critical care. Transfusion Requirements in Critical Care Investigators, Canadian Critical Care Trials Group. N Engl J Med 340:409–417
Cerhan JR, Engels EA, Cozen W et al (2008) Blood transfusion, anesthesia, surgery and risk of non-Hodgkin lymphoma in a population-based case–control study. Int J Cancer 123:888–894
Doyle BJ, Rihal CS, Gastineau DA, Holmes DR Jr (2009) Bleeding, blood transfusion, and increased mortality after percutaneous coronary intervention: implications for contemporary practice. J Am Coll Cardiol 53:2019–2027
Cornes P, Coiffier B, Zambrowski JJ (2007) Erythropoietic therapy for the treatment of anemia in patients with cancer: a valuable clinical and economic option. Curr Med Res Opin 23:357–368
Wu WC, Smith TS, Henderson WG et al (2010) Operative blood loss, blood transfusion, and 30-day mortality in older patients after major noncardiac surgery. Ann Surg 252:11–17
Bernard AC, Davenport DL, Chang PK, Vaughan TB, Zwischenberger JB (2009) Intraoperative transfusion of 1 U to 2 U packed red blood cells is associated with increased 30-day mortality, surgical-site infection, pneumonia, and sepsis in general surgery patients. J Am Coll Surg 208:931–937 7 e1–e2; discussion 8–9
Patel MS, Carson JL (2009) Anemia in the preoperative patient. Med Clin N Am 93:1095–1104
Karkouti K, Wijeysundera DN, Beattie WS (2008) Reducing bleeding in cardiac surgery I. Risk associated with preoperative anemia in cardiac surgery: a multicenter cohort study. Circulation 117:478–484
Corwin HL, Gettinger A, Pearl RG et al (2004) The CRIT study: anemia and blood transfusion in the critically ill–current clinical practice in the United States. Crit Care Med 32:39–52
Kulier A, Levin J, Moser R et al (2007) Impact of preoperative anemia on outcome in patients undergoing coronary artery bypass graft surgery. Circulation 116:471–479
Murphy GJ, Reeves BC, Rogers CA, Rizvi SI, Culliford L, Angelini GD (2007) Increased mortality, postoperative morbidity, and cost after red blood cell transfusion in patients having cardiac surgery. Circulation 116:2544–2552
Weber RS, Jabbour N, Martin RC II (2008) Anemia and transfusions in patients undergoing surgery for cancer. Ann Surg Oncol 15:34–45
Sugita S, Sasaki A, Iwaki K et al (2008) Prognosis and postoperative lymphocyte count in patients with hepatocellular carcinoma who received intraoperative allogenic blood transfusion: a retrospective study. Eur J Surg Oncol 34:339–345
Kneuertz PJ, Patel SH, Chu CK et al (2011) Effects of perioperative red blood cell transfusion on disease recurrence and survival after pancreaticoduodenectomy for ductal adenocarcinoma. Ann Surg Oncol 18:1327–1334
Wang T, Luo L, Huang H et al (2014) Perioperative blood transfusion is associated with worse clinical outcomes in resected lung cancer. Ann Thorac Surg 97:1827–1837
Opelz G, Terasaki PI (1978) Improvement of kidney–graft survival with increased numbers of blood transfusions. N Engl J Med 299:799–803
Baumgartner JM, Silliman CC, Moore EE, Banerjee A, McCarter MD (2009) Stored red blood cell transfusion induces regulatory T cells. J Am Coll Surg 208:110–119
Melis M, McLoughlin JM, Dean EM et al (2009) Correlations between neoadjuvant treatment, anemia, and perioperative complications in patients undergoing esophagectomy for cancer. J Surg Res 153:114–120
Kinoshita Y, Udagawa H, Tsutsumi K et al (2000) Usefulness of autologous blood transfusion for avoiding allogenic transfusion and infectious complications after esophageal cancer resection. Surgery 127:185–192
Ling FC, Hoelscher AH, Vallbohmer D et al (2009) Leukocyte depletion in allogeneic blood transfusion does not change the negative influence on survival following transthoracic resection for esophageal cancer. J Gastrointest Surg 13:581–586
Kader AS, Lim JT, Berthelet E, Petersen R, Ludgate D, Truong PT (2007) Prognostic significance of blood transfusions in patients with esophageal cancer treated with combined chemoradiotherapy. Am J Clin Oncol 30:492–497
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Additional information
Matthias Reeh, Tarik Ghadban and Josephine Dedow have contributed equally to this work and therefore share first authorship.
Rights and permissions
About this article
Cite this article
Reeh, M., Ghadban, T., Dedow, J. et al. Allogenic Blood Transfusion is Associated with Poor Perioperative and Long-Term Outcome in Esophageal Cancer. World J Surg 41, 208–215 (2017). https://doi.org/10.1007/s00268-016-3730-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-016-3730-8