Abstract
Background
While surgery offers the best curative-intent treatment, many patients with biliary tract malignancies have poor long-term outcomes. We sought to apply a non-mixture cure model to calculate the cure fraction and the time to cure after surgery of patients with peri-hilar cholangiocarcinoma (PHCC) or gallbladder cancer (GBC).
Methods
Using the Extrahepatic Biliary Malignancy Consortium, 576 patients who underwent curative-intent surgery for gallbladder carcinoma or peri-hilar cholangiocarcinoma between 1998 and 2014 at 10 major hepatobiliary institutions were identified and included in the analysis. A non-mixture cure model was adopted to compare mortality after surgery to the mortality expected for the general population matched by sex and age.
Results
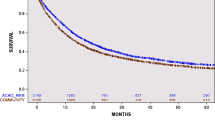
The median and 5-year overall survival (OS) were 1.9 years (IQR, 0.9–4.9) and 23.9 % (95 % CI, 19.6–28.6). Among all patients with PHCC or GBC, the probability of being cured after surgery was 14.5 % (95 % CI, 8.7–23.2); the time to cure was 9.7 years and the median survival of uncured patients was 1.8 years. Determinants of cure probabilities included lymph node metastasis and CA 19.9 level (p ≤ 0.05). The cure fraction for patients with a CA 19.9 < 50 U/ml and no lymph nodes metastases were 39.0 % versus only 5.1 % among patients with a CA 19.9 ≥ 50 who also had lymph node metastasis.
Conclusions
Examining an “all comer” cohort, <15 % of patients with PHCC or GBC could be considered cured after surgery. Factors such CA 19.9 level and lymph node metastasis independently predicted long-term outcome. Estimating the odds of statistical cure following surgery for biliary tract cancer can assist in decision-making as well as inform discussions around survivorship.



Similar content being viewed by others
References
Valero V 3rd et al (2012) Management of perihilar cholangiocarcinoma in the era of multimodal therapy. Expert Rev Gastroenterol Hepatol 6(4):481–495
Kanthan R et al (2015) Gallbladder cancer in the 21st century. J Oncol 2015:967472
Hansel DE et al (2003) Identification of novel cellular targets in biliary tract cancers using global gene expression technology. Am J Pathol 163(1):217–229
Tannapfel A et al (2003) Mutations of the BRAF gene in cholangiocarcinoma but not in hepatocellular carcinoma. Gut 52(5):706–712
Valle J et al (2010) Cisplatin plus gemcitabine versus gemcitabine for biliary tract cancer. N Engl J Med 362(14):1273–1281
Friend E et al (2011) Development of a questionnaire (EORTC module) to measure quality of life in patients with cholangiocarcinoma and gallbladder cancer, the EORTC QLQ-BIL21. Br J Cancer 104(4):587–592
El-Khoueiry AB et al (2012) SWOG 0514: a phase II study of sorafenib in patients with unresectable or metastatic gallbladder carcinoma and cholangiocarcinoma. Invest New Drugs 30(4):1646–1651
El-Khoueiry AB et al (2014) S0941: a phase 2 SWOG study of sorafenib and erlotinib in patients with advanced gallbladder carcinoma or cholangiocarcinoma. Br J Cancer 110(4):882–887
Ben-Josef E et al (2015) SWOG S0809: a Phase II intergroup trial of adjuvant capecitabine and gemcitabine followed by radiotherapy and concurrent capecitabine in extrahepatic cholangiocarcinoma and gallbladder carcinoma. J Clin Oncol 33(24):2617–2622
Jarnagin WR et al (2001) Staging, resectability, and outcome in 225 patients with hilar cholangiocarcinoma. Ann Surg 234(4):507–517 (discussion 517–519)
Akamatsu N, Sugawara Y, Hashimoto D (2011) Surgical strategy for bile duct cancer: advances and current limitations. World J Clin Oncol 2(2):94–107
Mao K et al (2016) Patterns and prognostic value of lymph node dissection for resected perihilar cholangiocarcinoma. J Gastroenterol Hepatol 31(2):417–426
Wang J et al (2015) Evaluation of adjuvant radiation therapy for resected gallbladder carcinoma: a multi-institutional experience. Ann Surg Oncol 22(Suppl 3):1100–1106
Hueman MT, Vollmer CM Jr, Pawlik TM (2009) Evolving treatment strategies for gallbladder cancer. Ann Surg Oncol 16(8):2101–2115
Amini N et al (2015) Lymph node status after resection for gallbladder adenocarcinoma: prognostic implications of different nodal staging/scoring systems. J Surg Oncol 111(3):299–305
Weiss MJ et al (2014) Multimodal treatment strategies for advanced hilar cholangiocarcinoma. Langenbecks Arch Surg 399(6):679–692
Poruk KE, Pawlik TM, Weiss MJ (2015) Perioperative management of hilar cholangiocarcinoma. J Gastrointest Surg 19(10):1889–1899
Maetani S, Gamel JW (2010) Evolution of cancer survival analysis. Surg Oncol 19(2):49–51 (discussion 61)
Lambert PC et al (2007) Estimating and modeling the cure fraction in population-based cancer survival analysis. Biostatistics 8(3):576–594
Cvancarova M et al (2013) Proportion cured models applied to 23 cancer sites in Norway. Int J Cancer 132(7):1700–1710
Dal Maso L et al (2014) Long-term survival, prevalence, and cure of cancer: a population-based estimation for 818 902 Italian patients and 26 cancer types. Ann Oncol 25(11):2251–2260
Spolverato G et al (2015) Can hepatic resection provide a long-term cure for patients with intrahepatic cholangiocarcinoma? Cancer 121(22):3998–4006
Edge SB, Byrd D, Compton CC, Fritz AG, Greene FL, Trotti A (2010) AJCC cancer staging manual, 7th edn. Springer, New York
Mayo SC et al (2011) Refining the definition of perioperative mortality following hepatectomy using death within 90 days as the standard criterion. HPB (Oxford) 13(7):473–482
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240(2):205–213
Othus M et al (2012) Cure models as a useful statistical tool for analyzing survival. Clin Cancer Res 18(14):3731–3736
Tsodikov AD, Ibrahim JG, Yakovlev AY (2003) Estimating cure rates from survival data: an alternative to two-component mixture models. J Am Stat Assoc 98(464):1063–1078
ftp.cdc.gov/pub/Health_Statistics/NCHS/Publications/NVSR/62_07/
Miyazaki M et al (2015) Clinical practice guidelines for the management of biliary tract cancers 2015: the 2nd English edition. J Hepatobiliary Pancreat Sci 22(4):249–273
Chan E, Berlin J (2015) Biliary tract cancers: understudied and poorly understood. J Clin Oncol 33(16):1845–1848
Park JO et al (2015) Gemcitabine plus cisplatin for advanced biliary tract cancer: a systematic review. Cancer Res Treat 47(3):343–361
Kim Y et al (2015) Patient perceptions regarding the likelihood of cure after surgical resection of lung and colorectal cancer. Cancer 121(20):3564–3573
Pawlik TM et al (2014) What are patients’ expectations about the effects of chemotherapy for advanced cancer? J Am Coll Surg 219(3):588–590
Cai C et al (2012) smcure: an R-package for estimating semiparametric mixture cure models. Comput Methods Progr Biomed 108(3):1255–1260
De Angelis R et al (1999) Mixture models for cancer survival analysis: application to population-based data with covariates. Stat Med 18(4):441–454
Cai WK et al (2014) Preoperative serum CA19-9 levels is an independent prognostic factor in patients with resected hilar cholangiocarcinoma. Int J Clin Exp Pathol 7(11):7890–7898
Goetze TO (2015) Gallbladder carcinoma: prognostic factors and therapeutic options. World J Gastroenterol 21(43):12211–12217
Goere D et al (2013) Is there a possibility of a cure in patients with colorectal peritoneal carcinomatosis amenable to complete cytoreductive surgery and intraperitoneal chemotherapy? Ann Surg 257(6):1065–1071
Hosokawa I et al (2016) Long-term survival benefit and potential for cure after R1 resection for colorectal liver metastases. Ann Surg Oncol 23(6):1897–1905
Rama R, Swaminathan R, Venkatesan P (2010) Cure models for estimating hospital-based breast cancer survival. Asian Pac J Cancer Prev 11(2):387–391
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Additional information
Gaya Spolverato and Fabio Bagante contributed equally to this manuscript.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Spolverato, G., Bagante, F., Ethun, C.G. et al. Defining the Chance of Statistical Cure Among Patients with Extrahepatic Biliary Tract Cancer. World J Surg 41, 224–231 (2017). https://doi.org/10.1007/s00268-016-3691-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-016-3691-y