Abstract
Purpose
To evaluate the correlation between HeF obtained from gadoxetic acid-enhanced MR imaging and clinical biomarkers for the assessment of liver function.
Methods
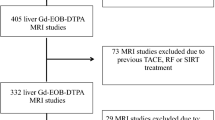
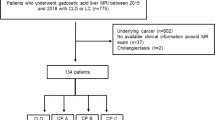
This prospective study was approved by our Institutional Review Board, and written informed consent was obtained from the patients. We recruited 48 patients carrying a known or suspected liver disease to undergo gadoxetic acid-enhanced MR imaging. The new model of the HeF was calculated from ΔR1 values of the liver and spleen. The HeF, quantitative liver-to-spleen contrast ratio (Q-LSC), and ΔT1 value (the reduction rate of the T1 value between the pre- and post-contrast images) were compared with the Child–Pugh and end-stage liver disease (MELD) scores.
Results
Among 48 patients, 40 were in Child–Pugh class A and 8 were in class B. The median HeF (P = 0.0001), Q-LSC (P = 0.015), and ΔT1 value (P = 0.0023) in patients in Child–Pugh class A were significantly higher than those in class B. The sensitivities, specificities, and area under the receiver-operating-characteristic curves for differentiating Child–Pugh class A and B were 95.0%, 87.5%, and 0.93 in the HeF; 77.5%, 75.0%, and 0.78 in the Q-LSC; and 57.5%, 100.0%, and 0.84 in the ΔT1 value, respectively. The HeF was significantly correlated with Child–Pugh (r = − 0.58, P < 0.0001) and MELD score (r = − 0.57, P < 0.0001).
Conclusions
The HeF was well correlated with Child–Pugh and MELD score and could be a new biomarker to assess liver function.






Similar content being viewed by others
References
Haimerl M, Verloh N, Zeman F, et al. Assessment of clinical signs of liver cirrhosis using T1 mapping on Gd-EOB-DTPA-enhanced 3T MRI. Plos One 2013; 8:e85658
Yamada A, Hara T, Li F, et al. Quantitative evaluation of liver function with use of gadoxetate disodium-enhanced MR imaging. Radiology 2011; 260:727-733
de Carli MA, de Carli LA, Correa MB, Junqueira G, Jr., Tovo CV, Coral GP. Performance of noninvasive scores for the diagnosis of advanced liver fibrosis in morbidly obese with nonalcoholic fatty liver disease. Eur J Gastroenterol Hepatol 2019;
Ringe KI, Husarik DB, Sirlin CB, Merkle EM. Gadoxetate disodium-enhanced MRI of the liver: part 1, protocol optimization and lesion appearance in the noncirrhotic liver. AJR American journal of roentgenology 2010; 195:13-28
Motosugi U, Ichikawa T, Sou H, et al. Liver parenchymal enhancement of hepatocyte-phase images in Gd-EOB-DTPA-enhanced MR imaging: which biological markers of the liver function affect the enhancement? J Magn Reson Imaging 2009; 30:1042-1046
Noda Y, Goshima S, Kajita K, et al. Biliary tract enhancement in gadoxetic acid-enhanced MRI correlates with liver function biomarkers. Eur J Radiol 2016; 85:2001-2007
Katsube T, Okada M, Kumano S, et al. Estimation of liver function using T1 mapping on Gd-EOB-DTPA-enhanced magnetic resonance imaging. Invest Radiol 2011; 46:277-283
Yoon JH, Lee JM, Kim E, Okuaki T, Han JK. Quantitative Liver Function Analysis: Volumetric T1 Mapping with Fast Multisection B1 Inhomogeneity Correction in Hepatocyte-specific Contrast-enhanced Liver MR Imaging. Radiology 2017; 282:408-417
Giraudeau C, Leporq B, Doblas S, et al. Gadoxetate-enhanced MR imaging and compartmental modelling to assess hepatocyte bidirectional transport function in rats with advanced liver fibrosis. Eur Radiol 2017; 27:1804-1811
Malinchoc M, Kamath PS, Gordon FD, Peine CJ, Rank J, ter Borg PC. A model to predict poor survival in patients undergoing transjugular intrahepatic portosystemic shunts. Hepatology 2000; 31:864-871
Goshima S, Kanematsu M, Watanabe H, et al. Gd-EOB-DTPA-enhanced MR imaging: prediction of hepatic fibrosis stages using liver contrast enhancement index and liver-to-spleen volumetric ratio. J Magn Reson Imaging 2012; 36:1148-1153
Dahlqvist Leinhard O, Dahlstrom N, Kihlberg J, et al. Quantifying differences in hepatic uptake of the liver specific contrast agents Gd-EOB-DTPA and Gd-BOPTA: a pilot study. Eur Radiol 2012; 22:642-653
Levitt DG. The pharmacokinetics of the interstitial space in humans. BMC Clin Pharmacol 2003; 3:3
Hanley JA, McNeil BJ. A method of comparing the areas under receiver operating characteristic curves derived from the same cases. Radiology 1983; 148:839-843
Razek AA, Abdalla A, Omran E, Fathy A, Zalata K. Diagnosis and quantification of hepatic fibrosis in children with diffusion weighted MR imaging. Eur J Radiol 2011; 78:129-134
Besheer T, Elalfy H, Abd El-Maksoud M, et al. Diffusion-weighted magnetic resonance imaging and micro-RNA in the diagnosis of hepatic fibrosis in chronic hepatitis C virus. World J Gastroenterol 2019; 25:1366-1377
Razek AA, Massoud SM, Azziz MR, El-Bendary MM, Zalata K, Motawea EM. Prediction of esophageal varices in cirrhotic patients with apparent diffusion coefficient of the spleen. Abdom Imaging 2015; 40:1465-1469
Nishie A, Ushijima Y, Tajima T, et al. Quantitative analysis of liver function using superparamagnetic iron oxide- and Gd-EOB-DTPA-enhanced MRI: comparison with Technetium-99 m galactosyl serum albumin scintigraphy. Eur J Radiol 2012; 81:1100-1104
Yoon JH, Lee JM, Kang HJ, et al. Quantitative Assessment of Liver Function by Using Gadoxetic Acid-enhanced MRI: Hepatocyte Uptake Ratio. Radiology 2019; 290:125-133
Rockey DC. Hepatic fibrosis, stellate cells, and portal hypertension. Clin Liver Dis 2006; 10:459-479, vii-viii
Cavalli G, Re G, Casali AM. Red pulp arterial terminals in congestive splenomegaly. A morphometric study. Pathology, research and practice 1984; 178:590-594
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Noda, Y., Goshima, S., Okuaki, T. et al. Hepatocyte fraction: correlation with noninvasive liver functional biomarkers. Abdom Radiol 45, 83–89 (2020). https://doi.org/10.1007/s00261-019-02238-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-019-02238-2