Abstract
Background
Laparoscopy has been widely used for surgical repair of large paraesophageal hernias (PEHs). The technique, however, entails substantial technical difficulties, such as repositioning the stomach in the abdominal cavity, sac excision, closure of the hiatal gap, and fundoplication. Knowledge of the long-term outcome (>10 years) is scarce. The aim of this article was to evaluate the long-term results of this approach, primarily the anatomic hernia recurrence rate and the impact of the repair on quality of life.
Methods
We identified all patients who underwent laparoscopic repair for PEH between November 1997 and March 2007 and who had a minimum follow-up of 48 months. In March 2011, all available patients were scheduled for an interview, and a radiologic examination with barium swallow was performed. During the interview the patients were asked about the existence/persistence of symptoms. An objective score test, the gastrointestinal quality of life index (GIQLI), was also administered.
Results
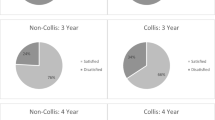
A total of 77 patients were identified: 17 men (22 %) and 60 women (78 %). The mean age at the time of fundoplication was 64 years (range 24–87 years) and at the review time 73 years (range 34–96 years). The amount of stomach contained within the PEH sac was <50 % in 39 patients (50 %), >50 % in 31 (40 %), and 100 % (intrathoracic stomach) in 7 (9.5 %). A 360º PTFe mesh was used to reinforce the repair in six cases and a polyethylene mesh in three. In May 2011, 55 of the 77 patients were available for interview (71 %), and the mean follow-up was 107 months (range 48–160 months). Altogether, 43 patients (66 %) were asymptomatic, and 12 (21 %) reported symptoms that included dysphagia in 7 patients, heartburn in 3, belching in 1, and chest pain in 1. Esophagography in 43 patients (78 %) revealed recurrence in 20 (46 %). All recurrences were small sliding hernias (<3 cm long). In all, 37 patients (67 %) answered the GIQLI questionnaire. The mean GIQLI score was 111 (range 59–137; normal 147). Patients with objective anatomic recurrence had a quality of life index of 110 (range 89–132) versus 122 in the nonrecurrent hernia group (range 77–138, p < 0.01). Mesh was used to buttress the esophageal hiatus in nine patients. One patient died during the follow-up period. Five of the remaining eight patients (62 %) developed dysphagia, a mesh-related symptom. Three patients required reoperation because of mesh-related complications. Esophagography revealed recurrence in four (50 %) of the eight patients. GIQLI scores were similar in patients with recurrence (126, range 134–119) and without it (111, range 133–186) (p > 0.05).
Conclusions
Long-term follow-up (up to 160 months) in our study showed that laparoscopic PEH repair is clinically efficacious but is associated with small anatomic recurrences in ≤50 % of patients. Further studies are needed to identify the anatomic, pathologic, and physiological factors that may impair outcome, allowing the procedure to be tailored to each patient.

Similar content being viewed by others
References
Schieman C, Grondin SC (2009) Paraesophageal hernia: clinical presentation, evaluation, and management controversies. Thorac Surg Clin 19:473–478
Nason KS, Luketich JD, Witteman BP et al (2012) The laparoscopic approach to paraesophageal hernia repair. J Gastrointest Surg 16:417–426
Hashemi M, Peters JH, DeMeester TR et al (2000) Laparoscopic repair of large type III hiatal hernia: objective followup reveals high recurrence rate. J Am Coll Surg 190:553–560
Targarona EM, Novell J, Vela S et al (2004) Mid term analysis of safety and quality of life after the laparoscopic repair of paraesophageal hiatal hernia. Surg Endosc 18:1045–1050
Furnee EJ, Draaisma WA, Simmermacher RK et al (2010) Long-term symptomatic outcome and radiologic assessment of laparoscopic hiatal hernia repair. Am J Surg 199:695–701
Dallemagne B, Kohnen L, Perretta S et al (2011) Laparoscopic repair of paraesophageal hernia: long-term follow-up reveals good clinical outcome despite high radiological recurrence rate. Ann Surg 253:291–296
Luketich JD, Nason KS, Christie NA et al (2010) Outcomes after a decade of laparoscopic giant paraesophageal hernia repair. J Thorac Cardiovasc Surg 139:395–404
Braghetto I, Korn O, Csendes A et al (2010) Postoperative results after laparoscopic approach for treatment of large hiatal hernias: is mesh always needed? Is the addition of an antireflux procedure necessary? Int Surg 95:80–87
Zaninotto G, Portale G, Costantini M et al (2007) Objective follow-up after laparoscopic repair of large type III hiatal hernia: assessment of safety and durability. World J Surg 31:2177–2183. doi:10.1007/s00268-007-9212-2
Mittal SK, Bikhchandani J, Gurney O et al (2011) Outcomes after repair of the intrathoracic stomach: objective follow-up of up to 5 years. Surg Endosc 25:556–566
Louie BE, Blitz M, Farivar AS et al (2011) Repair of symptomatic giant paraesophageal hernias in elderly (>70 years) patients results in improved quality of life. J Gastrointest Surg 15:389–396
Eypasch E, Williams JI, Wood-Dauphinee S et al (1995) Gastrointestinal quality of life index: development, validation and application of a new instrument. Br J Surg 82:216–222
Quintana JM, Cabriada J, López de Tejada I et al (2001) Translation and validation of the gastrointestinal quality of life index (GIQLI). Rev Esp Enferm Dig 93:693–706
Oelschlager BK, Petersen RP, Brunt LM et al (2012) Laparoscopic paraesophageal hernia repair: defining long-term clinical and anatomic outcomes. J Gastrointest Surg 16:453
Targarona EM, Bendahan G, Balague C et al (2004) Mesh in the hiatus: a controversial issue. Arch Surg 139:1286–1296
Herbella FA, Patti MG (2011) Hiatal mesh repair: current status. Surg Laparosc Endosc Percutan Tech 21:61–66
Stadlhuber RJ, Sherif AE, Mittal SK et al (2009) Mesh complications after prosthetic reinforcement of hiatal closure: a 28-case series. Surg Endosc 23:1219–1226
Oelschlager BK, Pellegrini CA, Hunter JG et al (2011) Biologic prosthesis to prevent recurrence after laparoscopic paraesophageal hernia repair: long term follow up from a prospective randomized trial. J Am Coll Surg 213:461–468
Conflict of interest
Drs. Eduardo M. Targarona, Samuel Grisales, Ozlem Uyanik, Carmen Balague, Juan Carlos Pernas, and Manuel Trias, have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Targarona, E.M., Grisales, S., Uyanik, O. et al. Long-Term Outcome and Quality of Life After Laparoscopic Treatment of Large Paraesophageal Hernia. World J Surg 37, 1878–1882 (2013). https://doi.org/10.1007/s00268-013-2047-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-013-2047-0