Abstract
Background
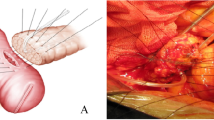
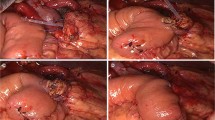
Among the types of pancreatic anastomosis used after pancreatoduodenectomy (PD), Blumgart type reconstruction has rapidly been distributed for its theoretical reasonableness, including secure tight adaptation of jejunal wall and pancreatic parenchyma without cause of parenchymal laceration. The clinical appropriateness of our modified Blumgart method was demonstrated by comparing to that of Kakita method.
Methods
Retrospective analysis of 156 patients underwent elective open PD, reconstructed former 78 patients with the Kakita method, utilizing a full-thickness penetrating suture for tight stump adhesion. The later 78 patients were treated with the modified Blumgart method, which involved clamping the pancreatic parenchymal stump by the jejunal seromuscular layers with horizontal mattress-type penetration sutures. Evaluated variables were the rate of pancreatic fistula (PF) and the length of postoperative hospital stay (POHS).
Results
The rate of ISGPF grade B + C PF was 29/78 (37.2 %) in the Kakita group and 16/78 (20.5 %) in the Blumgart group (P = 0.033). The median POHS for the Kakita group was 23 days, whereas that for the Blumgart group was 16 days (P < 0.001), one of the shortest value among Japanese high-volume centers. There was no perioperative intensive hemorrhage or deaths in either group.
Conclusion
A unique concept of Blumgart pancreatic anastomosis, i.e., utilizing the jejunum as an interstitial cushion to prevent pancreatic laceration at the knot site, has become realistic through a simple “one step” modification. This technique, also providing flexible handling space at main pancreatic duct anastomosis, should contribute to the improved PF prevention and shortening the POHS.



Similar content being viewed by others
References
Yeo CJ, Cameron JL, Sohn TA et al (1997) Six hundred fifty consecutive pancreaticoduodenectomies in the 1990 s: pathology, complications, and outcomes. Ann Surg 226:248–257
Buchler MW, Wagner M, Schmied BM et al (2003) Changes in morbidity after pancreatic resection: toward the end of completion pancreatectomy. Arch Surg 138:1310–1314
Bassi C, Dervenis C, Butturini G et al (2005) Postoperative pancreatic fistula: an international study group (ISGPF) definition. Surgery 138:8–13
Teh SH, Diggs BS, Deveney CW et al (2009) Patient and hospital characteristics on the variance of perioperative outcomes for pancreatic resection in the United States: a plea for outcome-based and not volume-based referral guidelines. Arch Surg 144:713–721
Harnoss JC, Ulrich AB, Harnoss JM et al (2014) Use and results of consensus definitions in pancreatic surgery: a systematic review. Surgery 155:47–57
Kimura W, Miyata H, Gotoh M et al (2014) A pancreaticoduodenectomy risk model derived from 8575 cases from a national single-race population (Japanese) using a web-based data entry system: the 30-day and in-hospital mortality rates for pancreaticoduodenectomy. Ann Surg 259:773–780
Poon RTP, Lo SH, Fong D et al (2002) Prevention of pancreatic anastomotic leakage after pancreaticoduodenectomy. Am J Surg 183:42–52
Duffas JP, Suc B, Msika S et al (2005) A controlled randomized multicenter trial of pancreatogastrostomy or pancreatojejunostomy after pancreatoduodenectomy. Am J Surg 189:720–729
Topal B, Fieuws S, Aerts R et al (2013) Pancreaticojejunostomy versus pancreaticogastrostomy reconstruction after pancreaticoduodenectomy for pancreatic or periampullary tumours: a multicentre randomised trial. Lancet Oncol 14:655–662
Kennedy EP, Yeo CJ (2011) Dunking pancreaticojejunostomy versus duct-to-mucosa anastomosis. J Hepatobiliary Pancreat Sci 18:769–774
Haane C, Mardin WA, Schmitz B et al (2013) Pancreatoduodenectomy–current status of surgical and perioperative techniques in Germany. Langenbecks Arch Surg 398:1097–1105
Peng SY, Wang JW, Lau WY et al (2007) Conventional versus binding pancreaticojejunostomy after pancreaticoduodenectomy: a prospective randomized trial. Ann Surg 245:692–698
Kakita A, Takahashi T, Yoshida M et al (1996) A simpler and more reliable technique of pancreatojejunal anastomosis. Surg Today 26:532–535
Kakita A, Yoshida M, Takahashi T (2001) History of pancreaticojejunostomy in pancreaticoduodenectomy: development of a more reliable anastomosis technique. J Hepatobilary Pancreat Surg 8:230–237
Satoi S, Toyokawa H, Yanagimoto H et al (2010) Is a nonstented duct-to-mucosa anastomosis using the modified Kakita method a safe procedure? Pancreas 39:165–170
Brennan M (2000) Pancreaticojejunostomy. In: Blumgart LH, Fong Y (eds) Surgery of the liver and biliary tract, 3rd edn. Saunders, New York, pp 1073–1089
Grobmyer SR, Kooby D, Blumgart LH et al (2010) Novel pancreaticojejunostomy with a low rate of anastomotic failure-related complications. J Am Coll Surg 210:54–59
Kleespies A, Rentsch M, Seeliger H et al (2009) Blumgart anastomosis for pancreaticojejunostomy minimizes severe complications after pancreatic head resection. Br J Surg 96:741–750
Fujii T, Sugimoto H, Yamada S et al (2014) Modified blumgart anastomosis for pancreaticojejunostomy: technical improvement in matched historical control study. J Gastrointest Surg 18:1108–1115
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Berger AC, Howard TJ, Kennedy EP et al (2009) Does type of pancreaticojejunostomy after pancreaticoduodenectomy decrease rate of pancreatic fistula? A randomized, prospective, dual-institution trial. J Am Coll Surg 208:738–747; discussion 747-739
Fong ZV, Ferrone CR, Thayer SP et al (2014) Understanding hospital readmissions after pancreaticoduodenectomy: can we prevent them?: a 10-year contemporary experience with 1,173 patients at the Massachusetts General Hospital. J Gastrointest Surg 18:137–144; discussion 144-135
Sugimoto M, Takahashi S, Gotohda N et al (2013) Schematic pancreatic configuration: a risk assessment for postoperative pancreatic fistula after pancreaticoduodenectomy. J Gastrointest Surg 17:1744–1751
Sakamoto Y, Kajiwara T, Esaki M et al (2009) Roux-en-Y reconstruction using staplers during pancreaticoduodenectomy: results of a prospective preliminary study. Surg Today 39:32–37
Tani M, Kawai M, Hirono S et al (2010) A prospective randomized controlled trial of internal versus external drainage with pancreaticojejunostomy for pancreaticoduodenectomy. Am J Surg 199:759–764
Kazaure HS, Roman SA, Sosa JA (2012) Association of postdischarge complications with reoperation and mortality in general surgery. Arch Surg 147:1000–1007
Hyder O, Dodson RM, Nathan H et al (2013) Influence of patient, physician, and hospital factors on 30-day readmission following pancreatoduodenectomy in the United States. JAMA Surg 148:1095–1102
Bassi C, Falconi M, Molinari E et al (2003) Duct-to-mucosa versus end-to-side pancreaticojejunostomy reconstruction after pancreaticoduodenectomy: results of a prospective randomized trial. Surgery 134:766–771
Acknowledgments
The authors thank Prof. Sata, from the Jichi medical University, Japan, for the useful discussion on the technique of modified Blumgart method.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Oda, T., Hashimoto, S., Miyamoto, R. et al. The Tight Adaptation at Pancreatic Anastomosis Without Parenchymal Laceration: An Institutional Experience in Introducing and Modifying the New Procedure. World J Surg 39, 2014–2022 (2015). https://doi.org/10.1007/s00268-015-3075-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-015-3075-8