Abstract
Background
Cervical cancer remains a leading cause of cancer-related mortality in women, particularly in developing countries. The causal association between genital human papilloma virus (HPV) infection and cervical cancer has been firmly established, and the oncogenic potential of certain HPV types has been clearly demonstrated. Vaccines targeting the oncogenic proteins, E6 and E7 of HPV-16 and -18 are the focus of current vaccine development. Previous studies have shown that calreticulin (CRT) enhances the MHC class I presentation of linked peptide/protein and may serve as an effective vaccination strategy for antigen-specific cancer treatment.
Methods
Two replication-deficient adenoviruses, one expressing HPV-16 E7 (Ad-E7) and the other expressing CRT linked to E7 (Ad-CRT/E7), were assessed for their ability to induce cellular immune response and tested for prophylactic and therapeutic effects in an E7-expressing mouse tumor model.
Results
Vaccination with Ad-CRT/E7 led to a dramatic increase in E7-specific T cell proliferation, interferon (IFN)-γ-secretion, and cytotoxic activity. Immunization of mice with Ad-CRT/E7 was effective in preventing E7-expressing tumor growth, as well as eradicating established tumors with long-term immunological memory.
Conclusion
Vaccination with an adenoviral vector expressing CRT-E7 fusion protein represents an effective strategy for immunotherapy of cervical cancer in rodents, with possible therapeutic potential in clinical settings.
Similar content being viewed by others
Introduction
Extensive epidemiologic data have strongly associated human papilloma virus (HPV) with a spectrum of anogenital neoplasms, including condylomata (genital warts), cervical dysplasia, and cervical carcinoma [1]. HPV DNA is detected in more than 99% of all tumors of the uterine cervix. Mucosotropic HPVs are grouped into low-risk or high-risk categories on the basis of each genotype’s association with a benign or malignant disease process [2, 3]. Low-risk HPV-6 and -11 are commonly detected in condyloma accuminata, but are virtually never found in cervical carcinoma. In contrast, high-risk types 16 and 18 are detected in nearly 70% of squamous cell carcinomas of the cervix [4]. The E6 and E7 genes of high-risk HPV types encode for oncoproteins that can immortalize human keratinocytes [5]. This potential appears to be limited to high-risk HPV types, because E6 and E7 from HPV-6 or -11 are non-transforming [5, 6].
E6 and E7 alter cell growth regulation by inactivating the products of tumor suppressor genes p53 and RB (retinoblastoma), respectively [7, 8]. HPV-E6 directs the ubiquitin degradation of p53, and the high-risk HPV-E7 directly binds and interferes with regulatory proteins of the RB family [9]. Similar to the adenoviral oncoprotein E1A, HPV-16 E7 binding with the RB gene product (pRB) results in release of E2F from the pRB/E2F complex. Thus, HPV-16 E7 protein has the ability to replace the E1A protein in transactivation of the adenovirus E2 promoter and other cellular genes [10]. E2F is central to the regulation of proto-oncogenes (e.g., c-myc), genes encoding proteins involved in regulating cell cycle progression (e.g., cyclin E) and DNA synthesis (e.g., DHFR, thymidine kinase, DNA polymerase α) [10]. However, previous studies have shown that E2F overexpression induces apoptosis in several cancer cell lines [11, 12]. Dysregulation of the centrosome duplication cycle has been implicated in tumorogenesis. E7 oncoprotein rapidly induces aberrant centrosome and centriole duplication in normal human cells [13].
The continued expression of these E6 and E7 proteins appears to be necessary for maintaining the malignant phenotype of cells transformed by E6 and E7. In addition, E7 is selectively retained and expressed in cervical tumors [1]. E7 is a viral protein with no appreciable homology to human cellular proteins. As such, the risk of inducing an autoimmune response by targeting E7 is theoretically eliminated. Therefore, E7 is an attractive target not only for development of cancer vaccine to prevent cervical tumors, but also a good model for exploration of immunotherapeutic approaches to stimulate immune responses against existing tumors [14, 15]. Recently, new approaches have been developed to prevent and treat cervical cancer, including the development of chimeric antigens to enhance immune responses against E7 [16–18]. For example, Zhang et al. developed an adenoviral vector expressing a fusion protein consisting of E7/CD40-ligand [19].
Calreticulin (CRT), an abundant 46 kDa Ca2+-binding protein located in the endoplasmic reticulum (ER), is considered to be related to the family of heat shock proteins (HSPs) [20]. The protein has been shown to associate with peptides delivered into the ER by transporters associated with antigen processing (TAP-1 and TAP-2) and with MHC class I-β2 microglobulin molecules to aid in antigen presentation [21–24]. Previous studies have shown that CRT can be complexed with peptides in vitro to elicit peptide-specific CD8+ T cell responses through exogenous administration [22]. In addition, peptide-bound CRT purified from tumor extracts has been shown to elicit an antitumor effect specific to the source tumor [25]. The DNA vaccine encoding CRT fused to full-length E7 (CRT/E7) is one of the most potent in generating E7-specific immune responses and antitumor effects [26]. Recent studies have shown that simultaneous vaccination of C57BL/6 mice or HLA-A2 transgenic mice with both CRT/E6 and CRT/E7 plasmids generates significant E6- and E7-specific T-cell immune responses in vaccinated mice [27].
To further improve antigen presentation through CRT fusion and the higher efficiency of antigen delivery, we sought to use an adenoviral vector expressing the CRT/E7 fusion against E7-expressing tumors. In the present study, we have constructed a replication-deficient adenovirus vector expressing the CRT/E7 fusion gene (Ad-CRT/E7) and explored its ability to induce antigen-specific immunotherapy. We showed that vaccination with Ad-CRT/E7 induces stronger E7-specific immune responses (ie., T cell proliferation, IFN-γ production, and cytotoxicity) compared to vaccination with an adenovirus vector expressing only E7 protein. The Ad-CRT/E7 vector provided 100% protection of vaccinated mice against growth of E7-expressing TC-1 tumors and generated long-term memory against these tumors. Most importantly, vaccination of tumor-bearing mice with Ad-CRT/E7 resulted in complete tumor regression in all tumor-bearing animals. The results suggest an adenovirus vaccine expressing CRT/E7 fusion is an effective vaccination approach against E7-expressing tumors and could potentially be clinically effective for the treatment of cervical cancer.
Materials and methods
Mice and cell lines
Female C57BL/6 mice aged 6–8 weeks were purchased from Jackson Laboratory (Bar Harbor, ME) and housed in the University of Louisville animal facility. Animal experiments were performed in accordance with institutional guidelines and were approved by the University of Louisville Institutional Animal Care and Use Committee. Jaws II, an immortalized C57BL/6 murine bone marrow derived dendritic cell line, was grown in MEM-α medium supplemented with 10% heat-inactivated fetal bovine serum (FBS), 100 U/ml penicillin/streptomycin, and 2 ng/ml GM-CSF (R&D Systems, Minneapolis, MN). A549 and HEK293 cells were maintained in α-MEM supplemented with 10% heat-inactivated FBS. TC-1 cells derived from primary epithelial cells of C57BL/6 mice co-transformed with HPV-16 E6 and E7, and c-Ha-ras oncogenes were maintained in RPMI 1640 supplemented with 10% heat-inactivated FBS. All of the cell lines were purchased from American Type Culture Collection (Manassas, VA).
Generation of recombinant adenovirus vectors
Three replication-deficient recombinant adenoviral vectors were used. Adenovirus expressing LacZ (Ad-LacZ) was provided by Dr B. French (University of Virginia, Charlottesville, VA) and used as a control vector that expresses nuclear-localized β-galactosidase under cytomegalovirus (CMV) promoter. Adenovirus expressing HPV-16 E7 (Ad-E7) was provided by H.C.J. Ertl (The Wistar Institute, Philadelphia, PA) [28]. For the generation of Ad-CRT/E7, CRT/E7 gene was excised from pcDNA3-CRT/E7 vector provided by Dr T.C. Wu (Johns Hopkins, Medical Institutions, Baltimore, MD) using XbaI and HindIII and subcloned into pZero 3.3 vector (Invitrogen, Carlsbad, CA). CRT/E7 was excised from pZero 3.3 using SpeI and HindIII and subcloned into pShuttle-cmv, which resulted in pS-cmvCRT/E7. Homologous recombination was carried out between pS-cmvCRT/E7 and pAdEasy-1, according to He et al. [29]. All vectors were propagated in HEK-293 cell line, purified by CsCl gradient, and titers were determined by standard plaque assays [29].
Detection of transgene expression
To determine the expression E7 and CRT/E7 proteins, A549 cells were infected at a multiplicity of infection (MOI) of 100 with Ad-E7, Ad-CRTE7, or Ad-LacZ. Forty-eight hours later, cells were lysed and subjected to SDS-PAGE (15% acrylamide for E7 and LacZ, and 8% acrylamide for CRT/E7 and LacZ) and Western blotting with mouse anti-HPV-16 E7 mAb (Santa Cruz Biotechnology, Santa Cruz, CA). Anti-mouse IgG tagged with horseradish peroxidase (Amersham) was used as secondary antibody. Detection was done using ECL Western blotting detection system (Amersham Arlington Heights, IL).
Confocal fluorescence microscopy
Jaws II cells infected at a MOI of 100 with Ad-LacZ, Ad-E7, or Ad-CRT/E7 were cultured for 48 h and then cytospun onto glass slides. Cells were fixed with 4% paraformaldehyde in phosphate buffered saline (PBS) for 30 min at room temperature, permeabilized for 30 min with PBS containing 0.05% saponin and 1% BSA, and then incubated with rabbit anti-calnexin MAb (Stressgen Biotechnologies, Victoria, British Columbia, Canada) or mouse anti-E7 (Santa Cruz Biotechnology, Santa Cruz, CA) at a concentration of 1 μg/ml for 1 h at room temperature. After several washes with PBS, cells were incubated with Cy3-conjugated F(ab′)2 fragment of goat anti-rabbit IgG or FITC-conjugated F(ab′)2 fragment goat anti-mouse IgM (Jackson ImmunoResearch Laboratories, West Grove, PA) at a concentration of 10 μg/ml for 30 min. The slides were washed with PBS containing 1% BSA. The glass slides were mounted with anti-fading medium, Mowiol 4–88 (Calbiochem Inc., La Jolla, CA), and covered with cover slips. Samples were examined on a confocal laser scanning microscope.
T cell proliferation assay
T cell proliferation assay was performed as described previously [30]. In brief, naïve mice were immunized by intraperitoneal (i.p.) injection with Ad-CRT/E7, Ad-E7, or Ad-LacZ (5 × 108 pfu/mouse). Splenocytes from these animals were harvested after 7 days, and cells (1 × 105 per well) were co-cultured with TC-1 cells (1 × 104 per well) treated previously with mitomycin C (30 μg/ml for 3 h). Cells were pulsed with [3H]-labeled thymidine (1 μCi/well) in the last 12 h of 3-day culture and harvested on a Tomtec Harvester 96 (Tomtec Inc., Hamden, CT) for quantification of incorporated thymidine. Results were expressed as mean counts per minute (cpm) of triplicate wells.
Detection of IFN-γ
Splenocytes (6 × 106 per ml) from immunized animals as mentioned above were co-cultured with mitomycin-C treated TC-1 cells (4 × 105 per well) in 24-well plates for 3 days. Culture supernatants were collected and levels of INF-γ were determined using IFN-γ ELISA kit (Biosource, Int., Camarillo, CA), according to the manufacturer’s protocol.
Cytotoxic lymphocyte assay
Splenocytes (2 × 107) from naïve mice immunized as mentioned above were co-cultured with 2 × 107 mitomycin C-treated TC-1 cells in a total volume of 5 ml of medium in 6-well plates in the presence of 10 U/ml IL-2 (Roche, Nutley, NJ). After 5 days of stimulation, viable splenocytes were recovered and used as effector cells against a fixed number of target TC-1 cells (1 × 104) at ratios of 1:50, 1:25, 1:10, 1:1, and 1:0. After 4 h incubation, supernatants were pooled and measured for the release of lactate dehydrogenase (LDH) using a non-radioactive cytotoxicity assay kit (Promega, Madison, WI), according to the manufacturer’s instructions. Specific lysis was calculated according to the formula: (%) cytotoxicity = 100 × (experimental-culture medium background)/(maximum LDH release-culture medium background).
Tumor protection assay
Four groups of ten mice were vaccinated by i.p. injection with PBS or 5 × 108 pfu/mouse of Ad-LacZ, Ad-E7, or Ad-CRT/E7. One week later, mice were subcutaneously (s.c) challenged with 1 × 105 TC-1 cells in the right leg. Tumor growth was monitored by palpation twice a week and by using calipers. Tumor size was expressed as the mean of two perpendicular diameters. Values and bars represent the mean and SD of tumor size, respectively. Animals bearing tumors were euthanized at day 28. Surviving animals were re-challenged with live tumor cells 60 days after first tumor challenge to assess the immunological memory.
Therapeutic assay
The therapeutic potential of the adenovirus vaccination was tested in two experimental settings. In the first experiment, three groups of ten mice were inoculated s.c. with 1 × 105 TC-1 cells in the right leg. Mice were injected i.p. with Ad-LacZ, Ad-E7, or Ad-CRT/E7 at a final concentration of 5 × 108 pfu in 100 μl of PBS three times starting at day 5 with 7-day intervals. In the second experiment, three groups of ten mice were inoculated s.c. with 1 × 105 TC-1 cells in the right leg. When the tumor was palpable (∼2 mm in diameter), mice were injected intratumorally with Ad-LacZ, Ad-E7, or Ad-CRT/E7 at a final concentration of 5 × 108 pfu in 100 μl of PBS followed by two more injections after 2 and 5 days. Surviving animals were re-challenged with live tumor cells 75 days after first tumor challenge.
Statistical analysis
Statistical analysis was performed using the paired Student’s t test. Values of Ad-CRT/E7 injection group were compared to the values of Ad-E7 or Ad-LacZ injection groups. P values <0.05 were considered significant.
Results
CRT/E7 fusion protein was efficiently expressed via adenoviral delivery
CRT plays a critical role in antigen processing and presentation by MHC class I molecules, and as such, has been exploited by several recent studies for the development of effective vaccines against tumors with defined tumor-associated antigens [18, 26, 31]. Previous studies have shown that CRT can enhance the presentation of E7 by antigen presenting cells, resulting in strong immune responses [18]. However, this effect is limited by the efficiency of the delivery system; as shown previously, four vaccinations of CRT/E7 DNA had the same antitumor effect as a single dose of Vac-CRT/E7 [31]. For higher efficiency that could provide complete treatment of tumors, replication-deficient recombinant adenovirus vectors are good candidates due to advantages, which include the ability to infect a broad range of cell types, high efficacy in delivery of antigens, and induction of both humoral and cellular responses [32].
A fusion gene consisting of CRT and HPV-16 E7 was subcloned under CMV promoter in replication-deficient adenoviral vector with N-terminal encapsidation signal (ES) and C-terminal poly A sequence as shown in Fig. 1 a. Expression of the fusion protein was confirmed in A549 cells infected with Ad-CRT/E7 using Western blots. CRT/E7 was detected as a band of ∼64 kDa protein, consistent with the expected sizes of 46 kDa CRT and 18 kDa E7 (Fig. 1 b). Cells infected with Ad-E7 scored positively for the 18 kDa E7 protein, whereas those infected with the adenoviral vector containing the LacZ gene (Ad-LacZ) revealed no detectable bands using antibody against E7.
Construction and characterization of adenovirus vector expressing CRT/E7. a The CRT/E7 fusion construct with cytomegalovirus (CMV) promoter, encapsidation signal (ES), poly A sequence, and the left and right inverted terminal repeat sequences (LITR or RITR, respectively). b Western blots showing the expression of E7 and Ad-CRT-E7 fusion proteins in A549 lung cancer cells infected at a multiplicity of infection of 100. Ad-LacZ construct served as negative control. E7 expression was detected using a mouse anti-HPV-16 E7. E7 was detected as 18 kDa, and CRT/E7 was detected as 64 kDa proteins
CRT/E7 was localized in the endoplasmic reticulum of dendritic cells
In as much as CRT plays a critical role in antigen processing via class I pathway, we investigated whether CRT could facilitate the transport of its fusion partner E7 into the endoplasmic reticulum (ER) of dendritic cells (DCs). Jaws II DC cell line was transduced with Ad-CRT/E7, Ad-E7, or Ad-LacZ, and transduced cells were analyzed for ER localization of E7 or CRT/E7 using confocal microscopy. For this purpose, images from immunofluorescent antibodies against E7 were compared with the distribution of calnexin, which serves as a marker for ER localization. As shown in Fig. 2, the distribution pattern of CRT/E7 was similar to that of calnexin in cells transduced with Ad-CRT/E7 (Fig. 2 a–c), suggesting that the fusion protein was transported into the ER. In contrast, E7 was localized in both ER and nuclei of Jaws II cells transduced with Ad-E7 (Fig. 2 d–f). Expression of E7 was not observed in Jaws II cells transduced with the control Ad-LacZ (Fig. 2 g–i). These data demonstrate that E7 in the fusion protein was specifically targeted to the ER for presentation in context of MHC class I molecules.
Confocal fluorescent microscopy demonstrating the expression and distribution of E7 and CRT/E7 proteins in DCs. Jaws II cells were infected at a multiplicity of infection of 100 with Ad-LacZ (g–i), Ad-E7 (d – f), or Ad-CRT/E7 (a–c), and analyzed for the detection of endogenous calnexin (red fluorescence; a, d, g), and E7 and CRT/E7 (green fluorescence; b, e, h) 48 h after infection. Co-localization of calnexin and CRT/E7 or E7 (c, f, i) was demonstrated by the yellow color formed in the combined images
Immunization with Ad-CRT/E7 induces E7-specifc T cell proliferation, IFN-γ production, and cytotoxic activity in vitro
T cell immunity is critical for an effective immune response to tumors [30, 33, 34]. To test the ability of Ad-CRT/E7 construct to generate anti-E7 T cell responses in vivo, mice were injected with Ad-CRT/E7, Ad-E7, and Ad-LacZ. Seven days later, splenocytes from immunized mice were harvested and tested against E7-expressing TC-1 tumor cells in proliferation assays. As shown in Fig. 3 a, both Ad-CRT/E7 and Ad-E7 vaccinations resulted in E7-specific T cell proliferative responses. However, there was a significant enhancement of T cell proliferation responses over that of Ad-E7 vaccine by immunization with Ad-CRT/E7. As expected, the Ad-LacZ-immunized group showed no significant effects on the levels of proliferation as well as TC-1 cells without splenocytes.
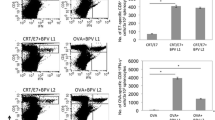
Immunization with Ad-CRT/E7 induces E7-specific cellular immune responses. Three groups of mice (n = 5) were immunized i.p. with Ad-LacZ, Ad-E7, or Ad-CRT/E7 (5 × 108 pfu/mouse). One week after immunization, spleen cells were collected and used for analyses. a T cell proliferation assay. Splenocytes (1 × 105 per well) were stimulated in vitro with mitomycin C-treated TC-1 cells (1 × 104 per well) for 3 days, pulsed with [3H]-labeled thymidine, and proliferation was determined as counts per minute (cpm). b IFN-γ production. Splenocytes (6 × 106 per ml) from immunized mice were stimulated with mitomycin-C treated TC-1 cells (4 × 105 per well) for 3 days, and supernatants were analyzed for IFN-γ production using ELISA. c Cytotoxic lymphocyte assay. Splenocytes (2 × 107 per ml) were stimulated in vitro with mitomycin C-treated TC-1 cells (2 × 107 per ml) in the presence of IL-2 (10 U/ml) for 5 days. Viable cells were recovered and used as effectors against fixed number of target TC-1 cells (1 × 104) at the indicated ratios for 4 h. Supernatants were pooled and measured for the release of lactate dehydrogenase (LDH). The experiments were repeated two more times. *P < 0.05 compared with Ad-E7 in paired Student’s t test
IFN-γ is used as a signature cytokine for Th1 responses as well as effector function of CD8+ T cells that are critical to tumor eradication [29]. Splenocytes from immunized mice generated significant levels of IFN-γ when stimulated in vitro by TC-1 cells (Fig. 3 b ). The INF-γ response upon immunization with Ad-CRT/E7 was superior to immunization with Ad-E7 immunization and specific for E7, since immunization with Ad-LacZ did not generate a measurable IFN-γ response against TC-1 cells.
To test whether the production of IFN-γ is associated with the generation of effective E7-specific cytolytic responses, splenocytes from Ad-CRT/E7, Ad-E7, and Ad-LacZ immunized mice were stimulated ex vivo with TC-1 cells in the presence of IL-2 for 5 days to expand effector cells. As shown in Fig. 3 c, vaccination with Ad-CRT/E7 induced significant levels of cytotoxic response against TC-1 cells as compared with Ad-E7. The cytolytic response was E7-specific, since splenocytes from mice immunized with Ad-LacZ did not have measurable cytolytic activity against TC-1 cells. Taken together, these data demonstrate that immunization with E7 linked to CRT is an effective approach to generate potent immune responses.
Vaccination with Ad-CRT/E7 protected mice against E7 expressing tumor challenge
Based on the effect of Ad-CRT/E7 on T cell responses, we next tested whether pre-vaccination with Ad-CRT/E7 could protect mice against tumor formation. For this purpose, four groups of ten mice were challenged with live TC-1 cells 1 week after immunization with PBS, Ad-LacZ, Ad-E7, or Ad-CRT/E7. Rapid tumor growth was observed in mice immunized with Ad-LacZ similar to the PBS control group. While immunization with Ad-CRT/E7 resulted in complete protection against tumor growth, immunization with Ad-E7 only resulted in 20% tumor-free survival. The tumor protection effect had long-term immunological memory, since re-challenge of tumor-free mice with a lethal dose of live tumor cells 60 days after the first inoculation resulted in tumor-free survival (Fig. 4).
Prevaccination with Ad-CRT/E7 protected mice against tumor growth. Four groups of ten naïve mice were vaccinated i.p. with PBS (open square), Ad-LacZ (filled square), Ad-E7 (open circle), and Ad-CRT/E7 (filled circle) at a concentration of 5 × 108 pfu/mouse. One week later, mice were challenged s.c. with live TC-1 cells (1 × 105) in the right leg. Tumor growth was monitored three times a week for over a period of 60 days. Surviving animals in both groups were re-challenged with TC-1 cells and monitored for an additional period of 60 days (arrow)
Vaccination with Ad-CRT/E7 induces a therapeutic effect against established tumors
In the majority of patients in Third World countries without screening programs, cervical cancer development is generally detected at an advanced stage [35]. Therefore, an efficient therapeutic approach is needed to treat cervical cancer. Hence, we asked whether Ad-CRT/E7 could be used for immunotherapy against established tumors in two different settings. In the first setting, a group of mice was injected i.p. with the adenoviral constructs three times at 7-day intervals, starting at day 5 after tumor challenge. All animals vaccinated with Ad-CRT/E7 had tumor-free survival for more than 60 days (Fig. 5 a, b), and no tumor growth was observed in these animals upon second challenge with live tumor cells. However, normal tumor growth was observed in mice treated with Ad-E7, similar to the mice treated with Ad-LacZ.
Systemic vaccination with Ad-CRT/E7 after tumor challenge resulted in regression of early-stage tumors. For the treatment of early stage of tumors, three groups of ten mice were inoculated s.c. with 1x105 live TC-1 cells in the right leg. Five days later, mice were vaccinated i.p with Ad-LacZ (filled square), Ad-E7 (open circle), and Ad-CRT/E7 (filled circle) at a concentration of 5 × 108 pfu/mouse three times at 7-day intervals (vertical arrows). Tumor growth was monitored three times a week, and tumor size was expressed as the mean of two perpendicular diameters. a Tumor growth is shown starting from first vaccination. b Survival was monitored for over a period of 60 days. Surviving animals were re-challenged with live tumor cells at day 75 and monitored (horizontal arrow)
In the second setting, the efficacy of the Ad-CRT/E7 to eliminate established TC-1 tumors was tested. Ad-CRT/E7, Ad-E7, and Ad-LacZ constructs were administered three times at 2-day intervals by intratumoral injection after the tumors were palpable. Tumor regression was observed in all mice after the third vaccination with Ad-CRT/E7, and tumor growth was not observed for over a period of 60 days and after the second challenge with live tumor cells at day 70 (Fig. 6 a–b). In contrast, vaccination with Ad-E7 or Ad-LacZ had no effect on tumor growth. Therefore, the efficacy of intratumoral injection of Ad-CRT/E7 was demonstrated. The results from these two vaccination settings demonstrate that Ad-CRT/E7 can be used as a potent therapeutic vaccine against both early and late-stage E7-expressing tumors.
Intratumoral vaccination with Ad-CRT/E7 resulted in regression of late-stage tumors. For the treatment of late stage of tumor, three groups of ten mice were inoculated s.c. with TC-1 cells in the right leg. When the tumors were palpable, Ad-LacZ (filled square), Ad-E7 (open circle), or Ad-CRT/E7 (filled circle) at a concentration of 5 × 108 pfu/mouse were injected three times at 2-day intervals (vertical arrows) inside the tumors. Tumor growth size was monitored, and tumor size was expressed as the means of two perpendicular diameters. a Tumor growth is shown starting from the first vaccination. b Survival was monitored for over a period of 60 days. Surviving animals were re-challenged with live tumor cells at day 75 and monitored (horizontal arrow)
Discussion
Two divergent immunologic approaches have evolved for the development of anti-HPV responses; prophylactic and therapeutic vaccines. In general, immunoprophylactic vaccines elicit humoral immune responses characterized by neutralizing antibodies against the virus. For example, vaccination with L1 and L2 virus-like particles (VLP) can induce antibodies that neutralize HPV and protect against experimental HPV infection [36–38]. Recently, an HPV-16 vaccine was approved by the FDA [39], which is based on HPV-16 L1 VLP. This vaccine is shown to be highly efficient to prevent carcinoma in situ development in women aged 16–23 years; it prevents HPV-16 infection, but does not treat patients with existing HPV infection or with cervical carcinoma. Most sexually active women may already be exposed to HPV [1], so it is unlikely that humoral immunity induced from VLP-based HPV vaccines would be effective in treating these women. Therefore, development of vaccines that induce the cellular arm of the immune system against cells expressing the tumor-associated/specific antigens will be an important therapeutic advance for individuals with HPV-induced tumors [1].
As the HPV-16 E7 antigen proved to be highly immunogenic and is expressed frequently in cervical cancer, several therapeutic and prophylactic vaccines based on the E7 as the common antigenic component have been developed in animal disease models. These approaches include vaccination with purified E7 protein [40], modified non-transformant HPV E6/E7 fusion proteins [16], DNA vectors encoding the translocation domain of a bacterial toxin conjugated with E7 [41], various viral vectors carrying E7 [42], dendritic cell-pulsed E7 [43], adenoviral vectors expressing E7 and IL-12 [33], or recombinant E7 with CpG oligonucleotides [30]. These vaccination approaches generally were successful in inducing CD8+ T cell responses against cancer cells with prophylactic as well as therapeutic efficacies. We herein demonstrated the effects of E7 fused to CRT, delivered by replication-deficient adenoviral vector against E7-expressing tumor cell line TC-1. Fusion of CRT to E7 plays two main roles in this approach: facilitation of antigen presentation and isolation of E7 from interference to cell cycle control.
Previous studies have shown that CRT is an abundant binding protein that is localized in the ER [20]. Therefore, CRT can directly transport E7 antigen to the ER and facilitate antigen presentation in association with MHC molecules. We tested this hypothesis via confocal fluorescence microscopy using a DC cell line transduced with Ad-CRT/E7 or Ad-E7. E7 protein was distributed in both ER and the nucleus in the cells transduced with Ad-E7, whereas fusion with CRT localized the E7 protein only in the ER. Transportation of wild-type E7 by CRT could “sequester” E7 in the ER. This effect could potentially diminish the possibility of inhibition of the tumor suppressor pRB by E7, although we have not yet tested that hypothesis. Interaction of E7 and regulatory proteins in pRB family could result in loss of control of cell growth, particularly through release of EF2-1 [9]. Therefore, using CRT/E7 fusion has a potential advantage over previously published approaches using the wild-type E7 as an immunogen by not interfering with the cell cycle control and eliminating the risk of vaccine-induced tumorigenesis.
The fusion of CRT/E7 has been tested in different studies with a search for an effective vector as a model vaccine against cervical cancer. For instance, Cheng et al. explored the effect of intradermal administration of a CRT/E7 DNA vaccine, which exhibited a dramatic increase in E7-specific CD8+ T cell precursors and a potent antitumor effect against E7-expressing tumors compared to E7 DNA or CRT DNA alone [18]. Recently, Hsieh et al. tested the CRT/E7 fusion gene against E7-expressing TC-1 tumors [31]. Vaccinia virus and DNA vaccine were compared and both vectors protected mice against tumor growth. Upon vaccination with vaccinia virus or DNA vector starting 5 days after tumor challenge, tumor growth was shown to slow down and tumors remained small [31]. Although vaccinia virus was very effective, many studies have shown that adenovirus vectors are more efficient as compared with other delivery systems in induction of anti-tumor immune responses against tumor-associated antigens [44]. Therefore, in the present study, we have tested the effect of CRT/E7 fusion delivered by a replication-deficient adenovirus vector. This vector protected the mice against tumor growth similar to previously published vaccinia virus and DNA vectors [31]. Most importantly, we herein demonstrated that the adenoviral vector was effective against both early-stage tumors and palpable/established tumors. Upon vaccination in both stages of tumor progression, the TC-1 tumors were completely treated. In addition, re-challenge with live tumor cells showed that these mice generated long-term immunological memory against E7-expressing TC-1 cells.
Therefore, the adenoviral vector expressing CRT/E7 fusion used in this study has potential clinical utility for the treatment of advanced cervical cancer and may have advantages over the other vector systems.
Previous studies have shown that immunologic barriers and dose/route of administration are factors that could prevent the effect of adenovirus vectors [45]. Antibodies against adenovirus are generated as soon as 2 days after immunization, and antibody titers depend on the dose of virus [46]. In addition, transgene expression could decline 7 days after immunization [47]. Intraperitoneal injection can have a rapid effect on antigen delivery to the lymph nodes. Although it is not tested, it may also induce immune responses against the adenovirus vector, particularly in the form of antibodies [48, 49]. On the other hand, several studies have shown that intratumoral injection of adenovirus induces a significant tumor regression [50, 51]. Intratumoral injection of the vectors could provide an important safety advantage over i.p or i.v. injection, because the vector could infect predominantly the cells in the tumor instead of other vital cells, such as liver cells, and could greatly reduce virus dissemination [52, 53]. While they were tested at different stages, the success in both vaccination protocols presented in this study revealed that adenovirus expressing CRT/E7 has the potential for treatment of both early and advanced stages of cervical cancer.
It must be recognized that the clinical utility of Ad-CRT/E7 in humans could be limited by the presence of preexisting neutralizing antibodies against adenovirus as a result of natural infection with this virus [54, 55], although little is known about the level or impact of neutralizing antibodies following subcutaneous or intramuscular injection. Neutralizing antibodies can diminish, but not necessarily eliminate gene transfer from adenoviral vectors [56–59]. Several studies have shown that the presence of neutralizing antibodies specific for the virus did not affect the usefulness of repeated applications of adenovirus-transduced DCs and boosted the CTL response even in mice previously infected with the recombinant vector [32, 60, 61]. Thus, the use of DCs transduced with recombinant adenovirus could circumvent the presence of neutralizing antibodies providing advantages over other forms of immunization.
In conclusion, our current data demonstrated that adenoviral vectors expressing the fusion of CRT and E7 can effectively be used as a prophylactic and therapeutic vaccine against E7-expressing tumors. The efficacy of this vaccine approach in clinical trials remains to be established, and if effective against cervical cancer, the same approach could be used to link CRT to non-viral tumor-associated antigens as a general approach for various cancer types as well as infectious agents.
References
Steller MA (2000) Cervical cancer vaccines: progress and prospects. J Soc Gynecol Investig 9:254–264
Walboomers JM, Jacobs MV, Manos MM, Bosch FX, Kummer JA, Shah KV, Snijders PJ, Peto J, Meijer CJ, Munoz N (1999) Human papillomavirus is a necessary cause of invasive cervical cancer worldwide. J Pathol 189:12–19
de Villiers EM (1989) Heterogeneity of the human papillomavirus group. J Virol 63:4898–4903
Bosch FX, Manos MM, Munoz N, Sherman M, Jansen AM, Peto J, Schiffman MH, Moreno V, Kurman R, Shah KV (1995) Prevalence of human papillomavirus in cervical cancer: a worldwide perspective. International biological study on cervical cancer (IBSCC) study group. J Natl Cancer Inst 87:796–802
Pecoraro G, Morgan D, Defendi V (1989) Differential effects of human papillomavirus type 6, 16, and 18 DNAs on immortalization and transformation of human cervical epithelial cells. Proc Natl Acad Sci USA 86:563–567
Barbosa MS, Vass WC, Lowy DR, Schiller JT (1991) In vitro biological activities of the E6 and E7 genes vary among human papillomaviruses of different oncogenic potential. J Virol 65:292–298
Munger K, Scheffner M, Huibregtse JM, Howley PM (1992) Interactions of HPV E6 and E7 oncoproteins with tumour suppressor gene products. Cancer Surv 12:197–217
Dyson N, Howley PM, Munger K, Harlow E (1989) The human papilloma virus-16 E7 oncoprotein is able to bind to the retinoblastoma gene product. Science 243:934–937
Thomas M, Banks L (1999) Human papillomavirus (HPV) E6 interactions with Bak are conserved amongst E6 proteins from high and low risk HPV types. J Gen Virol 80(Pt 6):1513–1517
Armstrong DJ, Roman A (1997) The relative ability of human papillomavirus type 6 and human papillomavirus type 16 E7 proteins to transactivate E2F-responsive elements is promoter- and cell-dependent. Virology 239:238–246
Dong YB, Yang HL, Elliott MJ, Liu TJ, Stilwell A, Atienza C Jr, McMasters KM (1999) Adenovirus-mediated E2F-1 gene transfer efficiently induces apoptosis in melanoma cells. Cancer 86:2021–2033
Elliott MJ, Dong YB, Yang H, McMasters KM (2001) E2F-1 up-regulates c-Myc and p14(ARF) and induces apoptosis in colon cancer cells. Clin Cancer Res 7:3590–3597
Duensing S, Duensing A, Lee DC, Edwards KM, Piboonniyom SO, Manuel E, Skaltsounis L, Meijer L, Munger K (2004) Cyclin-dependent kinase inhibitor indirubin-3′-oxime selectively inhibits human papillomavirus type 16 E7-induced numerical centrosome anomalies. Oncogene 23:8206–8215
Jansen KU, Shaw AR (2004) Human papillomavirus vaccines and prevention of cervical cancer. Annu Rev Med 55:319–331
Furumoto H, Irahara M (2002) Human papilloma virus (HPV) and cervical cancer. J Med Invest 49:124–133
Zhou X, Qian X, Zhao Q, Lu Y, Xiong M (2004) Efficient expression of modified human papillomavirus 16 e6/e7 fusion protein and the antitumor efficacy in a mouse model. Biol Pharm Bull 27:303–307
Li J, Sun Y, Garen A (2002) Immunization and immunotherapy for cancers involving infection by a human papillomavirus in a mouse model. Proc Natl Acad Sci USA 99:16232–16236
Cheng WF, Hung CF, Chai CY, Hsu KF, He L, Ling M, Wu TC (2001) Tumor-specific immunity and antiangiogenesis generated by a DNA vaccine encoding calreticulin linked to a tumor antigen. J Clin Invest 108:669–678
Zhang L, Tang Y, Akbulut H, Zelterman D, Linton P-J, Deisseroth AB (2003) An adenoviral vector cancer vaccine that delivers a tumor-associated antigen/CD40-ligand fusion protein to dendritic cells. Proc Natl Acad Sci USA 100(25):15101–15106
Nash PD, Opas M, Michalak M (1994) Calreticulin: not just another calcium-binding protein. Mol Cell Biochem 135:71–78
Conway EM, Liu L, Nowakowski B, Steiner-Mosonyi M, Ribeiro SP, Michalak M (1995) Heat shock-sensitive expression of calreticulin. In vitro and in vivo up-regulation. J Biol Chem 270:17011–17016
Basu S, Srivastava PK (1999) Calreticulin, a peptide-binding chaperone of the endoplasmic reticulum, elicits tumor- and peptide-specific immunity. J Exp Med 189:797–802
Spee P, Neefjes J (1997) TAP-translocated peptides specifically bind proteins in the endoplasmic reticulum, including gp96, protein disulfide isomerase and calreticulin. Eur J Immunol 27:2441–2449
Sadasivan B, Lehner PJ, Ortmann B, Spies T, Cresswell P (1996) Roles for calreticulin and a novel glycoprotein, tapasin, in the interaction of MHC class I molecules with TAP. Immunity 5:103–114
Pike SE, Yao L, Setsuda J, Jones KD, Cherney B, Appella E, Sakaguchi K, Nakhasi H, Atreya CD, Teruya-Feldstein J, Wirth P, Gupta G, Tosato G (1999) Calreticulin and calreticulin fragments are endothelial cell inhibitors that suppress tumor growth. Blood 94:2461–2468
Kim JW, Hung CF, Juang J, He L, Kim TW, Armstrong DK, Pai SI, Chen PG, Lin CT, Boyd DA, Wu TC (2004) Comparison of HPV DNA vaccines employing intracellular targeting strategies. Gene Ther 11:1011–1018
Peng S, Tomson TT, Trimble C, He L, Hung CF, Wu TC (2006). A combination of DNA vaccines targeting human papillomavirus type 16 E6 and E7 generates potent antitumor effects. Gene Ther 13:257–265
He Z, Wlazlo AP, Kowalczyk DW, Cheng J, Xiang ZQ, Giles-Davis W, Ertl HC (2000) Viral recombinant vaccines to the E6 and E7 antigens of HPV-16. Virology 270:146–161
He TC, Zhou S, da Costa LT, Yu J, Kinzler KW, Vogelstein B (1998) A simplified system for generating recombinant adenoviruses. Proc Natl Acad Sci USA 95:2509–2514
Kim TY, Myoung HJ, Kim JH, Moon IS, Kim TG, Ahn WS, Sin JI (2002) Both E7 and CpG-oligodeoxynucleotide are required for protective immunity against challenge with human papillomavirus 16 (E6/E7) immortalized tumor cells: involvement of CD4+ and CD8+ T cells in protection. Cancer Res 62:7234–7240
Hsieh CJ, Kim TW, Hung CF, Juang J, Moniz M, Boyd DA, He L, Chen PJ, Chen CH, Wu TC (2004) Enhancement of vaccinia vaccine potency by linkage of tumor antigen gene to gene encoding calreticulin. Vaccine 22:3993–4001
Brossart P, Goldrath AW, Butz EA, Martin S, Bevan MJ (1997) Virus-mediated delivery of antigenic epitopes into dendritic cells as a means to induce CTL. J Immunol 158:3270–3276
Jin HS, Park EK, Lee JM, NamKoong SI, Kim DG, Lee YJ, Jun HJ, Han BD, Bae SM, Ahn WS (2005) Immunization with adenoviral vectors carrying recombinant IL-12 and E7 enhanced the antitumor immunity to human papillomavirus 16-associated tumor. Gynecol Oncol 97:559–567
Liu DW, Tsao YP, Hsieh CH, Hsieh JT, Kung JT, Chiang CL, Huang SJ, Chen SL (2000a) Induction of CD8 T cells by vaccination with recombinant adenovirus expressing human papillomavirus type 16 E5 gene reduces tumor growth. J Virol 74:9083–9089
Sankaranarayanan R, Rajkumar R, Theresa R, Esmy PO, Mahe C, Bagyalakshmi KR, Thara S, Frappart L, Lucas E, Muwonge R, Shanthakumari S, Jeevan D, Subbarao TM, Parkin DM, Cherian J (2004) Initial results from a randomized trial of cervical visual screening in rural south India. Int J Cancer 109:461–467
Kirnbauer R, Booy F, Cheng N, Lowy DR, Schiller JT (1992) Papillomavirus L1 major capsid protein self-assembles into virus-like particles that are highly immunogenic. Proc Natl Acad Sci USA 89:12180–12184
Kirnbauer R, Taub J, Greenstone H, Roden R, Durst M, Gissmann L, Lowy DR, Schiller JT (1993) Efficient self-assembly of human papillomavirus type 16 L1 and L1–L2 into virus-like particles. J Virol 67:6929–6936
Suzich JA, Ghim SJ, Palmer-Hill FJ, White WI, Tamura JK, Bell JA, Newsome JA, Jenson AB, Schlegel R (1995) Systemic immunization with papillomavirus L1 protein completely prevents the development of viral mucosal papillomas. Proc Natl Acad Sci USA 92:11553–11557
Mao C, Koutsky LA, Ault KA, Wheeler CM, Brown DR, Wiley DJ, Alvarez FB, Bautista OM, Jansen KU, Barr E (2006) Efficacy of human papillomavirus-16 vaccine to prevent cervical intraepithelial neoplasia: a randomized controlled trial. Obstet Gynecol 107(1):18–27
Fernando GJ, Murray B, Zhou J, Frazer IH (1999) Expression, purification and immunological characterization of the transforming protein E7, from cervical cancer-associated human papillomavirus type 16. Clin Exp Immunol 115:397–403
Hung CF, Cheng WF, Hsu KF, Chai CY, He L, Ling M, Wu TC (2001) Cancer immunotherapy using a DNA vaccine encoding the translocation domain of a bacterial toxin linked to a tumor antigen. Cancer Res 61:3698–3703
Liu DW, Tsao YP, Kung JT, Ding YA, Sytwu HK, Xiao X, Chen SL (2000b) Recombinant adeno-associated virus expressing human papillomavirus type 16 E7 peptide DNA fused with heat shock protein DNA as a potential vaccine for cervical cancer. J Virol 74:2888–2894
Tillman BW, Hayes TL, DeGruijl TD, Douglas JT, Curiel DT (2000) Adenoviral vectors targeted to CD40 enhance the efficacy of dendritic cell-based vaccination against human papillomavirus 16-induced tumor cells in a murine model. Cancer Res 60:5456–5463
Basak S, Eck S, Gutzmer R, Smith AJ, Birebent B, Purev E, Staib L, Somasundaram R, Zaloudik J, Li W, Jacob L, Mitchell E, Speicher D, Herlyn D (2000) Colorectal cancer vaccines: antiidiotypic antibody, recombinant protein, and viral vector. Ann NY Acad Sci 910:237–253
Bessis N, Garcia-Cozar FJ, Boissier MC (2004) Immune responses to gene therapy vectors: influence on vector function and effector mechanisms. Gene Ther 11(Suppl 1):S10–17
Kajiwara K, Byrnes AP, Ohmoto Y, Charlton HM, Wood MJ, Wood KJ (2000) Humoral immune responses to adenovirus vectors in the brain. J Neuroimmunol 103:8–15
Kuzmin AI, Galenko O, Eisensmith RC (2001) An immunomodulatory procedure that stabilizes transgene expression and permits readministration of E1-deleted adenovirus vectors. Mol Ther 3:293–301
Gahery-Segard H, Juillard V, Gaston J, Lengagne R, Pavirani A, Boulanger P, Guillet JG (1997) Humoral immune response to the capsid components of recombinant adenoviruses: routes of immunization modulate virus-induced Ig subclass shifts. Eur J Immunol 27:653–659
Lasarte JJ, Corrales FJ, Casares N, Lopez-Diaz de Cerio A, Qian C, Xie X, Borras-Cuesta F, Prieto J (1999) Different doses of adenoviral vector expressing IL-12 enhance or depress the immune response to a coadministered antigen: the role of nitric oxide. J Immunol 162:5270–5277
Sangro B, Mazzolini G, Ruiz J, Herraiz M, Quiroga J, Herrero I, Benito A, Larrache J, Pueyo J, Subtil JC, Olague C, Sola J, Sadaba B, Lacasa C, Melero I, Qian C, Prieto J (2004) Phase I trial of intratumoral injection of an adenovirus encoding interleukin-12 for advanced digestive tumors. J Clin Oncol 22:1389–1397
Cordier Kellerman L, Valeyrie L, Fernandez N, Opolon P, Sabourin JC, Maubec E, LeRoy P, Kane A, Legrand A, Abina MA, Descamps V, Haddada H (2003) Regression of AK7 malignant mesothelioma established in immunocompetent mice following intratumoral gene transfer of interferon gamma. Cancer Gene Ther 10:481–490
Hu Z, Garen A (2000) Intratumoral injection of adenoviral vectors encoding tumor-targeted immunoconjugates for cancer immunotherapy. Proc Natl Acad Sci USA 97:9221–9225
Bramson JL, Hitt M, Gauldie J, Graham FL (1997) Pre-existing immunity to adenovirus does not prevent tumor regression following intratumoral administration of a vector expressing IL-12 but inhibits virus dissemination. Gene Ther 4:1069–1076
Rosenberg SA, Zhai Y, Yang JC, Schwartzentruber DJ, Hwu P, Marincola FM, Topalian SL, Restifo NP, Seipp CA, Einhorn JH, Roberts B, White DE (1998) Immunizing patients with metastatic melanoma using recombinant adenoviruses encoding MART-1 or gp100 melanoma antigens. J Natl Cancer Inst 90:1894–1900
Zhi Y, Figueredo J, Kobinger GP, Hagan H, Calcedo R, Miller JR, Gao G, Wilson JM (2006) Efficacy of severe acute respiratory syndrome vaccine based on a nonhuman primate adenovirus in the presence of immunity against human adenovirus. Hum Gene Ther 17:500–506
Mack CA, Song WR, Carpenter H, Wickham TJ, Kovesdi I, Harvey BG, Magovern CJ, Isom OW, Rosengart T, Falck-Pedersen E, Hackett NR, Crystal RG, Mastrangeli A (1997) Circumvention of anti-adenovirus neutralizing immunity by administration of an adenoviral vector of an alternate serotype. Hum Gene Ther 8:99–109
Ueno H, Li JJ, Tomita H, Yamamoto H, Pan Y, Kanegae Y, Saito I, Takeshita A (1995) Quantitative analysis of repeat adenovirus-mediated gene transfer into injured canine femoral arteries. Arterioscler Thromb Vasc Biol 15:2246–2253
Scaria A, St George JA, Gregory RJ, Noelle RJ, Wadsworth SC, Smith AE, Kaplan JM (1997) Antibody to CD40 ligand inhibits both humoral and cellular immune responses to adenoviral vectors and facilitates repeated administration to mouse airway. Gene Ther 4:611–617
Seiler P, Brundler MA, Zimmermann C, Weibel D, Bruns M, Hengartner H, Zinkernagel RM (1998) Induction of protective cytotoxic T cell responses in the presence of high titers of virus-neutralizing antibodies: implications for passive and active immunization. J Exp Med 187:649–654
Butterfield LH, Jilani SM, Chakraborty NG, Bui LA, Ribas A, Dissette VB, Lau R, Gamradt SC, Glaspy JA, McBride WH, Mukherji B, Economou JS (1998) Generation of melanoma-specific cytotoxic T lymphocytes by dendritic cells transduced with a MART-1 adenovirus. J Immunol 161:5607–5613
Kaplan JM, Yu Q, Piraino ST, Pennington SE, Shankara S, Woodworth LA, Roberts BL (1999) Induction of antitumor immunity with dendritic cells transduced with adenovirus vector-encoding endogenous tumor-associated antigens. J Immunol 163:699–707
Acknowledgments
Grant support. This work was supported by NIH Grant R01CA90784-01A1 and Kentucky Lung Cancer Research Program to K.M.M., CONACYT México to R.M.L., and Kentucky Lung Cancer Research Program to H.S. We thank Dr. T-C. Wu for providing pcDNA-CRT/E7 plasmid, Dr. H. C. J. Ertl for providing Ad-E7 vector, and Dr. B. French for providing Ad-LacZ vector.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gomez-Gutierrez, J.G., Elpek, K.G., Montes de Oca-Luna, R. et al. Vaccination with an adenoviral vector expressing calreticulin-human papillomavirus 16 E7 fusion protein eradicates E7 expressing established tumors in mice. Cancer Immunol Immunother 56, 997–1007 (2007). https://doi.org/10.1007/s00262-006-0247-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00262-006-0247-2