Abstract
Introduction
Unstable intertrochanteric femoral fractures in the elderly require either fixation or joint sacrificing surgery; proximal femoral nail (PFN) and bipolar hemiarthroplasties (BPH) are the most common interventions. PFN is considered to be the ideal construct for these fractures; however, the usage of hemiarthroplasties to facilitate earlier mobilization has been on a rise. Currently there is no consensus on the superiority of one of these two techniques over the other and the present review was done to determine this.
Research question
Is PFN a better alternative to BPH for unstable intertrochanteric femur fractures in the elderly?
Objective
The present systematic review and meta-analysis was conducted to determine the superiority of PFN over BPH by comparing the primary outcomes like mortality, Harris Hip scores (HHS), complications, and re-operations. Additionally, secondary outcomes like blood loss, duration of surgery, and period of hospital stays were also compared.
Methodology
Three databases of PubMed, EMBASE, and SCOPUS were searched for relevant articles that directly compared PFN and BPH in unstable intertrochanteric femur fractures in the elderly.
Results
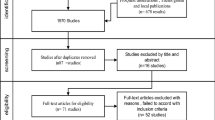
We analyzed a total of seven studies published between the years 2005 to 2017. There were four retrospective and three prospective randomized controlled studies. The number of patients in these studies ranged from 53 to 303.
Primary outcomes
There was a significant difference in HHS between two groups with standard mean difference of − 0.51 (range − 0.67 to −0.36), favouring the PFN group. The rate of mortality was higher in the BPH group with odds ratio of 2.07 (range 1.40–3.08). Implant-related complications like fractures and subsidence were more in BPH group but this was not significant.
Secondary outcomes
Mean surgical time (standard mean difference 2.19) and blood loss (3.75) were significantly less in the PFN group. The duration of hospital stay was also found to be significantly less in the PFN group (2.66).
Conclusion
Proximal femoral nails are superior to bipolar hemiarthroplasties for unstable intertrochanteric femoral fractures in the elderly. PFN imparts better functional outcomes and has lower rates of overall mortality. Additionally it is faster surgery, with lesser blood loss contributing to better results.












Similar content being viewed by others
References
Dhanwal DK, Sahoo S, Gautam VK, Saha R (2013) Hip fracture patients in India have vitamin D deficiency and secondary hyperparathyroidism. Osteoporos Int 24(2):553–557
Sankaran B (2000) Clinical studies: incidence of fracture neck of femur and intertrochanteric fractures in three Delhi hospitals. In: Sankaran B (ed) Osteoporosis. South East Asia Regional Office, World Health Organization, New Delhi, pp 9–18
Lips P (2001) Vitamin D deficiency and secondary hyperparathyroidism in the elderly: consequences for bone loss and fractures and therapeutic implications. Endocr Rev 22:477–501
Rainfray M, Dehail P, Salles N (2007) Complications of immobility and bed rest. Prevention and management. Rev Prat 57(6):671–676
Voleti PB, Liu SY, Baldwin KD, Mehta S, Donegan DJ (2015) Intertrochanteric femur fracture stability: a surrogate for general health in elderly patients? Geriatr Orthop Surg Rehabil 6(3):192–196
Koval KJ (2007) Intramedullary nailing of proximal femur fractures. Am J Orthop 36 (4 Suppl:4–7
Erturer RE, Sonmez MM, Sari S, Seckin MF, Kara A, Ozturk I (2012) Intramedullary osteosynthesis of instable intertrochanteric femur fractures with Profin nail in elderly patients. Acta Orthop Traumatol Turc 46(2):107–112
Ballal MSG, Emms N, Ramakrishnan M, Thomas G (2008) Proximal femoral nail failures in extracapsular fractures of the hip. J Orthop Surg 16(2):146–149
Gotze B, Bonnaire F, Weise K, Friedl HP (1998) Belastbahrkeit von Osteosynthesen bei instabilen per-und subtrochanteren Femurfrakturen. Aktuelle Traumatoll 28:197–204
Boldin C, Seibert FJ, Fankhauser F, Peicha G, Grechenig W, Szyszkowitz R (2003) The proximal femoral nail (PFN) – a minimal invasive treatment of unstable proximal femoral fractures: a prospective study of 55 patients with a followup of 15 months. Acta Orthop Scand 74(1):53–58
Tan BY, Lau AC, Kwek EB (2015) Morphology and fixation pitfalls of a highly unstable intertrochanteric fracture variant. J Orthop Surg (Hong Kong) 23(2):142–145
Kregor PJ, Obremskey WT, Kreder HJ, Swiontkowski MF (2014) Unstable pertrochanteric femoral fractures. J Orthop Trauma 28(Suppl 8):S25–S28
Temiz A, Durak A, Atici T (2015) Unstable intertrochanteric femur fractures in geriatric patients treated with the DLT trochanteric nail. Injury 46(Suppl 2):S 41–S 46
Park MS, Cho HM, Kim JH, Shin WJ (2013) Cementless bipolar hemiarthroplasty using a rectangular cross-section stem for unstable intertrochanteric fractures. Hip Int 23:316–322
Grimsrud C, Monzon RJ, Richman J, Ries MD (2005) Cemented hip arthroplasty with a novel cerclage cable technique for unstable intertrochanteric hip fractures. J Arthroplast 20:337–343
Singh V, Bhakta P, Zietak E, Hussain A (2016) Bone cement implantation syndrome: a delayed postoperative presentation. J Clin Anesth 31:274–277
Kim SY, Kim YG, Hwang JK (2005) Cementless calcar-replacement hemiarthroplasty compared with intramedullary fixation of unstable intertrochanteric fractures. A prospective, randomized study. J Bone Joint Surg Am 87(10):2186–2192
Desteli EE, İmren Y, Erdoğan M, Aydagün Ö (2015) Quality of life following treatment of trochanteric fractures with proximal femoral nail versus cementless bipolar hemiarthroplasty in elderly. Clin Invest Med 38(2):E63–E72
Görmeli G, Korkmaz MF, Görmeli CA, Adanaş C, Karataş T, Şimşek SA (2015) Comparison of femur intertrochanteric fracture fixation with hemiarthroplasty and proximal femoral nail systems. Ulus Travma Acil Cerrahi Derg 21(6):503–508
Özkayın N, Okçu G, Aktuğlu K (2015) Intertrochanteric femur fractures in the elderly treated with either proximal femur nailing or hemiarthroplasty: a prospective randomised clinical study. Injury 46(Suppl 2):S3–S8
Park BJ, Cho HM, Min WB (2015) A comparison of internal fixation and bipolar hemiarthroplasty for the treatment of reverse oblique intertrochanteric femoral fractures in elderly patients. Hip Pelvis 7(3):152–163
Tang P, Hu F, Shen J, Zhang L, Zhang L (2012) Proximal femoral nail antirotation versus hemiarthroplasty: a study for the treatment of intertrochanteric fractures. Injury 43(6):876–881
Esen E, Dur H, Ataoğlu MB, Ayanoğlu T, Turanlı S (2017) Evaluation of proximal femoral nail-antirotation and cemented, bipolar hemiarthroplasty with calcar replacement in treatment of intertrochanteric femoral fractures in terms of mortality and morbidity ratios. Eklem Hastalik Cerrahisi 28(1):35–40
Lindskog DM, Baumgaertner MR (2004) Unstable intertrochanteric hip fractures in the elderly. J Am Acad Orthop Surg 12:179–190
Khadgawat R, Brar KS, Gahlo M et al (2010) High prevalence of vitamin D deficiency in Asian-Indian patients with fragility hip fracture: a pilot study. J Assoc Physicians India 58:539–542
Singh M, Nagrath AR, Maini PS (1970) Changes in trabecular pattern of the upper end of the femur as an index of osteoporosis. J Bone Joint Surg Am 52(3):457–467
van Embden D, Rhemrev SJ, Meylaerts SA, Roukema GR (2010) The comparison of two classifications for trochanteric femur fractures: the AO/ASIF classification and the Jensen classification. Injury 41(4):377–381
Gallagher CA, Jones CW, Kimmel L et al (2019) Osteoarthritis is associated with increased failure of proximal femoral fracture fixation. Int Orthop 43(5):1223–1230
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kumar, P., Rajnish, R.K., Sharma, S. et al. Proximal femoral nailing is superior to hemiarthroplasty in AO/OTA A2 and A3 intertrochanteric femur fractures in the elderly: a systematic literature review and meta-analysis. International Orthopaedics (SICOT) 44, 623–633 (2020). https://doi.org/10.1007/s00264-019-04351-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-019-04351-9