Abstract
Background
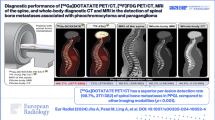
68 Ga-PSMA PET/CT has been widely used in patients with prostate cancer. Due to the limited axial field of view of conventional PET scanners, whole-body dynamic 68 Ga-PSMA PET/CT has not been performed. We investigated the time-activity curves (TACs) of prostate cancer pathological lesions and physiologic bladder activity to determine the optimal 68 Ga-PSMA PET/CT imaging time by total-body (TB) PET/CT.
Methods
Dynamic TB-PET performed on 11 patients with prostate cancer was analyzed. TACs were obtained by drawing regions of interest in normal organs and pathological lesions (primary prostate lesions and lymph nodes and bone metastases). We evaluated the 68 Ga-PSMA uptake pattern of normal organs, urinary bladder, and pathological lesions.
Results
The urinary bladder TAC increased slowly between 180 and 330 s post-injection and then rapidly between 5.5 and 60.0 min post-injection. The pathological lesion uptake increased rapidly during the first 5 min post-injection and then slowly through the remaining 55 min. Six minutes post-injection was the optimal time with the highest pathological lesion SUVmean values still higher than the urinary bladder activity value. However, these prostate lesion, lymph node metastasis, and bone metastasis SUVmean values were one-third, one-half, and one-half the corresponding values 60 min post-injection, suggesting that early imaging might miss low PSMA uptake lesions. A minimum of 35 min post-injection was required for the pathological lesions to have SUVmean values similar to the corresponding values at 60 min post-injection (all P > 0.05), even though the pathological lesion SUVmean values showed a continuous upward trend through the 60 min.
Conclusions
Combining early dynamic 68 Ga-PSMA PET (75–360 s) and conventional static imaging 60 min post-injection could avoid the urinary bladder activity interference to better detect pathological lesions and lesions with relatively low PSMA uptake. The pathological lesion SUVmean values at 35–59 min and 60 min post-injection were similar, so 68 Ga-PSMA PET imaging could also be made at 35–59 min post-injection.






Similar content being viewed by others

Data availability
The data can be obtained from the corresponding author upon request.
References
Perera M, Papa N, Roberts M, Williams M, Udovicich C, Vela I, Christidis D, Bolton D, Hofman MS, Lawrentschuk N, et al. Gallium-68 prostate-specific membrane antigen positron emission tomography in advanced prostate cancer-updated diagnostic utility, sensitivity, specificity, and distribution of prostate-specific membrane antigen-avid lesions: a systematic review and meta-analysis. Eur Urol. 2020;77(4):403–17.
Afshar-Oromieh A, Zechmann CM, Malcher A, Eder M, Eisenhut M, Linhart HG, Holland-Letz T, Hadaschik BA, Giesel FL, Debus J, et al. Comparison of PET imaging with a (68)Ga-LABELLED PSMA ligand and (18)F-choline-based PET/CT for the diagnosis of recurrent prostate cancer. Eur J Nucl Med Mol Imaging. 2014;41(1):11–20.
Fendler WP, Eiber M, Beheshti M, Bomanji J, Ceci F, Cho S, Giesel F, Haberkorn U, Hope TA, Kopka K et al: (68)Ga-PSMA PET/CT: Joint EANM and SNMMI Procedure Guideline for Prostate Cancer Imaging: Version 1.0. Eur J Nucl Med Mol Imaging 2017, 44(6):1014–1024.
Afshar-Oromieh A, Hetzheim H, Kubler W, Kratochwil C, Giesel FL, Hope TA, Eder M, Eisenhut M, Kopka K, Haberkorn U. Radiation dosimetry of (68)Ga-PSMA-11 (HBED-CC) and preliminary evaluation of optimal imaging timing. Eur J Nucl Med Mol Imaging. 2016;43(9):1611–20.
Afshar-Oromieh A, Malcher A, Eder M, Eisenhut M, Linhart HG, Hadaschik BA, Holland-Letz T, Giesel FL, Kratochwil C, Haufe S, et al. PET Imaging with a [68Ga]Gallium-labelled PSMA ligand for the diagnosis of prostate cancer: biodistribution in humans and first evaluation of tumour lesions. Eur J Nucl Med Mol Imaging. 2013;40(4):486–95.
Uprimny C, Kroiss AS, Decristoforo C, Fritz J, Warwitz B, Scarpa L, Roig LG, Kendler D, von Guggenberg E, Bektic J, et al. Early dynamic imaging in (68)Ga- PSMA-11 PET/CT allows discrimination of urinary bladder activity and prostate cancer lesions. Eur J Nucl Med Mol Imaging. 2017;44(5):765–75.
Badawi RD, Shi H, Hu P, Chen S, Xu T, Price PM, Ding Y, Spencer BA, Nardo L, Liu W, et al. First human imaging studies with the EXPLORER total-body PET scanner. J Nucl Med. 2019;60(3):299–303.
Zhang X, Zhou J, Cherry SR, Badawi RD, Qi J. Quantitative image reconstruction for total-body PET imaging using the 2-meter long EXPLORER scanner. Phys Med Biol. 2017;62(6):2465–85.
Cherry SR, Badawi RD, Karp JS, Moses WW, Price P, Jones T: Total-body imaging: transforming the role of positron emission tomography. Sci Transl Med 2017, 9(381).
Zhang X, Xie Z, Berg E, Judenhofer MS, Liu W, Xu T, Ding Y, Lv Y, Dong Y, Deng Z, et al. Total-body dynamic reconstruction and parametric imaging on the uEXPLORER. J Nucl Med. 2020;61(2):285–91.
Liu G, Xu H, Hu P, Tan H, Zhang Y, Yu H, Li X, Shi H. Kinetic metrics of (18)F-FDG in normal human organs identified by systematic dynamic total-body positron emission tomography. Eur J Nucl Med Mol Imaging. 2021;48(8):2363–72.
Demirci E, Sahin OE, Ocak M, Akovali B, Nematyazar J, Kabasakal L. Normal distribution pattern and physiological variants of 68Ga-PSMA-11 PET/CT imaging. Nucl Med Commun. 2016;37(11):1169–79.
Kabasakal L, Demirci E, Ocak M, Akyel R, Nematyazar J, Aygun A, Halac M, Talat Z, Araman A. Evaluation of PSMA PET/CT imaging using a 68Ga-HBED-CC ligand in patients with prostate cancer and the value of early pelvic imaging. Nucl Med Commun. 2015;36(6):582–7.
Barakat A, Yacoub B, Homsi ME, Saad Aldine A, El Hajj A, Haidar MB. Role of early PET/CT imaging with 68Ga-PSMA in staging and restaging of prostate cancer. Sci Rep. 2020;10(1):2705.
Kunikowska J, Cieslak B, Gierej B, Patkowski W, Kraj L, Kotulski M, Zieniewicz K, Krolicki L. [(68) Ga]Ga-prostate-specific membrane antigen PET/CT: a novel method for imaging patients with hepatocellular carcinoma. Eur J Nucl Med Mol Imaging. 2021;48(3):883–92.
Pozzessere C, Bassanelli M, Ceribelli A, Rasul S, Li S, Prior JO, Cicone F. Renal cell carcinoma: the oncologist asks, can PSMA PET/CT answer? Curr Urol Rep. 2019;20(11):68.
Raveenthiran S, Esler R, Yaxley J, Kyle S. The use of (68)Ga-PET/CT PSMA in the staging of primary and suspected recurrent renal cell carcinoma. Eur J Nucl Med Mol Imaging. 2019;46(11):2280–8.
Uijen MJM, Derks YHW, Merkx RIJ, Schilham MGM, Roosen J, Prive BM, van Lith SAM, van Herpen CML, Gotthardt M, Heskamp S et al: PSMA radioligand therapy for solid tumors other than prostate cancer: background, opportunities, challenges, and first clinical reports. Eur J Nucl Med Mol Imaging 2021.
Funding
This study was supported by the Nurture projects for the Youth Medical Talents-Medical Imaging Practitioners Program (grant number SHWRS(2021)_099), the Natural Science Foundation of Shanghai (grant number 21ZR1458900), the Nurture projects for the Youth Medical Talents-Medical Imaging Practitioners Program (grant number SHWRS(2020)_087) and NNSFC 81701724.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Ethics approval
The study involving human participants was in line with principles of Renji hospital ethics committee and the declaration of Helsinki in 1964. This study does not include animal-based research.
Consent to participate
The informed consent was not obtained.
Consent for publication
Not applicable.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Oncology—Genitourinary
Supplementary Information
The maximum intensity projection of dynamic reconstructed images with 92 frames. The animation lasts 92 s, and each second represents one frame.
Rights and permissions
About this article
Cite this article
Wen, J., Zhu, Y., Li, L. et al. Determination of optimal 68 Ga-PSMA PET/CT imaging time in prostate cancers by total-body dynamic PET/CT. Eur J Nucl Med Mol Imaging 49, 2086–2095 (2022). https://doi.org/10.1007/s00259-021-05659-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00259-021-05659-8