Abstract
Background
We retrospectively investigated the prognostic significance of various clinicopathological factors and preoperative nutritional status to select patients with stage IV colorectal cancer (CRC) who will have a poor prognosis after palliative resection of the primary tumor.
Methods
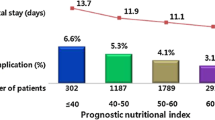
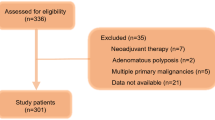
A total of 100 stage IV CRC patients who underwent palliative resection were enrolled. Various clinicopathological factors and Onodera’s prognostic nutritional index (OPNI) were evaluated to identify any possible relationship with the prognosis.
Results
At the time of the analysis, 83 patients had died, and the median survival time was 21 months. Of the 100 patients, 24 had primary tumor-related symptoms such as obstruction or bleeding. No significant correlation was noted between the OPNI and various clinicopathological factors. The multivariate analysis of patients without primary tumor-related symptoms revealed that the OPNI was an independent prognostic factor. The overall survival of the low-OPNI group was significantly worse than that of the high-OPNI group.
Conclusions
This retrospective study suggested that patients with a low OPNI may not be candidates for palliative resection, because it provides no survival benefit to these patients.

Similar content being viewed by others
References
Ries LA, Wingo PA, Millers DS et al (2000) The annual report to the nation on the status of cancer, 1973–1997, with a special section on colorectal cancer. Cancer 88:2398–2424
Morise Z, Sugioka A, Fujita J et al (2006) Does repeated surgery improve the prognosis of colorectal liver metastases? J Gastorointest Surg 10:6–11
Simmonds PC (2000) Palliative chemotherapy for advanced colorectal cancer: systemic review and meta-analysis. Colorectal Cancer Collaborative Group. Br Med J 321:531–535
Kemeny MM (2006) Surgery should be the primary treatment of synchronous colorectal metastasis in the asymptomatic patient. Ann Surg Oncol 13:140–141
Verbrene CJ, de Bock GH, Pijl MEJ et al (2011) Palliative resection of the primary tumor in stage IV rectal cancer. Colorectal Dis 14:314–319
Cook AD, Single R, McCahill LE (2005) Surgical resection of primary tumors in patients who present with stage IV colorectal cancer: an analysis of surveillance, epidemiology, and end results data, 1998–2000. Ann Surg Oncol 12:637–645
Konyalian VR, Rosing DK, Haukoos JS et al (2007) The role of primary tumor resection in patients with stage IV colorectal cancer. Colorectal Dis 9:430–437
Grothey A, Sargent D, Goldberg RM et al (2004) Survival of patients with advanced colorectal cancer improves with the availability of fluorouracil–leucovorin, irinotecan, and oxaliplatin in the course of treatment. J Clin Oncol 22:1209–1214
Saltz LB, Clarke S, Diaz-Rubio E et al (2008) Bevacizumab in combination with oxaliplatin-based chemotherapy as first line therapy in metastatic colorectal cancer: a randomized phase III study. J Clin Oncol 26:2013–2019
Van Custem E, Kohne CH, Hitre E et al (2009) Cetuximab and chemotherapy as initial treatment for metastatic colorectal cancer. N Engl J Med 360:1408–1417
Chibaudel B, Tournigand C, Andre T et al (2012) Therapeutic strategy in unresectable metastatic colorectal cancer. Ther Adv Med Oncol 4:75–89
Damjanov N, Weiss J, Haller DG (2009) Resection of primary colorectal cancer is not necessary in nonobstructed patients with metastatic disease. Oncologist 14:963–969
Rahban NN, Lordick F, Fink C et al (2012) Resection of the primary tumour versus no resection prior to systemic therapy in patients with colon cancer and synchronous unresectable metastases (UICC stageIV): SYNCHRONOUS: a randomized controlled multicenter trial (ISRCTN30964555). BMC Cancer 12:142–151
Poultsides GA, Paty PB (2011) Reassessing the need for primary tumor surgery in unresectable metastatic colorectal cancer: overview and perspective. Ther Adv Med Oncol 3:35–42
Katoh H, Yamashita K, Kokuba Y et al (2008) Surgical resection of stage IV colorectal cancer. World J Surg 32:1130–1137. doi:10.1007/s00268-008-9535-7
Delmore G (1997) Assessment of nutritional status in cancer patients: widely neglected? Support Care Cancer 5:376–380
Watanabe M, Iwatsuki M, Iwagami S et al (2012) Prognostic nutritional index predicts outcomes of gastrectomy in the elderly. World J Surg 36:1632–1639. doi:10.1007/s00268-012-1526-z
Nozoe T, Kimura Y, Ishida M et al (2002) Correlation of pre-operative nutritional condition with post-operative complications in surgical treatment for esophageal carcinoma. Eur J Surg Oncol 28:396–400
Pinato DJ, North BV, Sharma R (2012) A novel, externally validated inflammation-based prognostic algorithm in hepatocellular carcinoma: the prognostic nutritional index (PNI). Br J Cancer 106:1439–1445
Onodera T, Goseki N, Kosaki G (1984) Prognostic nutritional index in gastrointestinal surgery of malnourished cancer patients. Nippon Geka Gakkai Zasshi 85:1001–1005 in Japanese; English abstract
Nozoe T, Kohno M, Iguchi T et al (2012) The prognostic nutritional index can be a prognostic indicator in colorectal carcinoma. Surg Today 42:532–535
Sobin L, Gospodarowicz M, Wittekind C (2009) International Union Against Cancer. TNM classification of malignant tumors, 7th edn. Wiley-Blackwell, New York, pp 73–77
Chapman MA, Buckley D, Henson DB et al (1998) Preoperative carcinoembryonic antigen is related to tumor stage and long-term survival in colorectal cancer. Br J Cancer 78:1346–1349
Colotta F, Allavena P, Sica A et al (2009) Cancer-related inflammation, the seventh hallmark of cancer: link to genetic instability. Carcinogenesis 30:1073–1081
Argiles JM, Busquets S, Lopez-Soriano FJ (2003) Cytokines in the pathogenesis of cancer cachexia. Curr Opin Clin Nutr Metab Care 6:401–406
Beleo-Tome C, Monteiro-Grillo I, Camilo M et al (2012) Validation of the malnutrion universal screening tool (MUST) in cancer. Br J Nutr 108:343–348
Kondrup J, Allison SP, Elia M et al (2003) ESPEN guidelines for nutrition screening 2002. Clin Nutr 22:415–421
Burden ST, Hill J, Shaffer JL et al (2010) Nutritional status of preoperative colorectal cancer patients. J Hum Nutr Diet 23:402–407
Dewys WD, Begg C, Lavin PT et al (1980) Prognostic effect of weight loss prior to chemotherapy in cancer patients. Eastern Cooperative Oncology Group. Am J Med 69:491–497
Ross PJ, Ashley S, Norton A et al (2004) Do patients with weight loss have a worse outcome when undergoing chemotherapy for lung cancers? Br J Cancer 90:1905–1911
Murry DJ, Riva L, Poplack DG et al (1998) Impact of nutrition on pharmacokinetics of anti-neoplastic agents. Int J Cancer Suppl 11:48–51
Zhang Y, Gu Y, Guo T et al (2012) Perioperative immunonutrition for gastrointestinal cancer: a systematic review of randomized controlled trial. Surg Oncol 21:87–95
Conflict of interest
There is no financial support or relationship that may pose any conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Maeda, K., Shibutani, M., Otani, H. et al. Low Nutritional Prognostic Index Correlates with Poor Survival in Patients with Stage IV Colorectal Cancer Following Palliative Resection of the Primary Tumor. World J Surg 38, 1217–1222 (2014). https://doi.org/10.1007/s00268-013-2386-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-013-2386-x