Abstract
Background
In this study, we investigated the effect of matrix metalloproteinase-1 (MMP-1) on wound healing on skin in a model produced in rats.
Methods
Sixteen Sprague–Dawley male rats were included in the study. The four full-thickness skin wound was created on the dorsal area of each rat with 4.4 mm punch. The rats were randomly divided into two groups. MMP-1 and saline were administered intraperitoneally once daily for 7 days. The biopsies were taken from the separate wounds on the 4th, 7th, 14th and 21st days of the experiment. The lymphocytic response, vascular proliferation, fibroblast proliferation, epithelial hyperplasia, foreign body reaction, ulcer formation, acute inflammation, keloid scar formation and hypertrophic scar formation were compared in each group in histopathologically.
Results
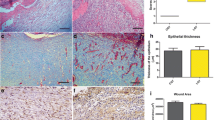
In our study, epithelial hyperplasia on 14th day was significantly higher in the MMP-1 group compared to the control group (p < 0.05). The lymphocytic response on 4th and 21th days, the vascular proliferation on 4th day, the fibroblast proliferation on 4th and 7th days, the acute inflammation on 4th day and the hypertrophic scar formation on 7th, 14th, 21st days were significantly lower in the MMP-1 group compared to the control group (p < 0.05). No statistically significant difference was found in comparison with other parameters (p > 0.05).
Conclusions
MMP-1 improves the wound-healing process of skin with higher epithelial hyperplasia and reduces scar formation in the animal model. Therefore, MMP-1 can potentially be used as an effective anti-fibrogenic agent for preventing or treating the hypertrophic scar.
No Level Assigned
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.


Similar content being viewed by others
References
Martin P (1997) Wound healing: aiming for perfect skin regeneration. Science 276(5309):75–81
Çakan D, Aydın S, Demir G, Başak K (2019) The effect of curcumin on healing in an animal nasal septal perforation model. Laryngoscope 129(10):E349–E354
Bayat A, McGrouther DA, Ferguson MW (2003) Skin scarring. BMJ 326:88–92
Brown BC, McKenna SP, Siddhi K, McGrouther DA, Bayat A (2008) The hidden cost of skin scars: quality of life after skin scarring. J Plast Reconstr Aesthet Surg 61(9):1049–1058
Tyack Z, Ziviani J, Kimble R, Plaza A, Jones A, Cuttle L, Simons M (2015) Measuring the impact of burn scarring on health-related quality of life: development and preliminary content validation of the Brisbane Burn Scar Impact Profile (BBSIP) for children and adults. Burns 41(7):1405–1419
Ogawa R (2010) The most current algorithms for the treatment and prevention of hypertrophic scars and keloids. Plast Reconstr Surg 125:557–568
Berman B, Maderal A, Raphael B (2017) Keloids and hypertrophic scars: pathophysiology, classification, and treatment. Dermatol Surg 43(Suppl 1):3–18
Sund B (2000) New developments in wound care. London: PJB Publications, pp 1–255, (Clinica Report CBS 836)
İkizoğlu G (2008) Ekstraselüler matriks, kan damarları ve sinirlerin biyolojisi. In: Tüzün Y, Gürer MA, Serveroğlu S, Oğuz O, Aksungur LA (eds), Dermatoloji. 3. baskı. İstanbul, Nobel Tıp Kitabevleri, 2008: 33–39
Lo DD, Zimmermann AS, Nauta A, Longaker MT, Lorenz HP (2012) Scarless fetal skin wound healing update. Birth Defects Res C Embryo Today 96(3):237–247
Denis JF, Lévesque M, Tran SD, Camarda AJ, Roy S (2013) Axolotl as a model to study scarless wound healing in vertebrates: role of the transforming growth factor beta signaling pathway. Adv Wound Care (New Rochelle). 2(5):250–260
Dollery CM, McEwan JR, Henney AM (1995) Matrix metalloproteinases and cardiovascular disease. Circ Res 77:863–868
Sternlicht MD, Werb Z (2001) How matrix metalloproteinases regulate cell behavior. Annu Rev Cell Dev Biol 17:463–516
Huang TY, Wu CH, Wang MH, Chen BS, Chiou LL, Lee HS (2015) Cooperative regulation of substrate stiffness and extracellular matrix proteins in skin wound healing of axolotls. Biomed Res Int 2015:712546
Mu X, Bellayr I, Pan H, Choi Y, Li Y (2013) Regeneration of soft tissues is promoted by MMP1 treatment after digit amputation in mice. PLoS ONE 8(3):e59105
Gurtner GC, Werner S, Barrandon Y, Longaker MT (2008) Wound repair and regeneration. Nature 453(7193):314–321
Johansson N, Ahonen M, Kähäri VM (2000) Matrix metalloproteinases in tumor invasion. Cell Mol Life Sci 57(1):5–15
Chen P, Parks WC (2009) Role of matrix metalloproteinases in epithelial migration. J Cell Biochem 108(6):1233–1243
Saarialho-Kere UK, Kovacs SO, Pentland AP, Olerud JE, Welgus HG, Parks WC (1993) Cell-matrix interactions modulate interstitial collagenase expression by human keratinocytes actively involved in wound healing. J Clin Invest 92(6):2858–2866
Iimuro Y, Nishio T, Morimoto T, Nitta T, Stefanovic B, Choi SK, Brenner DA, Yamaoka Y (2003) Delivery of matrix metalloproteinase-1 attenuates established liver fibrosis in the rat. Gastroenterology 124(2):445–458
Unemori EN, Amento EP (1990) Relax modulates synthesis and secretion of procollagenase and collagen by human dermal fibroblasts. J Bio Chem 265:10681–10685
Cho JW, Cho SY, Lee SR, Lee KS (2010) Onion extract and quercetin induce matrix metalloproteinase-1 in vitro and in vivo. Int J Mol Med 25(3):347–352
Rahmani-Neishaboor E, Yau FM, Jalili R, Kilani RT, Ghahary A (2010) Improvement of hypertrophic scarring by using topical anti-fibrogenic/anti-inflammatory factors in a rabbit ear model. Wound Repair Regen. 18(4):401–408
DiPietro LA (2013) Angiogenesis and scar formation in healing wounds. Curr Opin Rheumatol 25(1):87–91
Zhou Z, Apte SS, Soininen R, Cao R, Baaklini GY, Rauser RW, Wang J, Cao Y, Tryggvason K (2000) Impaired endochondral ossification and angiogenesis in mice deficient in membrane-type matrix metalloproteinase I. Proc Natl Acad Sci USA 97:4052–4057
Seifert AW, Monaghan JR, Voss SR, Maden M (2012) Skin regeneration in adult axolotls: a blueprint for scar-free healing in vertebrates. PLoS ONE 7(4):e32875
Schecter AD, Spirn B, Rossikhina M, Giesen PL, Bogdanov V, Fallon JT, Fisher EA, Schnapp LM, Nemerson Y, Taubman MB (2000) Release of active tissue factor by human arterial smooth muscle cells. Circ Res 87(2):126–132
Acknowledgements
This study has no financial supporters. The authors thank Professor Abdullah Tuten for proof reading.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest regarding the publication of this article.
Ethical Approval
All applicable institutional and/or national guidelines for the care and use of animals were followed. The study was approved by Acibadem University Experimental Ethics Committee (Decision date/no: 01.02.2017/32) and conducted in Acibadem University Experimental Animal Application and Research Center.
Informed Consent
Informed consent is not applicable to this type of animal study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Keskin, E.S., Keskin, E.R., Öztürk, M.B. et al. The Effect of MMP-1 on Wound Healing and Scar Formation. Aesth Plast Surg 45, 2973–2979 (2021). https://doi.org/10.1007/s00266-021-02369-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-021-02369-2