Abstract
Purpose
The aim of this study was to identify factors which contribute to loss of reduction (LOR).
Methods
Outpatient records and initial, post-reduction (PR) and follow-up radiographs of patients with a distal radial metaphyseal fracture were reviewed to determine demographic factors; fracture characteristics (obliquity, comminution, intact ulna); three-point cast index (3PI); and initial, PR, and follow-up displacement (angulation and translation in the sagittal and coronal planes). Univariate and multivariate regression were used to identify significant risk factors for LOR.
Results
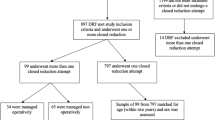
A total of 161 patients were included in our series (119 boys and 42 girls). Fifty-seven (35%) patients met the criteria for LOR. Multivariate logistic regression revealed that patients over 14 years old were 4.8 times more likely (p = 0.01) to lose reduction, and those with more than 10% PR translation in the sagittal plane were four times more likely (p = 0.03) to lose reduction. In younger patients, initial coronal translation and PR sagittal translation were independent risk factors. Patients with over 10% initial translation in the coronal plane were 2.4 times more likely (p = 0.01) to lose reduction, and those with over 10% PR translation in the sagittal plane were 2.7 times more likely (p = 0.03) to lose reduction. Three point cast index was not found to be a significant risk factor (1.64 vs. 1.57, p = 0.43).
Conclusion
Our study, the largest dedicated series of distal radial metaphyseal fractures, indicates that loss of reduction is common. Our analysis suggests that an anatomical reduction, which minimises residual translation, is the most important variable in preventing a loss of reduction.

Similar content being viewed by others
References
Galano GJ, Vitale MA, Kessler MW, Hyman JE, Vitale MG (2005) The most frequent traumatic orthopaedic injuries from a national pediatric inpatient population. J Pediatr Orthop 25:39–44
Pershad J, Williams S, Wan J, Sawyer JR (2009) Pediatric distal radial fractures treated by emergency physicians. J Emerg Med 37:341–344
Bae DS (2008) Pediatric distal radius and forearm fractures. J Hand Surg Am 33:1911–1923
Rodriguez-Merchan EC (2005) Pediatric fractures of the forearm. Clin Orthop Relat Res 432:65–72
Pretell Mazzini J, Rodriguez Martin J (2010) Paediatric forearm and distal radius fractures: Risk factors and re-displacement-role of casting indices. Int Orthop 34(3):407–412
Jones K, Weiner DS (1999) The management of forearm fractures in children: A plea for conservatism. J Pediatr Orthop 19:811–815
Do TT, Strub WM, Foad SL, Mehlman CT, Crawford AH (2003) Reduction versus remodeling in pediatric distal forearm fractures: A preliminary cost analysis. J Pediatr Orthop B 12:109–115
Alemdaroglu KB, Iltar S, Cimen O, Uysal M, Alagoz E, Atlihan D (2008) Risk factors in redisplacement of distal radial fractures in children. J Bone Joint Surg Am 90:1224–1230
Van Leemput W, De Ridder K (2009) Distal metaphyseal radius fractures in children: Reduction with or without pinning. Acta Orthop Belg 75:306–309
Proctor MT, Moore DJ, Paterson JM (1993) Redisplacement after manipulation of distal radial fractures in children. J Bone Joint Surg Br 75:453–454
Zamzam MM, Khoshhal KI (2005) Displaced fracture of the distal radius in children: Factors responsible for redisplacement after closed reduction. J Bone Joint Surg Br 87:841–843
Bae DS, Flynn JM, Frick SL, Noonan KJ (2009) The operative management of pediatric upper extremity fractures, forearm and wrist injuries. American Academy of Orthopaedic Surgeons Annual Meeting, February, Las Vegas, NV
Sharma S, Bowe D, Walters SJ, Flowers MJ (2011) Dorsal cortical comminution as a predictor of redisplacement of distal radius fractures in children. Injury 42(2):173–177
Miller BS, Taylor B, Widmann RF, Bae DS, Snyder BD, Waters PM (2005) Cast immobilization versus percutaneous pin fixation of displaced distal radius fractures in children: A prospective, randomized study. J Pediatr Orthop 25:490–494
Mani GV, Hui PW, Cheng JC (1993) Translation of the radius as a predictor of outcome in distal radial fractures of children. J Bone Joint Surg Br 75:808–811
Choi KY, Chan WS, Lam TP, Cheng JC (1995) Percutaneous kirschner-wire pinning for severely displaced distal radial fractures in children. A report of 157 cases. J Bone Joint Surg Br 77:797–801
Roy DR (1989) Completely displaced distal radius fractures with intact ulnas in children. Orthopedics 12:1089–1092
Gibbons CL, Woods DA, Pailthorpe C, Carr AJ, Worlock P (1994) The management of isolated distal radius fractures in children. J Pediatr Orthop 14:207–210
Widman R WP, Reeves S (1994) Complications of closed treatment of distal radius fractures in children. Edited by America, A. M. o. t. P. O. S. o. N., Miami, FL
Hove LM, Brudvik C (2008) Displaced paediatric fractures of the distal radius. Arch Orthop Trauma Surg 128:55–60
Bhatia M, Housden PH (2006) Re-displacement of paediatric forearm fractures: Role of plaster moulding and padding. Injury 37:259–268
Malviya A, Tsintzas D, Mahawar K, Bache CE, Glithero PR (2007) Gap index: A good predictor of failure of plaster cast in distal third radius fractures. J Pediatr Orthop B 16:48–52
Friberg KS (1979) Remodelling after distal forearm fractures in children. III. Correction of residual angulation in fractures of the radius. Acta Orthop Scand 50:741–749
Friberg KS (1979) Remodelling after distal forearm fractures in children. II. The final orientation of the distal and proximal epiphyseal plates of the radius. Acta Orthop Scand 50:731–739
Friberg KS (1979) Remodelling after distal forearm fractures in children. I. The effect of residual angulation on the spatial orientation of the epiphyseal plates. Acta Orthop Scand 50:537–546
Conflict of interest statement
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Pretell Mazzini, J., Beck, N., Brewer, J. et al. Distal metaphyseal radius fractures in children following closed reduction and casting: can loss of reduction be predicted?. International Orthopaedics (SICOT) 36, 1435–1440 (2012). https://doi.org/10.1007/s00264-012-1493-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-012-1493-x