Abstract
Background
Efficient blood transfusion management presents an ongoing challenge for many trauma centers. We present the Emergency Transfusion Score (ETS), a measure that may allow important time and cost savings in the treatment of severely injured patients in the Emergency Room (ER).
Methods
The ETS includes the parameters low blood pressure, free fluid on ultrasound, clinical instability of the pelvic ring, age, admission from the scene, and trauma mechanism. An ETS ≥ 3 indicates a transfusion probability of 5% and was set as the cut-off to order blood products (10 packed red blood cells [PRBC]/10 fresh frozen plasma [FFP]).
Results
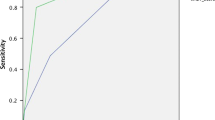
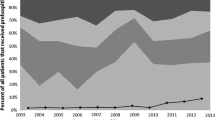
A total of 481 patients requiring trauma team activation (ISS 18 ±18; 7/03–12/04) were prospectively included. The ETS was < 3 in 306 patients (64%) and ≥ 3 in 175 subjects (36%). Some 40 patients (8.3%) received blood (8 ± 8 PRBC) after 23 ± 9 min during ER treatment, and 39 of these patients had an ETS of ≥ 3 (5.4 ± 1.5 points). Sensitivity of the ETS was 97.5%; specificity, 68%. Positive predictive value of the ETS was 0.222; negative predictive value, 0.998.
Conclusions
(1) The ETS is a safe and highly sensitive tool with which to detect severely injured patients in need of blood products. (2) The ETS is highly predictive for patients not in need of PRBC (negative predictive value 0.998) and helps to avoid unnecessary cross-matching and transport. (3) After implementation of the ETS, a sum of about 109,296 USD was saved per year by reducing the costs for cross-matching, transportation, and wasted blood products.
Similar content being viewed by others
References
American College of Surgeons Committee on Trauma (1999) Resources for Optimal Care of the Injured Patient. American College of Surgeons, Chicago
Zimmer-Gembeck MJ, Southard PA, Hedges JR, et al. (1995) Triage in an established trauma system. J Trauma 39:922–928
Ruchholtz S, Pehle B, Lewan U, et al. (2006). The emergency room transfusion score (ETS): prediction of blood transfusion requirement in initial resuscitation after severe trauma. Transfus Med 16:49–56
MacLeod JB, Lynn M, McKenney MG, et al. (2003). Early coagulopathy predicts mortality in trauma. J Trauma 55:39–44
Clarke JR, Davidson SJ, Bergman GE, et al. (1980). Optimal blood ordering for emergency department patients. Ann Emerg Med 9:2–6
Baker JB, Korn CS, Robinson K, et al. (2001). Type and crossmatch of the trauma patient. J Trauma 50:878–881
West HC, Jurkovich G, Donnell C, et al. (1989). Immediate prediction of blood requirements in trauma victims. South Med J 82:186–189
Hooker EA, Miller FB, Hollander JL, et al. (1994). Do all trauma patients need early crossmatching for blood? J Emerg Med 12:447–451
Yucel N, Lefering R, Maegele M, et al.; the Polytrauma Study Group of the German Trauma Society (2006) Trauma Associated Severe Hemorrhage (TASH) score: probability of mass transfusion as surrogate for life threatening hemorrhage after multiple trauma. J Trauma 60:1228–1236
Ruchholtz S, Waydhas C, Lewan U, et al. (2002). A multidisciplinary quality management system for the early treatment of severely injured patients: implementation and results in two trauma centers. Intensive Care Med 28:1395–1404
Starr AJ, Griffin DR, Reinert CM, et al. (2002) Pelvic ring disruptions: prediction of associated injuries, transfusion requirement, pelvic arteriography, complications and mortality. J Orthop Trauma 16:553–561
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kuhne, C.A., Zettl, R.P., Fischbacher, M. et al. Emergency Transfusion Score (ETS): A Useful Instrument for Prediction of Blood Transfusion Requirement in Severely Injured Patients. World J Surg 32, 1183–1188 (2008). https://doi.org/10.1007/s00268-007-9425-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-007-9425-4