Abstract
Background
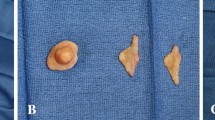
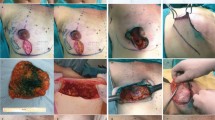
The surgical goals of gender reassignment surgery of the breast in female-to male transsexuals (FMT) is the aesthetic shaping of a male thoracic wall with minimal scarring, while preserving the sensitivity of the nipple-areola complex (NAC). For large and ptotic breasts, we perform a mastectomy over an inframammary access with inferior pedicled NAC under color Doppler visualization of the perforators. This paper presents the technique, including complications and assessment of quality of life, as part of a unicentric analysis.
Methods
This was a retrospective analysis of 23 patients (46 mastectomies) performed between September 2014 and September 2020. The complication rate and the number of corrective surgeries were recorded for quality assessment. A semiquantitative score was used to evaluate aesthetic outcome, nipple sensitivity, quality of life, and sexuality.
Results
A total of 46 mastectomies were performed in 23 patients. The patient survey showed high patient satisfaction. Loss of nipple sensitivity was observed after one mastectomy (2.17%). In 91.67% of cases, patients reported that their appearance reflected how they feel on the inside. In 75% of cases, patients reported feeling equal to other men. The overall complication rate was 10.87%. Shape correction due to persistent excess of volume was rare (2.17%, equivalent to one mastectomy).
Conclusion
Subcutaneous mastectomy with inferior nipple pedicle can be performed with a high degree of safety and satisfaction in FMT. Color Doppler-guided visualization of the perforator vessels is helpful in allowing a thin pedicle preparation, thus reducing the need for secondary surgeries to optimize the shape.
Level of Evidence IV
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.





Similar content being viewed by others
References
Blanchard R, Clemmensen LH, Steiner BW (1987) Heterosexual and homosexual gender dysphoria. Arch Sex Behav 16(2):139–152
Cohen-Kettenis PT, Gooren LJ (1999) Transsexualism: a review of etiology, diagnosis and treatment. J Psychosom Res 46(4):315–333
van de Grift TC, Cohen-Kettenis PT, Steensma TD, De Cuypere G, Richter-Appelt H, Haraldsen IRH, Dikmans REG, Cerwenka SC, Kreukels BPC, Steensma TD (2016) Body satisfaction and physical appearance in gender dysphoria. Arch Sex Behav 45(3):575–585
Lindsay WRN (1979) Creation of a male chest in female transsexuals. Ann Plast Surg 3(1):39–46
Hage JJ, Kesteren PJ (1995) Chest-wall contouring in female-to-male transsexuals: basic considerations and review of the literature. Plast Reconstr Surg 96(2):386–391
Hage JJ, Bloem JJ (1995) Chest-wall contouring for female-to-male transsexuals: Amsterdam experience. Ann Plast Surg 34(1):59–66
Beek TF, Kreukels BPC, Cohen-Kettenis PT, Steensma TD (2015) Partial treatment requests and underlying motives of applicants for gender affirming interventions. J Sex Med 12(11):2201–2205
Monstrey SJ, Ceulemans P, Hoebeke P (1992) Sex reassignment surgery in the female-to-male transsexual. Semin Plast Surg 25(3):229–244
Kornstein AN, Cinelli PB (1992) Inferior pedicle reduction technique for larger forms of gynecomastia. Aesthetic Plast Surg 16(4):331–335
Morselli PG, Summo V, Pinto V, Fabbri E, Meriggiola MC (2019) Chest-wall masculinization in female-to-male transsexuals. Ann Plast Surg 83(6):629–635
Monstrey S, Salvaggi G, Ceulemans P, van Landuyt K, Bowman C, Blondeel P, Hamdi M, De Cuypere G (2008) Chest-wall contouring surgery in female-to-male transsexuals: a new algorithm. Plast Reconstr Surg 121(3):849–859
Wolter A, Diedrichson J, Scholz T, Arens-Landwehr A, Liebau J (2015) Sexual reassignment surgery in female-to-male transsexuals: an algorithm for subcutaneous mastectomy. J Plast Reconstr Aesthetic Surg 68(2):184–191
Kühn S, Keval S, Sader R, Küenzlen L, Kiehlmann M, Djedovic G, Bozkurt A, Rieger UM (2019) Mastectomy in female-to-male transgender patients: a single-center 24-years retrospective analysis. Arch Plast Surg 46(5):433–440
Pusic AL, Klassen AF, Scott AM, Klok JA, Cordeiro PG, Cano SJ (2009) Development of a new patient-reported outcome measure for breast surgery: the BREAST-Q. Plast reconstr surg 124(2):345–353
Becker I, Nieder TO, Cerwenka S, Briken P, Kreukels BPC, Cohen-Kettenis PT, De Cuypere G, Hebold Haraldsen IR, Richter-Appelt H (2016) Body image in young gender dysphoric adults: a European multi-center study. Arch Sex Behav 45(3):559–574
Takayani S, Nakagawa C (2006) Chest wall contouring for female-to-male transsexuals. Aesthetic Plast Surg 30(2):206–212
Cregten-Escobar P, Bouman MB, Buncamper ME, Mullender MG (2012) Subcutaneous mastectomy in female-to-male transexuals: a retrospective cohort-analysis of 202 patients. J Sex Med 9(12):3148–3153
Ginsberg BA (2016) Dermatologic care of transgender patients. Int J Womens Dermatol 3(1):65–67
Marks DH, Awosika O, Rengifo-Pardo M, Ehrlich A (2019) Dermatologic surgical care for transgender individuals. Dermatol Surg 45(3):446–457
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflicts of interest to disclose.
Ethical standards
The study was performed in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
Written informed consent was obtained from all Patients.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Caro, C., Florek, A., Hahn, M. et al. Color Doppler Sonography Assisted Subcutaneous Mastectomy with Inferior Pedicled Nipple-Areola Complex in Female-to-Male Transsexuals: A Retrospective Cohort Analysis. Aesth Plast Surg 48, 1126–1132 (2024). https://doi.org/10.1007/s00266-022-02945-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-022-02945-0