Abstract
Background
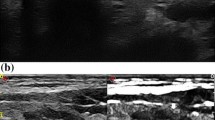
Identification and removal of small, non-palpable tumors located within previous surgical scar tissue is challenging and time consuming and may be associated with increased risk in patients with recurrent papillary thyroid carcinoma (PTC). The purpose of the present study was to present our surgeon-performed technique and to evaluate the usefulness of ultrasound-guided intratumoral indigo carmine injection (US-III) for intraoperative tumor localization in patients with recurrent PTC.
Methods
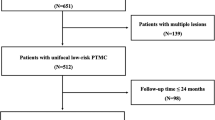
Sixteen patients with recurrent PTC in which tumors were <1.5 cm and not palpable were enrolled in this prospective study from January 2012 through March 2013.
Results
The mean size of the target tumors was 0.85 cm (range 0.4–1.3 cm) on preoperative US. The average time required for the US-III procedure was 7.7 min (range 5–11 min). The mean volume of injected indigo carmine was 0.56 mL (range 0.3–1.0 mL); this injection expanded the tumors by a mean of 0.2 cm (23.5 % increase compared with the initial tumor size; range 0.0–0.4 cm), increasing the mean size of the target tumors to 1.05 cm (range 0.5–1.5 cm). In 15 (93.8 %) of the 16 patients, the recurrent tumors were successfully removed with the aid of US-III. No complications occurred in any of the patients as a result of the US-III or subsequent surgeries.
Conclusions
US-III is a safe and effective technique that can be performed by the surgeon for the intraoperative localization of small non-palpable tumors within previous scar tissue in patients with recurrent PTC.



Similar content being viewed by others
References
Ahn D, Heo SJ, Park JH et al (2011) Clinical relationship between Hashimoto’s thyroiditis and papillary thyroid cancer. Acta Oncol 50:1228–1234
Jemal A, Siegel R, Ward E et al (2009) Cancer statistics, 2009. CA Cancer J Clin 59:225–249
Tang KT, Lee CH (2010) BRAF mutation in papillary thyroid carcinoma: pathogenic role and clinical implications. J Chin Med Assoc 73:113–128
Pacini F, Schlumberger M, Dralle H et al (2006) European consensus for the management of patients with differentiated thyroid carcinoma of the follicular epithelium. Eur J Endocrinol 154:787–803
Kim MK, Mandel SH, Baloch Z et al (2004) Morbidity following central compartment reoperation for recurrent or persistent thyroid cancer. Arch Otolaryngol Head Neck Surg 130:1214–1216
Kang TW, Shin JH, Han BK et al (2009) Preoperative ultrasound-guided tattooing localization of recurrences after thyroidectomy: safety and effectiveness. Ann Surg Oncol 16:1655–1659
Harari A, Sippel RS, Goldstein R et al (2012) Successful localization of recurrent thyroid cancer in reoperative neck surgery using ultrasound-guided methylene blue dye injection. J Am Coll Surg 215:555–561
Terzioglu T, Senyurek YG, Tunca F et al (2010) Excision efficiency of radioguided occult lesion localization in reoperative thyroid and parathyroid surgery. Thyroid 20:1271–1278
Sippel RS, Elaraj DM, Poder L et al (2009) Localization of recurrent thyroid cancer using intraoperative ultrasound-guided dye injection. World J Surg 33:434–439. doi:10.1007/s00268-008-9797-0
Hartl DM, Chami L, Al Ghuzlan A et al (2009) Charcoal suspension tattoo localization for differentiated thyroid cancer recurrence. Ann Surg Oncol 16:2602–2608
Triponez F, Poder L, Zarnegar R et al (2006) Hook needle-guided excision of recurrent differentiated thyroid cancer in previously operated neck compartments: a safe technique for small, nonpalpable recurrent disease. J Clin Endocrinol Metab 91:4943–4947
Duprez R, Lebas P, Marc OS et al (2010) Preoperative US-guided hook-needle insertion in recurrent lymph nodes of papillary thyroid cancer: a help for the surgeon. Eur J Radiol 73:40–42
Salhab M, Al Sarakbi W, Mokbel K (2005) Skin and fat necrosis of the breast following methylene blue dye injection for sentinel node biopsy in a patient with breast cancer. Int Semin Surg Oncol 2:26
Schultz P, Schwarz GA (1970) Radiculomyelopathy following intrathecal instillation of methylene blue. A hazard reaffirmed. Arch Neurol 22:240–244
Tukenmez M, Erbil Y, Barbaros U et al (2007) Radio-guided nonpalpable metastatic lymph node localization in patients with recurrent thyroid cancer. J Surg Oncol 96:534–538
Cooper DS, Doherty GM, Haugen BR et al (2009) Revised American Thyroid Association management guidelines for patients with thyroid nodules and differentiated thyroid cancer. Thyroid 19:1167–1214
Sugitani I, Toda K, Yamada K et al (2010) Three distinctly different kinds of papillary thyroid microcarcinoma should be recognized: our treatment strategies and outcomes. World J Surg 34:1222–1231. doi:10.1007/s00268-009-0359-x
Ito Y, Miyauchi A, Inoue H et al (2010) An observational trial for papillary thyroid microcarcinoma in Japanese patients. World J Surg 34:28–35. doi:10.1007/s00268-009-0303-0
Shin JE, Baek JH, Lee JH (2013) Radiofrequency and ethanol ablation for the treatment of recurrent thyroid cancers: current status and challenges. Curr Opin Oncol 25:14–19
Heilo A, Sigstad E, Fagerlid KH et al (2011) Efficacy of ultrasound-guided percutaneous ethanol injection treatment in patients with a limited number of metastatic cervical lymph nodes from papillary thyroid carcinoma. J Clin Endocrinol Metab 96:2750–2755
Lewis BD, Hay ID, Charboneau JW et al (2002) Percutaneous ethanol injection for treatment of cervical lymph node metastases in patients with papillary thyroid carcinoma. Am J Roentgenol 178:699–704
Peter C, Hongwan D, Kupfer A et al (2000) Pharmacokinetics and organ distribution of intravenous and oral methylene blue. Eur J Clin Pharmacol 56:247–250
Lee M, Sharifi R (1996) Methylene blue versus indigo carmine. Urology 47:783–784
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ahn, D., Sohn, J.H. & Kim, H. Surgeon-performed Intraoperative Tumor Localization in Recurrent Papillary Thyroid Carcinoma by Ultrasound-guided Intratumoral Indigo Carmine Injection. World J Surg 38, 1995–2001 (2014). https://doi.org/10.1007/s00268-014-2504-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-014-2504-4