Abstract
Introduction
The development of coagulopathy of trauma is multifactorial associated with hypoperfusion and consumption of coagulation factors. Previous studies have compared the role of factor replacement versus FPP for reversal of trauma coagulopathy. The purpose of our study was to determine the time to correction of coagulopathy and blood product requirement in patients who received PCC+FFP compared with patients who received FFP alone.
Methods
We performed a retrospective analysis of a prospectively maintained database of all coagulopathic (INR ≥ 1.5) trauma patients presenting to our level I trauma center during a 2-years period (2011–2012). Patients were stratified into two groups: patients who received PCC+FFP and patients who received FFP alone. Patients in the two groups were matched in a 1:3 (PCC+FFP:FFP) ratio using propensity score matching for demographics, injury severity, vital parameters, and initial INR. The two groups were then compared for: correction of INR, time to correction of INR, thromboembolic complications, mortality, and cost of therapy.
Results
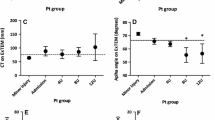
A total of 252 were included in the analysis [PCC+FFP:63; FFP:189]. The mean age was 44 ± 20 years; 70 % were male, with a median ISS score of 27 [16–38]. PCC use was associated with an accelerated correction of INR (394 vs. 1,050 min; p 0.001), reduction in requirement of pack red blood cell (6.6 vs. 10 units; p 0.001) and FFP (2.8 vs. 3.9 units; p 0.01), and decline in mortality (23 vs. 28 %; p 0.04). PCC+FFP use was associated with a higher cost of therapy ($1,470 ± 845 vs. 1,171 ± 949; p 0.01) but lower overall cost of transfusion ($7,110 ± 1,068 vs. 9,571 ± 1,524; p 0.01) compared with FFP therapy alone.
Conclusions
PCC in conjunction with FFP rapidly corrects INR in a matched cohort of trauma patients not on warfarin therapy compared with FFP therapy alone. The use of PCC as an adjunct to FFP therapy is associated with reduction of blood product requirement and also lowers overall cost.


Similar content being viewed by others
References
Spinella PC, Holcomb JB (2009) Resuscitation and transfusion principles for traumatic hemorrhagic shock. Blood Rev 23:231–240
Joseph B, Amini A, Friese RS (2012) Factor IX complex for the correction of traumatic coagulopathy. J Trauma Acute Care Surg 72(4):828–834
Joseph B, Hadjizacharia P, Aziz H et al (2013) Prothrombin complex concentrate: an effective therapy in reversing the coagulopathy of traumatic brain injury. J Trauma Acute Care Surg 74(1):248–253
Brohi K, Cohen MJ, Ganter MT (2007) Acute coagulopathy of trauma initiated by hypoperfusion modulated through the protein C pathway. Ann Surg 245(5):812–818
Darlington DN, Craig T, Gonzales MD et al (2013) Acute coagulopathy of trauma in the rat. Shock 39(5):440–446
Dickneite G, Pragst I (2009) Prothrombin complex concentrate vs fresh frozen plasma for reversal of dilutional coagulopathy in a porcine trauma model. Br J Anaesth 102:345–354
Dickneite G, Dorr B, Kaspereit F, Tanaka K (2010) Prothrombin complex concentrate versus recombinant factor VIIa for reversal of hemodilutional coagulopathy in a porcine trauma model. J Trauma 68:1151–1157
Stein DM, Dutton RP, Kramer ME, Handley C, Scalea TM (2008) Recombinant factor VIIa: decreasing time to neurosurgical intervention in patients with severe traumatic brain injury. J Trauma 64:620–628
Brown CV, Foulkrod KH, Lopez D (2010) Recombinant factor VIIa for the correction of coagulopathy before emergent craniotomy in blunt trauma patients. J Trauma 68(2):348–352
Stein DM, Dutton RP, Kramer ME, Scalea TM (2009) Reversal of coagulopathy in critically ill patients with traumatic brain injury: recombinant factor VIIa is more cost-effective than plasma. J Trauma 66(1):63–72
Joseph B, Aziz H, Zangbar B et al (2014) Acquired coagulopathy of traumatic brain injury defined by routine laboratory tests: which laboratory values matter? J Trauma Acute Care Surg 76(1):121–125
Santry HP, Alam HB (2010) Fluid resuscitation: past, present, and the future. Shock 33(3):229–241
Holcomb JB, Jenkins D, Rhee P et al (2007) Damage control resuscitation: directly addressing the early coagulopathy of trauma. J Trauma Acute Care Surg 62(2):307–310
Lauzier F, Cook D, Griffith L (2007) Fresh frozen plasma transfusion in critically ill patients. Crit Care Med 35(7):1655–1659
Demeyere R, Gillardin S, Arnout J et al (2010) Comparison of fresh frozen plasma and prothrombin complex concentrate for the reversal of oral anticoagulants in patients undergoing cardiopulmonary bypass surgery: a randomized study. Vox Sang 99(3):251–260
Sarode R, Matevosyan K, Bhagat R et al (2012) Rapid warfarin reversal: a 3-factor prothrombin complex concentrate and recombinant factor VIIa cocktail for intracerebral hemorrhage. J Neurosurg 116(3):491–497
Food and Drug Administration, Profilnine SD – Factor IX Complex, http://www.fda.gov/downloads/BiologicsBloodVaccines/BloodBloodProducts/ApprovedProducts/LicensedProductsBLAs/FractionatedPlasmaProducts/UCM261964.pdf
Holland L, Warkentin TE, Refaai M et al (2009) Suboptimal effect of a three-factor prothrombin complex concentrate (Profilnine-SD) in correcting supratherapeutic international normalized ratio due to warfarin overdose. Transfusion 49(6):1171–1177
Joseph B, Zangbar B, Pandit V et al (2014) The conjoint effect of reduced crystalloid administration and decreased damage-control laparotomy use in the development of abdominal compartment syndrome. J Trauma Acute Care Surg 76(2):457–461
Acknowledgments
This study has not been supported by anyone. The authors have no financial or proprietary interest in the subject matter or materials discussed in the manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Joseph, B., Aziz, H., Pandit, V. et al. Prothrombin Complex Concentrate Versus Fresh-Frozen Plasma for Reversal of Coagulopathy of Trauma: Is There a Difference?. World J Surg 38, 1875–1881 (2014). https://doi.org/10.1007/s00268-014-2631-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-014-2631-y