Abstract
Aim
The aim of this study was to evaluate the preoperative physiological risk profile for postoperative morbidity and mortality after emergency treatment of complicated peptic ulcer disease (PUD).
Methods
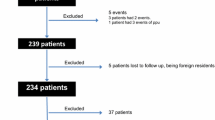
Operative notes and hospital files of 261 patients—111 female, 150 male; median age 67 years (range 17–100 years)—undergoing an emergency operation from 1993 to 2005 were analyzed retrospectively. The physiologic subscore of the POSSUM score (POSSUM-phys) was analyzed with regard to predicting postoperative complications. Follow-up was obtained from questionnaires sent to family practitioners or by patient interviews.
Results
The overall complication rate was 44%, and mortality was 24%. Among risk factors studied (e.g., sex, patient’s age, duration of symptoms, type of surgery), a high POSSUM-phys score was the strongest predictor for postoperative sepsis, anastomotic/suture dehiscence, postoperative bleeding, and mortality. Cut points for patients at risk could be calculated. Surgical procedures (organ-preserving versus resection) had no influence when matched for POSSUM-phys score. Nevertheless, organ resections were associated with higher scores. Recurrent PUD was a rare event (7.6%).
Conclusion
The preoperative physiologic POSSUM score is a promising instrument for identifying patients at increased risk to develop major postoperative complications after emergency surgery for complicated PUD. Prospective studies are needed to prove its applicability for adjusting treatment to individual patients.




Similar content being viewed by others
References
Mikulicz J (1885) Ueber Laparotomie bei Magen- und Darmperforation. Leipzig, Breitkopf
Svanes K, Stangeland L, Viste A, et al. (1995) Morbidity, ability to swallow, and survival, after oesophagectomy for cancer of the oesophagus and cardia. Eur J Surg 161:669–675
Svanes C, Ovrebo K, Soreide O (1996) Ulcer bleeding and perforation: non-steroidal anti-inflammatory drugs or Helicobacter pylori. Scand J Gastroenterol Suppl 220:128–131
Lassen A, Hallas J, Schaffalitzky de Muckadell OB (2006) Complicated and uncomplicated peptic ulcers in a Danish county 1993–2002: a population-based cohort study. Am J Gastroenterol 101:945–953
Gisbert JP, Legido J, Garcia-Sanz I, et al. (2004) Helicobacter pylori and perforated peptic ulcer prevalence of the infection and role of non-steroidal anti-inflammatory drugs. Dig Liver Dis 36:116–120
Wolfe MM, Lichtenstein DR, Singh G (1999) Gastrointestinal toxicity of nonsteroidal antiinflammatory drugs. N Engl J Med 340:1888–1899
Paimela H, Tuompo PK, Perakyl T, et al. (1991) Peptic ulcer surgery during the H2-receptor antagonist era: a population-based epidemiological study of ulcer surgery in Helsinki from 1972 to 1987. Br J Surg 78:28–31
Stabile BE, Passaro E Jr (1993) Surgery for duodenal and gastric ulcer disease. Adv Surg 26:275–306
Marshall BJ, Warren JR (1984) Unidentified curved bacilli in the stomach of patients with gastritis and peptic ulceration. Lancet 1:1311–1315
Dubois F (2000) New surgical strategy for gastroduodenal ulcer: laparoscopic approach. World J Surg 24:270–276
Zittel TT, Jehle EC, Becker HD (2000) Surgical management of peptic ulcer disease today: indication, technique and outcome. Langenbecks Arch Surg 385:84–96
Copeland GP, Jones D, Walters M (1991) POSSUM: a scoring system for surgical audit. Br J Surg 78:355–360
Bobrzynski A, Beben P, Budzynski A, et al. (2002) Incidence of complications of peptic ulcers in patients with Helicobacter pylori (Hp) infection and/or NSAID use in the era of Hp eradication. Med Sci Monit 8:CR554–557
Paimela H, Oksala NK, Kivilaakso E (2004) Surgery for peptic ulcer today: a study on the incidence, methods and mortality in surgery for peptic ulcer in Finland between 1987 and 1999. Dig Surg 21:185–191
Schwesinger WH, Page CP, Sirinek KR, et al. (2001) Operations for peptic ulcer disease: paradigm lost. J Gastrointest Surg 5:438–443
Bulut OB, Rasmussen C, Fischer A (1996) Acute surgical treatment of complicated peptic ulcers with special reference to the elderly. World J Surg 20:574–577
Lipof T, Shapiro D, Kozol RA (2006) Surgical perspectives in peptic ulcer disease and gastritis. World J Gastroenterol 12:3248–3252
Behrman SW (2005) Management of complicated peptic ulcer disease. Arch Surg 140:201–208
Bornman PC, Krige JE (2004) New paradigms in the management of complicated peptic ulcers: the final requiem for vagotomy? S Afr J Surg 42:113–115
Noguiera C, Silva AS, Santos JN, et al. (2003) Perforated peptic ulcer: main factors of morbidity and mortality. World J Surg 27:782–787
Wysocki A, Biesiada Z, Beben P, et al. (2000) Perforated gastric ulcer. Dig Surg 17:132–137
Makela JT, Kiviniemi H, Ohtonen P, et al. (2002) Factors that predict morbidity and mortality in patients with perforated peptic ulcers. Eur J Surg 168:446–451
Testini M, Portincasa P, Piccinni G, et al. (2003) Significant factors associated with fatal outcome in emergency open surgery for perforated peptic ulcer. World J Gastroenterol 9:2338–2340
Hall JC, Hall JL (1996) ASA status and age predict adverse events after abdominal surgery. J Qual Clin Pract 16:103–108
Jones HJ, de Cossart L (1999) Risk scoring in surgical patients. Br J Surg 86:149–157
Sillakivi T, Lang A, Tein A, et al. (2000) Evaluation of risk factors for mortality in surgically treated perforated peptic ulcer. Hepatogastroenterology 47:1765–1768
Blomgren LG (1997) Perforated peptic ulcer: long-term results after simple closure in the elderly. World J Surg 21:412–414; discussion 414–415
Hermansson M, Stael von Holstein C, Zilling T (1999) Surgical approach and prognostic factors after peptic ulcer perforation. Eur J Surg 165:566–572
Tsugawa K, Koyanagi N, Hashizume M, et al. (2001) The therapeutic strategies in performing emergency surgery for gastroduodenal ulcer perforation in 130 patients over 70 years of age. Hepatogastroenterology 48:156–162
Gilliam AD, Speake WJ, Lobo DN, et al. (2003) Current practice of emergency vagotomy and Helicobacter pylori eradication for complicated peptic ulcer in the United Kingdom. Br J Surg 90:88–90
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Egberts, JH., Summa, B., Schulz, U. et al. Impact of Preoperative Physiological Risk Profile on Postoperative Morbidity and Mortality After Emergency Operation of Complicated Peptic Ulcer Disease. World J Surg 31, 1449–1457 (2007). https://doi.org/10.1007/s00268-007-9061-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-007-9061-z