Abstract
Background
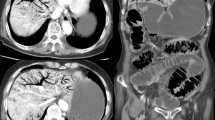
Portal venous gas (PVG) has been reported to be associated with lethal surgical diagnosis. Recent studies tend to confirm the clinical significance of gas in the portal vein; however, some patients are managed without surgical treatment. The aim of this study was to assess both the diagnoses and the treatment of patients with PVG in an emergency surgical setting.
Materials and methods
We performed a retrospective chart review of 15 patients with PVG in the emergency setting detected by computed tomography (CT) between July 1999 and July 2004. Characteristics assessed included age, sex, clinical presentation, first CT diagnosis of both PVG and the underlying pathology, American Society of Anesthesiologists (ASA) score, surgical findings, final clinical diagnosis, duration of hospitalization, and evolution of the illness/mortality. All patients were examined one month after operation.
Results
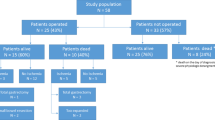
This series of 5 women and 10 men ranged in age from 38 to 90 years at the time they underwent emergency surgical treatment. The mean preoperative ASA score was 4.20. Computed tomography diagnosed the underlying pathology in all cases: bowel obstruction (4 cases), bowel necrosis (9 cases), and diffuse peritonitis (2 cases). The mean length of hospital stay was 12.4 days. The mortality rate was 46.6%; (7 patients).
Conclusions
A wide range of pathologies can generate PVG. Computed tomography can detect both the presence of gas and the underlying pathology. In emergency situations, all the diagnosed causal pathologies required a surgical procedure without delay. We report that the prognosis was related to the pathology itself and was not influenced by the presence of PVG.
Similar content being viewed by others
REFERENCES
Liebman PR, Patten MT, Manny J, et al. Hepatic-portal venous gas in adults: etiology, pathophysiology and clinical significance. Ann Surg 1978;187:281–287
Wolfe JN, Evans WA. Gas in the portal veins of the liver in infants: a roentgenographic demonstration with postmortem anatomical correlation. AJR Am J Roentgenol 1955;74:486–489
Beyer W. CRC Standard Probability and Statistics Tables. Boca Raton, FL, CRC Press 1991:154
Hong JJ, Gadaleta D, Rossi P, et al. Portal vein gas, a changing clinical entity. Report of 7 patients and review of the literature. Arch Surg 1997;132:1071–1075
Iannitti DA, Gregg SC, Mayo-Smith WW, et al. Portal venous gas detected by computed tomography: is surgery imperative? Dig Surg 2003;20:306–315
Kinoshita H, Shinozaki M, Tanimura H, et al. Clinical features and management of hepatic portal venous gas: four case reports and cumulative review of the literature. Arch Surg 2001;136:1410–1414
Faberman RS, Mayo-Smith WW. Outcome of 17 patients with portal venous gas detected by CT. AJR Am J Roentgenol 1997;169:1535–1538
Chevallier P, Peten E, Souci J, et al. Detection of portal venous gas on sonography, but not on CT. Eur Radiol 2002;12:1175–1178
Griffiths DM, Gough MH. Gas in the hepatic portal veins. Br J Surg 1986;73:172–176
Venugopal C, Colley DP. Portal venous gas in a patient with Crohn’s disease. J Clin Gastroenterol 1990;12:595–597
Lee CS, Kuo YC, Peng SM, et al. Sonographic detection of hepatic portal venous gas associated with suppurative cholangitis. J Clin Ultrasound 1993;21:331–334
Schulze CG, Blum U, Haag K. Hepatic portal venous gas. Imaging modalities and clinical significance. Acta Radiol 1995;36:377–378
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Monneuse, O., Pilleul, F., Barth, X. et al. Portal Venous Gas Detected on Computed Tomography in Emergency Situations: Surgery Is Still Necessary. World J Surg 31, 1066–1072 (2007). https://doi.org/10.1007/s00268-006-0589-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-006-0589-0