Abstract
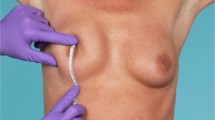
When using the inframammary access incision for breast augmentation, careful planning is critical to allow the surgeon to set the inframammary fold (IMF) at the most optimal position, minimize scar visibility, and mitigate the main disadvantage of this approach. Current popular evaluation systems for breast augmentation include the High Five and Randquist systems and they base their calculations on inconsistent variables like skin stretch measurements. We propose a simple method that is not dependent on skin stretch measurements to properly determine implant size, profile, and position of the inframammary fold. Excluding digital scans and computer-based systems that are not universally available, the proposed simplified assessment tool was compared to the two most popular manual measuring tools (High Five and Randquist). Twenty-five female volunteers were included in the study. The projected IMF positions over the midsternal line for each measuring tool were recorded on each patient and the sternal notch (SN) to projected IMF distance SN–IMF1 (simplified evaluation system), SN–IMF2 (High Five System), and SN–IMF3 (Randquist system) were compared. The anticipated new IMF position is determined based on the vertical implant dimension and not on breast base width. For most subjects, the differences between the three evaluation systems were minimal. The proposed breast measurement tool constitutes a new, much simpler, and practical method that proved to be successful in our hands.
Level of Evidence V This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.







Similar content being viewed by others
References
Shridharani S, Bellamy J, Mofid M, Singh N (2013) Breast augmentation. Eplasty 13:ic46. Available at http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3685325/ (accessed September 20, 2013)
Auclair E, Blondeel P, Del Vecchio DA (2013) Composite breast augmentation: soft-tissue planning using implants and fat. Plast Reconstr Surg 132:558–568
Adams WP Jr, Mallucci P (2012) Breast augmentation. Plast Reconstr Surg 130(4):597e–611e
Spear S, Bulan E, Venturi M (2004) Breast augmentation. Plast Reconstr Surg 114(5):73E–81E
Tebbetts JB (2002) A system for breast implant selection based on patient tissue characteristics and implant-soft tissue dynamics. Plast Reconstr Surg 109:1396–1409
Vegas M, Martin del Yerro JL (2013) Stiffness, compliance, resilience, and creep deformation: understanding implant-soft tissue dynamics in the augmented breast: fundamentals based on materials science. Aesthetic Plast Surg 37:922–930
Brown T (2013) Patient expectations after breast augmentation: the imperative to audit your sizing system. Aesthetic Plast Surg 37(6):1134–1139
Martin del Yerro JL, Vegas MR, Sanz I, Moreno E, Fernandez V, Puga S, Vecino M, Biggs T (2014) Breast augmentation with anatomic implants: a method based on the breast implantation base. Aesthetic Plast Surg 38(2):329–337
Donfrancesco A, Montemurro P, Hedén P (2013) Three-dimensional simulated images in breast augmentation surgery: an investigation of patients satisfaction and the correlation between prediction and actual outcome. Plast Reconstr Surg 132:810–822
Adams WP Jr (2008) The process of breast augmentation: four sequential steps for optimizing outcomes for patients. Plast Reconstr Surg 122:1892–1900
Tebbetts JB, Adams WP (2005) Five critical decisions in breast augmentation using five measurements in 5 minutes: the high five decision support process. Plast Reconstr Surg 116:2005–2016
Martin del Yerro JL, Vegas M, Fernandez V, Moreno E, Sanz I, Puga S, Vecino MG, Biggs TM (2013) Selecting the implant height in breast augmentation with anatomical prosthesis: the “Number Y”. Plast Reconstr Surg 131:1404–1412
Hidalgo D (2013) Discussion: prospective prospective outcome study of 225 cases of breast augmentation. Plast Reconstr Surg 131:1167–1168
Georgii J, Eder M, Burger K, Klotz S, Ferstl F, Kovacs L, Westermann R (2014) A computational tool for pre-operative breast augmentation planning in aesthetic plastic surgery. IEEE J Biomed Health Inform 18(3):907–919. Available at http://wwwcg.in.tum.de/fileadmin/user_upload/Lehrstuehle/Lehrstuhl_XV/Research/Publications/2013/BHI13/BHI13.pdf accessed 20 September 2013
Gladilin E, Gabrielova B, Montemurro P, Hedén P (2011) Customized planning of augmentation mammaplasty with silicon implants using three-dimensional optical body scans and biomechanical modeling of soft tissue outcome. Aesthetic Plast Surg 35:494–501
Swanson E (2013) Prospective outcome study of 225 cases of breast augmentation. Plast Reconstr Surg 131:1158–1166
Tepper O, Small K, Unger J, Feldman D, Kumar N, Choi M, Karp N (2009) 3D analysis of breast augmentation defines operative changes and their relationship to implant dimensions. Ann Plast Surg 62:570–575
Adams WP (2007) The high five process: tissue-based planning for breast augmentation. Plast Surg Nurs 27:197–201
Zayakova Y (2013) Planning augmentation mammaplasty of breast asymmetries. Khirurgiia (Sofiia) 2:20–25
Randquist C, Gribbe O (2010) Highly cohesive textured form stable gel implants: principles and technique. Aesthetic and reconstructive surgery of the breast. Elsevier Ltd, Edinburgh, pp 339–355
Atiyeh B, Al-Amm C, El-Musa K (2002) The transverse intra-areolar infra-nipple incision for augmentation mammoplasty. Aesthetic Plast Surg 26:151–155
Hidalgo D (2000) Breast augmentation: choosing the optimal incision, implant, and pocket plane. Plast Reconstr Surg 105:2202–2216 discussion 2217-2218
Fanous N, Tawilé C, Brousseau V (2008) Minimal inframammary incision for breast augmentation. Can J Plast Surg 16:14–17
Kovacs L, Eder M, Zimmermann A, Muller D, Schuster T, Papadopulos N, Biemer E, Kloppel M, Machens HG (2012) Three-dimensional evaluation of breast augmentation and the influence of anatomic and round implants on operative breast shape changes. Aesthetic Plast Surg 36:879–887
Brody GS (2004) The perfect breast: is it attainable? Does it exist? Plast Reconstr Surg 113:1500–1503
Hall-Findlay E (2010) The three breast dimensions: analysis and effecting change. Plast Reconstr Surg 125:1632–1642
Hammond D (2013) Discussion: three-dimensional simulated images in breast augmentation surgery: an investigation of patients’ satisfaction and the correlation between prediction and actual outcome. Plast Reconstr Surg 132:823–825
Tebbetts JB, Teitelbaum S (2010) High and extra-high-projection breast implants: potential consequences for patients. Plast Reconstr Surg 126:2150–2159
Choudry U, Kim N (2012) Preoperative assessment preferences and reported reoperation rates for size change in primary breast augmentation: a survey of ASPS members. Plast Reconstr Surg 130:1352–1359
Creasman CN, Mordaunt D, Liolios T, Chiu C, Gabriel A, Maxwell GP (2011) Four-dimensional breast imaging, part II: clinical implementation and validation of a computer imaging system for breast augmentation planning. Aesthet Surg J 31:925–938
Jacobson JM, Gatti ME, Schaffner AD, Hill LM, Spear SL (2012) Effect of incision choice on outcomes in primary breast augmentation. Aesthet Surg J 32:456–462
Losken A (2011) Commentary on: four-dimensional breast imaging, parts I and II. Aesthet Surg J 31:939–940
Adams W Jr (2012) Commentary on: effect of incision choice on outcomes in primary breast augmentation. Aesthet Surg J 32:463–464
Stutman RL, Codner M, Mahoney A, Amei A (2012) Comparison of breast augmentation incisions and common complications. Aesthetic Plast Surg 36:1096–1104
Namnoum J, Largent J, Kaplan H, Oefelein M, Brown M (2013) Primary breast augmentation clinical trial outcomes stratified by surgical incision, anatomical placement and implant device type. J Plast Reconstr Aesthet Surg 66:1165–1172
Stevens WG, Nahabedian MY, Calobrace MB, Harrington JL, Capizzi PJ, Cohen R, d’Incelli RC, Beckstrand M (2013) Risk factor analysis for capsular contracture: a five-year Sientra study analysis using round, smooth and textured implants for breast augmentation. Plast Reconstr Surg 132(5):1115–1123
Wiener TC (2008) Relationship of incision choice to capsular contracture. Aesthetic Plast Surg 32:303–306
Conflict of interest
The authors have no conflicts of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Atiyeh, B.S., Dibo, S.A., Nader, M. et al. Preoperative Assessment Tool for the Planning of Inframammary Incision and Implant Profile in Breast Augmentation. Aesth Plast Surg 38, 878–886 (2014). https://doi.org/10.1007/s00266-014-0381-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-014-0381-8