Abstract
Purpose
The aim of the study was to verify the ability of nanoparticulate bioactive glass (BAG) to infiltrate into the porous titanium (Ti) layer on Ti-based implants to promote osseointegration.
Methods
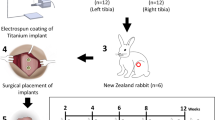
The porous titanium layer on Ti-based implants was impregnated with nanoparticulate BAG. The implants without or with BAG were implanted bilaterally in tibial holes of ten New Zealand white rabbits. The rabbits were sacrificed after ten weeks for examinations. Beside histological examination, EDXS analysis of polished cross-sections of explanted implants was also performed with the aim to quantitatively evaluate the bone-to-pore contact and bone-in-pore ratio.
Results
After ten weeks, EDXS analyses of cross-sections of the explanted implants confirmed that bioactive glass was fully resorbed and that the pores throughout the thickness of the porous titanium layer were to a large extent filled with a new bone. In the absence of bioactive glass, only the outer part of the porous layer was filled with bone. The implants without BAG in the porous Ti-layer exhibited similar bone-to-pore contact, while significant improvement of bone ingrowth into the pores was observed for the implants with BAG (38%), as opposed to those without it (22%).
Conclusion
This study confirmed that the nanoparticulate bioactive glass within the porous titanium surface layer on implants promotes osseointegration and stimulates the formation of bone within the pores.





Similar content being viewed by others
References
Ryan G, Pandit A, Apatsidis DP (2006) Fabrication methods of porous metals for use in orthopaedic applications. Biomaterials 27(13):2651–2670. doi:10.1016/j.biomaterials.2005.12.002
Daugaard H, Elmengaard B, Bechtold JE, Jensen T, Soballe K (2010) The effect on bone growth enhancement of implant coatings with hydroxyapatite and collagen deposited electrochemically and by plasma spray. J Biomed Mater Res A 92A(3):913–921. doi:10.1002/Jbm.A.32303
Kim HW, Koh YH, Li LH, Lee S, Kim HE (2004) Hydroxyapatite coating on titanium substrate with titania buffer layer processed by sol–gel method. Biomaterials 25(13):2533–2538. doi:10.1016/j.biomaterials.2003.09.041
Allan I, Newman H, Wilson M (2002) Particulate Bioglass (R) reduces the viability of bacterial biofilms formed on its surface in an in vitro model. Clin Oral Implan Res 13(1):53–58
Keshaw H, Forbes A, Day RM (2005) Release of angiogenic growth factors from cells encapsulated in alginate beads with bioactive glass. Biomaterials 26(19):4171–4179. doi:10.1016/j.biomaterials.2004.10.021
Lepparanta O, Vaahtio M, Peltola T, Zhang D, Hupa L, Hupa M, Ylanen H, Jukka IS, Matti KV, Eerola E (2008) Antibacterial effect of bioactive glasses on clinically important anaerobic bacteria in vitro. J Mater Sci-Mater M 19(2):547–551. doi:10.1007/s10856-007-3018-5
Leu A, Leach JK (2008) Proangiogenic potential of a collagen/bioactive glass substrate. Pharm Res 25(5):1222–1229. doi:10.1007/s11095-007-9508-9
Liu X, Tao S, Ding C (2002) Bioactivity of plasma sprayed dicalcium silicate coatings. Biomaterials 23(3):963–968. doi:10.1016/s0142-9612(01)00210-1
D'Alessio L, Teghil R, Zaccagnino M, Zaccardo I, Ferro D, Marotta V (1999) Pulsed laser ablation and deposition of bioactive glass as coating material for biomedical applications. Appl Surf Sci 138–139:527–532. doi:10.1016/s0169-4332(98)00610-2
Fathi MH, Doostmohammadi A (2009) Bioactive glass nanopowder and bioglass coating for biocompatibility improvement of metallic implant. J Mater Process Technol 209(3):1385–1391. doi:10.1016/j.jmatprotec.2008.03.051
Novak S, Drnovšek N, Murn G (2011) Implant having a multilayerd coating and a process for preparing thereof. PCT/SI2011/000020. PCT, Slovenia
Underwood E (1970) Quantitative stereology. Addison-Wesley, New York
Hench LL (2006) The story of Bioglass (R). J Mater Sci-Mater M 17(11):967–978. doi:10.1007/s10856-006-0432-z
Xynos ID, Edgar AJ, Buttery LDK, Hench LL, Polak JM (2000) Ionic products of bioactive glass dissolution increase proliferation of human osteoblasts and induce insulin-like growth factor II mRNA expression and protein synthesis. Biochem Bioph Res Co 276(2):461–465. doi:10.1006/bbrc.2000.3503
Hench LL (2009) Genetic design of bioactive glass. J Eur Ceram Soc 29(7):1257–1265. doi:10.1016/j.jeurceramsoc.2008.08.002
Varanasi VG, Owyoung JB, Saiz E, Marshall SJ, Marshall GW, Loomer PM (2011) The ionic products of bioactive glass particle dissolution enhance periodontal ligament fibroblast osteocalcin expression and enhance early mineralized tissue development. J Biomed Mater Res A 98A(2):177–184. doi:10.1002/Jbm.A.33102
Kokubo T (1998) Apatite formation on surfaces of ceramics, metals and polymers in body environment. Acta Mater 46(7):2519–2527
Saiz E, Lopez-Esteban S, Fujino S, Oku T, Suganuma K, Tomsia AP (2003) Characterization of metal/glass interfaces in bioactive glass coatings on Ti-6Al-4 V and Co-Cr alloys. In: Meyers MA, Ritchie RO, Sarikaya M (eds) Nano and microstructural design of advanced materials. Elsevier Science Ltd, Oxford, pp 61–67. doi:10.1016/b978-008044373-7/50034-6
Acknowledgements
The work has been performed as a part of the PhD study of Mrs. Nataša Drnovšek, and within the Meddelcoat project (FP6-IP-SME). Financial support of the Slovenian Research Agency is also acknowledged. The authors wish to thank Katja Rade and Gregor Murn for help in samples preparation and analyses and Prof. Rok Romih for his valuable suggestions on preparation for histological observation.
Conflict of interests
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Drnovšek, N., Novak, S., Dragin, U. et al. Bioactive glass enhances bone ingrowth into the porous titanium coating on orthopaedic implants. International Orthopaedics (SICOT) 36, 1739–1745 (2012). https://doi.org/10.1007/s00264-012-1520-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-012-1520-y